Sarafem Tablets Prescribing Information
Package insert / product label
Generic name: fluoxetine hydrochloride
Dosage form: tablet
Drug class: Selective serotonin reuptake inhibitors
Medically reviewed by Drugs.com. Last updated on Mar 25, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Drug Abuse and Dependence
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Storage and Handling
- Patient Counseling Information
- Medication Guide
Highlights of Prescribing Information
SARAFEM (fluoxetine hydrochloride tablets) for oral use
Initial U.S. Approval: 1987
WARNING: SUICIDALITY AND ANTIDEPRESSANT DRUGS
See full prescribing information for complete boxed warning.
Increased risk of suicidal thinking and behavior in children, adolescents, and young adults taking antidepressants for Major Depressive Disorder (MDD) and other psychiatric disorders. SARAFEM is not approved for use in pediatric patients (5.1).
Recent Major Changes
Warnings and Precautions (5.2) 01/2017
Indications and Usage for Sarafem Tablets
SARAFEM is a selective serotonin reuptake inhibitor (SSRI) indicated for the treatment of Premenstrual Dysphoric Disorder (PMDD) (1.1)
Sarafem Tablets Dosage and Administration
- 20 mg/day continuously or intermittently (2.1)
Dosage Forms and Strengths
- Tablets: 10 mg, 15 mg, 20 mg (3)
Contraindications
- Serotonin Syndrome and MAOIs: Do not use with MAOIs intended to treat psychiatric disorders with SARAFEM or within 5 weeks of stopping treatment with SARAFEM. Do not use SARAFEM within 14 days of stopping an MAIO intended to treat psychiatric disorders. In addition, do not start SARAFEM in a patient who is being treated with linezolid or intravenous methylene blue (4.1)
- Do not use with pimozide due to risk of drug interaction or QTc prolongation (4.2, 7.9)
- Do not use with thioridazine due to QTc interval prolongation or potential for elevated thioridazine plasma levels. Do not use thioridazine within 5 weeks of discontinuing SARAFEM (4.2, 7.9)
Warnings and Precautions
-
Clinical Worsening and Suicide Risk: Monitor for clinical worsening and suicidal thinking and behavior (5.1)
-
Serotonin Syndrome: Serotonin syndrome has been reported with SSRIs and SNRIs, including SARAFEM, both when taken alone, but especially when co-administered with other serotonergic agents (including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, tryptophan, buspirone, amphetamines, and St. John’s Wort). If such symptoms occur, discontinue SARAFEM and initiate supportive treatment. If concomitant use of SARAFEM with other serotonergic drugs is clinically warranted, patients should be made aware of a potential increased risk of serotonin syndrome, particularly during treatment initiation and dose increases (5.2)
-
Allergic Reactions and Rash: Discontinue upon appearance of rash or allergic phenomena (5.3)
-
Activation of Mania/Hypomania: Screen for Bipolar Disorder and monitor for mania/hypomania (5.4)
-
Seizures: Use cautiously in patients with a history of seizures or with conditions that potentially lower the seizure threshold (5.5)
-
Altered Appetite and Weight: Significant weight loss has occurred (5.6)
-
Abnormal Bleeding: May increase the risk of bleeding. Use with NSAIDs, aspirin, warfarin, or drugs that affect coagulation may potentiate the risk of gastrointestinal or other bleeding (5.7)
-
Angle-Closure Glaucoma: Angle closure glaucoma has occurred in patients who have untreated anatomically narrow angles and who are treated with antidepressants (5.8)
-
Hyponatremia: Has been reported with fluoxetine in association with syndrome of inappropriate antidiuretic hormone (SIADH) (5.9)
-
Anxiety and Insomnia: May occur (5.10)
-
Potential for Cognitive and Motor Impairment: Has potential to impair judgment, thinking, and motor skills. Use caution when operating machinery (5.12)
- Long Half-Life: Changes in dose will not be fully reflected in plasma for several weeks (5.13)
Adverse Reactions/Side Effects
Most common adverse reactions (incidence rate greater than or equal to 5% and greater than placebo) associated with SARAFEM 20 mg (either continuous or intermittent) for PMDD:
Headache, asthenia, pain, accidental injury, infection, flu syndrome, nausea, diarrhea, insomnia, dizziness, nervousness, thinking abnormal, libido decreased, rhinitis, and pharyngitis (6.1).
To report SUSPECTED ADVERSE REACTIONS, contact Allergan at 1-800-433-8871 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
Drug Interactions
-
Monoamine Oxidase Inhibitors (MAOI): Fluoxetine is contraindicated for use with MAOI’s, or within 14 days of discontinuing an MAOI due to risk of drug interaction. At least 5 weeks should be allowed after stopping fluoxetine before starting treatment with an MAOI (4, 7.1)
-
Pimozide: Fluoxetine is contraindicated for use with pimozide due to risk of drug interaction or QTc prolongation (4, 7.9)
-
Thioridazine: Fluoxetine is contraindicated for use with thioridazine due to QTc interval prolongation or potential for elevated thioridazine plasma levels. Do not use thioridazine within 5 weeks of discontinuing SARAFEM (4, 7.9)
-
Drugs Metabolized by CYP2D6: Fluoxetine is a potent inhibitor of CYP2D6 enzyme pathway (7.9)
-
Tricyclic Antidepressants (TCAs): Monitor TCA levels during coadministration with SARAFEM or when SARAFEM has been recently discontinued (7.9)
-
CNS Acting Drugs: Caution should be used when taken in combination with other centrally acting drugs (7.2)
-
Benzodiazepines: Diazepam – increased t½ , alprazolam - further psychomotor performance decrement due to increased levels (7.9)
-
Antipsychotics: Potential for elevation of haloperidol and clozapine levels (7.9)
-
Anticonvulsants: Potential for elevated phenytoin and carbamazepine levels and clinical anticonvulsant toxicity (7.9)
-
Serotonergic Drugs: Potential for Serotonin Syndrome (5.2, 7.3)
-
Triptans: There have been rare postmarketing reports of Serotonin Syndrome with use of an SSRI and a triptan (5.2, 7.4)
-
Tryptophan: Concomitant use with tryptophan is not recommended (5.2, 7.5)
-
Drugs that Interfere with Hemostasis (for example, NSAIDs, Aspirin, Warfarin): May potentiate the risk of bleeding (7.6)
- Drugs Tightly Bound to Plasma Proteins: May cause a shift in plasma concentrations (7.8, 7.9)
Use In Specific Populations
-
Pregnancy: PMDD does not exist during pregnancy. Fluoxetine should be used during pregnancy only if the potential benefit justifies the potential risks to the fetus (8.1)
-
Nursing Mothers: Breast feeding is not recommended (8.3)
- Hepatic Impairment: Lower or less frequent dosing may be appropriate in patients with cirrhosis (8.6)
See 17 for PATIENT COUNSELING INFORMATION, Medication Guide and Medication Guide.
Revised: 1/2017
Full Prescribing Information
WARNING: SUICIDALITY AND ANTIDEPRESSANT DRUGS
Antidepressants increased the risk compared to placebo of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults in short-term studies of Major Depressive Disorder (MDD) and other psychiatric disorders. Anyone considering the use of SARAFEM or any other antidepressant in a child, adolescent, or young adult must balance this risk with the clinical need. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction in risk with antidepressants compared to placebo in adults aged 65 and older. Depression and certain other psychiatric disorders are themselves associated with increases in the risk of suicide. Patients of all ages who are started on antidepressant therapy should be monitored appropriately and observed closely for clinical worsening, suicidality, or unusual changes in behavior. Families and caregivers should be advised of the need for close observation and communication with the prescriber. SARAFEM is not approved for use in pediatric patients [see Warnings and Precautions (5.1) and Use in Specific Populations (8.4)].
1. Indications and Usage for Sarafem Tablets
1.1 Premenstrual Dysphoric Disorder (PMDD)
SARAFEM is indicated for the treatment of premenstrual dysphoric disorder (PMDD) [see Clinical Studies (14.1)].
The effectiveness of SARAFEM in long-term use (that is, for more than 6 months) has not been systematically evaluated in placebo-controlled trials. The use of SARAFEM for extended periods should be periodically re-evaluated for the individual patient [see Dosage and Administration (2.1)].
2. Sarafem Tablets Dosage and Administration
2.1 Treatment
The recommended dose of SARAFEM for the treatment of PMDD is 20 mg/day given continuously (every day of the menstrual cycle) or intermittently (defined as starting a daily dose 14 days prior to the anticipated onset of menstruation through the first full day of menses and repeating with each new cycle). The dosing regimen should be based on individual patient characteristics. In a study comparing continuous dosing of fluoxetine 20 and 60 mg/day to placebo, both doses were proven to be effective, but there was no statistically significant added benefit for the 60 mg/day compared with the 20 mg/day dose. Fluoxetine doses above 60 mg/day have not been systematically studied in patients with PMDD. The maximum fluoxetine dose should not exceed 80 mg/day [see Clinical Studies (14.1)].
Systematic evaluation of SARAFEM has shown that its efficacy in PMDD is maintained for periods of up to 6 months at a dose of 20 mg/day given continuously and up to 3 months at a dose of 20 mg/day given intermittently [see Clinical Studies (14.1)]. Patients should be periodically re-assessed to determine the need for continued treatment.
2.2 Dosing in Specific Populations
Treatment of Pregnant Women — PMDD does not exist in pregnancy. However, if there is a need to treat pregnant women with fluoxetine, the physician should carefully consider the potential risks and potential benefits of treatment. Neonates exposed to SSRIs or SNRIs late in the third trimester have developed complications requiring prolonged hospitalization, respiratory support, and tube feeding [see Use in Specific Populations (8.1)].
Hepatic Impairment — A lower or less frequent dosage should be used in patients with hepatic impairment [see Clinical Pharmacology (12.3) and Use in Specific Populations (8.6)].
Concomitant Illness — Patients with concurrent disease or on multiple concomitant medications may require dosage adjustments [see Warnings and Precautions (5.11) and Clinical Pharmacology (12.3)].
2.3 Discontinuation of Treatment
Symptoms associated with discontinuation of fluoxetine, SNRIs, and SSRIs, have been reported [see Warnings and Precautions (5.14)].
2.4 Switching a Patient To or From a Monoamine Oxidase Inhibitor (MAOI) Intended to Treat Psychiatric Disorders
At least 14 days should elapse between discontinuation of an MAOI intended to treat psychiatric disorders and initiation of therapy with SARAFEM. Conversely, at least 5 weeks should be allowed after stopping SARAFEM before starting an MAOI intended to treat psychiatric disorders [see Contraindications (4.1)].
2.5 Use of SARAFEM with Other MAOIs such as Linezolid or Methylene Blue
Do not start SARAFEM in a patient who is being treated with linezolid or intravenous methylene blue because there is an increased risk of serotonin syndrome. In a patient who requires more urgent treatment of a psychiatric condition, other interventions, including hospitalization, should be considered [see Contraindications (4.1)].
In some cases, a patient already receiving SARAFEM therapy may require urgent treatment with linezolid or intravenous methylene blue. If acceptable alternatives to linezolid or intravenous methylene blue treatment are not available and the potential benefits of linezolid or intravenous methylene blue treatment are judged to outweigh the risks of serotonin syndrome in a particular patient, SARAFEM should be stopped promptly, and linezolid or intravenous methylene blue can be administered. The patient should be monitored for symptoms of serotonin syndrome for five weeks or until 24 hours after the last dose of linezolid or intravenous methylene blue, whichever comes first. Therapy with SARAFEM may be resumed 24 hours after the last dose of linezolid or intravenous methylene blue [see Warnings and Precautions (5.2)].
