Flovent Prescribing Information
Package insert / product label
Generic name: fluticasone propionate
Dosage form: inhalation aerosol
Drug class: Inhaled corticosteroids
Medically reviewed by Drugs.com. Last updated on Oct 2, 2023.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
FLOVENT HFA (fluticasone propionate inhalation aerosol), for oral inhalation use
Initial U.S. Approval: 1994
Indications and Usage for Flovent
Flovent Dosage and Administration
- •
- For oral inhalation only. (2.1)
- •
- Starting dosage is based on prior asthma therapy and disease severity. (2.2)
- •
- Adult and adolescent patients aged 12 years and older: 88 mcg twice daily up to a maximum dosage of 880 mcg twice daily. (2.2)
- •
- Pediatric patients aged 4 to 11 years: 88 mcg twice daily. (2.2)
Dosage Forms and Strengths
Contraindications
Warnings and Precautions
- •
- Candida albicans infection of the mouth and pharynx may occur. Monitor patients periodically. Advise the patient to rinse his/her mouth with water without swallowing after inhalation to help reduce the risk. (5.1)
- •
- Potential worsening of infections (e.g., existing tuberculosis; fungal, bacterial, viral, or parasitic infections; ocular herpes simplex). Use with caution in patients with these infections. More serious or even fatal course of chickenpox or measles can occur in susceptible patients. (5.3)
- •
- Risk of impaired adrenal function when transferring from systemic corticosteroids. Taper patients slowly from systemic corticosteroids if transferring to FLOVENT HFA. (5.4)
- •
- Hypercorticism and adrenal suppression may occur with very high dosages or at the regular dosage in susceptible individuals. If such changes occur, discontinue FLOVENT HFA slowly. (5.5)
- •
- Assess for decrease in bone mineral density initially and periodically thereafter. (5.7)
- •
- Monitor growth of pediatric patients. (5.8)
- •
- Glaucoma and cataracts may occur with long-term use of an inhaled corticosteroid (ICS). Consider referral to an ophthalmologist in patients who develop ocular symptoms or use FLOVENT HFA long term. (5.9)
Adverse Reactions/Side Effects
Most common adverse reactions (incidence >3%) are upper respiratory tract infection or inflammation, throat irritation, sinusitis, dysphonia, candidiasis, cough, bronchitis, and headache. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact GlaxoSmithKline at 1-888-825-5249 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Strong cytochrome P450 3A4 inhibitors (e.g., ritonavir, ketoconazole): Use not recommended. May increase risk of systemic corticosteroid effects. (7.1)
Use In Specific Populations
Hepatic impairment: Monitor patients for signs of increased drug exposure. (8.6)
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 9/2023
Related/similar drugs
fluticasone, dexamethasone, Symbicort, budesonide, prednisolone, Breo Ellipta, Dupixent
Full Prescribing Information
1. Indications and Usage for Flovent
FLOVENT HFA is indicated for the maintenance treatment of asthma as prophylactic therapy in adult and pediatric patients aged 4 years and older.
Limitations of Use
FLOVENT HFA is not indicated for the relief of acute bronchospasm.
2. Flovent Dosage and Administration
2.1 Administration Information
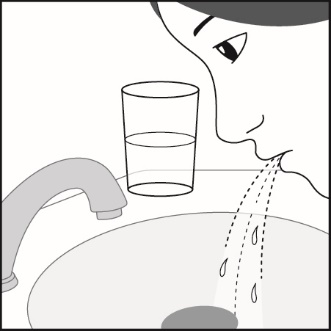
FLOVENT HFA should be administered by the orally inhaled route only. After inhalation, rinse mouth with water without swallowing to help reduce the risk of oropharyngeal candidiasis.
A valved holding chamber and mask may be used to deliver FLOVENT HFA to young patients.
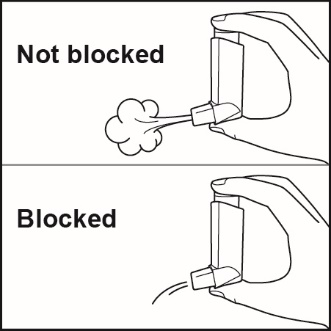
Priming
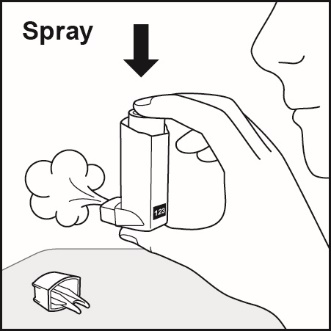
Prime FLOVENT HFA before using for the first time by releasing 4 sprays into the air away from the face, shaking well for 5 seconds before each spray. In cases where the inhaler has not been used for more than 7 days or when it has been dropped, prime the inhaler again by shaking well for 5 seconds and releasing 1 spray into the air away from the face. Avoid spraying in eyes.
2.2 Recommended Dosage
Adult and Adolescent Patients Aged 12 Years and Older
The recommended starting dosage for patients aged 12 years and older who are not on an inhaled corticosteroid (ICS): 88 mcg (2 inhalations of 44 mcg fluticasone propionate) twice daily by oral inhalation, approximately 12 hours apart.
- •
- The maximum recommended dosage for patients aged 12 years and older is 880 mcg twice daily.
Pediatric Patients Aged 4 to 11 Years
The recommended dosage for patients aged 4 to 11 years: 88 mcg (2 inhalations of 44 mcg fluticasone propionate) twice daily by oral inhalation, approximately 12 hours apart.
General Dosing Recommendations
The starting dosage is based on previous asthma therapy and asthma severity, including consideration of patients’ current control of asthma symptoms and risk of future exacerbation.
If symptoms arise between doses, an inhaled short-acting beta2-agonist should be used for immediate relief.
Individual patients will experience a variable time to onset and degree of symptom relief. Maximum benefit may not be achieved for 1 to 2 weeks or longer after starting treatment.
For other patients, and for patients who do not respond adequately to the starting dosage after 2 weeks of therapy, higher dosages may provide additional asthma control.
If a dosage regimen fails to provide adequate control of asthma, the therapeutic regimen should be re-evaluated and additional therapeutic options, e.g., replacing the current strength with a higher strength, initiating an ICS and long-acting beta2-agonist (LABA) combination product, or initiating oral corticosteroids, should be considered.
After asthma stability has been achieved, titrate to the lowest effective dosage to reduce the possibility of side effects.
3. Dosage Forms and Strengths
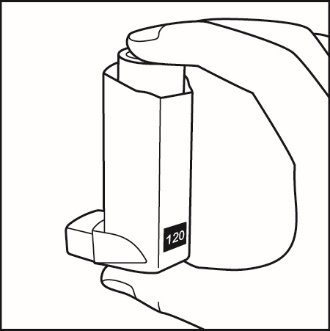
Inhalation aerosol: dark orange plastic inhaler with a peach cap containing a pressurized metered-dose aerosol canister containing 120 metered inhalations and fitted with a counter.
- •
- 44 mcg of fluticasone propionate from the mouthpiece per actuation
- •
- 110 mcg of fluticasone propionate from the mouthpiece per actuation
- •
- 220 mcg of fluticasone propionate from the mouthpiece per actuation
5. Warnings and Precautions
5.1 Oropharyngeal Candidiasis
In clinical trials, the development of localized infections of the mouth and pharynx with Candida albicans has occurred in subjects treated with FLOVENT HFA. When such an infection develops, it should be treated with appropriate local or systemic (i.e., oral) antifungal therapy while treatment with FLOVENT HFA continues, but at times therapy with FLOVENT HFA may need to be interrupted. Advise the patient to rinse his/her mouth with water without swallowing following inhalation to help reduce the risk of oropharyngeal candidiasis.
5.2 Acute Asthma Episodes
FLOVENT HFA is not to be regarded as a bronchodilator and is not indicated for rapid relief of bronchospasm. Patients should be instructed to contact their physicians immediately when episodes of asthma that are not responsive to bronchodilators occur during the course of treatment with FLOVENT HFA. During such episodes, patients may require therapy with oral corticosteroids.
5.3 Immunosuppression and Risk of Infections
Persons who are using drugs that suppress the immune system are more susceptible to infections than healthy individuals. Chickenpox and measles, for example, can have a more serious or even fatal course in susceptible children or adults using corticosteroids. In such children or adults who have not had these diseases or been properly immunized, particular care should be taken to avoid exposure. How the dose, route, and duration of corticosteroid administration affect the risk of developing a disseminated infection is not known. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is also not known. If a patient is exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If a patient is exposed to measles, prophylaxis with pooled intramuscular immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing information.) If chickenpox develops, treatment with antiviral agents may be considered.
ICS should be used with caution, if at all, in patients with active or quiescent tuberculosis infections of the respiratory tract; systemic fungal, bacterial, viral, or parasitic infections; or ocular herpes simplex.
5.4 Transferring Patients from Systemic Corticosteroid Therapy
Hypothalamic-Pituitary-Adrenal Suppression/Adrenal Insufficiency
Particular care is needed for patients who have been transferred from systemically active corticosteroids to ICS because deaths due to adrenal insufficiency have occurred in patients with asthma during and after transfer from systemic corticosteroids to less systemically available ICS. After withdrawal from systemic corticosteroids, a number of months are required for recovery of hypothalamic-pituitary-adrenal (HPA) function.
