Picc (Peripherally Inserted Central Catheter)
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What do I need to know about a peripherally inserted central catheter (PICC)?
A PICC is a catheter (small tube) used to give treatments and to take blood. The catheter is inserted into an arm vein. These veins are called peripheral veins. The catheter is guided through the peripheral vein into a central vein near your heart.
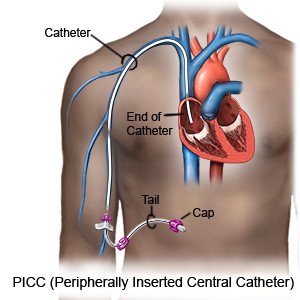 |
Why may I need a PICC?
- You need to have your blood drawn often.
- You will be given medicines often, or you need medicines that must work quickly.
- Your central venous pressure needs to be monitored.
- You need IV medicines after you leave the hospital. The PICC allows you to get your medicines at home.
- You cannot eat or drink anything by mouth.
What do I need to know about how a PICC is placed?
- You will get local anesthesia to numb the area. The catheter will be put into a vein. It will be guided up until the tip is in the vena cava. This is an area close to your heart. Ultrasound or x-ray pictures will be used to make sure the catheter is in the correct position. The other end of the catheter will stay outside your body.
- The catheter will be flushed with liquid. Heparin may be used to flush the line to prevent blood clots. Medicine will be placed at the insertion site (the place where it goes into your skin). The medicine helps prevent an infection at the site.
- The catheter will be secured to your skin with a dressing. The dressing holds it in place, keeps it clean, and helps prevent infection. The dressing will be clear so you can check the insertion site for signs of infection. Another x-ray helps make sure the catheter is in the right place and is ready for you to use.
- Healthcare providers will watch for problems during the PICC placement. You could have bleeding when the PICC is inserted. An infection could develop at the insertion site. An infection that enters your bloodstream can cause serious illness. Rarely, your lung could get pierced when the PICC is inserted. This can cause a collapsed lung.
What will healthcare providers teach me about the PICC?
- Supplies you need to keep on hand to use, care for, and flush the PICC
- How to use the PICC, and when to keep it clamped
- How and when to flush and care for the PICC
- Problems that may develop, such as a hole in the catheter, and what to do to fix the problems
- How to bathe and do your daily activities with a PICC in place
- How to prevent infections
- Signs and symptoms of an infection to watch for and what to do if an infection develops
What can I do to prevent an infection?
The area around your catheter may get infected, or you may get an infection in your bloodstream. A bloodstream infection is called a central line-associated bloodstream infection (CLABSI). A CLABSI is caused by bacteria getting into your bloodstream through your catheter. This can lead to severe illness. The following are ways you can help prevent an infection:
- Wash your hands often. Use soap or an alcohol-based hand rub to clean your hands. Clean your hands before and after you touch the catheter or the catheter site. Remind anyone who cares for your catheter to wash his or her hands.

- Limit contact with the catheter. Do not touch or handle your catheter unless you need to care for it. Do not pull, push on, or move the catheter when you clean your skin or change the dressing. Wear clean medical gloves when you touch your catheter or change dressings.
- Clean your skin as directed. Clean the skin around your catheter every day and before you change your dressing. Ask your healthcare provider what to use to clean your skin. Check your skin every day for signs of infection, such as pain, redness, swelling, and oozing. Contact your healthcare provider if you see these signs.
- Change the dressing as directed. Keep a sterile dressing over the catheter site. Change the dressing as directed or when it is loose, wet, dirty, or falls off. Clean the skin under the dressing with the solution your healthcare provider suggests. Let the area dry before you put on the new dressing. Do not blow on your skin to help it dry.
- Keep the area dry. Wrap your arm with plastic and seal it with medical tape before you bathe. Take showers instead of baths. Do not swim or soak in a hot tub.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