The risk of administering methylene blue by non-intravenous routes (such as oral tablets or by local injection) or in intravenous doses much lower than 1 mg/kg with SARAFEM is unclear. The clinician should, nevertheless, be aware of the possibility of emergent symptoms of serotonin syndrome with such use [see Warnings and Precautions (5.2)].
3. Dosage Forms and Strengths
• 10 mg tablet is a cream, round tablet embossed with S10 on one side.
• 15 mg tablet is a white, round tablet embossed with S15 on one side.
• 20 mg tablet is a yellow, round tablet embossed with S20 on one side.
4. Contraindications
4.1 Monoamine Oxidase Inhibitors
The use of MAOIs intended to treat psychiatric disorders with SARAFEM or within 5 weeks of stopping treatment with SARAFEM is contraindicated because of an increased risk of serotonin syndrome. The use of SARAFEM within 14 days of stopping an MAOI intended to treat psychiatric disorders is also contraindicated [see Dosage and Administration (2.4) and Warnings and Precautions (5.2)].
Starting SARAFEM in a patient who is being treated with MAOIs such as linezolid or intravenous methylene blue is also contraindicated because of an increased risk of serotonin syndrome [see Dosage and Administration (2.5) and Warnings and Precautions (5.2)].
4.2 Other Contraindications
The use of SARAFEM is contraindicated with the following:
• Pimozide [see Drug Interactions (7.9)]
• Thioridazine [see Drug Interactions (7.9)]
5. Warnings and Precautions
5.1 Clinical Worsening and Suicide Risk
Patients with Major Depressive Disorder (MDD), both adult and pediatric, may experience worsening of their depression and/or the emergence of suicidal ideation and behavior (suicidality) or unusual changes in behavior, whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. Suicide is a known risk of depression and certain other psychiatric disorders, and these disorders themselves are the strongest predictors of suicide. There has been a long-standing concern, however, that antidepressants may have a role in inducing worsening of depression and the emergence of suicidality in certain patients during the early phases of treatment. Pooled analyses of short-term placebo-controlled trials of antidepressant drugs (SSRIs and others) showed that these drugs increase the risk of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults (ages 18 to 24) with Major Depressive Disorder (MDD) and other psychiatric disorders. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction with antidepressants compared to placebo in adults aged 65 and older.
The pooled analyses of placebo-controlled trials in children and adolescents with MDD, Obsessive Compulsive Disorder (OCD), or other psychiatric disorders included a total of 24 short-term trials of 9 antidepressant drugs in over 4400 patients. The pooled analyses of placebo-controlled trials in adults with MDD or other psychiatric disorders included a total of 295 short-term trials (median duration of 2 months) of 11 antidepressant drugs in over 77,000 patients. There was considerable variation in risk of suicidality among drugs, but a tendency toward an increase in the younger patients for almost all drugs studied. There were differences in absolute risk of suicidality across the different indications, with the highest incidence in MDD. The risk differences (drug versus placebo), however, were relatively stable within age strata and across indications. These risk differences (drug-placebo difference in the number of cases of suicidality per 1000 patients treated) are provided in Table 1.
| Age Range | Drug-Placebo Difference in Number of
Cases of Suicidality per 1000 Patients Treated |
| Increases Compared to Placebo | |
| <18 | 14 additional cases |
| 18-24 | 5 additional cases |
| Decreases Compared to Placebo | |
| 25-64 | 1 fewer case |
| ≥65 | 6 fewer cases |
No suicides occurred in any of the pediatric trials. There were suicides in the adult trials, but the number was not sufficient to reach any conclusion about drug effect on suicide.
It is unknown whether the suicidality risk extends to longer-term use, that is, beyond several months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with depression that the use of antidepressants can delay the recurrence of depression.
All patients being treated with antidepressants for any indication should be monitored appropriately and observed closely for clinical worsening, suicidality, and unusual changes in behavior, especially during the initial few months of a course of drug therapy, or at times of dose changes, either increases or decreases.
The following symptoms, anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, and mania, have been reported in adult and pediatric patients being treated with antidepressants for Major Depressive Disorder as well as for other indications, both psychiatric and nonpsychiatric. Although a causal link between the emergence of such symptoms and either the worsening of depression and/or the emergence of suicidal impulses has not been established, there is concern that such symptoms may represent precursors to emerging suicidality.
Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse, or who are experiencing emergent suicidality or symptoms that might be precursors to worsening depression or suicidality, especially if these symptoms are severe, abrupt in onset, or were not part of the patient’s presenting symptoms.
If the decision has been made to discontinue treatment, medication should be tapered, as rapidly as is feasible, but with recognition that abrupt discontinuation can be associated with certain symptoms [see Warnings and Precautions (5.14)].
Families and caregivers of patients being treated with antidepressants for Major Depressive Disorder or other indications, both psychiatric and nonpsychiatric, should be alerted about the need to monitor patients for the emergence of agitation, irritability, unusual changes in behavior, and the other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to health care providers. Such monitoring should include daily observation by families and caregivers. Prescriptions for SARAFEM should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
It should be noted that SARAFEM is not approved for treating any indication in the pediatric population.
5.2 Serotonin Syndrome
The development of a potentially life-threatening serotonin syndrome has been reported with SNRIs and SSRIs, including SARAFEM, alone but particularly with concomitant use of other serotonergic drugs (including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, tryptophan, buspirone, amphetamines, and St. John’s Wort) and with drugs that impair metabolism of serotonin (in particular, MAOIs, both those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue).
Serotonin syndrome symptoms may include mental status changes (for example, agitation, hallucinations, delirium, and coma), autonomic instability (for example, tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (for example, tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and/or gastrointestinal symptoms (for example, nausea, vomiting, diarrhea). Patients should be monitored for the emergence of serotonin syndrome.
The concomitant use of SARAFEM with MAOIs intended to treat psychiatric disorders is contraindicated. SARAFEM should also not be started in a patient who is being treated with MAOIs such as linezolid or intravenous methylene blue. All reports with methylene blue that provided information on the route of administration involved intravenous administration in the dose range of 1mg/kg to 8 mg/kg. No reports involved the administration of methylene blue by other routes (such as oral tablets or local tissue injection) or at lower doses. There may be circumstances when it is necessary to initiate treatment with an MAOI such as linezolid or intravenous methylene blue in a patient taking SARAFEM. SARAFEM should be discontinued before initiating treatment with the MAOI [see Contraindications (4.1) and Dosage and Administration (2.5)].
If concomitant use of SARAFEM with other serotonergic drugs, that is, triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, buspirone, amphetamines, tryptophan and St. John’s Wort is clinically warranted, patients should be made aware of a potential increased risk for serotonin syndrome, particularly during treatment initiation and dose increases.
Treatment with SARAFEM and any concomitant serotonergic agents, should be discontinued immediately if the above events occur and supportive symptomatic treatment should be initiated.
5.3 Allergic Reactions and Rash
In 4 clinical trials for PMDD, 4% of 415 patients treated with SARAFEM reported rash and/or urticaria. None of these cases were classified as serious and 2 of 415 patients (both receiving 60 mg) were withdrawn from treatment because of rash and/or urticaria.
In US fluoxetine clinical trials for conditions other than PMDD, 7% of 10,782 patients developed various types of rashes and/or urticaria. Among the cases of rash and/or urticaria reported in premarketing clinical trials, almost a third were withdrawn from treatment because of the rash and/or systemic signs or symptoms associated with the rash. Clinical findings reported in association with rash include fever, leukocytosis, arthralgias, edema, carpal tunnel syndrome, respiratory distress, lymphadenopathy, proteinuria, and mild transaminase elevation. Most patients improved promptly with discontinuation of fluoxetine and/or adjunctive treatment with antihistamines or steroids, and all patients experiencing these reactions were reported to recover completely.
In premarketing clinical trials for conditions other than PMDD, 2 patients are known to have developed a serious cutaneous systemic illness. In neither patient was there an unequivocal diagnosis, but one was considered to have a leukocytoclastic vasculitis, and the other, a severe desquamating syndrome that was considered variously to be a vasculitis or erythema multiforme. Other patients have had systemic syndromes suggestive of serum sickness.
Since the introduction of fluoxetine, systemic reactions, possibly related to vasculitis and including lupus-like syndrome, have developed in patients with rash. Although these reactions are rare, they may be serious, involving the lung, kidney, or liver. Death has been reported to occur in association with these systemic reactions.
Anaphylactoid reactions, including bronchospasm, angioedema, laryngospasm, and urticaria alone and in combination, have been reported.
Pulmonary reactions, including inflammatory processes of varying histopathology and/or fibrosis, have been reported rarely. These reactions have occurred with dyspnea as the only preceding symptom.
Whether these systemic reactions and rash have a common underlying cause or are due to different etiologies or pathogenic processes is not known. Furthermore, a specific underlying immunologic basis for these reactions has not been identified. Upon the appearance of rash or of other possibly allergic phenomena for which an alternative etiology cannot be identified, SARAFEM should be discontinued.
5.4 Screening Patients for Bipolar Disorder and Monitoring for Mania/Hypomania
A major depressive episode may be the initial presentation of Bipolar Disorder. It is generally believed (though not established in controlled trials) that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk for Bipolar Disorder. Whether any of the symptoms described for clinical worsening and suicide risk represent such a conversion is unknown. However, prior to initiating treatment with an antidepressant, patients with depressive symptoms should be adequately screened to determine if they are at risk for Bipolar Disorder; such screening should include a detailed psychiatric history, including a family history of suicide, Bipolar Disorder, and depression. It should be noted that SARAFEM is not indicated for the treatment of depressive episodes associated with Bipolar I Disorder.
No patients treated with SARAFEM in 4 PMDD clinical trials (N = 415) reported mania/hypomania. In all US fluoxetine clinical trials for conditions other than PMDD, 0.7% of 10,782 patients reported mania/hypomania. Activation of mania/hypomania may occur with medications used to treat depression, especially in patients predisposed to Bipolar I Disorder.
5.5 Seizures
No patients treated with SARAFEM in 4 PMDD clinical trials (N = 415) reported seizures. In all US fluoxetine clinical trials for conditions other than PMDD, 0.2% of 10,782 patients reported convulsions. SARAFEM should be introduced with care in patients with a history of seizures.
5.6 Altered Appetite and Weight
In 2 placebo-controlled clinical trials for PMDD, patients treated with SARAFEM reported changes in appetite and weight [see Table 2]. For individual rates for SARAFEM 20 mg given as continuous and intermittent dosing, see Table 4 and accompanying footnote [see Adverse Reactions (6.1)].
| Percentage of Patients Reporting Adverse Reaction | |||
| Treatment Emergent
Adverse Reaction | 20 mg (continuous and
intermittent pooled) | 60 mg (continuous) | Placebo (pooled) |
| Anorexia (decreased appetite) | 4% | 13% | 2% |
| Weight Loss (>7%) | 7% | 12% | 3% |
| Weight Gain (>7%) | 8% | 6% | 1% |
In US placebo-controlled clinical trials of fluoxetine for other approved indications, changes in appetite and weight have also been reported [see Adverse Reactions (6.1) Table 5].
5.7 Abnormal Bleeding
SNRIs and SSRIs, including fluoxetine, may increase the risk of bleeding reactions. Concomitant use of aspirin, nonsteroidal anti-inflammatory drugs, warfarin, and other anti-coagulants may add to this risk. Case reports and epidemiological studies (case-control and cohort design) have demonstrated an association between use of drugs that interfere with serotonin reuptake and the occurrence of gastrointestinal bleeding. Bleeding reactions related to SNRIs and SSRIs use have ranged from ecchymoses, hematomas, epistaxis, and petechiae to life-threatening hemorrhages.