Patients who have been previously maintained on 20 mg or more of prednisone (or its equivalent) may be most susceptible, particularly when their systemic corticosteroids have been almost completely withdrawn. During this period of HPA suppression, patients may exhibit signs and symptoms of adrenal insufficiency when exposed to trauma, surgery, or infection (particularly gastroenteritis) or other conditions associated with severe electrolyte loss. Although FLOVENT HFA may control asthma symptoms during these episodes, in recommended doses it supplies less than normal physiological amounts of glucocorticoid systemically and does NOT provide the mineralocorticoid activity that is necessary for coping with these emergencies.
During periods of stress or a severe asthma attack, patients who have been withdrawn from systemic corticosteroids should be instructed to resume oral corticosteroids (in large doses) immediately and to contact their physicians for further instruction. These patients should also be instructed to carry a warning card indicating that they may need supplementary systemic corticosteroids during periods of stress or a severe asthma attack.
Patients requiring oral corticosteroids should be weaned slowly from systemic corticosteroid use after transferring to FLOVENT HFA. Prednisone reduction can be accomplished by reducing the daily prednisone dose by 2.5 mg on a weekly basis during therapy with FLOVENT HFA. Lung function (mean forced expiratory volume in 1 second [FEV1] or morning peak expiratory flow [AM PEF]), beta-agonist use, and asthma symptoms should be carefully monitored during withdrawal of oral corticosteroids. In addition, patients should be observed for signs and symptoms of adrenal insufficiency, such as fatigue, lassitude, weakness, nausea and vomiting, and hypotension.
Unmasking of Allergic Conditions Previously Suppressed by Systemic Corticosteroids
Transfer of patients from systemic corticosteroid therapy to FLOVENT HFA may unmask allergic conditions previously suppressed by the systemic corticosteroid therapy (e.g., rhinitis, conjunctivitis, eczema, arthritis, eosinophilic conditions).
Corticosteroid Withdrawal Symptoms
During withdrawal from oral corticosteroids, some patients may experience symptoms of systemically active corticosteroid withdrawal (e.g., joint and/or muscular pain, lassitude, depression) despite maintenance or even improvement of respiratory function.
5.5 Hypercorticism and Adrenal Suppression
Fluticasone propionate will often help control asthma symptoms with less suppression of HPA function than therapeutically equivalent oral doses of prednisone. Since fluticasone propionate is absorbed into the circulation and can be systemically active at higher doses, the beneficial effects of FLOVENT HFA in minimizing HPA dysfunction may be expected only when recommended dosages are not exceeded and individual patients are titrated to the lowest effective dose. A relationship between plasma levels of fluticasone propionate and inhibitory effects on stimulated cortisol production has been shown after 4 weeks of treatment with fluticasone propionate inhalation aerosol. Since individual sensitivity to effects on cortisol production exists, physicians should consider this information when prescribing FLOVENT HFA.
Because of the possibility of significant systemic absorption of ICS in sensitive patients, patients treated with FLOVENT HFA should be observed carefully for any evidence of systemic corticosteroid effects. Particular care should be taken in observing patients postoperatively or during periods of stress for evidence of inadequate adrenal response.
It is possible that systemic corticosteroid effects such as hypercorticism and adrenal suppression (including adrenal crisis) may appear in a small number of patients who are sensitive to these effects. If such effects occur, FLOVENT HFA should be reduced slowly, consistent with accepted procedures for reducing systemic corticosteroids, and other treatments for management of asthma symptoms should be considered.
5.6 Hypersensitivity Reactions, including Anaphylaxis
Immediate hypersensitivity reactions (e.g., urticaria, angioedema, rash, bronchospasm, hypotension), including anaphylaxis, may occur after administration of FLOVENT HFA [see Contraindications (4)].
5.7 Reduction in Bone Mineral Density
Decreases in bone mineral density (BMD) have been observed with long-term administration of products containing ICS. The clinical significance of small changes in BMD with regard to long-term consequences such as fracture is unknown. Patients with major risk factors for decreased bone mineral content, such as prolonged immobilization, family history of osteoporosis, postmenopausal status, tobacco use, advanced age, poor nutrition, or chronic use of drugs that can reduce bone mass (e.g., anticonvulsants, oral corticosteroids), should be monitored and treated with established standards of care.
A 2-year trial in 160 subjects (females aged 18 to 40 years, males 18 to 50) with asthma receiving chlorofluorocarbon (CFC)-propelled fluticasone propionate inhalation aerosol 88 or 440 mcg twice daily demonstrated no statistically significant changes in BMD at any time point (24, 52, 76, and 104 weeks of double-blind treatment) as assessed by dual-energy x-ray absorptiometry at lumbar regions L1 through L4.
5.8 Effect on Growth
Orally inhaled corticosteroids may cause a reduction in growth velocity when administered to pediatric patients. Monitor the growth of pediatric patients receiving FLOVENT HFA routinely (e.g., via stadiometry). To minimize the systemic effects of orally inhaled corticosteroids, including FLOVENT HFA, titrate each patient’s dosage to the lowest dosage that effectively controls his/her symptoms [see Dosage and Administration (2.2), Use in Specific Populations (8.4)].
5.9 Glaucoma and Cataracts
Glaucoma, increased intraocular pressure, and cataracts have been reported in patients following the long-term administration of ICS, including fluticasone propionate. Consider referral to an ophthalmologist in patients who develop ocular symptoms or use FLOVENT HFA long term.
5.10 Paradoxical Bronchospasm
As with other inhaled medicines, bronchospasm may occur with an immediate increase in wheezing after dosing. If bronchospasm occurs following dosing with FLOVENT HFA, it should be treated immediately with an inhaled, short-acting bronchodilator; FLOVENT HFA should be discontinued immediately; and alternative therapy should be instituted.
5.11 Drug Interactions with Strong Cytochrome P450 3A4 Inhibitors
The use of strong cytochrome P450 3A4 (CYP3A4) inhibitors (e.g., ritonavir, atazanavir, clarithromycin, indinavir, itraconazole, nefazodone, nelfinavir, saquinavir, ketoconazole, telithromycin) with FLOVENT HFA is not recommended because increased systemic corticosteroid adverse effects may occur [see Drug Interactions (7.1), Clinical Pharmacology (12.3)].
5.12 Eosinophilic Conditions and Churg-Strauss Syndrome
In rare cases, patients on inhaled fluticasone propionate may present with systemic eosinophilic conditions. Some of these patients have clinical features of vasculitis consistent with Churg-Strauss syndrome, a condition that is often treated with systemic corticosteroid therapy. These events usually, but not always, have been associated with the reduction and/or withdrawal of oral corticosteroid therapy following the introduction of fluticasone propionate. Cases of serious eosinophilic conditions have also been reported with other ICS in this clinical setting. Physicians should be alert to eosinophilia, vasculitic rash, worsening pulmonary symptoms, cardiac complications, and/or neuropathy presenting in their patients. A causal relationship between fluticasone propionate and these underlying conditions has not been established.
6. Adverse Reactions/Side Effects
The following clinically significant adverse reactions are described elsewhere in the labeling:
- •
- Oropharyngeal candidiasis infection [see Warnings and Precautions (5.1)]
- •
- Immunosuppression and risk of infections [see Warnings and Precautions (5.3)]
- •
- Hypercorticism and adrenal suppression [see Warnings and Precautions (5.5)]
- •
- Reduction in bone mineral density [see Warnings and Precautions (5.7)]
- •
- Growth effects [see Warnings and Precautions (5.8)]
- •
- Glaucoma and cataracts [see Warnings and Precautions (5.9)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The incidence of common adverse reactions in Table 1 is based upon 2 placebo-controlled U.S. clinical trials in which 812 adult and adolescent subjects (457 females and 355 males) previously treated with as-needed bronchodilators and/or ICS were treated twice daily for up to 12 weeks with 2 inhalations of FLOVENT HFA 44 mcg, FLOVENT HFA 110 mcg, FLOVENT HFA 220 mcg (dosages of 88, 220, or 440 mcg twice daily), or placebo.
|
Adverse Event |
FLOVENT HFA 88 mcg Twice Daily (n = 203) % |
FLOVENT HFA 220 mcg Twice Daily (n = 204) % |
FLOVENT HFA 440 mcg Twice Daily (n = 202) % |
Placebo (n = 203) % |
|
Ear, nose, and throat | ||||
|
18 |
16 |
16 |
14 |
|
8 |
8 |
10 |
5 |
|
2 |
5 |
5 |
1 |
|
6 |
7 |
4 |
3 |
|
2 |
3 |
6 |
<1 |
|
Gastrointestinal | ||||
|
4 |
2 |
5 |
<1 |
|
Lower respiratory | ||||
|
4 |
6 |
4 |
5 |
|
2 |
2 |
6 |
5 |
|
Neurological | ||||
|
11 |
7 |
5 |
6 |
Table 1 includes all events (whether considered drug-related or nondrug-related by the investigator) that occurred at a rate of over 3% in any of the groups treated with FLOVENT HFA and were more common than in the placebo group. Less than 2% of subjects discontinued from the trials because of adverse reactions. The average duration of exposure was 73 to 76 days in the active treatment groups compared with 60 days in the placebo group.
