Muscular Dystrophy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is muscular dystrophy?
Muscular dystrophy (MD) is an inherited disease that causes muscle weakness and loss. There are several types, such as Duchenne and Becker muscular dystrophy, that affect muscles in different parts of your body. Muscle weakness may lead to difficulty walking. In some cases, it can also lead to difficulty eating, drinking, or breathing.
How is MD diagnosed?
- Blood tests are done to check for muscle damage and genetic markers of MD.
- An MRI takes pictures of your muscles to show if you have MD. You may be given contrast liquid to help the muscles show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- An electromyography measures the electrical activity of your muscles at rest and with movement.
- A muscle biopsy is a procedure to remove a small sample of muscle. Your healthcare provider will send the sample to a lab for tests.
How is MD treated?
There is no cure for MD. The goal of treatment is to help reduce your symptoms and maintain your strength. You may need to work with specialists to help with breathing, eating, and other functions affected by MD. You may need any of the following:
- Assistive devices , such as braces, crutches, or wheelchairs, help you move. They can also help protect and support your body to prevent injury.
- Medicines may be given to decrease pain and inflammation, or relax your muscles. Your healthcare provider may also recommend medicine to help other medical conditions that may result from MD.
- Physical, occupational, or speech, therapy are programs to help you learn how to take care of yourself. A physical therapist will teach you exercises to help improve movement and strength, and to decrease pain. An occupational therapist will teach you skills to help with your daily activities. A speech therapist will help you strengthen the muscles in your face that you use to speak.
- Respiratory therapy may be needed to help prevent or manage breathing problems. It may include the use of devices that help you breathe better.
- Early intervention and special education programs may be needed for children. These programs will help children grow, develop, and manage symptoms of MD.
- Surgery may be done to release tight muscles so it is easier for you to move.
Related medications
How can I manage my symptoms?
- Do breathing exercises as directed. Deep breathing can help you breathe more easily. Breathe out with pursed or puckered lips. Use your diaphragm to breathe. Put one hand on your abdomen and breathe in, causing your hand to move outward or upward. This helps make more room so your lungs can take in more air. Your healthcare provider may teach you or family members how to watch for signs of breathing problems.
- Learn safe ways to eat and swallow. Talk with your healthcare provider if you have trouble swallowing. He or she will show you safer ways to swallow and teach you which foods and liquids are safe to eat and drink. He or she may also recommend soft foods or thick liquids to make it easier to swallow. In some cases, you may receive nutrition through an IV or tube into your stomach.
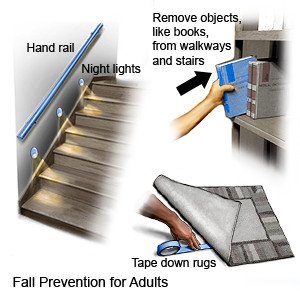
- Stay safe at home and when you walk. Use a 4-pronged cane or walker to help you keep your balance when you walk. Remove loose carpeting from the floor to reduce your risk for a fall. Use chairs with side arms and hard cushions to make it easier to get up or out of a chair. Put grab bars on the walls beside toilets and inside showers and bathtubs. These will help you get up and help prevent falls. You may want to put a shower chair inside the shower.
- Ask about vaccines. The flu and pneumonia vaccines may help reduce your risk for lung infections. Ask your healthcare provider when to get these shots.
- Maintain a healthy weight. A healthy weight may help prevent too much stress on your muscles. It may also decrease your risk for breathing problems. Exercise and a healthy eating plan can help you maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Also ask about an exercise program and eating plan that are right for you.
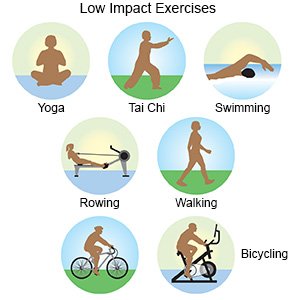
- Exercise as directed. You will need to work with an exercise specialist to prevent injury or muscle damage. Low-impact exercise, such as swimming, can help your heart and muscles work better and decrease tiredness. Your healthcare provider may also recommend strength training, such as weightlifting. Drink liquids before, during, and after exercise to prevent dehydration. Stop exercising if you have shortness of breath. Do not exercise again if you feel weaker after exercise, or your muscles are sore or heavy for up to 48 hours after exercise.
- Use a sleeping pad or mattress that can help you get a restful sleep. It may be difficult to find a comfortable position for sleep. Ask your healthcare provider what pad or mattress you can use to help you be more comfortable.
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have trouble breathing.
When should I call my doctor?
- You have a fever.
- You have difficulty having a bowel movement.
- You have more weakness than usual.
- You have trouble swallowing.
- You are depressed or feel you cannot cope with your MD.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Muscular Dystrophy
Treatment options
- Medications for Familial Periodic Paralysis
- Medications for Muscular Dystrophy
- Medications for Myopathy
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
