Rotavirus Infection in Children
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What is a rotavirus infection?
Rotavirus infection causes severe diarrhea, vomiting, and fever. This can cause life-threatening dehydration. Rotavirus can spread through coughing, food or water, or contact with the bowel movement of an infected person. Rotavirus can remain on objects, such as clothes or toys, for many days. The infection can spread when someone touches an infected object.
What increases my child's risk for a rotavirus infection?
- Age 3 months to 2 years
- Attends daycare
- Frequent travel
- A weak immune system, such as from cancer, HIV, or organ or bone marrow transplants
What are the signs and symptoms of a rotavirus infection?
Symptoms usually begin 1 to 3 days after infection. The rotavirus infection can be spread 2 days before symptoms start, and up to 10 days after. Symptoms normally last from 3 to 8 days and may include more than one of the following:
- Fever
- Nausea, vomiting, and abdominal pain
- Severe, watery diarrhea that usually starts 1 to 2 days after a fever and vomiting
- Fatigue and irritability
- Headaches
How is a rotavirus infection diagnosed?
Your child's healthcare provider will examine your child. Tell the provider about your child's symptoms, including when the diarrhea started and how often it occurs. The provider will check your child for signs of dehydration. A sample of your child's bowel movement may be sent to a lab to be tested for infection.
How is a rotavirus infection treated?
Your child may need any of the following if he or she is dehydrated or at risk for dehydration:
- Extra liquids may be needed. Ask how much liquid your child should drink each day. Good liquids to drink include water or fruit juice. Your child may need an oral rehydrating solution (ORS). This is a drink that contains the right amount of salt, sugar, and minerals in water. If you breastfeed, continue to breastfeed your baby.
- A nasogastric (NG) tube or IV may be needed if your child cannot drink liquids or the dehydration is severe. Liquids can be given through an NG tube that is put in through the nose and down into the stomach.
What can I do to prevent the spread of a rotavirus infection?
- Have your child wash his or her hands often. He or she should wash after using the bathroom and before preparing or eating food. Have your child use soap and water. Show him or her how to rub soapy hands together, lacing the fingers. Wash the front and back of the hands, and in between the fingers. The fingers of one hand can scrub under the fingernails of the other hand. Teach your child to wash for at least 20 seconds. Use a timer, or sing a song that is at least 20 seconds. An example is the happy birthday song 2 times. Have your child rinse with warm, running water for several seconds. Then dry with a clean towel or paper towel. Your older child can use hand sanitizer with alcohol if soap and water are not available.

- Remind your child to cover a sneeze or cough. Show your child how to use a tissue to cover his or her mouth and nose. Have your child throw the tissue away in a trash can right away. Then your child should wash his or her hands well or use a hand sanitizer. Show your child how to use the bend of his or her arm if a tissue is not available.
- Tell your child not to share items. Examples include toys, drinks, and food.
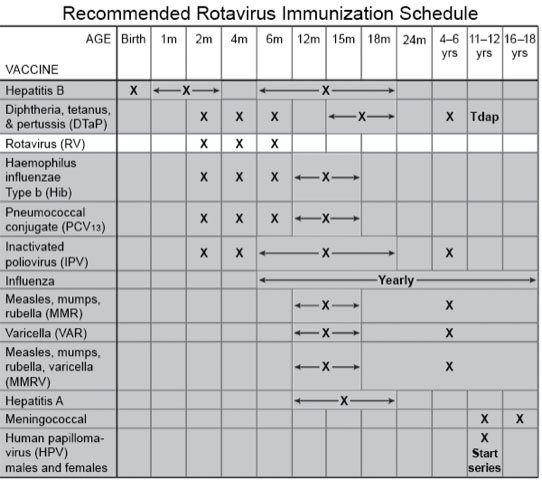
- Ask your child's healthcare provider about the rotavirus vaccine. The vaccine is given routinely to children. Your child will get doses at 2 and 4 months. A third dose may be needed at 6 months. The final dose should be given no later than 8 months of age.
- Clean items that are touched often. Use chlorine-based disinfectants to clean surfaces, toilets, toys, and shared items in your home.
- Keep your child away from other people while he or she is sick. Do not let your child return to school or daycare until his or her healthcare provider says it is safe.
Call your local emergency number (911 in the US) if:
- Your child's body seems floppy and weak, or he or she does not respond to you at all.
- Your child has trouble breathing, or his or her heartbeat is faster than usual.
When should I seek immediate care?
- The soft spot on your baby's head is sunken.
- Your child cannot, or will not, drink at all.
- Your child has a dry, sticky mouth, cries without tears, or has sunken-looking eyes.
- Your child is confused or sleepier than usual.
- Your child cannot stop vomiting.
- Your child's hands and feet suddenly become cold.
When should I call my child's doctor?
- Your child is drinking less liquid than usual.
- Your child urinates less than usual, or your baby has fewer than 6 wet diapers in 1 day.
- Your child has a fever that is not going away or is getting worse.
- Your child has blood in his or her bowel movements.
- Your child has stomach pain, and diarrhea more often.
- Your child's body is puffy and swollen, and his or her face is red.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