Additional Adverse Reactions
Other adverse reactions not previously listed, whether considered drug-related or not by the investigators, that were reported more frequently by subjects with asthma treated with FLOVENT HFA compared with subjects treated with placebo include the following: rhinitis, rhinorrhea/post-nasal drip, nasal sinus disorders, laryngitis, diarrhea, viral gastrointestinal infections, dyspeptic symptoms, gastrointestinal discomfort and pain, hyposalivation, musculoskeletal pain, muscle pain, muscle stiffness/tightness/rigidity, dizziness, migraines, fever, viral infections, pain, chest symptoms, viral skin infections, muscle injuries, soft tissue injuries, urinary infections.
Fluticasone propionate inhalation aerosol (440 or 880 mcg twice daily) was administered for 16 weeks to 168 subjects with asthma requiring oral corticosteroids (Trial 3). Adverse reactions not included above but reported by more than 3 subjects in either group treated with FLOVENT HFA and more commonly than in the placebo group included nausea and vomiting, arthralgia and articular rheumatism, and malaise and fatigue.
In 2 long-term trials (26 and 52 weeks), the pattern of adverse reactions in subjects treated with FLOVENT HFA at dosages up to 440 mcg twice daily was similar to that observed in the 12-week trials. There were no new and/or unexpected adverse reactions with long-term treatment.
Pediatric Subjects Aged 4 to 11 Years
FLOVENT HFA has been evaluated for safety in 56 pediatric subjects who received 88 mcg twice daily for 4 weeks. Types of adverse reactions in these pediatric subjects were generally similar to those observed in adults and adolescents.
6.2 Postmarketing Experience
In addition to adverse reactions reported from clinical trials, the following adverse reactions have been identified during postapproval use of fluticasone propionate. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These events have been chosen for inclusion due to either their seriousness, frequency of reporting, or causal connection to fluticasone propionate or a combination of these factors.
Ear, Nose, and Throat
Aphonia, facial and oropharyngeal edema, and throat soreness and irritation.
Endocrine and Metabolic
Cushingoid features, growth velocity reduction in children/adolescents, hyperglycemia, osteoporosis, and weight gain.
Eye
Cataracts.
Gastrointestinal Disorders
Dental caries and tooth discoloration.
Immune System Disorders
Immediate and delayed hypersensitivity reactions, including urticaria, anaphylaxis, rash, and angioedema and bronchospasm, have been reported.
Infections and Infestations
Esophageal candidiasis.
Psychiatry
Agitation, aggression, anxiety, depression, and restlessness. Behavioral changes, including hyperactivity and irritability, have been reported very rarely and primarily in children.
Respiratory
Asthma exacerbation, chest tightness, cough, dyspnea, immediate and delayed bronchospasm, paradoxical bronchospasm, pneumonia, and wheeze.
Skin
Contusions, cutaneous hypersensitivity reactions, ecchymoses, and pruritus.
7. Drug Interactions
7.1 Inhibitors of Cytochrome P450 3A4
Fluticasone propionate is a substrate of CYP3A4. The use of strong CYP3A4 inhibitors (e.g., ritonavir, atazanavir, clarithromycin, indinavir, itraconazole, nefazodone, nelfinavir, saquinavir, ketoconazole, telithromycin) with FLOVENT HFA is not recommended because increased systemic corticosteroid adverse effects may occur.
Ritonavir
A drug interaction trial with fluticasone propionate aqueous nasal spray in healthy subjects has shown that ritonavir (a strong CYP3A4 inhibitor) can significantly increase plasma fluticasone propionate exposure, resulting in significantly reduced serum cortisol concentrations [see Clinical Pharmacology (12.3)]. During postmarketing use, there have been reports of clinically significant drug interactions in patients receiving fluticasone propionate and ritonavir, resulting in systemic corticosteroid effects including Cushing’s syndrome and adrenal suppression.
Ketoconazole
Coadministration of orally inhaled fluticasone propionate (1,000 mcg) and ketoconazole (200 mg once daily) resulted in a 1.9-fold increase in plasma fluticasone propionate exposure and a 45% decrease in plasma cortisol area under the curve (AUC), but had no effect on urinary excretion of cortisol.
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
There are insufficient data on the use of FLOVENT HFA in pregnant women. There are clinical considerations with the use of FLOVENT HFA in pregnant women. (See Clinical Considerations.) In animals, teratogenicity characteristic of corticosteroids, decreased fetal body weight and/or skeletal variations in rats, mice, and rabbits, was observed with subcutaneously administered maternal toxic doses of fluticasone propionate less than the maximum recommended human daily inhaled dose (MRHDID) on a mcg/m2 basis. (See Data.) However, fluticasone propionate administered via inhalation to rats decreased fetal body weight but did not induce teratogenicity at a maternal toxic dose less than the MRHDID on a mcg/m2 basis. (See Data.) Experience with oral corticosteroids suggests that rodents are more prone to teratogenic effects from corticosteroids than humans.
The estimated risk of major birth defects and miscarriage for the indicated population is unknown. In the U.S. general population, the estimated risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryofetal Risk: In women with poorly or moderately controlled asthma, there is an increased risk of several perinatal outcomes such as pre-eclampsia in the mother and prematurity, low birth weight, and small for gestational age in the neonate. Pregnant women with asthma should be closely monitored and medication adjusted as necessary to maintain optimal asthma control.
Data
Human Data: Following inhaled administration, fluticasone propionate was detected in the neonatal cord blood after delivery.
Animal Data: In embryofetal development studies with pregnant rats and mice dosed by the subcutaneous route throughout the period of organogenesis, fluticasone propionate was teratogenic in both species. Omphalocele, decreased body weight, and skeletal variations were observed in rat fetuses, in the presence of maternal toxicity, at a dose approximately 0.5 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 100 mcg/kg/day). The rat no observed adverse effect level (NOAEL) was observed at approximately 0.17 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 30 mcg/kg/day). Cleft palate and fetal skeletal variations were observed in mouse fetuses at a dose approximately 0.1 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 45 mcg/kg/day). The mouse NOAEL was observed with a dose approximately 0.04 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 15 mcg/kg/day).
In an embryofetal development study with pregnant rats dosed by the inhalation route throughout the period of organogenesis, fluticasone propionate produced decreased fetal body weights and skeletal variations, in the presence of maternal toxicity, at a dose approximately 0.14 times the MRHDID (on a mcg/m2 basis with a maternal inhalation dose of 25.7 mcg/kg/day); however, there was no evidence of teratogenicity. The NOAEL was observed with a dose approximately 0.03 times the MRHDID (on a mcg/m2 basis with a maternal inhalation dose of 5.5 mcg/kg/day).
In an embryofetal development study in pregnant rabbits that were dosed by the subcutaneous route throughout organogenesis, fluticasone propionate produced reductions of fetal body weights, in the presence of maternal toxicity, at doses approximately 0.006 times the MRHDID and higher (on a mcg/m2 basis with a maternal subcutaneous dose of 0.57 mcg/kg/day). Teratogenicity was evident based upon a finding of cleft palate for 1 fetus at a dose approximately 0.04 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 4 mcg/kg/day). The NOAEL was observed in rabbit fetuses with a dose approximately 0.001 times the MRHDID (on a mcg/m2 basis with a maternal subcutaneous dose of 0.08 mcg/kg/day).
Fluticasone propionate crossed the placenta following subcutaneous administration to mice and rats and oral administration to rabbits.
In a pre- and post-natal development study in pregnant rats dosed from late gestation through delivery and lactation (Gestation Day 17 to Postpartum Day 22), fluticasone propionate was not associated with decreases in pup body weight, and had no effects on developmental landmarks, learning, memory, reflexes, or fertility at doses up to 0.3 times the MRHDID (on a mcg/m2 basis with maternal subcutaneous doses up to 50 mcg/kg/day).
8.2 Lactation
Risk Summary
There are no available data on the presence of fluticasone propionate in human milk, the effects on the breastfed child, or the effects on milk production. Other corticosteroids have been detected in human milk. However, fluticasone propionate concentrations in plasma after inhaled therapeutic doses are low and therefore concentrations in human breast milk are likely to be correspondingly low [see Clinical Pharmacology (12.3)]. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for FLOVENT HFA and any potential adverse effects on the breastfed child from FLOVENT HFA or from the underlying maternal condition.
Data
Animal Data: Subcutaneous administration of tritiated fluticasone propionate at a dose of 10 mcg/kg/day to lactating rats resulted in measurable levels in milk.
8.4 Pediatric Use
The safety and effectiveness of FLOVENT HFA in pediatric patients aged 4 years and older have been established [see Adverse Reactions (6.1), Clinical Pharmacology (12.3), Clinical Studies (14.2)]. Use of FLOVENT HFA in patients aged 4 to 11 years is supported by evidence from adequate and well-controlled trials in adults and adolescents aged 12 years and older, pharmacokinetic trials in patients aged 4 to 11 years, established efficacy of fluticasone propionate formulated as FLOVENT DISKUS (fluticasone propionate inhalation powder) and FLOVENT ROTADISK (fluticasone propionate inhalation powder) in patients aged 4 to 11 years, and supportive findings with FLOVENT HFA in a trial conducted in subjects aged 4 to 11 years.
