Hysteroscopic Sterilization
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What do I need to know about hysteroscopic sterilization?
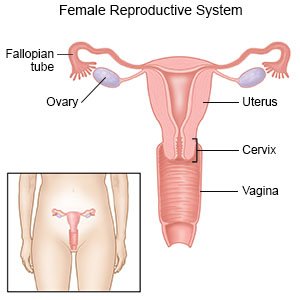
Hysteroscopic sterilization is a procedure to block your fallopian tubes to prevent pregnancy. Small coils made of nickel or titanium are guided into your fallopian tubes. Scar tissue builds up around the coils. The scar tissue prevents sperm from reaching an egg. The coils will never be removed from your fallopian tubes. This is a permanent form of birth control. You will need to be sure you will not ever want to become pregnant before you have this procedure.
 |
How do I prepare for this procedure?
- You will be given local anesthesia as a shot of medicine put into your cervix. It is used to numb the area and dull the pain. You may still feel pressure or pushing during the procedure. Tell your healthcare provider if you have ever had an allergic reaction to local anesthesia.
- Tell your healthcare provider if you are allergic to nickel or any other metals.
What will happen during this procedure?
- You will be placed on a table with your knees bent and feet in stirrups. A hysteroscope will be inserted into your uterus through your vagina and cervix. A camera at the end of the scope will show the inside of your uterus on a monitor. Saline solution will be inserted through the scope. This solution makes your uterus larger and allows your healthcare provider to see your fallopian tubes better.
- When the opening of your fallopian tube is seen, a thin wire will be put through the scope. A coil will be attached to the wire. The wire will be inserted into the opening of your fallopian tube. The coil will then be released into the tube. Once released, the coil will expand and attach to your tube wall. After the coil has been placed inside your fallopian tube, the wire and scope will be removed. The same procedure will then be done for your other fallopian tube.
What will happen after this procedure?
It will take at least 3 months after your procedure for your tubes to be completely blocked. You may still get pregnant during that time. You will need to use a form of birth control until your healthcare provider says the blockage is complete.
What are the risks of this procedure?
- You may have an allergic response to the metal coil used for your procedure. After your procedure, you may have nausea, dizziness, or feel faint. You may have abnormal vaginal bleeding or spotting. You may also have cramping or pain in your abdomen and lower back. Your uterus or fallopian tubes may get a tear from your procedure. You may get blood clots. The coil may move out of place. The coil may move into another area of your body, such as your uterus.
- Even after 3 months, your tubes may not be blocked. You may need to have another procedure or surgery to prevent pregnancy permanently.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