Patients should be cautioned about the risk of bleeding associated with the concomitant use of fluoxetine and NSAIDs, aspirin, warfarin, or other drugs that affect coagulation [see Drug Interactions (7.6)].
5.8 Angle-Closure Glaucoma
The pupillary dilation that occurs following use of many antidepressants and SARAFEM may trigger an angle closure attack in a patient with anatomically narrow angles who does not have a patent iridectomy.
5.9 Hyponatremia
Hyponatremia has been reported during treatment with SNRIs and SSRIs, including fluoxetine. In many cases, this hyponatremia appears to be the result of the syndrome of inappropriate antidiuretic hormone secretion (SIADH). Cases with serum sodium lower than 110 mmol/L have been reported and appeared to be reversible when fluoxetine was discontinued. Elderly patients may be at greater risk of developing hyponatremia with SNRIs and SSRIs. Also, patients taking diuretics or who are otherwise volume depleted may be at greater risk [see Use in Specific Populations (8.5)]. Discontinuation of SARAFEM should be considered in patients with symptomatic hyponatremia and appropriate medical intervention should be instituted.
Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which may lead to falls. More severe and/or acute cases have been associated with hallucination, syncope, seizure, coma, respiratory arrest, and death.
5.10 Anxiety and Insomnia
In 2 placebo-controlled clinical trials for PMDD, patients treated with SARAFEM reported anxiety, nervousness, and insomnia [see Table 3].
For individual rates of anxiety, nervousness, and insomnia with SARAFEM 20 mg given as continuous or intermittent dosing, see Table 5 and accompanying footnote [see Adverse Reactions (6.1)].
| Percentage of Patients Reporting Adverse Reaction | |||
| Treatment
Emergent Adverse Reaction | 20 mg (continuous
and intermittent pooled) | 60 mg (continuous) | Placebo (pooled) |
| Anxiety | 3% | 9% | 4% |
| Nervousness | 5% | 9% | 3% |
| Insomnia | 9% | 26% | 7% |
Anxiety, nervousness, and insomnia were associated with discontinuation for SARAFEM [see Table 4 and Warnings and Precautions (5.14)].
| Percentage of Patient Discontinuation due to Adverse Reaction | |||
| Treatment
Emergent Adverse Reaction | 20 mg (continuous
and intermittent pooled) | 60 mg (continuous) | Placebo (pooled) |
| Anxiety | 0% | 6% | 1% |
| Nervousness | 1% | 0% | 0.5% |
| Insomnia | 1% | 4% | 0.5% |
In US placebo-controlled clinical trials of fluoxetine for other approved indications, anxiety, nervousness, and insomnia have been among the most commonly reported adverse reactions [see Table 6 and Adverse Reactions (6.1)].
5.11 Use in Patients with Concomitant Illness
Clinical experience with fluoxetine in patients with concomitant systemic illness is limited. Caution is advisable in using fluoxetine in patients with diseases or conditions that could affect metabolism or hemodynamic responses.
Cardiovascular — Fluoxetine has not been evaluated or used to any appreciable extent in patients with a recent history of myocardial infarction or unstable heart disease. Patients with these diagnoses were systematically excluded from clinical studies during the product’s premarket testing. However, the electrocardiograms of 312 patients who received fluoxetine in double-blind trials, for a condition other than PMDD, were retrospectively evaluated; no conduction abnormalities that resulted in heart block were observed. The mean heart rate was reduced by approximately 3 beats/min.
Glycemic Control — In patients with diabetes, fluoxetine may alter glycemic control. Hypoglycemia has occurred during therapy with fluoxetine, and hyperglycemia has developed following discontinuation of the drug. As is true with many other types of medication when taken concurrently by patients with diabetes, insulin and/or oral hypoglycemic, dosage may need to be adjusted when therapy with fluoxetine is instituted or discontinued.
5.12 Potential for Cognitive and Motor Impairment
SARAFEM has the potential to impair judgment, thinking, or motor skills. Patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that the drug treatment does not affect them adversely.
5.13 Long Elimination Half-Life
Because of the long elimination half-lives of the parent drug and its major active metabolite, changes in dose will not be fully reflected in plasma for several weeks, affecting both strategies for titration to final dose and withdrawal from treatment. This is of potential consequence when drug discontinuation is required or when drugs are prescribed that might interact with fluoxetine and norfluoxetine following the discontinuation of fluoxetine [see Clinical Pharmacology (12.3) and Drug Interactions (7)].
5.14 Discontinuation of Treatment
During marketing of SARAFEM, SNRIs, and SSRIs, there have been spontaneous reports of adverse reactions occurring upon discontinuation of these drugs, particularly when abrupt, including the following: dysphoric mood, irritability, agitation, dizziness, sensory disturbances (for example, paresthesias such as electric shock sensations), anxiety, confusion, headache, lethargy, emotional lability, insomnia, and hypomania. While these reactions are generally self-limiting, there have been reports of serious discontinuation symptoms.
Patients should be monitored for these symptoms when discontinuing treatment with SARAFEM. A gradual reduction in the dose rather than abrupt cessation is recommended whenever possible. If intolerable symptoms occur following a decrease in the dose or upon discontinuation of treatment, then resuming the previously prescribed dose may be considered. Subsequently, the dose may continue to be decreased but at a more gradual rate. Plasma fluoxetine and norfluoxetine concentration decrease gradually at the conclusion of therapy which may minimize the risk of discontinuation symptoms with this drug.
6. Adverse Reactions/Side Effects
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect or predict the rates observed in practice.
Multiple doses of fluoxetine have been administered to 10,782 patients with various diagnoses in US clinical trials. Adverse reactions were recorded by clinical investigators using descriptive terminology of their own choosing. Consequently, it is not possible to provide a meaningful estimate of the proportion of individuals experiencing adverse reactions without first grouping similar types of reactions into a limited (that is, reduced) number of standardized reaction categories.
In the tables and tabulations that follow, COSTART Dictionary terminology has been used to classify reported adverse reactions. The stated frequencies represent the proportion of individuals who experienced, at least once, a treatment-emergent adverse reaction of the type listed. A reaction was considered treatment-emergent if it occurred for the first time or worsened while receiving therapy following baseline evaluation. It is important to emphasize that reactions reported during therapy were not necessarily caused by it.
The prescriber should be aware that the figures in the tables and tabulations cannot be used to predict the incidence of side effects in the course of usual medical practice where patient characteristics and other factors differ from those that prevailed in the clinical trials. Similarly, the cited frequencies cannot be compared with figures obtained from other clinical investigations involving different treatments, uses, and investigators. The cited figures, however, do provide the prescribing physician with some basis for estimating the relative contribution of drug and nondrug factors to the side effect incidence rate in the population studied.
Incidence in placebo-controlled PMDD clinical trials — In 1 of 3 placebo-controlled, continuous-dosing trials and 1 placebo-controlled, intermittent-dosing trial of fluoxetine in PMDD, treatment-emergent adverse reactions reporting rates were assessed. The information contained in Table 5 enumerates the most common treatment-emergent adverse reactions associated with the use of SARAFEM 20 mg (incidence of at least 5% for SARAFEM 20 mg and greater than placebo) for the treatment of PMDD and is based on data from the continuous-dosing trial at the recommended dose of SARAFEM (SARAFEM 20 mg, N = 104; placebo, N = 108) and data from the intermittent-dosing trial of fluoxetine in PMDD (SARAFEM 20 mg, N = 86; placebo, N = 88).
| Percentage of Patients Reporting Adverse Reaction | |||
| Body System/Adverse Reaction1 | SARAFEM
20 mg/day Continuously (N = 104) | SARAFEM
20 mg/day Intermittently (N = 86) | Placebo
(Pooled) (N = 196) |
| Body as a Whole | |||
| Headache | 13 | 15 | 11 |
| Asthenia | 12 | 8 | 4 |
| Pain | 9 | 3 | 7 |
| Accidental injury | 8 | 1 | 5 |
| Infection | 7 | 0 | 3 |
| Flu syndrome | 12 | 3 | 7 |
| Digestive System | |||
| Nausea | 13 | 9 | 6 |
| Diarrhea | 6 | 2 | 6 |
| Nervous System | |||
| Insomnia | 9 | 10 | 7 |
| Dizziness | 7 | 2 | 3 |
| Nervousness | 7 | 3 | 3 |
| Thinking abnormal2 | 6 | 5 | 0 |
| Libido decreased | 3 | 9 | 1 |
| Respiratory System | |||
| Rhinitis | 23 | 16 | 15 |
| Pharyngitis | 10 | 6 | 5 |
1 Included in the table are adverse reactions reported by at least 5% of patients taking SARAFEM 20 mg either continuously or intermittently. For additional adverse reaction terms referenced in Warnings and Precautions, reporting rates for SARAFEM 20 mg continuous and intermittent were, respectively: anxiety 4.8%, 1.2% and anorexia 3.8%, 3.5%.
2 Thinking abnormal is the COSTART term that captures concentration difficulties.
Incidence in US depression, OCD, and bulimia placebo-controlled clinical trials (excluding data from extensions of trials) — Table 6 enumerates the most common treatment-emergent adverse reactions associated with the use of fluoxetine up to 80 mg (incidence of at least 2% for fluoxetine and greater than placebo) in female patients ages 18 to 45 years from US placebo-controlled clinical trials in the treatment of depression, OCD, and bulimia.
| Percentage of Patients Reporting Adverse Reaction | ||
| Body System/Adverse Reaction1 | Fluoxetine (N = 1145) | Placebo (N = 553) |
| Body as a Whole | ||
| Headache | 24 | 21 |
| Asthenia | 14 | 6 |
| Flu syndrome | 7 | 3 |
| Abdominal pain | 6 | 5 |
| Accidental injury | 4 | 3 |
| Fever | 3 | 2 |
| Cardiovascular System | ||
| Palpitation | 3 | 2 |
| Vasodilatation | 3 | 1 |
| Digestive System | ||
| Nausea | 27 | 11 |
| Anorexia | 11 | 4 |
| Dry mouth | 11 | 8 |
| Diarrhea | 10 | 7 |
| Dyspepsia | 7 | 5 |
| Constipation | 5 | 3 |
| Vomiting | 3 | 2 |
| Metabolic and Nutritional
Disorders | ||
| Weight loss | 3 | 1 |
| Nervous System | ||
| Insomnia | 24 | 11 |
| Nervousness | 14 | 10 |
| Anxiety | 13 | 9 |
| Somnolence | 13 | 6 |
| Tremor | 12 | 1 |
| Dizziness | 11 | 5 |
| Libido decreased | 4 | 1 |
| Abnormal dreams | 3 | 2 |
| Thinking abnormal2 | 3 | 2 |
| Respiratory System | ||
| Pharyngitis | 6 | 5 |
| Yawn | 5 | -- |
| Skin and Appendages Skin and
Subcutaneous Tissue Disorders | ||
| Sweating | 8 | 3 |
| Rash | 5 | 3 |
| Special Senses | ||
| Abnormal vision | 3 | 1 |
| Urogenital System | ||
| Urinary frequency | 2 | 1 |
1 Included are reactions reported by at least 2% of patients taking fluoxetine, except the following adverse reactions, which had an incidence on placebo greater than fluoxetine (depression, OCD, and bulimia combined): back pain, cough increased, depression (includes suicidal thoughts), dysmenorrhea, flatulence, infection, myalgia, pain, pruritus, rhinitis, sinusitis.
2 Thinking abnormal is the COSTART term that captures concentration difficulties.
Incidence less than 0.5%.