The safety and effectiveness of FLOVENT HFA in pediatric patients younger than 4 years have not been established.
Effects on Growth
Orally inhaled corticosteroids may cause a reduction in growth velocity when administered to pediatric patients. A reduction of growth velocity in children or teenagers may occur as a result of poorly controlled asthma or from use of corticosteroids including ICS. The effects of long-term treatment of children and adolescents with ICS, including fluticasone propionate, on final adult height are not known.
Controlled clinical trials have shown that ICS may cause a reduction in growth in pediatric patients. In these trials, the mean reduction in growth velocity was approximately 1 cm/year (range: 0.3 to 1.8 cm/year) and appeared to depend upon dose and duration of exposure. This effect was observed in the absence of laboratory evidence of HPA axis suppression, suggesting that growth velocity is a more sensitive indicator of systemic corticosteroid exposure in pediatric patients than some commonly used tests of HPA axis function. The long-term effects of this reduction in growth velocity associated with orally inhaled corticosteroids, including the impact on final adult height, are unknown. The potential for “catch-up” growth following discontinuation of treatment with orally inhaled corticosteroids has not been adequately studied. The effects on growth velocity of treatment with orally inhaled corticosteroids for over 1 year, including the impact on final adult height, are unknown. The growth of children and adolescents receiving orally inhaled corticosteroids, including FLOVENT HFA, should be monitored routinely (e.g., via stadiometry). The potential growth effects of prolonged treatment should be weighed against the clinical benefits obtained and the risks associated with alternative therapies. To minimize the systemic effects of orally inhaled corticosteroids, including FLOVENT HFA, each patient should be titrated to the lowest dose that effectively controls his/her symptoms.
Since a cross trial comparison in adult and adolescent subjects (aged 12 years and older) indicated that systemic exposure of inhaled fluticasone propionate from FLOVENT HFA would be higher than exposure from FLOVENT ROTADISK, results from a trial to assess the potential growth effects of FLOVENT ROTADISK in pediatric subjects (aged 4 to 11 years) are provided.
A 52-week placebo-controlled trial to assess the potential growth effects of fluticasone propionate inhalation powder (FLOVENT ROTADISK) at 50 and 100 mcg twice daily was conducted in the U.S. in 325 prepubescent children (244 males and 81 females) aged 4 to 11 years. The mean growth velocities at 52 weeks observed in the intent-to-treat population were 6.32 cm/year in the placebo group (n = 76), 6.07 cm/year in the 50-mcg group (n = 98), and 5.66 cm/year in the 100-mcg group (n = 89). An imbalance in the proportion of children entering puberty between groups and a higher dropout rate in the placebo group due to poorly controlled asthma may be confounding factors in interpreting these data. A separate subset analysis of children who remained prepubertal during the trial revealed growth rates at 52 weeks of 6.10 cm/year in the placebo group (n = 57), 5.91 cm/year in the 50-mcg group (n = 74), and 5.67 cm/year in the 100-mcg group (n = 79). In children aged 8.5 years, the mean age of children in this trial, the range for expected growth velocity is: boys – 3rd percentile = 3.8 cm/year, 50th percentile = 5.4 cm/year, and 97th percentile = 7.0 cm/year; girls – 3rd percentile = 4.2 cm/year, 50th percentile = 5.7 cm/year, and 97th percentile = 7.3 cm/year. The clinical relevance of these growth data is not certain.
Pediatric Patients Younger than 4 Years
Pharmacokinetics: [see Clinical Pharmacology (12.3)].
Pharmacodynamics: A 12-week, double-blind, placebo-controlled, parallel-group trial was conducted in children with asthma aged 1 to younger than 4 years. Twelve-hour overnight urinary cortisol excretion after a 12-week treatment period with 88 mcg of FLOVENT HFA twice daily (n = 73) and with placebo (n = 42) were calculated. The mean and median change from baseline in urine cortisol over 12 hours were -0.7 and 0.0 mcg for FLOVENT HFA and 0.3 and -0.2 mcg for placebo, respectively.
In a 1-way crossover trial in children aged 6 to younger than 12 months with reactive airways disease (N = 21), serum cortisol was measured over a 12-hour dosing period. Subjects received placebo treatment for a 2-week period followed by a 4-week treatment period with 88 mcg of FLOVENT HFA twice daily with an AeroChamber Plus Valved Holding Chamber (VHC) with mask. The geometric mean ratio of serum cortisol over 12 hours [AUC(0-12 h)] following FLOVENT HFA (n = 16) versus placebo (n = 18) was 0.95 (95% CI: 0.72, 1.27).
Safety: FLOVENT HFA administered as 88 mcg twice daily was evaluated for safety in 239 pediatric subjects aged 1 to younger than 4 years in a 12-week, double-blind, placebo-controlled trial. Treatments were administered with an AeroChamber Plus VHC with mask. The following events occurred with a frequency >3% and more frequently in subjects receiving FLOVENT HFA than in subjects receiving placebo, regardless of causality assessment: pyrexia, nasopharyngitis, upper respiratory tract infection, vomiting, otitis media, diarrhea, bronchitis, pharyngitis, and viral infection.
FLOVENT HFA administered as 88 mcg twice daily was evaluated for safety in 23 pediatric subjects aged 6 to 12 months in an open-label placebo-controlled trial. Treatments were administered with an AeroChamber Plus VHC with mask for 2 weeks with placebo followed by 4 weeks with active drug. There was no discernable difference in the types of adverse events reported between subjects receiving placebo compared with the active drug.
In Vitro Testing of Dose Delivery with Holding Chambers: In vitro dose characterization studies were performed to evaluate the delivery of FLOVENT HFA via holding chambers with attached masks. The studies were conducted with 2 different holding chambers (AeroChamber Plus VHC and AeroChamber Z-STAT Plus VHC) with masks (small and medium size) at inspiratory flow rates of 4.9, 8.0, and 12.0 L/min in combination with holding times of 0, 2, 5, and 10 seconds. The flow rates were selected to be representative of inspiratory flow rates of children aged 6 to 12 months, 2 to 5 years, and over 5 years, respectively. The mean delivered dose of fluticasone propionate through the holding chambers with masks was lower than the 44 mcg of fluticasone propionate delivered directly from the actuator mouthpiece. The results were similar through both holding chambers (see Table 2 for data for the AeroChamber Plus VHC). The fine particle fraction (approximately 1 to 5 μm) across the flow rates used in these studies was 70% to 84% of the delivered dose, consistent with the removal of the coarser fraction by the holding chamber. In contrast, the fine particle fraction for FLOVENT HFA delivered without a holding chamber typically represents 42% to 55% of the delivered dose measured at the standard flow rate of 28.3 L/min. These data suggest that, on a per kilogram basis, young children receive a comparable dose of fluticasone propionate when delivered via a holding chamber and mask as adults do without their use.
| a Centers for Disease Control growth charts, developed by the National Center for Health Statistics in collaboration with the National Center for Chronic Disease Prevention and Health Promotion (2000). Ranges correspond to the average of the 50th percentile weight for boys and girls at the ages indicated. b A single inhalation of FLOVENT HFA in a 70-kg adult without use of a valved holding chamber and mask delivers approximately 44 mcg, or 0.6 mcg/kg. |
||||||
|
Age |
Mask |
Flow Rate (L/min) |
Holding Time (seconds) |
Mean Medication Delivery through AeroChamber Plus Valved Holding Chamber (mcg/actuation) |
Body Weight 50th Percentile (kg)a |
Medication Delivered per Actuation (mcg/kg)b |
|
6 to 12 Months |
Small |
4.9 |
0 |
8.3 |
7.5-9.9 |
0.8-1.1 |
|
2 |
6.7 |
0.7-0.9 |
||||
|
5 |
7.5 |
0.8-1.0 |
||||
|
10 |
7.5 |
0.8-1.0 |
||||
|
2 to 5 Years |
Small |
8.0 |
0 |
7.3 |
12.3-18.0 |
0.4-0.6 |
|
2 |
6.8 |
0.4-0.6 |
||||
|
5 |
6.7 |
0.4-0.5 |
||||
|
10 |
7.7 |
0.4-0.6 |
||||
|
2 to 5 Years |
Medium |
8.0 |
0 |
7.8 |
12.3-18.0 |
0.4-0.6 |
|
2 |
7.7 |
0.4-0.6 |
||||
|
5 |
8.1 |
0.5-0.7 |
||||
|
10 |
9.0 |
0.5-0.7 |
||||
|
>5 Years |
Medium |
12.0 |
0 |
12.3 |
18.0 |
0.7 |
|
2 |
11.8 |
0.7 |
||||
|
5 |
12.0 |
0.7 |
||||
|
10 |
10.1 |
0.6 |
||||
8.5 Geriatric Use
Of the total number of subjects treated with FLOVENT HFA in U.S. and non-U.S. clinical trials, 173 were aged 65 years or older, 19 of which were 75 years or older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger subjects, but greater sensitivity of some older individuals cannot be ruled out.
