Head Injury in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about a head injury?
A head injury can include your child's scalp, face, skull, or brain and range from mild to severe. Effects can appear immediately after the injury or develop later. The effects may last a short time or be permanent. Healthcare providers may want to check your child's recovery over time. Treatment may change as he or she recovers or develops new health problems from the head injury.
What are the signs and symptoms of a head injury?
- An open wound, swelling, or bruising
- Mild to moderate headache
- Dizziness or loss of balance
- Nausea or vomiting
- Ringing in the ears or neck pain
- Confusion, especially right after the injury
- Change in mood, such as feeling restless or irritable
- Trouble thinking, remembering, or concentrating
- Short-term loss of newly learned skills, such as toilet training
- Drowsiness or less energy than usual
- Change in how your child sleeps, such as sleeping more than usual or waking during the night
How is a head injury diagnosed?
- Your child's healthcare provider will ask about the injury and your child's symptoms. The provider may check how your child's pupils react to light. Your child's brain function, memory, hand grasp, and balance may also be checked.
- Your child may need a CT scan to check for bleeding or major damage to his or her skull or brain. Your child may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if your child has ever had an allergic reaction to contrast liquid.
How is a head injury treated?
A mild head injury may not need to be treated. Your child may be given medicine to decrease pain. A concussion, hematoma (collection of blood), or traumatic brain injury may need both immediate and long-term treatment.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Related medications
How can I manage my child's head injury?
- Have your child rest or do quiet activities for 24 hours or as directed. Limit TV, video games, computer time, and schoolwork. Do not let your child play sports or do activities that may cause a blow to the head. Your child should not return to sports until a healthcare provider says it is okay. Your child will need to return to sports slowly.
- Apply ice on your child's head for 15 to 20 minutes every hour as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it. Ice helps decrease swelling and pain.
- Watch your child for problems during the first 24 hours , or as directed. Call for help if needed. When your child is awake, ask questions every few hours to make sure he or she is thinking clearly. An example is to ask your child's name or favorite food.
- Tell your child's teachers, coaches, or daycare providers about the injury and symptoms to watch for. Ask for extra time to finish schoolwork or exams, if needed.
How can I help prevent another head injury?
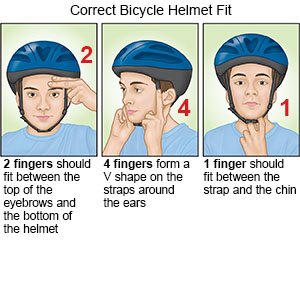
- Have your child wear a helmet that fits properly. Helmets help decrease your child's risk for a serious head injury. Your child should wear a helmet when he or she plays sports, or rides a bike, scooter, or skateboard. Talk to your child's healthcare provider about other ways you can protect your child during sports.
- Have your child wear a seat belt or sit in a child safety seat in the car. This decreases your child's risk for a head injury if he or she is in a car accident. Ask your child's healthcare provider for more information about child safety seats.

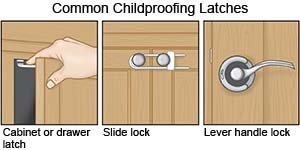
- Make your home safe for your child. Home safety measures can help prevent head injuries. Put self-latching gates at the bottoms and tops of stairs. Always make sure that the gate is closed and locked. Gates will help protect your child from falling and getting a head injury. Screw the gate to the wall at the tops of stairs. Put soft bumpers on furniture edges and corners. Secure heavy furniture, such as a dresser or bookcase, so your child cannot pull it over.
Call your local emergency number (911 in the US) for any of the following:
- You cannot wake your child.
- Your child has a seizure.
- Your child stops responding to you or faints.
- Your child has blurry or double vision.
- Your child's speech becomes slurred or confused.
- Your child has weakness, loss of feeling, or problems walking.
- Your child's pupils are larger than usual, or one pupil is a different size than the other.
- Your child has blood or clear fluid coming out of his or her ears or nose.
When should I seek immediate care?
- Your child's headache or dizziness gets worse or becomes severe.
- Your child has repeated or forceful vomiting.
- Your child is confused.
- Your child has a bulging soft spot on his or her head.
- Your child is harder to wake than usual.
When should I call my child's doctor?
- Your child will not stop crying or will not eat.
- Your child's symptoms last longer than 6 weeks after the injury.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Head Injury
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
