Cholecystectomy
Medically reviewed by Drugs.com. Last updated on Nov 27, 2023.
What is Cholecystectomy?

Cholecystectomy is the surgical removal of the gallbladder, the small saclike organ located near the liver in the upper right side of the abdomen. It is attached to the main duct that carries bile from the liver into the intestine. Bile helps your body to break down and absorb fats. The gallbladder temporarily stores bile from the liver. When you eat, the gallbladder contracts, and squeezes extra bile into the intestine to aid digestion.
There are two ways to remove the gallbladder:
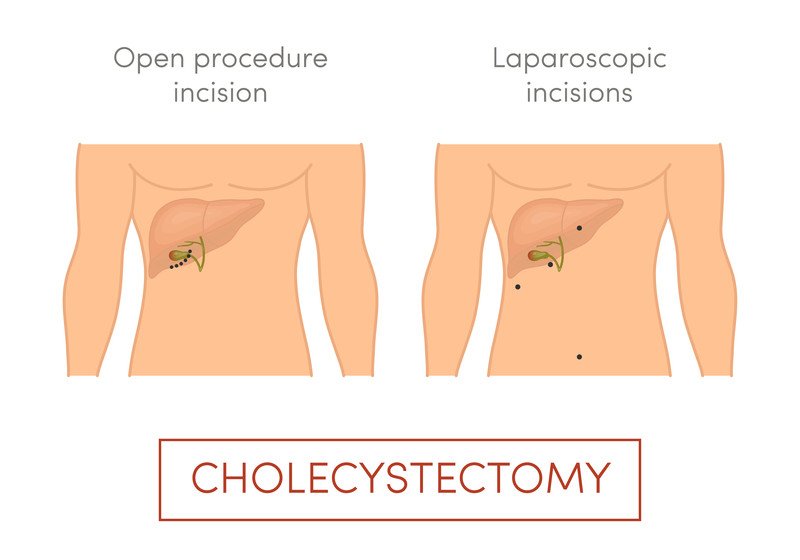
- Traditional surgery – The surgeon cuts open the abdomen and removes the gallbladder through an incision that is about 6 inches long. The abdomen is then stitched closed again.
- Laparoscopic surgery – The surgeon makes four small (less than an inch) incisions for a laparoscope and instruments. A laparoscope is a tube-like instrument with a camera for viewing, and with it the surgeon can to guide the surgical instruments to remove the gallbladder. The gallbladder is cut away from the liver and the bile duct and removed through one of the small incisions.
Over 90% of the time, laparoscopic surgery is used because it requires a shorter hospital stay, is less painful, and has a shorter recovery time compared to traditional surgery. Traditional surgery is usually used because the person has significant abdominal scarring from prior surgery, severe inflammation, unusual anatomy, or other factors that make surgery with a laparoscope very difficult and riskier.
Most people have no side effects from living without a gallbladder. Bile can still pass directly from the liver to the intestines, so the gallbladder usually is not necessary. Occasionally, people notice a tendency to diarrhea after the gallbladder is removed.
What It's Used For
Surgeons remove gallbladders to prevent complications from gallstones, which are rocklike lumps that form inside the gallbladder. Gallstones can cause symptoms as simple as intermittent crampy pain after eating, but they also can lead to cholecystitis, cholangitis, or pancreatitis.
Cholecystitis is an inflammation or infection of the gallbladder that develops when a gallstone blocks the bile duct (or tube) that leads from the gallbladder to the main bile duct. Cholecystitis causes fever, nausea or vomiting, and pain in the upper right side of the abdomen.
Cholangitis is an infection of the bile ducts that may occur when a gallstone passes out of the gallbladder and blocks the main bile duct between the liver and intestine.
Pancreatitis is an inflammation of the pancreas that can be caused by a gallstone blocking the duct coming from the pancreas (this pancreatic duct is attached to the bile duct). This leads to pancreatic enzymes irritating and inflaming the pancreas.
Cholecystitis is not usually a severe problem, but cholangitis and pancreatitis can be.
Preparation
Your doctor will review your allergies and your medical and surgical history. If there is any chance that you may be pregnant or you are trying to get pregnant, tell your doctor before your surgery.
About one week before surgery, you will need to stop taking blood-thinning medications. Beginning at midnight on the night before your surgery, you must not eat or drink anything. This reduces the risk of vomiting during surgery.
You will need to have someone drive you home after surgery.
How It's Done
No matter which type of surgery you have, you will be put under general anesthesia, making you unconscious during your surgery. An intravenous (IV) line inserted into one of your veins will deliver fluids and medications.
- Traditional surgery – The surgeon cuts a 6-inch incision in the upper right side of your abdomen and removes your gallbladder. Often, a test called cholangiography is done during the operation to look for any stones that may have passed into the main bile duct (in this test, a dye is injected into the bile ducts and X-rays are taken). If stones are seen on the X-rays, they may be removed, and a tube may then be placed in the common bile duct (and coming out of the skin) for drainage, until some time after the surgery. After the gallbladder is removed, the incision is closed with stitches. While in the hospital, you gradually will resume eating a normal diet and get out of bed. Usually you stay in the hospital for two to five days.
- Laparoscopic surgery – The surgeon makes a small incision at the navel and puts air into the abdomen to make it easier to see. This help to avoid damaging any organs with the incisions or instruments. Next the laparoscope is inserted through the small incision at your navel. Once the laparoscope is inside your abdomen, a camera on the laparoscope transmits images to a viewing screen. Three smaller incisions are made, and the surgical instruments are inserted through these incisions. The surgeon cuts out the gallbladder, and removes the gallbladder through one of the incisions, usually the one at your bellybutton. All of the instruments are removed, and the surgeon closes the incisions with stitches or surgical tape. After you wake up from anesthesia, the IV line remains in place until you can drink fluids on your own, usually within a few hours after surgery. If you are having a same-day procedure, you can leave the hospital when you feel well enough to go home safely. You may be able to eat a light meal later that day (in the evening). Sometimes patients stay in the hospital until the next morning.
If there are any difficulties during a laparoscopic surgery, the surgeon will switch to a traditional cholecystectomy. This may happen if there is too much bleeding, if there is much scarring from previous surgery, if the gallbladder is difficult to remove, or if there is severe infection.
Follow-Up
You will need to visit your doctor for follow-up sometime after you leave the hospital. This may be within a few days to a few weeks after you return home from the hospital. Your doctor will check the healing of your incisions and remove any stitches. After laparoscopic surgery, you usually can return to work within three to seven days. After traditional surgery, you may need to wait three to six weeks before going back to work. Check with your doctor before resuming specific activities, such as sports, heavy labor and lifting.
Risks
Possible complications of a cholecystectomy include infection, bleeding, blood clots, damage to bile ducts, retained gall stones, and injury to surrounding organs. Occasionally, people have diarrhea after cholecystectomy. A medication called cholestyramine (Questran) can help to treat the diarrhea.
When to Call a Professional
Once you return home from the hospital, call your doctor immediately if you develop a fever or if your incision becomes red, tender or swollen.
Additional Information:
American College of Surgeons (ACS)
https://www.facs.org/
American Liver Foundation
https://www.liverfoundation.org/
National Institutes of Diabetes and Digestive and Kidney Diseases
https://www.niddk.nih.gov/
Image: Masia8/Dreamstime
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