Adverse reactions associated with discontinuation in two placebo-controlled PMDD clinical trials — In a continuous-dosing PMDD placebo-controlled trial, the most common adverse reaction (incidence at least 2% for SARAFEM 20 mg and greater than placebo) associated with discontinuation was nausea (3% for SARAFEM 20 mg, N = 104 and 1% for placebo, N = 108). In an intermittent-dosing placebo-controlled trial, no reactions associated with discontinuation reached an incidence of 2% for SARAFEM 20 mg. In these clinical trials, more than one reaction may have been recorded as the cause of discontinuation.
Adverse reactions associated with discontinuation in depression, OCD, and bulimia placebo-controlled US clinical trials (excluding data from extensions of trials) — In female patients age 18 to 45 years in US depression, OCD, and bulimia placebo-controlled clinical trials combined, which collected a single primary reaction associated with discontinuation (incidence at least 1% for fluoxetine and at least twice that for placebo), insomnia (1%, N = 561) was the only reaction reported.
Female sexual dysfunction with SSRIs — Although changes in sexual desire, sexual performance, and sexual satisfaction often occur as manifestations of a mood-related disorder, they may also be a consequence of pharmacologic treatment. In particular, some evidence suggests that SSRIs can cause such untoward sexual experiences. Reliable estimates of the incidence and severity of untoward experiences involving sexual desire, performance, and satisfaction are difficult to obtain, however, in part because patients and physicians may be reluctant to discuss them. Accordingly, estimates of the incidence of untoward sexual experience and performance, cited in product labeling, are likely to underestimate their actual incidence. For example, in women (age 18 to 45) receiving fluoxetine for indications other than PMDD, decreased libido was seen at an incidence of 4% for fluoxetine compared with 1% for placebo. There have been spontaneous reports in women (age 18 to 45) taking fluoxetine for indications other than PMDD of orgasmic dysfunction, including anorgasmia.
There are no adequate and well-controlled studies examining sexual dysfunction with fluoxetine treatment. While it is difficult to know the precise risk of sexual dysfunction associated with the use of SSRIs, physicians should routinely inquire about such possible side effects.
6.2 Other Reactions
Following is a list of all treatment-emergent adverse reactions reported at anytime by females and males taking fluoxetine in all US clinical trials for conditions other than PMDD as of May 8, 1995 (10,782 patients) except (1) those listed in the body or footnotes of Tables 1 or 5 above or elsewhere in labeling; (2) those for which the COSTART terms were uninformative or misleading; (3) those adverse reactions for which a causal relationship to fluoxetine use was considered remote; (4) adverse reactions occurring in only 1 patient treated with fluoxetine and which did not have a substantial probability of being acutely life-threatening; and (5) adverse reactions that could only occur in males.
Adverse reactions are classified within body system categories using the following definitions: frequent adverse reactions are defined as those occurring on one or more occasions in at least 1/100 patients; infrequent adverse reactions are those occurring in 1/100 to 1/1000 patients; rare adverse reactions are those occurring in less than 1/1000 patients.
Body as a Whole — Frequent: chest pain and chills; Infrequent: face edema, intentional overdose, malaise, pelvic pain, suicide attempt; Rare: acute abdominal syndrome, hypothermia, intentional injury, photosensitivity reaction.
Cardiovascular System — Frequent: hypertension; Infrequent: angina pectoris, arrhythmia, congestive heart failure, hypotension, migraine, myocardial infarct, postural hypotension, syncope, vascular headache; Rare: bradycardia, cerebral embolism, cerebral ischemia, extrasystoles, heart block, pallor, peripheral vascular disorder, phlebitis, shock, thrombophlebitis, thrombosis, vasospasm, ventricular arrhythmia, ventricular extrasystoles, ventricular fibrillation.
Digestive System — Frequent: increased appetite; Infrequent: aphthous stomatitis, cholelithiasis, colitis, dysphagia, eructation, esophagitis, gastritis, gastroenteritis, glossitis, gum hemorrhage, hyperchlorhydria, increased salivation, liver function tests abnormal, melena, mouth ulceration, stomach ulcer, stomatitis, thirst; Rare: biliary pain, bloody diarrhea, cholecystitis, duodenal ulcer, enteritis, esophageal ulcer, fecal incontinence, hepatitis, intestinal obstruction, liver fatty deposit, pancreatitis, peptic ulcer, salivary gland enlargement, tongue edema.
Endocrine System — Infrequent: hypothyroidism; Rare: diabetic acidosis, diabetes mellitus.
Hemic and Lymphatic System — Infrequent: anemia, ecchymosis; Rare: blood dyscrasia, hypochromic anemia, leukopenia, lymphedema, lymphocytosis, petechia, purpura, thrombocythemia.
Metabolic and Nutritional —Infrequent: dehydration, generalized edema, gout, hypercholesteremia, hyperlipemia, hypokalemia, peripheral edema; Rare: alcohol intolerance, alkaline phosphatase increased, BUN increased, creatine phosphokinase increased, hyperkalemia, hyperuricemia, hypocalcemia, iron deficiency anemia, SGPT increased.
Musculoskeletal System — Infrequent: arthritis, bone pain, bursitis, leg cramps, tenosynovitis; Rare: arthrosis, chondrodystrophy, myasthenia, myopathy, myositis, osteomyelitis, osteoporosis, rheumatoid arthritis.
Nervous System — Frequent: amnesia, emotional lability, paresthesia, and sleep disorder; Infrequent: abnormal gait, acute brain syndrome, akathisia, apathy, ataxia, buccoglossal syndrome, CNS depression, CNS stimulation, depersonalization, euphoria, hostility, hyperkinesia, hypertonia, hypesthesia, incoordination, libido increased, myoclonus, neuralgia, neuropathy, neurosis, paranoid reaction, personality disorder1, psychosis, vertigo; Rare: abnormal electroencephalogram, antisocial reaction, circumoral paresthesia, delusions, dysarthria, dystonia, extrapyramidal syndrome, foot drop, hyperesthesia, neuritis, paralysis, reflexes decreased, stupor.
Respiratory System — Infrequent: asthma, epistaxis, hiccup, hyperventilation; Rare: apnea, atelectasis, cough decreased, emphysema, hemoptysis, hypoventilation, hypoxia, larynx edema, lung edema, pneumothorax, stridor.
Skin and Appendages — Infrequent: acne, alopecia, contact dermatitis, eczema, maculopapular rash, skin discoloration, skin ulcer; Rare: furunculosis, herpes zoster, hirsutism, psoriasis, purpuric rash, seborrhea.
Special Senses — Frequent: ear pain, taste perversion, tinnitus; Infrequent: conjunctivitis, dry eyes, mydriasis, photophobia; Rare: blepharitis, deafness, diplopia, exophthalmos, glaucoma, hyperacusis, iritis, parosmia, scleritis, strabismus, taste loss, visual field defect.
Urogenital System — Infrequent: abortion2, albuminuria, amenorrhea2, anorgasmia, breast enlargement, breast pain, cystitis, dysuria, female lactation2, fibrocystic breast2, hematuria, leukorrhea2, menorrhagia2, metrorrhagia2, nocturia, polyuria, urinary incontinence, urinary retention, urinary urgency, vaginal hemorrhage2; Rare: breast engorgement, glycosuria, hypomenorrhea2, kidney pain, oliguria, uterine hemorrhage2, uterine fibroids enlarged2.
1 Personality disorder is the COSTART term for designating non-aggressive objectionable behavior.
2 Adjusted for gender.
6.3 Postmarketing Experience
The following adverse reactions have been identified during post approval use of fluoxetine. Because these reactions are reported voluntarily from a population of uncertain size, it is difficult to reliably estimate their frequency or evaluate a causal relationship to drug exposure.
Voluntary reports of adverse reactions temporally associated with fluoxetine that have been received since market introduction and that may have no causal relationship with the drug include the following: aplastic anemia, atrial fibrillation1, cataract, cerebrovascular accident1, cholestatic jaundice, dyskinesia (including, for example, a case of buccal-lingual-masticatory syndrome with involuntary tongue protrusion reported to develop in a 77 year-old female after 5 weeks of fluoxetine therapy and which completely resolved over the next few months following drug discontinuation), eosinophilic pneumonia1, epidermal necrolysis, erythema multiforme, erythema nodosum, exfoliative dermatitis, gynecomastia, heart arrest1, hepatic failure/necrosis, hyperprolactinemia, hypoglycemia, immune-related hemolytic anemia, kidney failure, movement disorders developing in patients with risk factors including drugs associated with such reactions and worsening of pre-existing movement disorders, optic neuritis, pancreatitis1, pancytopenia, pulmonary embolism, pulmonary hypertension, QT prolongation, Stevens-Johnson syndrome, thrombocytopenia1, thrombocytopenic purpura, ventricular tachycardia (including torsades de pointes–type arrhythmias), vaginal bleeding, and violent behaviors1.
1 These terms represent serious adverse reactions, but do not meet the definition for adverse drug reactions. They are included here because of their seriousness.
7. Drug Interactions
The potential for interaction by a variety of mechanisms (for example, pharmacodynamic, pharmacokinetic drug inhibition or enhancement, etc.) is a possibility.
7.1 Monoamine Oxidase Inhibitors (MAOI)
Concomitant use of SARAFEM (fluoxetine) in patients taking MAOIs is contraindicated. There have been reports of serious, sometimes fatal, reactions (including hyperthermia, rigidity, myoclonus, autonomic instability with possible rapid fluctuations of vital signs, and mental status changes that include extreme agitation progressing to delirium and coma) in patients receiving fluoxetine in combination with a monoamine oxidase inhibitor (MAOI), and in patients who have recently discontinued fluoxetine and are then started on an MAOI. Some cases presented with features resembling neuroleptic malignant syndrome. Therefore, fluoxetine, including SARAFEM, should not be used in combination with an MAOI, or within a minimum of 14 days of discontinuing therapy with an MAOI [see Contraindications (4)]. Since fluoxetine and its major metabolite have very long elimination half-lives, at least 5 weeks (perhaps longer, especially if fluoxetine has been prescribed chronically and/or at higher doses) should be allowed after stopping fluoxetine before starting an MAOI [see Dosage and Administration (2.4 and 2.5), Contraindications (4.1), Warnings and Precautions (5.2), and Clinical Pharmacology (12.3)].
7.2 CNS Acting Drugs
Caution is advised if the concomitant administration of fluoxetine, including SARAFEM, and other CNS acting drugs is required. In evaluating individual cases, consideration should be given to using lower initial doses of the concomitantly administered drugs, using conservative titration schedules, and monitoring of clinical status [see Clinical Pharmacology (12.3)].
7.3 Serotonergic Drugs
Based on the mechanism of action of SNRIs and SSRIs, including SARAFEM, and the potential for serotonin syndrome, caution is advised when SARAFEM is coadministered with other drugs that may affect the serotonergic neurotransmitter systems, such as triptans, linezolid (an antibiotic which is a reversible non-selective MAOI), lithium, tramadol, amphetamines, or St. John’s Wort [see Warnings and Precautions (5.2)]. The concomitant use of SARAFEM with SNRIs, SSRIs, or tryptophan is not recommended [see Dosage and Administration (2.4 and 2.5), Contraindications (4.1), Warnings and Precautions (5.2), and Drug Interactions (7.4), (7.5)].
7.4 Triptans
There have been rare postmarketing reports of serotonin syndrome with use of an SSRI and a triptan. If concomitant treatment of SARAFEM with a triptan is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases [see Warnings and Precautions (5.2) and Drug Interactions (7.3)].
7.5 Tryptophan
Five patients receiving fluoxetine in combination with tryptophan experienced adverse reactions, including agitation, restlessness, and gastrointestinal distress. The concomitant use with tryptophan is not recommended [see Warnings and Precautions (5.2) and Drug Interactions (7.3)].
