Hardware Removal
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What do I need to know about hardware removal?
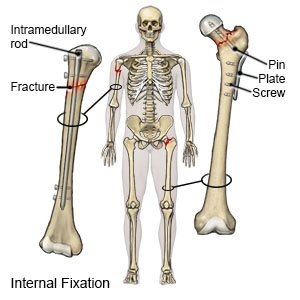
Hardware removal is surgery to take out devices used to hold your broken bones together while they heal. These devices may include pins, screws, plates, or wires. You may need hardware removed because you have pain or an infection. Hardware in young children may need to be removed to prevent problems with bone growth.
 |
How do I prepare for hardware removal?
- Your surgeon will tell you how to prepare. He or she may tell you not to eat or drink anything after midnight on the day of surgery. Arrange to have someone drive you home after surgery.
- Tell your surgeon about all the medicines you currently take. He or she will tell you if you need to stop any medicine before surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon about all your allergies. Tell him or her if you had an allergic reaction to any medicine, including antibiotics or anesthesia.
What will happen during hardware removal?
- You may be given general anesthesia to keep you asleep during surgery. You may instead have local anesthesia to numb the area where you are having surgery. You will be awake during the surgery if you have local anesthesia. You may also receive medicine to keep you calm and relaxed during surgery.
- An incision will be made near the location of your hardware. Your surgeon may use the original surgery incision or create a new incision.
- Your surgeon will use small tools to loosen and remove the hardware. Scar tissue that formed around the hardware may also need to be removed. The hardware may be removed or replaced with new hardware.
- The incision will be closed with stitches. A bandage will cover your incision to help prevent infection.
What should I expect after hardware removal?
- Take deep breaths and cough 10 times each hour. This will decrease your risk for a lung infection. Take a deep breath and hold it for as long as you can. Let the air out and then cough strongly. Deep breaths help open your airway. You may be given an incentive spirometer to help you take deep breaths. Put the plastic piece in your mouth and take a slow, deep breath, then let the air out and cough. Repeat these steps 10 times every hour.
- Medicines may be given to prevent or treat pain, nausea, or an infection caused by bacteria.
- Physical therapy (PT) may be started. PT can help you learn to move safely while you heal. You may also increase range of motion and build strength. PT may continue after you leave the hospital.
What are the risks of hardware removal?
- Nerves, ligaments, and muscles may be damaged. Your bone may fracture again while the hardware is being removed. You may get a blood clot in your leg or arm. This may become life-threatening.
- You may still have pain, even after the hardware is removed. You may have trouble going back to your usual activities. You may have a permanent scar.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
