Chronic Myeloid Leukemia
Medically reviewed by Drugs.com. Last updated on Sep 1, 2024.
Chronic myeloid leukemia (CML) is also called chronic myelogenous leukemia. It is cancer of the bone marrow and blood cells. With CML, blood cells that should become white blood cells (WBCs) do not fully grow. These cells do not fight infection like a normal WBC should. They crowd the bone marrow and prevent normal blood cells from growing and fighting infection.
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
Drinking liquids:
Men 19 years or older should drink about 3 liters of liquid each day (about 13 eight-ounce cups). Women 19 years or older should drink about 2 liters of liquid each day (about 9 eight-ounce cups). It is especially important to drink enough liquids if you are vomiting from chemotherapy. Follow your healthcare provider's advice if you must change the amount of liquids you drink. For most people, healthy liquids to drink are water, juices, and milk. If you are used to drinking liquids that contain caffeine, such as coffee, these can also be counted in your daily liquid amount. Try to drink enough liquid each day, and not just when you feel thirsty. It may be helpful to drink liquids between your meals instead of with your meals.
A heart monitor
is also called an ECG or EKG. Sticky pads placed on your skin record your heart's electrical activity.
A pulse oximeter
is a device that measures the amount of oxygen in your blood. A cord with a clip or sticky strip is placed on your finger, ear, or toe. The other end of the cord is hooked to a machine.
Reverse isolation:
You may be put on reverse isolation safety measures if your body is having a hard time fighting infections. You are given a private room to protect you from other people's germs. Healthcare providers and visitors may wear gloves, a face mask, or a gown to keep their germs away from you. Everyone should wash their hands when entering and leaving your room.
Medicines:
You may be given medicines to treat problems caused by your CML. For example, you may be given antibiotics or other medicines to help your body fight infection. You may be given fever or pain medicine. You may take medicines to help you cope with chemotherapy side effects such as upset stomach or diarrhea.
Tests:
- Blood tests are used to count the number of each type of blood cell (RBCs, WBCs, platelets). The tests may also show the phase of CML that you have.
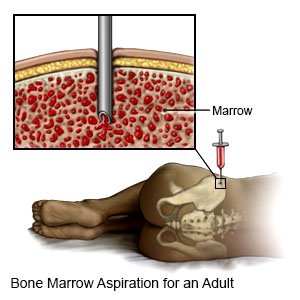
- A bone marrow biopsy is a procedure used to take a small amount of bone marrow from the bone in your hip. This test helps healthcare providers to learn which phase of CML you have.
Treatment:
- A blood transfusion replaces blood in your body to help it work properly. A blood transfusion is given through an IV. Blood is tested for safety before it is used.
- Medicines may be given to decrease the growth of CML cells and increase the growth of normal blood cells.
- Chemotherapy is used to kill cancer cells before a bone marrow stem cell transplant.
- A transplant is rarely used to replace your bone marrow or to give you stem cells. Stem cells are the part of the bone marrow that make or change into blood cells. The stem cells go into your bone marrow and become blood cells.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Venous access device:
An IV catheter or tube may be placed in a large vein (blood vessel) near your collarbone, in your neck, or in your arm. Some examples of these venous access devices are Hickman. Groshong, and PICC lines. You may also have a port, which is a type of venous access device that is placed under the skin and connected to a large vein. You may need a venous access device to receive chemotherapy, other medicines and fluids that need to be given through a big vein. A venous access device can stay in longer than a regular IV can. You may need this device to receive chemotherapy treatments.
RISKS:
- Chemotherapy and medicines used to treat CML may cause side effects such as nausea, vomiting, and diarrhea. You may feel very tired and have extra body fluid. You could have a bad reaction to a bone marrow transplant or stem cell transplant. You may get a blood clot in your leg or arm. This can cause pain and swelling, and it can stop blood from flowing where it needs to go in your body. The blood clot can break loose and travel to your lungs or brain. A blood clot in your lungs can cause chest pain and trouble breathing. A blood clot in your brain can cause a stroke. These problems can be life-threatening.
- Treatment of CML may be slow to work, or may not work at all. CML may not go away or it may get worse. If your CML goes into remission, it may return. CML may also spread to other parts of your body. If you do not have treatment, or the treatment does not work, you could die.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Chronic Myeloid Leukemia
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