7.6 Drugs that Interfere with Hemostasis (for example, NSAIDS, Aspirin, Warfarin)
Serotonin release by platelets plays an important role in hemostasis. Epidemiological studies of the case-control and cohort design that have demonstrated an association between use of psychotropic drugs that interfere with serotonin reuptake and the occurrence of upper gastrointestinal bleeding have also shown that concurrent use of an NSAID or aspirin may potentiate this risk of bleeding. Altered anticoagulant effects, including increased bleeding, have been reported when SNRIs or SSRIs are coadministered with warfarin. Patients receiving warfarin therapy should be carefully monitored when fluoxetine is initiated or discontinued [see Warnings and Precautions (5.7)].
7.7 Electroconvulsive Therapy (ECT)
There are no clinical studies establishing the benefit of the combined use of ECT and fluoxetine. There have been rare reports of prolonged seizures in patients on fluoxetine receiving ECT treatment.
7.8 Potential for Other Drugs to affect SARAFEM
Drugs Tightly Bound to Plasma Proteins — Because fluoxetine is tightly bound to plasma proteins, adverse effects may result from displacement of protein-bound fluoxetine by other tightly bound drugs [see Clinical Pharmacology (12.3)].
7.9 Potential for SARAFEM to affect Other Drugs
Pimozide — Concomitant use of SARAFEM in patients taking pimozide is contraindicated. Clinical studies of pimozide with other antidepressants demonstrate an increase in drug interaction or QTc prolongation. While a specific study with pimozide and fluoxetine has not been conducted, the potential for drug interactions or QTc prolongation warrants restricting the concurrent use of pimozide and fluoxetine [see Contraindications (4)].
Thioridazine — Concomitant use of SARAFEM in patients taking thioridazine is contraindicated. Thioridazine should not be administered with fluoxetine or within a minimum of 5 weeks after fluoxetine has been discontinued [see Contraindications (4)].
In a study of 19 healthy male subjects, which included 6 slow and 13 rapid hydroxylators of debrisoquin, a single 25 mg oral dose of thioridazine produced a 2.4-fold higher Cmax and a 4.5-fold higher AUC for thioridazine in the slow hydroxylators compared with the rapid hydroxylators. The rate of debrisoquin hydroxylation is felt to depend on the level of CYP2D6 isozyme activity. Thus, this study suggests that drugs which inhibit CYP2D6, such as certain SSRIs, including fluoxetine, will produce elevated plasma levels of thioridazine.
Thioridazine administration produces a dose-related prolongation of the QTc interval, which is associated with serious ventricular arrhythmias, such as torsades de pointes-type arrhythmias, and sudden death. This risk is expected to increase with fluoxetine-induced inhibition of thioridazine metabolism.
Drugs Metabolized by CYP2D6 — Fluoxetine inhibits the activity of CYP2D6, and may make individuals with normal CYP2D6 metabolic activity resemble a poor metabolizer. Coadministration of fluoxetine with other drugs that are metabolized by CYP2D6, including certain antidepressants (for example, tricyclic antidepressants (TCAs)), antipsychotics (for example, phenothiazines and most atypicals), and antiarrhythmics (for example, propafenone, flecainide, and others) should be approached with caution. Therapy with medications that are predominantly metabolized by the CYP2D6 system and that have a relatively narrow therapeutic index (see list below) should be initiated at the low end of the dose range if a patient is receiving fluoxetine concurrently or has taken it in the previous 5 weeks. Thus, his/her dosing requirements resemble those of poor metabolizers. If fluoxetine is added to the treatment regimen of a patient already receiving a drug metabolized by CYP2D6, the need for decreased dose of the original medication should be considered. Drugs with a narrow therapeutic index represent the greatest concern (for example, flecainide, propafenone, vinblastine, and TCAs). Due to the risk of serious ventricular arrhythmias and sudden death potentially associated with elevated plasma levels of thioridazine, thioridazine should not be administered with fluoxetine or within a minimum of 5 weeks after fluoxetine has been discontinued [see Contraindications (4)].
Tricyclic Antidepressants (TCAs) — In 2 studies, previously stable plasma levels of imipramine and desipramine have increased greater than 2- to 10-fold when fluoxetine has been administered in combination. This influence may persist for 3 weeks or longer after fluoxetine is discontinued. Thus, the dose of TCAs may need to be reduced and plasma TCA concentrations may need to be monitored temporarily when fluoxetine is coadministered or has been recently discontinued [see Clinical Pharmacology (12.3)].
Benzodiazapines — The half-life of concurrently administered diazepam may be prolonged in some patients [see Clinical Pharmacology (12.3)]. Coadministration of alprazolam and fluoxetine has resulted in increased alprazolam plasma concentrations and in further psychomotor performance decrement due to increased alprazolam levels.
Antipsychotics — Some clinical data suggests a possible pharmacodynamic and/or pharmacokinetic interaction between SSRIs and antipsychotics. Elevation of blood levels of haloperidol and clozapine has been observed in patients receiving concomitant fluoxetine [see Contraindications (4)].
Anticonvulsants — Patients on stable doses of phenytoin and carbamazepine have developed elevated plasma anticonvulsant concentrations and clinical anticonvulsant toxicity following initiation of concomitant fluoxetine treatment.
Lithium — There have been reports of both increased and decreased lithium levels when lithium was used concomitantly with fluoxetine. Cases of lithium toxicity and increased serotonergic effects have been reported. Lithium levels should be monitored when these drugs are administered concomitantly.
Drugs Tightly Bound to Plasma Proteins — Because fluoxetine is tightly bound to plasma proteins, the administration of fluoxetine to a patient taking another drug that is tightly bound to protein (for example, warfarin, digitoxin) may cause a shift in plasma concentrations potentially resulting in an adverse effect [see Clinical Pharmacology (12.3)].
Drugs Metabolized by CYP3A4 — In an in vivo interaction study involving coadministration of fluoxetine with single doses of terfenadine (a CYP3A4 substrate), no increase in plasma terfenadine concentrations occurred with concomitant fluoxetine.
Additionally, in vitro studies have shown ketoconazole, a potent inhibitor of CYP3A4 activity, to be at least 100 times more potent than fluoxetine or norfluoxetine as an inhibitor of the metabolism of several substrates for this enzyme, including astemizole, cisapride, and midazolam. These data indicate that fluoxetine’s extent of inhibition of CYP3A4 activity is not likely to be of clinical significance.
8. Use In Specific Populations
8.1 Pregnancy
Pregnancy Category C — It should be noted that the diagnosis of PMDD does exist during pregnancy. Fluoxetine should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. All pregnancies have a background risk of birth defects, loss, or other adverse outcome regardless of drug exposure.
Treatment of Pregnant Women during the First Trimester — There are no adequate and well-controlled clinical studies on the use of fluoxetine in pregnant women. Results of a number of published epidemiological studies assessing the risk of fluoxetine exposure during the first trimester of pregnancy have demonstrated inconsistent results. More than 10 cohort studies and case-control studies failed to demonstrate an increased risk for congenital malformations overall. However, one prospective cohort study conducted by the European Network of Teratology Information Services reported an increased risk of cardiovascular malformations in infants born to women (N = 253) exposed to fluoxetine during the first trimester of pregnancy compared to infants of women (N = 1359) who were not exposed to fluoxetine. There was no specific pattern of cardiovascular malformations. Overall, however, a causal relationship has not been established.
Nonteratogenic Effects — Neonates exposed to fluoxetine and other SSRIs or serotonin and norepinephrine reuptake inhibitors (SNRIs), late in the third trimester have developed complications requiring prolonged hospitalization, respiratory support, and tube feeding. Such complications can arise immediately upon delivery. Reported clinical findings have included respiratory distress, cyanosis, apnea, seizures, temperature instability, feeding difficulty, vomiting, hypoglycemia, hypotonia, hypertonia, hyperreflexia, tremor, jitteriness, irritability, and constant crying. These features are consistent with either a direct toxic effect of SSRIs and SNRIs or, possibly, a drug discontinuation syndrome. It should be noted that, in some cases, the clinical picture is consistent with serotonin syndrome [see Warnings and Precautions (5.2)].
Infants exposed to SSRIs in pregnancy may have an increased risk for persistent pulmonary hypertension of the newborn (PPHN). PPHN occurs in 1 to 2 per 1,000 live births in the general population and is associated with substantial neonatal morbidity and mortality. Several recent epidemiological studies suggest a positive statistical association between SSRI use (including fluoxetine) in pregnancy and PPHN. Other studies do not show a significant statistical association.
Physicians should also note the results of a prospective longitudinal study of 201 pregnant women with a history of major depression, who were either on antidepressants or had received antidepressants less than 12 weeks prior to their last menstrual period, and were in remission. Women who discontinued antidepressant medication during pregnancy showed a significant increase in relapse of their major depression compared to those women who remained on antidepressant medication throughout pregnancy.
When treating a pregnant woman with fluoxetine, the physician should carefully consider both the potential risks of taking an SSRI, along with the established benefits of treating depression with an antidepressant. The decision can only be made on a case by case basis.
Animal Data — In embryo-fetal development studies in rats and rabbits, there was no evidence of teratogenicity following administration of fluoxetine at doses up to 12.5 and 15 mg/kg/day, respectively (1.5 and 3.6 times, respectively, the maximum recommended human dose (MRHD) of 80 mg on a mg/m2 basis) throughout organogenesis. However, in rat reproduction studies, an increase in stillborn pups, a decrease in pup weight, and an increase in pup deaths during the first 7 days postpartum occurred following maternal exposure to 12 mg/kg/day (1.5 times the MRHD on a mg/m2 basis) during gestation or 7.5 mg/kg/day (0.9 times the MRHD on a mg/m2 basis) during gestation and lactation. There was no evidence of developmental neurotoxicity in the surviving offspring of rats treated with 12 mg/kg/day during gestation. The no-effect dose for rat pup mortality was 5 mg/kg/day (0.6 times the MRHD on a mg/m2 basis).
8.2 Labor and Delivery
The effect of fluoxetine on labor and delivery in humans is unknown. However, because fluoxetine crosses the placenta and because of the possibility that fluoxetine may have adverse effects on the newborn, fluoxetine should be used during labor and delivery only if the potential benefit justifies the potential risk to the fetus.
8.3 Nursing Mothers
Because fluoxetine is excreted in human milk, nursing while on SARAFEM is not recommended. In one breast-milk sample, the concentration of fluoxetine plus norfluoxetine was 70.4 ng/mL. The concentration in the mother’s plasma was 295.0 ng/mL. No adverse effects on the infant were reported. In another case, an infant nursed by a mother on fluoxetine developed crying, sleep disturbance, vomiting, and watery stools. The infant’s plasma drug levels were 340 ng/mL of fluoxetine and 208 ng/mL of norfluoxetine on the second day of feeding.
8.4 Pediatric Use
Safety and effectiveness of SARAFEM in the pediatric population have not been established [see Boxed Warning and Warnings and Precautions (5.1)]. When considering the use of SARAFEM in a child or adolescent, the potential risks must be balanced with the clinical need. Significant toxicity, including myotoxicity, long-term neurobehavioral and reproductive toxicity, and impaired bone development, has been observed following exposure of juvenile animals to fluoxetine. Some of these effects occurred at clinically relevant exposures.
As with other SSRIs, decreased weight gain has been observed in association with the use of fluoxetine in children and adolescent patients. After 19 weeks of treatment in a clinical trial, pediatric subjects treated with fluoxetine gained an average of 1.1 cm less in height and 1.1 kg less in weight than subjects treated with placebo. In addition, fluoxetine treatment was associated with a decrease in alkaline phosphatase levels. The safety of fluoxetine treatment for pediatric patients has not been systematically assessed for chronic treatment longer than several months in duration. In particular, there are no studies that directly evaluate the longer-term effects of fluoxetine on the growth, development and maturation of children and adolescent patients. Therefore, height and weight should be monitored periodically in pediatric patients receiving fluoxetine [see Warnings and Precautions (5.6)].
