Cataract Removal
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about cataract removal:
Cataract removal is a procedure to remove a cloudy lens from your eye. An artificial lens called an intraocular lens (IOL) is put in its place. This will improve your vision. The procedure is usually done on one eye at a time. Your healthcare provider will wait about 4 weeks before removing your other cataract.
How to prepare for cataract removal:
- Your healthcare provider will measure your eye's length and how much it curves. He or she will also check your vision. This helps him or her choose the best IOL to put in your eye when the cataract is removed.
- Your healthcare provider may tell you to stop taking anticoagulants 1 to 2 weeks before your procedure. Your provider may give you antibiotic eyedrops to use for a few days before your procedure to prevent infection. Make arrangements for someone to drive you home after your procedure.
What happens during the procedure:
- Your healthcare provider may put drops in your eye to dilate your pupil. This makes it easier for healthcare providers to put in the IOL without damaging your eye. He or she may also use eye drops to numb your eyes. Your healthcare provider may, instead, give you a shot of numbing medicine beside, under, or in your eye. You will also be given a pill to relax you and reduce your anxiety.
- After your pupil is fully dilated, a tool will hold your eye open to prevent blinking. A small incision will be made in your cornea (clear covering over your iris). A tiny instrument will be placed next to the cloudy lens. This instrument uses sound waves to break the lens into small pieces that are suctioned out. The IOL will then be placed in this area. The incision will close on its own. Antibiotic and anti-inflammatory drops may be placed in your eye.
What will happen after the procedure:
You will be able to go home after the procedure.
- An eye shield may be used to cover your eye and protect it from damage.
- Eyedrops will be given to help prevent infection and decrease inflammation.
Risks:
You may develop an eye infection and bleeding inside the eye. Your retina may swell, or a piece may break off. This is called detachment. You may go blind. You may develop glaucoma (increased pressure inside your eye). You may have swelling in and damage to your cornea. Sometimes the area where the IOL is placed also clouds up. This may happen months or even years after the procedure.
Seek care immediately if:
- You suddenly see flashes or floaters, followed by partial vision loss like a curtain covered your eye.
- Your eye suddenly goes blind.
- You have severe eye pain with eye redness, swelling, new floaters, and more blurry vision.
Contact your ophthalmologist if:
- You have changes in your vision.
- Your eye pain increases.
- Your eye is red, swollen, or draining fluid or pus.
- You have a headache or nausea, or you are vomiting.
- You have questions or concerns about your condition or care.
Medicines:
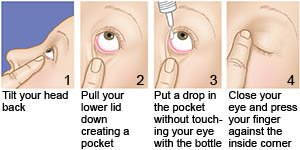
- Eyedrops contain medicine to help prevent infection and decrease inflammation. Wash your hands before you instill eyedrops. Do not touch the tip of the dropper to your eye. Ask your healthcare provider for more information about how to instill eyedrops.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Follow up with your ophthalmologist within 24 hours and as directed:
You will need to have your eye checked. Write down your questions so you remember to ask them during your visits.
Eye care:
- Wear your eye shield when you sleep to prevent damage.

- Do not rub your eye.
- Keep dust, dirt, and water out of your eye to prevent infection.
- Do not lift heavy objects or bend over. Both can increase the pressure in your eye. Ask your healthcare provider how much weight is safe for you to lift. You may be told not to lift anything heavier than 25 pounds for 3 weeks after your procedure.
- Wear UVB protective sunglasses and a brimmed hat outside to help prevent sun damage to your eyes.
- If you smoke, it is never too late to quit. Smoking can damage your eye and prevent it from healing after your procedure. Do not smoke or let anyone smoke around you. Ask your healthcare provider for information if you need help quitting.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
