The originating document has been archived. We cannot confirm the completeness, accuracy, or currency of the content.
Penetrating Injuries to the Pancreas
Medically reviewed by Drugs.com. Last updated on Feb 20, 2025.
WHAT YOU SHOULD KNOW:
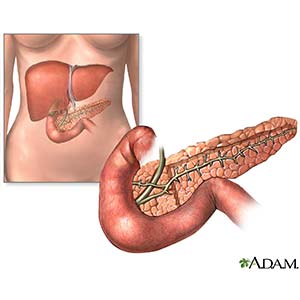
- Penetrating injuries are also called piercing injuries. These may be caused by anything that goes through the skin and into the body. Piercing injuries to the pancreas may cause a tear, cut, or bruise to the organ. These may also result in a severely (badly) damaged organ and bleeding. Gunshot or stab wounds to the abdomen (stomach) or wounds from an accident may injure this organ. Shrapnel, small fragments from a grenade, or other pointed and sharp objects may also cause piercing injuries. The pancreas is an organ behind the stomach that makes enzymes that help you digest food.
- Signs and symptoms may include bleeding or pain and tenderness in your abdomen. Bruising, swelling, or burns on the injured area may also be seen. A complete check-up of your body, including your skin, chest, back, and abdomen, may help diagnose piercing injuries. Imaging tests that take pictures of your abdomen, such as x-rays, ultrasound, and computerized tomography (CT) scan, may be done. Treatment may include drainage, or surgery to repair or take out part of the injured pancreas. The type of surgery that you have will depend on your symptoms, condition, and how severe your injuries are. With treatment, such as surgery, your pancreas may heal over time, and serious problems may be prevented.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your caregivers to decide what care you want to receive. You always have the right to refuse treatment.RISKS:
- Treatment for piercing injuries of the pancreas carries certain risks. Surgery may cause you to bleed too much or other parts of your abdomen to be damaged. You may get an infection. You may get a blood clot in your leg or arm. This can cause pain and swelling, and it can stop blood from flowing where it needs to go in your body. The blood clot can break loose and travel to your lungs. A blood clot in your lungs can cause chest pain and trouble breathing. This problem can be life-threatening.
- If an injury to the pancreas is left untreated, medical problems could develop or worsen. Piercing injuries may cause internal bleeding, leakage of pancreatic fluid, and can be life-threatening. An abscess (pus), or fistula (abnormal connection from the pancreas to another body part) may form. Ask your caregiver if you are worried or have questions about your condition, care, or treatment.
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
Central line:
This is a special IV catheter or tube. It is put into a large vein (blood vessel) near your collarbone, in your neck, or in your groin. The groin is the area where your abdomen meets your upper leg. Other central lines, such as a PICC, may be put into your arm. You may need a central line to receive medicines or IV fluids that need to be given through a big vein. You may need a central line if it is hard for caregivers to insert a regular IV. Also, a central line may stay in longer than a regular IV can. Some central lines may also be used to take blood samples.
An IV
is a small tube placed in your vein that is used to give you medicine or liquids.
Drains:
These are thin rubber tubes put into your skin to drain fluid from around your incision. The drains are taken out when the incision stops draining.
A Foley catheter
is a tube put into your bladder to drain urine into a bag. Keep the bag below your waist. This will prevent urine from flowing back into your bladder and causing an infection or other problems. Also, keep the tube free of kinks so the urine will drain properly. Do not pull on the catheter. This can cause pain and bleeding, and may cause the catheter to come out. Caregivers will remove the catheter as soon as possible to help prevent infection.
Jejunostomy tube (J-Tube):
A jejunostomy tube is a small, flexible tube that is put into a small cut in your abdomen. The end of the tube goes into your small intestine (bowel). The tube is used to give you liquids, food, and medicine. You may have a J-tube for a short time, or long-term. If you need it long-term, your tube may need to be replaced with a new one at certain times.
Nasogastric (NG) tube:
An NG tube is put into your nose, and passes down your throat until it reaches your stomach. Food and medicine may be given through an NG tube if you cannot take anything by mouth. The tube may instead be attached to suction if caregivers need to keep your stomach empty.
Medicines:
You may be given the following medicines:
- Antibiotics: This medicine is given to help treat or prevent an infection caused by bacteria.
- Pain medicine: Caregivers may give you medicine to take away or decrease your pain.
- Do not wait until the pain is severe to ask for your medicine. Tell caregivers if your pain does not decrease. The medicine may not work as well at controlling your pain if you wait too long to take it.
- Pain medicine can make you dizzy or sleepy. Prevent falls by calling a caregiver when you want to get out of bed or if you need help.
- Td vaccine: This vaccine is a booster shot used to help prevent diphtheria and tetanus. The Td booster may be given to adolescents and adults every 10 years or for certain wounds and injuries.
Tests:
One or more of the following tests may be done. Certain tests use a special dye to help organs and structures show up better. Tell caregivers if you are allergic to shellfish (lobster, crab, or shrimp), as you may also be allergic to this dye.
- Blood tests: You may need blood taken to give caregivers information about how your body is working. The blood may be taken from your hand, arm, or IV.
- Computerized tomography scan: This is also called CT scan. A special X-ray machine uses a computer to take pictures of different areas of your abdomen and pelvis. It may be used to look at your bones, organs, and blood vessels. Before taking the pictures, you may be given dye through an IV in your vein.
- Endoscopic retrograde cholangiopancreatography: This is also called ERCP. This test is done during an endoscopy to find injuries to the pancreas, or other problems. Dye is put into the endoscopy tube.
- Abdominal ultrasound: This test is done so caregivers can see the tissues and organs of your abdomen. Gel will be put on your abdomen and a small sensor will be moved across your abdomen. The sensor uses sound waves to send pictures of your abdomen to a TV-like screen.
- X-rays: X-rays of your abdomen may be taken. These may help caregivers look for broken bones, other injuries, or the presence of a foreign body inside your body.
Treatment options:
- Blood transfusion: You will get whole or parts of blood through an IV during a transfusion. Blood is tested for diseases, such as hepatitis and HIV, to be sure it is safe.
- Surgery: Caregivers may do surgery to clean and look for problems, such as bleeding, inside your abdomen. The type of surgery to be done will depend on how severe the injury is and whether other organs are affected. You may need to have more than one surgery. You may have any of the following:
- Drainage: Draining will clean out any old blood or fluid from the pancreas in your abdomen. This may be done by putting thin rubber tubes into your abdomen. The tube may be connected to a suction machine.
- Repair: Caregivers may use sutures (threads) to close a cut or repair an injured organ.
- Excision: This may be done if the pancreas is badly injured. Caregivers may do surgery to take out part of the injured pancreas. The remaining portion of the pancreas may then be connected and sutured (sewn) to other organs.
Vital signs:
Caregivers will check your blood pressure, heart rate, breathing rate, and temperature. They will also ask about your pain. These vital signs give caregivers information about your current health.
Learn more about Penetrating Injuries to the Pancreas
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