In a study in which fluoxetine (3, 10, or 30 mg/kg) was orally administered to young rats from weaning (Postnatal Day 21) through adulthood (Day 90), male and female sexual development was delayed at all doses, and growth (body weight gain, femur length) was decreased during the dosing period in animals receiving the highest dose. At the end of the treatment period, serum levels of creatine kinase (marker of muscle damage) were increased at the intermediate and high doses, and abnormal muscle and reproductive organ histopathology (skeletal muscle degeneration and necrosis, testicular degeneration and necrosis, epididymal vacuolation and hypospermia) was observed at the high dose. When animals were evaluated after a recovery period (up to 11 weeks after cessation of dosing), neurobehavioral abnormalities (decreased reactivity at all doses and learning deficit at the high dose) and reproductive functional impairment (decreased mating at all doses and impaired fertility at the high dose) were seen; in addition, testicular and epididymal microscopic lesions and decreased sperm concentrations were found in the high dose group, indicating that the reproductive organ effects seen at the end of treatment were irreversible. The reversibility of fluoxetine-induced muscle damage was not assessed. Adverse effects similar to those observed in rats treated with fluoxetine during the juvenile period have not been reported after administration of fluoxetine to adult animals. Plasma exposures (AUC) to fluoxetine in juvenile rats receiving the low, intermediate, and high dose in this study were approximately 0.1 to 0.2, 1 to 2, and 5 to 10 times, respectively, the average exposure in pediatric patients receiving the maximum recommended dose (MRD) of 20 mg/day. Rat exposures to the major metabolite, norfluoxetine, were approximately 0.3 to 0.8, 1 to 8, and 3 to 20 times, respectively, pediatric exposure at the MRD.
A specific effect of fluoxetine on bone development has been reported in mice treated with fluoxetine during the juvenile period. When mice were treated with fluoxetine (5 or 20 mg/kg, intraperitoneal) for 4 weeks starting at 4 weeks of age, bone formation was reduced resulting in decreased bone mineral content and density. These doses did not affect overall growth (body weight gain or femoral length). The doses administered to juvenile mice in this study are approximately 0.5 and 2 times the MRD for pediatric patients on a body surface area (mg/m2) basis.
In another mouse study, administration of fluoxetine (10 mg/kg intraperitoneal) during early postnatal development (Postnatal Days 4 to 21) produced abnormal emotional behaviors (decreased exploratory behavior in elevated plus-maze, increase shock avoidance latency) in adulthood (12 weeks of age). The dose used in this study is approximately equal to the pediatric MRD on a mg/m2 basis. Because of the early dosing period in this study, the significance of these findings to the approved pediatric use in humans is uncertain.
8.6 Hepatic Impairment
In subjects with cirrhosis of the liver, the clearances of fluoxetine and its active metabolite, norfluoxetine, were decreased, thus increasing the elimination half-lives of these substances. A lower or less frequent dose of fluoxetine should be used in patients with cirrhosis. Caution is advised when using SARAFEM in patients with diseases or conditions that could affect its metabolism [see Dosage and Administration (2.3) and Clinical Pharmacology (12.3)].
9. Drug Abuse and Dependence
9.3 Dependence
Fluoxetine has not been systematically studied, in animals or humans, for its potential for abuse, tolerance, or physical dependence. While the pre-marketing clinical experience with fluoxetine did not reveal any tendency for a withdrawal syndrome or any drug seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this limited experience the extent to which a CNS active drug will be misused, diverted, and/or abused once marketed. Consequently, physicians should carefully evaluate patients for history of drug abuse and follow such patients closely, observing them for signs of misuse or abuse of SARAFEM (for example, development of tolerance, incrementation of dose, drug-seeking behavior).
10. Overdosage
10.1 Human Experience
Worldwide exposure to fluoxetine hydrochloride is estimated to be over 38 million patients (circa 1999). Of the 1578 cases of overdose involving fluoxetine hydrochloride, alone or with other drugs, reported from this population, there were 195 deaths.
Among 633 adult patients who overdosed on fluoxetine hydrochloride alone, 34 resulted in a fatal outcome, 378 completely recovered, and 15 patients experienced sequelae after overdosage, including abnormal accommodation, abnormal gait, confusion, unresponsiveness, nervousness, pulmonary dysfunction, vertigo, tremor, elevated blood pressure, impotence, movement disorder, and hypomania. The remaining 206 patients had an unknown outcome. The most common signs and symptoms associated with non-fatal overdosage were seizures, somnolence, nausea, tachycardia, and vomiting. The largest known ingestion of fluoxetine hydrochloride in adult patients was 8 grams in a patient who took fluoxetine alone and who subsequently recovered. However, in an adult patient who took fluoxetine alone, an ingestion as low as 520 mg has been associated with lethal outcome, but causality has not been established.
Among pediatric patients (ages 3 months to 17 years), there were 156 cases of overdose involving fluoxetine alone or in combination with other drugs. Six patients died, 127 patients completely recovered, 1 patient experienced renal failure, and 22 patients had an unknown outcome. One of the six fatalities was a 9-year-old boy who had a history of OCD, Tourette’s syndrome with tics, attention deficit disorder, and fetal alcohol syndrome. He had been receiving 100 mg of fluoxetine daily for 6 months in addition to clonidine, methylphenidate, and promethazine. Mixed-drug ingestion or other methods of suicide complicated all 6 overdoses in children that resulted in fatalities. The largest ingestion in pediatric patients was 3 grams which was nonlethal.
Other important adverse reactions reported with fluoxetine overdose (single or multiple drugs) include coma, delirium, ECG abnormalities (such as QT interval prolongation and ventricular tachycardia, including torsades de pointes-type arrhythmias), hypotension, mania, neuroleptic malignant syndrome-like reactions, pyrexia, stupor, and syncope.
10.2 Animal Experience
Studies in animals do not provide precise or necessarily valid information about the treatment of human overdose. However, animal experiments can provide useful insights into possible treatment strategies.
The oral median lethal dose in rats and mice was found to be 452 and 248 mg/kg, respectively. Acute high oral doses produced hyperirritability and convulsions in several animal species.
Among 6 dogs purposely overdosed with oral fluoxetine, 5 experienced grand mal seizures. Seizures stopped immediately upon the bolus intravenous administration of a standard veterinary dose of diazepam. In this short-term study, the lowest plasma concentration at which a seizure occurred was only twice the maximum plasma concentration seen in humans taking 80 mg/day, chronically.
In a separate single-dose study, the ECG of dogs given high doses did not reveal prolongation of the PR, QRS, or QT intervals. Tachycardia and an increase in blood pressure were observed. Consequently, the value of the ECG in predicting cardiac toxicity is unknown. Nonetheless, the ECG should ordinarily be monitored in cases of human overdose [see Overdosage (10.3)].
10.3 Management of Overdose
Treatment should consist of those general measures employed in the management of overdosage with any SSRI.
Ensure an adequate airway, oxygenation, and ventilation. Monitor cardiac rhythm and vital signs. General supportive and symptomatic measures are also recommended. Induction of emesis is not recommended. Gastric lavage with a large-bore orogastric tube with appropriate airway protection, if needed, may be indicated if performed soon after ingestion, or in symptomatic patients.
Activated charcoal should be administered. Due to the large volume of distribution of this drug, forced diuresis, dialysis, hemoperfusion, and exchange transfusion are unlikely to be of benefit. No specific antidotes for fluoxetine are known.
A specific caution involves patients who are taking or have recently taken fluoxetine and might ingest excessive quantities of a TCA. In such a case, accumulation of the parent tricyclic and/or an active metabolite may increase the possibility of clinically significant sequelae and extend the time needed for close medical observation [see Drug Interactions (7.9)].
Based on experience in animals, which may not be relevant to humans, fluoxetine-induced seizures that fail to remit spontaneously may respond to diazepam.
In managing overdosage, consider the possibility of multiple drug involvement. The physician should consider contacting a poison control center for additional information on the treatment of any overdose. Telephone numbers for certified poison control centers are listed in the Physicians’ Desk Reference (PDR).
11. Sarafem Tablets Description
SARAFEM (fluoxetine hydrochloride tablets) is a selective serotonin reuptake inhibitor (SSRI) for oral administration. It is designated (±)-N-methyl-3-phenyl-3-[(α, α, α -trifluoro-p-tolyl)oxy]propylamine hydrochloride and has the empirical formula of C17H18F3NO•HCl. Its molecular weight is 345.79. The structural formula is:
![The structural formula for SARAFEM (fluoxetine hydrochloride tablets) is a selective serotonin reuptake inhibitor (SSRI) for oral administration. It is designated (±)-N-methyl-3-phenyl-3-[(a,a,a-trifluoro-p-tolyl)oxy]propylamine hydrochloride and has the empirical formula of C17H18F3NO•HCl. Its molecular weight is 345.79.](https://www.drugs.com/pro/images/e731be04-0595-49dd-b87a-c2b9ba6ba68c/sarafem-01.jpg)
Fluoxetine hydrochloride is a white to off-white crystalline solid with a solubility of 14 mg/mL in water.
Each SARAFEM tablet contains fluoxetine hydrochloride equivalent to 10 mg (32.3 µmol), 15 mg (48.5 µmol) or 20 mg (64.7 µmol) of fluoxetine. Each tablet also contains microcrystalline cellulose, croscarmellose sodium, colloidal silicon dioxide, magnesium stearate, FD&C Yellow No. 6 aluminum lake (10 mg and 20 mg tablets) and D&C Yellow No. 10 aluminum lake (10 mg and 20 mg tablets).
12. Sarafem Tablets - Clinical Pharmacology
12.1 Mechanism of Action
Although the exact mechanism of SARAFEM is unknown, it is presumed to be linked to its inhibition of CNS neuronal uptake of serotonin.
12.2 Pharmacodynamics
Studies at clinically relevant doses in humans have demonstrated that fluoxetine blocks the uptake of serotonin into human platelets. Studies in animals also suggest that fluoxetine is a much more potent uptake inhibitor of serotonin than of norepinephrine.
Antagonism of muscarinic, histaminergic, and α1- adrenergic receptors has been hypothesized to be associated with various anticholinergic, sedative, and cardiovascular effects of classical tricyclic antidepressant (TCA) drugs. Fluoxetine binds to these and other membrane receptors from brain tissue much less potently in vitro than do the tricyclic drugs.
Enantiomers — Fluoxetine is a racemic mixture (50/50) of R-fluoxetine and S-fluoxetine enantiomers. In animal models, both enantiomers are specific and potent serotonin uptake inhibitors with essentially equivalent pharmacologic activity. The S-fluoxetine enantiomer is eliminated more slowly and is the predominant enantiomer present in plasma at steady state.
12.3 Pharmacokinetics
Systemic Bioavailability/Absorption —Mean plasma fluoxetine concentrations following single-dose administration of SARAFEM 20 mg tablets are shown in Figure 1; fluoxetine and norfluoxetine pharmacokinetic parameters are shown in Table 7.