8.6 Hepatic Impairment
Formal pharmacokinetic studies using FLOVENT HFA have not been conducted in patients with hepatic impairment. Since fluticasone propionate is predominantly cleared by hepatic metabolism, impairment of liver function may lead to accumulation of fluticasone propionate in plasma. Therefore, patients with hepatic disease should be closely monitored.
10. Overdosage
Chronic overdosage may result in signs/symptoms of hypercorticism [see Warnings and Precautions (5.5)].
11. Flovent Description
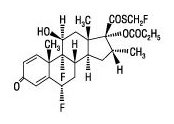
FLOVENT HFA is a pressurized metered dose inhaler for oral inhalation. The active component of FLOVENT HFA 44 mcg, FLOVENT HFA 110 mcg, and FLOVENT HFA 220 mcg is fluticasone propionate, a corticosteroid having the chemical name S-(fluoromethyl) 6α,9-difluoro-11β,17-dihydroxy-16α-methyl-3-oxoandrosta-1,4-diene-17β-carbothioate,17-propionate and the following chemical structure:
Fluticasone propionate is a white powder with a molecular weight of 500.6, and the empirical formula is C25H31F3O5S. It is practically insoluble in water, freely soluble in dimethyl sulfoxide and dimethylformamide, and slightly soluble in methanol and 95% ethanol.
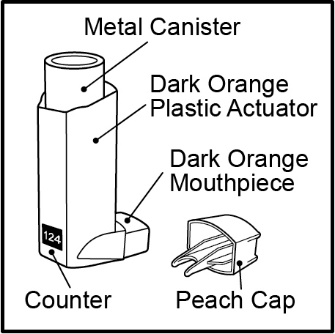
FLOVENT HFA is a dark orange plastic inhaler with a peach cap containing a pressurized metered-dose aerosol canister fitted with a counter. Each canister contains a microcrystalline suspension of micronized fluticasone propionate in propellant HFA-134a (1,1,1,2-tetrafluoroethane). It contains no other excipients.
After priming, each actuation of the inhaler delivers 50, 125, or 250 mcg of fluticasone propionate in 60 mg of suspension (for the 44-mcg product) or in 75 mg of suspension (for the 110- and 220-mcg products) from the valve. Each actuation delivers 44, 110, or 220 mcg of fluticasone propionate from the actuator. The actual amount of drug delivered to the lung will depend on patient factors, such as the coordination between the actuation of the inhaler and inspiration through the delivery system.
Prime FLOVENT HFA before using for the first time by releasing 4 sprays into the air away from the face, shaking well for 5 seconds before each spray. In cases where the inhaler has not been used for more than 7 days or when it has been dropped, prime the inhaler again by shaking well for 5 seconds and releasing 1 spray into the air away from the face. Avoid spraying in eyes.
12. Flovent - Clinical Pharmacology
12.1 Mechanism of Action
Fluticasone propionate is a synthetic trifluorinated corticosteroid with anti-inflammatory activity. Fluticasone propionate has been shown in vitro to exhibit a binding affinity for the human glucocorticoid receptor that is 18 times that of dexamethasone, almost twice that of beclomethasone‑17‑monopropionate (BMP), the active metabolite of beclomethasone dipropionate, and over 3 times that of budesonide. Data from the McKenzie vasoconstrictor assay in man are consistent with these results. The clinical significance of these findings is unknown.
Inflammation is an important component in the pathogenesis of asthma. Corticosteroids have been shown to have a wide range of actions on multiple cell types (e.g., mast cells, eosinophils, neutrophils, macrophages, lymphocytes) and mediators (e.g., histamine, eicosanoids, leukotrienes, cytokines) involved in inflammation. These anti-inflammatory actions of corticosteroids contribute to their efficacy in asthma.
Though effective for the treatment of asthma, corticosteroids do not affect asthma symptoms immediately. Individual patients will experience a variable time to onset and degree of symptom relief. Maximum benefit may not be achieved for 1 to 2 weeks or longer after starting treatment. When corticosteroids are discontinued, asthma stability may persist for several days or longer.
Trials in subjects with asthma have shown a favorable ratio between topical anti-inflammatory activity and systemic corticosteroid effects with recommended doses of orally inhaled fluticasone propionate. This is explained by a combination of a relatively high local anti-inflammatory effect, negligible oral systemic bioavailability (<1%), and the minimal pharmacological activity of the only metabolite detected in man.
12.2 Pharmacodynamics
Serum cortisol concentrations, urinary excretion of cortisol, and urine 6-β-hydroxycortisol excretion collected over 24 hours in 24 healthy subjects following 8 inhalations of fluticasone propionate HFA 44, 110, and 220 mcg decreased with increasing dose. However, in patients with asthma treated with 2 inhalations of fluticasone propionate HFA 44, 110, and 220 mcg twice daily for at least 4 weeks, differences in serum cortisol AUC(0-12 h) (n = 65) and 24-hour urinary excretion of cortisol (n = 47) compared with placebo were not related to dose and generally not significant. In the trial with healthy volunteers, the effect of propellant was also evaluated by comparing results following the 220-mcg strength inhaler containing HFA 134a propellant with the same strength of inhaler containing CFC 11/12 propellant. A lesser effect on the HPA axis with the HFA formulation was observed for serum cortisol, but not urine cortisol and 6-betahydroxy cortisol excretion. In addition, in a crossover trial in children with asthma aged 4 to 11 years (N = 40), 24-hour urinary excretion of cortisol was not affected after a 4-week treatment period with 88 mcg of fluticasone propionate HFA twice daily compared with urinary excretion after the 2-week placebo period. The ratio (95% CI) of urinary excretion of cortisol over 24 hours following fluticasone propionate HFA versus placebo was 0.987 (0.796, 1.223).
The potential systemic effects of fluticasone propionate HFA on the HPA axis were also studied in subjects with asthma. Fluticasone propionate given by inhalation aerosol at dosages of 440 or 880 mcg twice daily was compared with placebo in oral corticosteroid-dependent subjects with asthma (range of mean dose of prednisone at baseline: 13 to 14 mg/day) in a 16-week trial. Consistent with maintenance treatment with oral corticosteroids, abnormal plasma cortisol responses to short cosyntropin stimulation (peak plasma cortisol <18 mcg/dL) were present at baseline in the majority of subjects participating in this trial (69% of subjects later randomized to placebo and 72% to 78% of subjects later randomized to fluticasone propionate HFA). At week 16, 8 subjects (73%) on placebo compared with 14 (54%) and 13 (68%) subjects receiving fluticasone propionate HFA (440 and 880 mcg twice daily, respectively) had post-stimulation cortisol levels of <18 mcg/dL.
12.3 Pharmacokinetics
Absorption
Fluticasone propionate acts locally in the lung; therefore, plasma levels do not predict therapeutic effect. Trials using oral dosing of labeled and unlabeled drug have demonstrated that the oral systemic bioavailability of fluticasone propionate is negligible (<1%), primarily due to incomplete absorption and presystemic metabolism in the gut and liver. In contrast, the majority of the fluticasone propionate delivered to the lung is systemically absorbed.
Distribution
Following intravenous administration, the initial disposition phase for fluticasone propionate was rapid and consistent with its high lipid solubility and tissue binding. The volume of distribution averaged 4.2 L/kg.
The percentage of fluticasone propionate bound to human plasma proteins averages 99%. Fluticasone propionate is weakly and reversibly bound to erythrocytes and is not significantly bound to human transcortin.
Elimination
Following intravenous dosing, fluticasone propionate showed polyexponential kinetics and had a terminal elimination half-life of approximately 7.8 hours. The total clearance of fluticasone propionate is high (average, 1,093 mL/min), with renal clearance accounting for <0.02% of the total. Less than 5% of a radiolabeled oral dose was excreted in the urine as metabolites, with the remainder excreted in the feces as parent drug and metabolites.
Metabolism: The only circulating metabolite detected in man is the 17β-carboxylic acid derivative of fluticasone propionate, which is formed through the CYP3A4 pathway. This metabolite had less affinity (approximately 1/2,000) than the parent drug for the glucocorticoid receptor of human lung cytosol in vitro and negligible pharmacological activity in animal studies. Other metabolites detected in vitro using cultured human hepatoma cells have not been detected in man.
Specific Populations
Male and Female Patients: No significant difference in clearance (CL/F) of fluticasone propionate was observed.
Pediatric Patients: A population pharmacokinetic analysis was performed for FLOVENT HFA using steady-state data from 4 controlled clinical trials and single-dose data from 1 controlled clinical trial. The combined cohort for analysis included 269 subjects (161 males and 108 females) with asthma aged 6 months to 66 years who received treatment with FLOVENT HFA. Most of these subjects (n = 215) were treated with FLOVENT HFA 44 mcg given as 88 mcg twice daily. FLOVENT HFA was delivered using an AeroChamber Plus VHC with a mask to subjects aged younger than 4 years. Data from adult subjects with asthma following FLOVENT HFA 110 mcg given as 220 mcg twice daily (n = 15) and following FLOVENT HFA 220 mcg given as 440 mcg twice daily (n = 17) at steady state were also included. Data for 22 subjects came from a single-dose crossover study of 264 mcg (6 doses of FLOVENT HFA 44 mcg) with and without AeroChamber Plus VHC in children with asthma aged 4 to 11 years.
