Chemical Pleurodesis
Medically reviewed by Drugs.com. Last updated on Apr 2, 2024.
AMBULATORY CARE:
Pleurodesis
is a procedure to remove air or fluid buildup in the pleural space in your chest. The pleural space is a small, fluid-filled space between your pleura. Pleura are thin layers of tissue that form a 2-layered lining around your lungs. Pleurodesis brings the 2 layers together so there is no room for air or fluid buildup.
 |
How to prepare for pleurodesis:
- Your healthcare provider will talk to you about how to prepare for your procedure. Tell your provider about all medicines you currently take. Include prescription, over-the-counter, and herbal medicines. He or she may tell you to stop taking certain medicines a few days before your procedure. Examples include blood thinners, NSAIDs, and aspirin. Tell your provider if you have ever had an allergic reaction to anesthesia or another medicine.
- Your provider may need to take a sample of the fluid inside your pleural space for testing. You may need blood tests, chest x-rays, an ultrasound, or a CT scan before your procedure. Your provider may use some of these tests to decide where he or she will put your chest tube. Tell your provider if you have ever had an allergic reaction to contrast liquid. If you are a woman, tell your provider if you are or could be pregnant. Some tests could be harmful to an unborn baby.
- Your provider may tell you not to eat or drink anything after midnight on the day of your procedure. He or she will tell you which medicines to take or not take on the day of your procedure. Arrange to have someone drive you home after your pleurodesis.
What will happen during chemical pleurodesis:
Pleurodesis may be done in surgery or at the bedside. Your surgeon will determine which procedure is best for you.
- Surgical pleurodesis: You may be given general anesthesia to keep you asleep so you do not feel pain. Your surgeon will put a chest tube in and drain some of the excess fluid or air from your pleural space. He or she will then inject medicine through the tube into your pleural space.
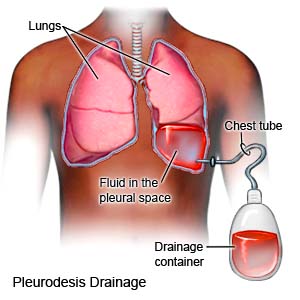
- Bedside pleurodesis: You may be given local anesthesia or conscious sedation. You will be awake, but you should not feel pain. Your surgeon will put a chest tube in and drain some of the excess fluid or air from your pleural space. He or she will then put a medicine into the chest tube and clamp it. You may be asked to change your position several times.
What to expect after pleurodesis:
- Your chest tube will be unclamped after 1 to 4 hours and connected to a collection chamber with suction.
- You may need to stay in the hospital for several days after your procedure. This will allow your healthcare providers to check how much fluid is draining from your pleural space. Your surgeon will remove your chest tube and send you home when there is little to no drainage from your pleural space. A CT scan may also show if fluid or air still remains.
- You may have some chest pain after the procedure. This is normal. Pain medicine may be given if the pain continues. Oxygen may also be given if your blood oxygen level is lower than it should be.
Risks of chemical pleurodesis:
- You may develop a fever. The medicines used for pleurodesis may upset your stomach. Fluids in your pleural space may not be drained completely. The fluids may build up again, and you may need to have another pleurodesis. You may develop an infection or empyema (pus in your pleural space caused by bacteria).
- You may develop pneumonia or other serious lung problems. You may bleed more than expected. You may develop acute respiratory distress syndrome (ARDS)that can cause life-threatening breathing problems.
Call your local emergency number (911 in the US) if:
- You have chest pain that gets worse.
- You have shortness of breath.
Call your doctor if:
- You have a fever.
- Your incision site is red, swollen, or warm to the touch.
- You feel dizzy.
- You cough more than usual.
- You have questions or concerns about your condition or care.
Wound care:
Care for your wound as directed. You may be told it is okay to shower after 2 days. Carefully wash the wound with soap and water. Gently pat the area dry and put on new, clean bandages as directed. Change your bandages when they get wet or dirty. Do not take a bath or swim for 2 weeks, or until your healthcare provider says it is okay.
Self-care:
- Limit your activity. Rest when you feel it is needed. Slowly start to do more each day. Ask your healthcare provider when you can return to work, drive, or travel by airplane.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can worsen your symptoms and cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Follow up with your healthcare provider as directed:
You may need to have another chest x-ray or CT scan to check your lungs after pleurodesis. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