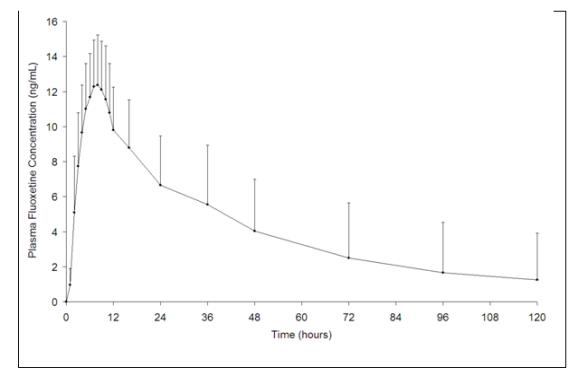
Figure 1. Mean (± SD) Plasma Fluoxetine Concentrations Following Single-Dose Administration of SARAFEM 20 mg Tablets to Healthy Female Volunteers (n = 23)
| Dose | Analyte | Cmax
(ng/mL) | Tmax (hour) | AUC(0-t)
(ng·h/mL) | T1/2a
(hour) |
| SARAFEM 20 mg | Fluoxetine | 13.2 (22) | 8.0 (2.0-10.0) | 722.4 (138) | 26.5 (15.7-310.0) |
| Norfluoxetine | 9.7 (37) | 48.0 (11.0-144.0) | 2114.3 (41) | 110.4 (66.8-308.0) | |
| a) 3 subjects had longer fluoxetine elimination half-life values ranging from 100-300 hours; see Clinical issues relating to metabolism/elimination for more information on “poor metabolizers” | |||||
Food does not appear to affect the systemic bioavailability of fluoxetine, although it may delay its absorption by 1 to 2 hours, which is probably not clinically significant. Thus, fluoxetine may be administered with or without food.
Protein Binding — Over the concentration range from 200 to 1000 ng/mL, approximately 94.5% of fluoxetine is bound in vitro to human serum proteins, including albumin and α1-glycoprotein. The interaction between fluoxetine and other highly protein-bound drugs has not been fully evaluated, but may be important [see Drug Interactions (7.8 and 7.9)].
Metabolism — Fluoxetine is extensively metabolized in the liver to norfluoxetine and a number of other unidentified metabolites. The only identified active metabolite, norfluoxetine, is formed by demethylation of fluoxetine. In animal models, S-norfluoxetine is a potent and selective inhibitor of serotonin uptake and has activity essentially equivalent to R- or S-fluoxetine. R-norfluoxetine is significantly less potent than the parent drug in the inhibition of serotonin uptake.
Variability in Metabolism — A subset (about 7%) of the population has reduced activity of the drug metabolizing enzyme cytochrome P450 2D6 (CYP2D6). Such individuals are referred to as “poor metabolizers” of drugs such as debrisoquin, dextromethorphan, and the TCAs. In a study involving labeled and unlabeled enantiomers administered as a racemate, these individuals metabolized S-fluoxetine at a slower rate and thus achieved higher concentrations of S-fluoxetine. Consequently, concentrations of S-norfluoxetine at steady state were lower. The metabolism of R-fluoxetine in these poor metabolizers appears normal. When compared with normal metabolizers, the total sum at steady state of the plasma concentrations of the 4 active enantiomers was not significantly greater among poor metabolizers. Thus, the net pharmacodynamic activities were essentially the same. Alternative, nonsaturable pathways (non-2D6) also contribute to the metabolism of fluoxetine. This explains how fluoxetine achieves a steady-state concentration rather than increasing without limit.
Because fluoxetine’s metabolism, like that of a number of other compounds including TCAs and other selective serotonin reuptake inhibitors (SSRIs), involves the CYP2D6 system, concomitant therapy with drugs also metabolized by this enzyme system (such as the TCAs) may lead to drug interactions [see Drug Interactions (7.9)].
Excretion — The primary route of elimination appears to be hepatic metabolism to inactive metabolites excreted by the kidney.
Accumulation and Slow Elimination — The relatively slow elimination of fluoxetine (elimination half-life of 1 to 3 days after acute administration and 4 to 6 days after chronic administration) and its active metabolite, norfluoxetine (elimination half-life of 4 to 16 days after acute and chronic administration), leads to significant accumulation of these active species in chronic use and delayed attainment of steady state, even when a fixed dose is used [see Warnings and Precautions (5.12)]. After 30 days of dosing at 40 mg/day, plasma concentrations of fluoxetine in the range of 91 to 302 ng/mL and norfluoxetine in the range of 72 to 258 ng/mL have been observed. Plasma concentrations of fluoxetine were higher than those predicted by single-dose studies, because fluoxetine’s metabolism is not proportional to dose. Norfluoxetine, however, appears to have linear pharmacokinetics. Its mean terminal half-life after a single dose was 8.6 days and after multiple dosing was 9.3 days. Steady-state levels after prolonged dosing are similar to levels seen at 4 to 5 weeks.
The long elimination half-lives of fluoxetine and norfluoxetine assure that, even when dosing is stopped, active drug substance will persist in the body for weeks (primarily depending on individual patient characteristics, previous dosing regimen, and length of previous therapy at discontinuation). This is of potential consequence when drug discontinuation is required or when drugs are prescribed that might interact with fluoxetine and norfluoxetine following the discontinuation of SARAFEM.
Hepatic Impairment — As might be predicted from its primary site of metabolism, liver impairment can affect the elimination of fluoxetine. The elimination half-life of fluoxetine was prolonged in a study of cirrhotic patients, with a mean of 7.6 days compared with the range of 2 to 3 days seen in subjects without liver disease; norfluoxetine elimination was also delayed, with a mean duration of 12 days for cirrhotic patients compared with the range of 7 to 9 days in normal subjects. This suggests that the use of fluoxetine in patients with liver disease must be approached with caution. If fluoxetine is administered to patients with liver disease, a lower or less frequent dose should be used [see Dosage and Administration (2.3), Use in Specific Populations (8.6)].
Renal Impairment — In depressed patients on dialysis (N = 12), fluoxetine administered as 20 mg once daily for 2 months produced steady-state fluoxetine and norfluoxetine plasma concentrations comparable with those seen in patients with normal renal function. While the possibility exists that renally excreted metabolites of fluoxetine may accumulate to higher levels in patients with severe renal dysfunction, use of a lower or less frequent dose is not routinely necessary in renally impaired patients.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity — The dietary administration of fluoxetine to rats and mice for 2 years at doses of up to 10 and 12 mg/kg/day, respectively [approximately 1.2 and 0.7 times, respectively, the maximum recommended human dose (MRHD) of 80 mg on a mg/m2 basis], produced no evidence of carcinogenicity.
Mutagenicity — Fluoxetine and norfluoxetine have been shown to have no genotoxic effects based on the following assays: bacterial mutation assay, DNA repair assay in cultured rat hepatocytes, mouse lymphoma assay, and in vivo sister chromatid exchange assay in Chinese hamster bone marrow cells.
Impairment of Fertility — Two fertility studies conducted in adult rats at doses of up to 7.5 and 12.5 mg/kg/day (approximately 0.9 and 1.5 times the MRHD on a mg/m2 basis) indicated that fluoxetine had no adverse effects on fertility. However, adverse effects on fertility were seen when juvenile rats were treated with fluoxetine [see Use in Specific Populations (8.4)].
13.2 Animal Toxicology and/or Pharmacology
Phospholipids are increased in some tissues of mice, rats, and dogs given fluoxetine chronically. This effect is reversible after cessation of fluoxetine treatment. Phospholipid accumulation in animals has been observed with many cationic amphiphilic drugs, including fenfluramine, imipramine, and ranitidine. The significance of this effect in humans is unknown.
14. Clinical Studies
14.1 Premenstrual Dysphoric Disorder (PMDD)
The effectiveness of SARAFEM for the treatment of PMDD was established in 3 placebo-controlled trials (1 intermittent and 2 continuous dosing). In an intermittent dosing trial described below, patients met Diagnostic and Statistical Manual-4th edition (DSM-IV) criteria for PMDD. In the continuous dosing trials described below, patients met Diagnostic and Statistical Manual-3rd edition revised (DSM-IIIR) criteria for Late Luteal Phase Dysphoric Disorder (LLPDD), the clinical entity now referred to as PMDD in the DSM-IV. Patients on oral contraceptives were excluded from these trials; therefore, the efficacy of fluoxetine in combination with oral contraceptives for the treatment of PMDD is unknown.
In an intermittent dosing double-blind, parallel group study of 3 months duration, patients (N = 260 randomized) were treated with fluoxetine 10 mg/day, fluoxetine 20 mg/day, or placebo. Fluoxetine or placebo was started 14 days prior to the anticipated onset of menstruation and was continued through the first full day of menses. Efficacy was assessed with the Daily Record of Severity of Problems (DRSP), a patient-rated instrument that mirrors the diagnostic criteria for PMDD as identified in the DSM-IV, and includes assessments for mood, physical symptoms, and other symptoms. Fluoxetine 20 mg/day was shown to be significantly more effective than placebo as measured by the DRSP total score. Fluoxetine 10 mg/day was not shown to be significantly more effective than placebo on this outcome. The average DRSP total score decreased 38% on fluoxetine 20 mg/day, 35% on fluoxetine 10 mg/day, and 30% on placebo.
In the first continuous dosing double-blind, parallel group study of 6 months duration involving N = 320 patients, fixed doses of fluoxetine 20 and 60 mg/day given daily throughout the menstrual cycle were shown to be significantly more effective than placebo as measured by a Visual Analogue Scale (VAS) total score (including mood and physical symptoms). The average total VAS score decreased 7% on placebo treatment, 36% on 20 mg, and 39% on 60 mg fluoxetine. The difference between the 20 and 60 mg doses was not statistically significant. The following table shows the percentage of patients meeting criteria for either moderate or marked improvement on the VAS total score:
| Improvement | N | Placebo | N | Fluoxetine 20 mg | N | Fluoxetine 60 mg |
| Moderate | 94 | 11% | 95 | 37% | 85 | 38% |
| Marked | 94 | 4% | 95 | 6% | 85 | 18% |
In a second continuous dosing double-blind, cross-over study, patients (N = 19) were treated with fluoxetine 20 to 60 mg/day (mean dose = 27 mg/day) and placebo daily throughout the menstrual cycle for a period of 3 months each. Fluoxetine was significantly more effective than placebo as measured by within cycle follicular to luteal phase changes in the VAS total score (mood, physical, and social impairment symptoms). The average VAS total score (follicular to luteal phase increase) was 3.8 times higher during placebo treatment than what was observed during fluoxetine treatment.
In another continuous dosing double-blind, parallel group study, patients with LLPDD (N = 42) were treated daily with fluoxetine 20 mg/day, bupropion 300 mg/day, or placebo for 2 months. Neither fluoxetine nor bupropion was shown to be superior to placebo on the primary endpoint, that is, response rate [defined as a rating of 1 (very much improved) or 2 (much improved) on the CGI], possibly due to sample size.
16. How is Sarafem Tablets supplied
16.1 How Supplied
SARAFEM® (fluoxetine hydrochloride tablets) is available in 10 mg1, 15 mg1 and 20 mg1 strengths.
The 10 mg tablet is a cream, round tablet embossed with S10 on one side:
NDC 0430-0210-14 - Four blister cards of 7 tablets each
The 15 mg tablet is a white, round tablet embossed with S15 on one side:
NDC 0430-0215-14 - Four blister cards of 7 tablets each
The 20 mg tablet is a yellow, round tablet embossed with S20 on one side:
NDC 0430-0220-14 - Four blister cards of 7 tablets each
________________
1 Equivalent to fluoxetine base.
17. Patient Counseling Information
See the FDA-approved Medication Guide.
17.1 General Information
Healthcare providers should instruct their patients to read the Medication Guide before starting therapy with SARAFEM and to reread it each time the prescription is renewed.
Healthcare providers should inform patients, their families, and their caregivers about the benefits and risks associated with treatment with SARAFEM and should counsel them in its appropriate use. Healthcare providers should instruct patients, their families, and their caregivers to read the Medication Guide and should assist them in understanding its contents. Patients should be given the opportunity to discuss the contents of the Medication Guide and to obtain answers to any questions they may have.