Stratification of exposure data following FLOVENT HFA 88 mcg by age and study indicated that systemic exposure to fluticasone propionate at steady state was similar in children aged 6 to younger than 12 months, children aged 1 to younger than 4 years, and adults and adolescents aged 12 years and older. Exposure was lower in children aged 4 to 11 years, who did not use a VHC, as shown in Table 3.
|
Age |
Valved Holding Chamber |
N |
AUC(0-τ), pg•h/mL (95% CI) |
Cmax, pg/mL (95% CI) |
|
6 to <12 Months |
Yes |
17 |
141 (88, 227) |
19 (13, 29) |
|
1 to <4 Years |
Yes |
164 |
143 (131, 157) |
20 (18, 21) |
|
4 to 11 Years |
No |
14 |
68 (48, 97) |
11 (8, 16) |
|
≥12 Years |
No |
20 |
149 (106, 210) |
20 (15, 27) |
The lower exposure to fluticasone propionate in children aged 4 to 11 years who did not use a VHC may reflect the inability to coordinate actuation and inhalation of the metered-dose inhaler. The impact of the use of a VHC on exposure to fluticasone propionate in patients aged 4 to 11 years was evaluated in a single-dose crossover trial with FLOVENT HFA 44 mcg given as 264 mcg. In this trial, use of a VHC increased systemic exposure to fluticasone propionate (Table 4), possibly correcting for the inability to coordinate actuation and inhalation.
|
Age |
Valved Holding Chamber |
N |
AUC(0-∞), pg•h/mL (95% CI) |
Cmax, pg/mL (95% CI) |
|
4 to 11 Years |
Yes |
22 |
373 (297, 468) |
61 (51, 73) |
|
4 to 11 Years |
No |
21 |
141 (111, 178) |
23 (19, 28) |
There was a dose-related increase in systemic exposure in subjects aged 12 years and older receiving higher doses of fluticasone propionate (220 and 440 mcg twice daily). The AUC(0-τ) in pg•h/mL was 358 (95% CI: 272, 473) and 640 (95% CI: 477, 858), and Cmax in pg/mL was 47.3 (95% CI: 37, 61) and 87 (95% CI: 68, 112) following fluticasone propionate 220 and 440 mcg, respectively.
Patients with Hepatic and Renal Impairment: Formal pharmacokinetic studies using FLOVENT HFA have not been conducted in patients with hepatic or renal impairment. However, since fluticasone propionate is predominantly cleared by hepatic metabolism, impairment of liver function may lead to accumulation of fluticasone propionate in plasma. Therefore, patients with hepatic disease should be closely monitored.
Racial or Ethnic Groups: No significant difference in clearance (CL/F) of fluticasone propionate in Caucasian, African‑American, Asian, or Hispanic populations was observed.
Drug Interaction Studies
Inhibitors of Cytochrome P450 3A4: Ritonavir: Fluticasone propionate is a substrate of CYP3A4. Coadministration of fluticasone propionate and the strong CYP3A4 inhibitor ritonavir is not recommended based upon a multiple-dose, crossover drug interaction trial in 18 healthy subjects. Fluticasone propionate aqueous nasal spray (200 mcg once daily) was coadministered for 7 days with ritonavir (100 mg twice daily). Plasma fluticasone propionate concentrations following fluticasone propionate aqueous nasal spray alone were undetectable (<10 pg/mL) in most subjects, and when concentrations were detectable, peak levels (Cmax) averaged 11.9 pg/mL (range: 10.8 to 14.1 pg/mL) and AUC(0-τ) averaged 8.43 pg•h/mL (range: 4.2 to 18.8 pg•h/mL). Fluticasone propionate Cmax and AUC(0-τ) increased to 318 pg/mL (range: 110 to 648 pg/mL) and 3,102.6 pg•h/mL (range: 1,207.1 to 5,662.0 pg•h/mL), respectively, after coadministration of ritonavir with fluticasone propionate aqueous nasal spray. This significant increase in plasma fluticasone propionate exposure resulted in a significant decrease (86%) in serum cortisol AUC.
Ketoconazole: In a placebo-controlled crossover trial in 8 healthy adult volunteers, coadministration of a single dose of orally inhaled fluticasone propionate (1,000 mcg) with multiple doses of ketoconazole (200 mg) to steady state resulted in increased plasma fluticasone propionate exposure, a reduction in plasma cortisol AUC, and no effect on urinary excretion of cortisol.
Following orally inhaled fluticasone propionate alone, AUC(2-last) averaged 1.559 ng•h/mL (range: 0.555 to 2.906 ng•h/mL) and AUC(2-∞) averaged 2.269 ng•h/mL (range: 0.836 to 3.707 ng•h/mL). Fluticasone propionate AUC(2-last) and AUC(2-∞) increased to 2.781 ng•h/mL (range: 2.489 to 8.486 ng•h/mL) and 4.317 ng•h/mL (range: 3.256 to 9.408 ng•h/mL), respectively, after coadministration of ketoconazole with orally inhaled fluticasone propionate. This increase in plasma fluticasone propionate concentration resulted in a decrease (45%) in serum cortisol AUC.
Erythromycin: In a multiple-dose drug interaction trial, coadministration of orally inhaled fluticasone propionate (500 mcg twice daily) and erythromycin (333 mg 3 times daily) did not affect fluticasone propionate pharmacokinetics.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Fluticasone propionate demonstrated no tumorigenic potential in mice at oral doses up to 1,000 mcg/kg (approximately 3 and 10 times the MRHDID for adults and children aged 4 to 11 years, respectively, on a mcg/m2 basis) for 78 weeks or in rats at inhalation doses up to 57 mcg/kg (approximately 0.3 times and approximately equivalent to the MRHDID for adults and children aged 4 to 11 years, respectively, on a mcg/m2 basis) for 104 weeks.
Fluticasone propionate did not induce gene mutation in prokaryotic or eukaryotic cells in vitro. No significant clastogenic effect was seen in cultured human peripheral lymphocytes in vitro or in the in vivo mouse micronucleus test.
Fertility and reproductive performance were unaffected in male and female rats at subcutaneous doses up to 50 mcg/kg (approximately 0.3 times the MRHDID for adults on a mcg/m2 basis).
14. Clinical Studies
14.1 Adult and Adolescent Subjects Aged 12 Years and Older
Three randomized, double-blind, parallel-group, placebo-controlled, U.S. clinical trials were conducted in 980 adult and adolescent subjects (aged 12 years and older) with asthma to assess the efficacy and safety of FLOVENT HFA in the treatment of asthma. Fixed dosages of 88, 220, and 440 mcg twice daily (each dose administered as 2 inhalations of the 44-, 110-, and 220-mcg strengths, respectively) and 880 mcg twice daily (administered as 4 inhalations of the 220-mcg strength) were compared with placebo to provide information about appropriate dosing to cover a range of asthma severity. Subjects in these trials included those inadequately controlled with bronchodilators alone (Trial 1), those already receiving ICS (Trial 2), and those requiring oral corticosteroid therapy (Trial 3). In all 3 trials, subjects were allowed to use VENTOLIN (albuterol, USP) Inhalation Aerosol as needed for relief of acute asthma symptoms. In Trials 1 and 2, other maintenance asthma therapies were discontinued.
Trial 1 enrolled 397 subjects with asthma inadequately controlled on bronchodilators alone. FLOVENT HFA was evaluated at dosages of 88, 220, and 440 mcg twice daily for 12 weeks. Baseline FEV1 values were similar across groups (mean 67% of predicted normal). All 3 dosages of FLOVENT HFA demonstrated a statistically significant improvement in lung function as measured by improvement in AM pre-dose FEV1 compared with placebo. This improvement was observed after the first week of treatment and was maintained over the 12-week treatment period.
At Endpoint (last observation), mean change from baseline in AM pre-dose percent predicted FEV1 was greater in all 3 groups treated with FLOVENT HFA (9.0% to 11.2%) compared with the placebo group (3.4%). The mean differences between the groups treated with FLOVENT HFA 88, 220, and 440 mcg and the placebo group were statistically significant, and the corresponding 95% confidence intervals were (2.2%, 9.2%), (2.8%, 9.9%), and (4.3%, 11.3%), respectively.
Figure 1 displays results of pulmonary function tests (mean percent change from baseline in FEV1 prior to AM dose) for the recommended starting dosage of FLOVENT HFA (88 mcg twice daily) and placebo from Trial 1. This trial used predetermined criteria for lack of efficacy (indicators of worsening asthma), resulting in withdrawal of more subjects in the placebo group. Therefore, pulmonary function results at Endpoint (the last evaluable FEV1 result, including most subjects’ lung function data) are also displayed.
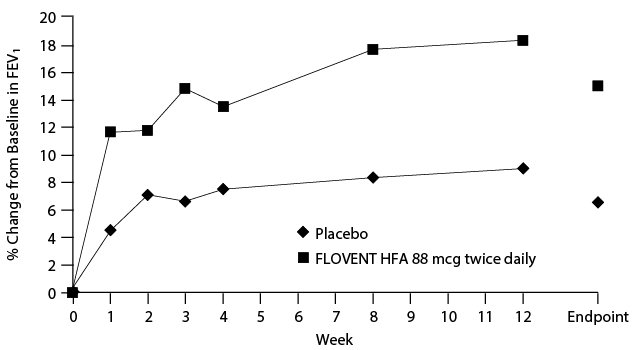
Figure 1. A 12-Week Clinical Trial in Subjects Aged 12 Years and Older Inadequately Controlled on Bronchodilators Alone: Mean Percent Change from Baseline in FEV1 Prior to AM Dose (Trial 1)
In Trial 2, FLOVENT HFA at dosages of 88, 220, and 440 mcg twice daily was evaluated over 12 weeks of treatment in 415 subjects with asthma who were already receiving an ICS at a daily dose within its recommended dose range in addition to as-needed albuterol. Baseline FEV1 values were similar across groups (mean 65% to 66% of predicted normal). All 3 dosages of FLOVENT HFA demonstrated a statistically significant improvement in lung function, as measured by improvement in FEV1, compared with placebo. This improvement was observed after the first week of treatment and was maintained over the 12-week treatment period. Discontinuations from the trial for lack of efficacy (defined by a pre-specified decrease in FEV1 or PEF, or an increase in use of VENTOLIN or nighttime awakenings requiring treatment with VENTOLIN) were lower in the groups treated with FLOVENT HFA (6% to 11%) compared with placebo (50%).
At Endpoint (last observation), mean change from baseline in AM pre-dose percent predicted FEV1 was greater in all 3 groups treated with FLOVENT HFA (2.2% to 4.6%) compared with the placebo group (-8.3%). The mean differences between the groups treated with FLOVENT HFA 88, 220, and 440 mcg and the placebo group were statistically significant, and the corresponding 95% confidence intervals were (7.1%, 13.8%), (8.2%, 14.9%), and (9.6%, 16.4%), respectively.
Figure 2 displays the mean percent change from baseline in FEV1 from Week 1 through Week 12. This trial also used predetermined criteria for lack of efficacy, resulting in withdrawal of more subjects in the placebo group; therefore, pulmonary function results at Endpoint are also displayed.
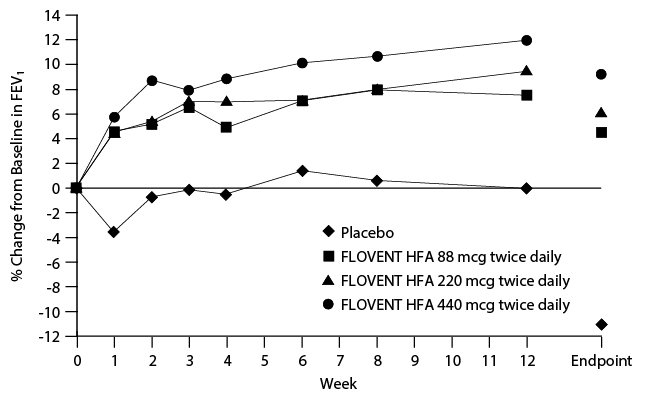
Figure 2. A 12-Week Clinical Trial in Subjects Aged 12 Years and Older Already Receiving Daily Inhaled Corticosteroids: Mean Percent Change from Baseline in FEV1 Prior to AM Dose (Trial 2)
In both trials, use of VENTOLIN, AM and PM PEF, and asthma symptom scores showed numerical improvement with FLOVENT HFA compared with placebo.
Trial 3 enrolled 168 subjects with asthma requiring oral prednisone therapy (average baseline daily prednisone dose ranged from 13 to 14 mg). FLOVENT HFA at dosages of 440 and 880 mcg twice daily was evaluated over a 16-week treatment period. Baseline FEV1 values were similar across groups (mean 59% to 62% of predicted normal). Over the course of the trial, subjects treated with either dosage of FLOVENT HFA required a statistically significantly lower mean daily oral prednisone dose (6 mg) compared with placebo-treated subjects (15 mg). Both dosages of FLOVENT HFA enabled a larger percentage of subjects (59% and 56% in the groups treated with FLOVENT HFA 440 and 880 mcg, respectively, twice daily) to eliminate oral prednisone as compared with placebo (13%) (see Figure 3). There was no efficacy advantage of FLOVENT HFA 880 mcg twice daily compared with 440 mcg twice daily. Accompanying the reduction in oral corticosteroid use, subjects treated with either dosage of FLOVENT HFA had statistically significantly improved lung function, fewer asthma symptoms, and less use of VENTOLIN Inhalation Aerosol compared with the placebo-treated subjects.
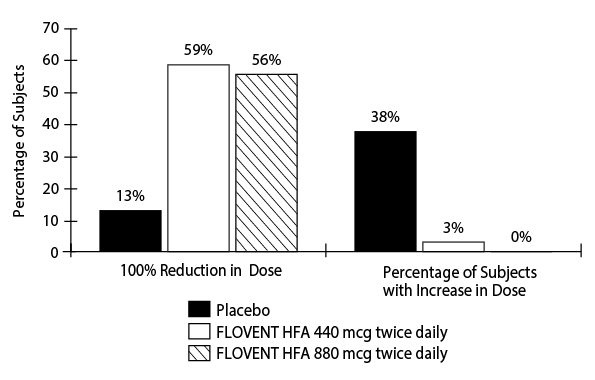
Figure 3. A 16-Week Clinical Trial in Subjects Aged 12 Years and Older Requiring Chronic Oral Prednisone Therapy: Change in Maintenance Prednisone Dose
Two long-term safety trials (Trial 4 and Trial 5) of ≥6 months’ duration were conducted in 507 adult and adolescent subjects with asthma. Trial 4 was designed to monitor the safety of 2 doses of FLOVENT HFA, while Trial 5 compared fluticasone propionate HFA with fluticasone propionate CFC. Trial 4 enrolled 182 subjects who were treated daily with low to high doses of ICS, beta-agonists (short-acting [as needed or regularly scheduled] or long-acting), theophylline, inhaled cromolyn or nedocromil sodium, leukotriene receptor antagonists, or 5-lipoxygenase inhibitors at baseline. FLOVENT HFA at dosages of 220 and 440 mcg twice daily was evaluated over a 26-week treatment period in 89 and 93 subjects, respectively. Trial 5 enrolled 325 subjects who were treated daily with moderate to high doses of ICS, with or without concurrent use of salmeterol or albuterol, at baseline. Fluticasone propionate HFA at a dosage of 440 mcg twice daily and fluticasone propionate CFC at a dosage of 440 mcg twice daily were evaluated over a 52-week treatment period in 163 and 162 subjects, respectively. Baseline FEV1 values were similar across groups (mean 81% to 84% of predicted normal). Throughout the 52-week treatment period, asthma control was maintained with both formulations of fluticasone propionate compared with baseline. In both trials, none of the subjects were withdrawn due to lack of efficacy.
14.2 Pediatric Subjects Aged 4 to 11 Years
A 12-week clinical trial conducted in 241 pediatric subjects with asthma was supportive of efficacy but inconclusive due to measurable levels of fluticasone propionate in 6/48 (13%) of the plasma samples from subjects randomized to placebo. Efficacy in subjects aged 4 to 11 years is extrapolated from adult data with FLOVENT HFA and other supporting data [see Use in Specific Populations (8.4)].
16. How is Flovent supplied
FLOVENT HFA is supplied in the following boxes of 1 as a pressurized aluminum canister fitted with a counter and supplied with a dark orange actuator with a peach cap:
- •
- FLOVENT HFA 44 mcg: 10.6-g canister containing 120 actuations (NDC 0173-0718-20)
- •
- FLOVENT HFA 110 mcg: 12-g canister containing 120 actuations (NDC 0173-0719-20)
- •
- FLOVENT HFA 220 mcg: 12-g canister containing 120 actuations (NDC 0173-0720-20)
Each inhaler is packaged with a Patient Information leaflet.
The dark orange actuator supplied with FLOVENT HFA should not be used with any other product canisters, and actuators from other products should not be used with a FLOVENT HFA canister.
Counter
FLOVENT HFA has a counter attached to the canister. The counter starts at 124 and counts down each time a spray is released. The correct amount of medication in each actuation cannot be assured after the counter reads 000, even though the canister is not completely empty and will continue to operate. The inhaler should be discarded when the counter reads 000.
Contents under Pressure
Do not puncture. Do not use or store near heat or open flame. Exposure to temperatures above 120°F may cause bursting. Never throw canister into fire or incinerator.
Storage
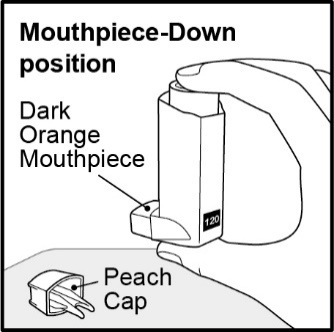
Store at room temperature between 68°F and 77°F (20°C and 25°C); excursions permitted from 59°F to 86°F (15°C to 30°C) [See USP Controlled Room Temperature]. Store the inhaler with the mouthpiece down. For best results, the inhaler should be at room temperature before use.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Patient Information and Instructions for Use).
Oropharyngeal Candidiasis
Inform patients that localized infections with Candida albicans occurred in the mouth and pharynx in some patients. If oropharyngeal candidiasis develops, treat it with appropriate local or systemic (i.e., oral) antifungal therapy while still continuing therapy with FLOVENT HFA, but at times therapy with FLOVENT HFA may need to be temporarily interrupted under close medical supervision. Advise patients to rinse the mouth with water without swallowing after inhalation to help reduce the risk of thrush. [See Warnings and Precautions (5.1).]
Status Asthmaticus and Acute Asthma Symptoms
Inform patients that FLOVENT HFA is not a bronchodilator and is not intended for use as rescue medicine for acute asthma exacerbations. Advise patients to treat acute asthma symptoms with an inhaled, short-acting beta2-agonist such as albuterol. Instruct patients to contact their physicians immediately if there is deterioration of their asthma. [See Warnings and Precautions (5.2).]
Immunosuppression and Risk of Infections
Warn patients who are on immunosuppressant doses of corticosteroids to avoid exposure to chickenpox or measles and, if exposed, to consult their physicians without delay. Inform patients of potential worsening of existing tuberculosis; fungal, bacterial, viral, or parasitic infections; or ocular herpes simplex. [See Warnings and Precautions (5.3).]
Hypercorticism and Adrenal Suppression
Advise patients that FLOVENT HFA may cause systemic corticosteroid effects of hypercorticism and adrenal suppression. Additionally, inform patients that deaths due to adrenal insufficiency have occurred during and after transfer from systemic corticosteroids. Patients should taper slowly from systemic corticosteroids if transferring to FLOVENT HFA. [See Warnings and Precautions (5.5).]
Hypersensitivity Reactions, including Anaphylaxis
Advise patients that immediate hypersensitivity reactions (e.g., urticaria, angioedema, rash, bronchospasm, hypotension), including anaphylaxis, may occur after administration of FLOVENT HFA. Patients should discontinue FLOVENT HFA if such reactions occur. [See Warnings and Precautions (5.6).]
Reduction in Bone Mineral Density
Advise patients who are at an increased risk for decreased BMD that the use of corticosteroids may pose an additional risk. [See Warnings and Precautions (5.7).]
Reduced Growth Velocity
Inform patients that orally inhaled corticosteroids, including FLOVENT HFA, may cause a reduction in growth velocity when administered to pediatric patients. Physicians should closely follow the growth of children and adolescents taking corticosteroids by any route. [See Warnings and Precautions (5.8).]
Glaucoma and Cataracts
Advise patients that long-term use of ICS may increase the risk of some eye problems (cataracts or glaucoma); consider regular eye examinations. [See Warnings and Precautions (5.9).]
Use Daily for Best Effect
Patients should use FLOVENT HFA at regular intervals as directed. Individual patients will experience a variable time to onset and degree of symptom relief and the full benefit may not be achieved until treatment has been administered for 1 to 2 weeks or longer. Patients should not increase the prescribed dosage but should contact their physicians if symptoms do not improve or if the condition worsens. Instruct patients not to stop use of FLOVENT HFA abruptly. Patients should contact their physicians immediately if they discontinue use of FLOVENT HFA.
Trademarks are owned by or licensed to the GSK group of companies. The other brands listed are trademarks owned by or licensed to their respective owners and are not owned by or licensed to the GSK group of companies. The makers of these brands are not affiliated with and do not endorse the GSK group of companies or its products.
GlaxoSmithKline
Durham, NC 27701
©2023 GSK group of companies or its licensor.
FLH:14PI
|
PATIENT INFORMATION FLOVENT (FLO vent) HFA (fluticasone propionate inhalation aerosol) for oral inhalation use |
|
What is FLOVENT HFA? FLOVENT HFA is a prescription inhaled corticosteroid (ICS) medicine used for the long-term treatment of asthma in people aged 4 years and older.
|
|
Do not use FLOVENT HFA:
|
|
Before using FLOVENT HFA, tell your healthcare provider about all of your medical conditions, including if you:
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. FLOVENT HFA and certain other medicines may interact with each other. This may cause serious side effects. Especially tell your healthcare provider if you take antifungal or anti-HIV medicines. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine. |
|
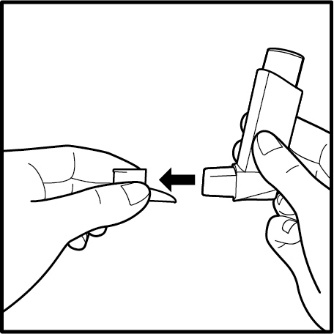
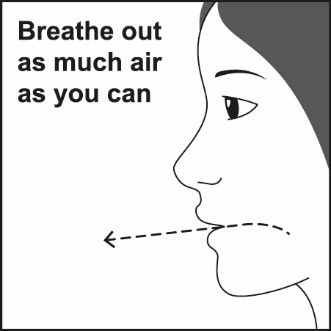
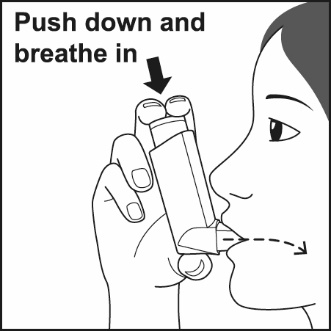
How should I use FLOVENT HFA? Read the step-by-step instructions for using FLOVENT HFA at the end of this Patient Information.
|
|
What are the possible side effects of FLOVENT HFA? FLOVENT HFA can cause serious side effects, including:
Common side effects of FLOVENT HFA include:
These are not all the possible side effects of FLOVENT HFA. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|
How should I store FLOVENT HFA?
Keep FLOVENT HFA and all medicines out of the reach of children. |
|
General information about the safe and effective use of FLOVENT HFA. Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use FLOVENT HFA for a condition for which it was not prescribed. Do not give FLOVENT HFA to other people, even if they have the same symptoms that you have. It may harm them. You can ask your healthcare provider or pharmacist for information about FLOVENT HFA that was written for health professionals. |
|
What are the ingredients in FLOVENT HFA? Active ingredient: fluticasone propionate Inactive ingredient: propellant HFA-134a For more information about FLOVENT HFA, call 1-888-825-5249. Trademarks are owned by or licensed to the GSK group of companies. GlaxoSmithKline, Durham, NC 27701 ©2023 GSK group of companies or its licensor. FLH:10PIL |
- This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: September 2023
PRINCIPAL DISPLAY PANEL
NDC 0173-0718-20
Flovent HFA
(fluticasone propionate inhalation aerosol)
44 mcg
For oral inhalation with FLOVENT HFA actuator only.
Attention Pharmacist: Detach Patient Information leaflet from package insert and dispense with inhaler.
See prescribing information for dosage information.
Rx only
Net Wt. 10.6 g
120 Metered Actuations
gsk
©2021 GSK group of companies or its licensor.
Made in Singapore
- 62000000062556 Rev. 5/21
PRINCIPAL DISPLAY PANEL
NDC 0173-0719-20
Flovent HFA
(fluticasone propionate inhalation aerosol)
110 mcg
For oral inhalation with FLOVENT HFA actuator only.
Attention Pharmacist: Detach Patient Information leaflet from package insert and dispense with inhaler.
See prescribing information for dosage information.
Rx only
Net Wt. 12 g
120 Metered Actuations
gsk
©2021 GSK group of companies or its licensor.
Made in Singapore
- 62000000062557 Rev. 5/21
PRINCIPAL DISPLAY PANEL
NDC 0173-0720-20
Flovent HFA
(fluticasone propionate inhalation aerosol)
220 mcg
For oral inhalation with FLOVENT HFA actuator only.
Attention Pharmacist: Detach Patient Information leaflet from package insert and dispense with inhaler.
See prescribing information for dosage information.
Rx only
Net Wt. 12 g
120 Metered Actuations
gsk
©2021 GSK group of companies or its licensor.
Made in Singapore
- 62000000062558 Rev. 5/21
| FLOVENT
HFA
fluticasone propionate aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| FLOVENT
HFA
fluticasone propionate aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| FLOVENT
HFA
fluticasone propionate aerosol, metered |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - GlaxoSmithKline LLC (167380711) |
Frequently asked questions
- What are the risks of using Flonase long-term?
- How often can you use Flonase nasal spray?
- How long does it take for Flonase to work?
- What's the difference between Xhance and Flonase Allergy Relief?
- Can I use fluticasone nasal spray to relieve stuffy nose due to a cold?
More about Flovent (fluticasone)
- Check interactions
- Compare alternatives
- Reviews (34)
- Side effects
- Dosage information
- During pregnancy
- Drug class: inhaled corticosteroids
Patient resources
Professional resources
Other brands
Arnuity Ellipta, ArmonAir Digihaler, ArmonAir RespiClick