Patients should be advised of the following issues and asked to alert their healthcare provider if these occur while taking SARAFEM.
17.2 Clinical Worsening and Suicide Risk
Patients, their families, and their caregivers should be encouraged to be alert to the emergence of anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, mania, other unusual changes in behavior, worsening of depression, and suicidal ideation, especially early during antidepressant treatment and when the dose is adjusted up or down. Families and caregivers of patients should be advised to look for the emergence of such symptoms on a day-to-day basis, since changes may be abrupt. Such symptoms should be reported to the patient’s prescriber or health professional, especially if they are severe, abrupt in onset, or were not part of the patient’s presenting symptoms. Symptoms such as these may be associated with an increased risk for suicidal thinking and behavior and indicate a need for very close monitoring and possibly changes in the medication [see Boxed Warning and Warnings and Precautions (5.1)].
17.3 Serotonin Syndrome
Patients should be cautioned about the risk of serotonin syndrome with the concomitant use of SARAFEM and other serotonergic agents including triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, buspirone, amphetamines, tryptophan, and St. John’s Wort [see Contraindications (4.1), Warnings and Precautions (5.2), and Drug Interactions (7.3)].
Patients should be advised of the signs and symptoms associated with serotonin syndrome that may include mental status changes (for example, agitation, hallucinations, delirium, and coma), autonomic instability (for example, tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular changes (for example, tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and/or gastrointestinal symptoms (for example, nausea, vomiting, diarrhea). Patients should be cautioned to seek medical care immediately if they experience these symptoms.
17.4 Allergic Reactions and Rash
Patients should be advised to notify their physician if they develop a rash or hives [see Warnings and Precautions (5.3)]. Patients should also be advised of the signs and symptoms associated with a severe allergic reaction, including swelling of the face, eyes, or mouth, or trouble breathing. Patients should be cautioned to seek medical care immediately if they experience these symptoms.
17.5 Abnormal Bleeding
Patients should be cautioned about the concomitant use of fluoxetine and NSAIDs, aspirin, warfarin, or other drugs that affect coagulation since combined use of psychotropic drugs that interfere with serotonin reuptake and these agents have been associated with an increased risk of bleeding [see Warnings and Precautions (5.7) and Drug Interactions (7.6)]. Patients should be advised to call their doctor if they experience any increased or unusual bruising or bleeding while taking SARAFEM.
17.6 Angle-Closure Glaucoma
Patients should be advised that taking SARAFEM can cause mild pupillary dilation, which in susceptible individuals, can lead to an episode of angle-closure glaucoma. Pre-existing glaucoma is almost always open-angle glaucoma because angle-closure glaucoma, when diagnosed, can be treated definitively with iridectomy. Open-angle glaucoma is not a risk factor for angle-closure glaucoma. Patients may wish to be examined to determine whether they are susceptible to angle-closure, and have a prophylactic procedure (e.g., iridectomy), if they are susceptible [See Warnings and Precautions (5.8)].
17.7 Hyponatremia
Patients should be advised that hyponatremia has been reported as a result of treatment with SNRIs and SSRIs, including SARAFEM. Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which may lead to falls. More severe and/or acute cases have been associated with hallucination, syncope, seizure, coma, respiratory arrest, and death [see Warnings and Precautions (5.9)].
17.8 Potential for Cognitive and Motor Impairment
SARAFEM may impair judgment, thinking, or motor skills. Patients should be advised to avoid driving a car or operating hazardous machinery until they are reasonably certain that their performance is not affected [see Warnings and Precautions (5.12)].
17.9 Use of Concomitant Medications
Patients should be advised to inform their physician if they are taking, or plan to take, any prescription medication, including Symbyax, Prozac, Prozac Weekly, or over-the-counter drugs, including herbal supplements or alcohol. Patients should also be advised to inform their physicians if they plan to discontinue any medications they are taking while on SARAFEM.
17.10 Discontinuation of Treatment
Patients should be advised to take SARAFEM exactly as prescribed, and to continue taking SARAFEM as prescribed even after their symptoms improve. Patients should be advised that they should not alter their dosing regimen, or stop taking SARAFEM without consulting their physician [see Warnings and Precautions (5.14)]. Patients should be advised to consult with their healthcare provider if their symptoms do not improve with SARAFEM.
17.11 Use in Specific Populations
Pregnancy — Patients should be advised to notify their physician if they become pregnant or intend to become pregnant during therapy. Fluoxetine should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus [see Use in Specific Populations (8.1)].
Nursing Mothers — Patients should be advised to notify their physician if they intend to breastfeed an infant during therapy. Because fluoxetine is excreted in human milk, nursing while taking SARAFEM is not recommended [see Use in Specific Populations (8.3)].
Distributed by:
Allergan USA, Inc.
Irvine, CA 92612
Sarafem® is a registered trademark of Allergan Pharmaceuticals International Limited
© 2016 Allergan. All rights reserved.
Medication Guide
Medication Guide
SARAFEM® (SAIR-a-fem)
(fluoxetine hydrochloride)
Tablets
Read the Medication Guide that comes with SARAFEM before you start taking it and each time you get a refill. There may be new information. This Medication Guide does not take the place of talking to your healthcare provider about your medical condition or treatment. Talk with your healthcare provider if there is something you do not understand or you want to learn more about.
SARAFEM is in a class of drugs called selective serotonin reuptake inhibitors (SSRIs), which are often used for the treatment of depression and anxiety disorders. Although SARAFEM is not a treatment for depression, it contains fluoxetine hydrochloride, the same active ingredient in some antidepressants.
What is the most important information I should know about SARAFEM?
SARAFEM and other antidepressant medicines may cause serious side effects including:
1. Suicidal thoughts or actions:
-
SARAFEM and other antidepressant medicines may increase suicidal thoughts or actions in some children, teenagers, or young adults within the first few months of treatment or when the dose is changed.
- Depression or other serious mental illnesses are the most important causes of suicidal thoughts or actions.
- Watch for these changes and call your healthcare provider right away if you notice:
○ New or sudden changes in mood, behavior, actions, thoughts, or feelings, especially if severe.
○ Pay particular attention to such changes when SARAFEM is started or when the dose is changed.
Keep all follow-up visits with your healthcare provider and call between visits if you are worried about symptoms.
Call your healthcare provider right away if you have any of the following symptoms, or call 911 if an emergency, especially if they are new, worse, or worry you:
- attempts to commit suicide
- acting on dangerous impulses
- acting aggressive or violent
- thoughts about suicide or dying
- new or worse depression
- new or worse anxiety or panic attacks
- feeling agitated, restless, angry or irritable
- trouble sleeping
- an increase in activity or talking more than what is normal for you
- other unusual changes in behavior or mood
Call your healthcare provider right away if you have any of the following symptoms, or call 911 if an emergency. SARAFEM may be associated with these serious side effects:
2. Serotonin Syndrome. This condition can be life-threatening and may include:
- agitation, hallucinations, coma or other changes in mental status
- coordination problems or muscle twitching (overactive reflexes)
- racing heartbeat, high or low blood pressure
- sweating or fever
- nausea, vomiting, or diarrhea
- muscle rigidity
- dizziness
- flushing
- tremor
- seizures
3. Severe allergic reactions:
- trouble breathing
- swelling of the face, tongue, eyes or mouth
- rash, itchy welts (hives) or blisters, alone or with fever or joint pain
4. Manic episodes:
- greatly increased energy
- severe trouble sleeping
- racing thoughts
- reckless behavior
- unusually grand ideas
- excessive happiness or irritability
- talking more or faster than usual
5. Seizures or convulsions
6. Changes in appetite or weight. Children and adolescents should have height and weight monitored during treatment.
7. Abnormal bleeding: SARAFEM and other antidepressant medicines may increase your risk of bleeding or bruising, especially if you take the blood thinner warfarin (Coumadin®, Jantoven®), a non-steroidal anti-inflammatory drug (NSAID’s, like ibuprofen or naproxen), or aspirin.
8. Visual Problems
- eye pain
- changes in vision
- swelling or redness in or around the eye
Only some people are at risk for these problems. You may want to undergo an eye examination to see if you are at risk and receive preventative treatment if you are.
9. Low salt (sodium) levels in the blood. Elderly people may be at greater risk for this. Symptoms may include:
- headache
- weakness or feeling unsteady
- confusion, problems concentrating or thinking or memory problems
Do not stop SARAFEM without first talking to your healthcare provider. Stopping SARAFEM too quickly may cause serious symptoms including:
- anxiety, irritability, high or low mood, feeling restless or changes in sleep habits
- headache, sweating, nausea, dizziness
- electric shock-like sensations, shaking, confusion
What is SARAFEM?
SARAFEM is a prescription medicine used to treat premenstrual dysphoric disorder (PMDD).
It is not known if SARAFEM is safe and effective in children.
Talk with your healthcare provider if you do not think that your condition is getting better with SARAFEM treatment.
Who should not take SARAFEM?
Do not take SARAFEM if you:
- take a Monoamine Oxidase Inhibitor (MAOI). Ask your healthcare provider or pharmacist if you are not sure if you take an MAOI, including the antibiotic linezolid.
○ Do not take an MAOI within 5 weeks of stopping SARAFEM unless directed to do so by your healthcare provider.
○ Do not start SARAFEM if you stopped taking an MAOI in the last 2 weeks unless directed to do so by your healthcare provider.
Women who take SARAFEM close in time to an MAOI may have serious or even life-threatening side effects. Get medical help right away if you have any of these symptoms:
• high fever
• uncontrolled muscle spasms
• stiff muscles
• rapid changes in heart rate or blood pressure
• confusion
• loss of consciousness (pass out)
-
take Mellaril® (thioridazine). Do not take Mellaril® within 5 weeks of stopping SARAFEM because this can cause serious heart rhythm problems or sudden death.
- take the antipsychotic medicine pimozide (Orap®) because this can cause serious heart problems.
What should I tell my healthcare provider before taking SARAFEM? Ask if you are not sure.
Before starting SARAFEM, tell your healthcare provider if you:
- Are taking certain drugs or treatments such as:
○ Triptans used to treat migraine headache
○ Medicines used to treat mood, anxiety, psychotic or thought disorders, including tricyclics, lithium, buspirone, amphetamines, SSRIs, SNRIs, MAOIs or antipsychotics
○ Tramadol and fentanyl
○ Over-the-counter supplements such as tryptophan or St. John’s Wort
○ Electroconvulsive therapy (ECT)
- have liver problems
- have kidney problems
- have heart problems
- have or had seizures or convulsions
- have bipolar disorder or mania
- have low sodium levels in your blood
- have a history of a stroke
- have high blood pressure
- have or had bleeding problems
- are pregnant or plan to become pregnant. It is not known if SARAFEM will harm your unborn baby.
- are breastfeeding or plan to breastfeed. Some SARAFEM may pass into your breast milk. Talk to your healthcare provider about the best way to feed your baby while taking SARAFEM.
Tell your healthcare provider about all the medicines that you take, including prescription and non-prescription medicines, vitamins, and herbal supplements. SARAFEM and some medicines may interact with each other, may not work as well, or may cause serious side effects.
Your healthcare provider or pharmacist can tell you if it is safe to take SARAFEM with your other medicines. Do not start or stop any medicine while taking SARAFEM without talking to your healthcare provider first.
If you take SARAFEM, you should not take any other medicines that contain fluoxetine hydrochloride:
- Symbyax®
- Prozac®
- Prozac® WeeklyTM
How should I take SARAFEM?
- Take SARAFEM exactly as prescribed. Your healthcare provider may need to change the dose of SARAFEM until it is the right dose for you.
- Talk to your healthcare provider if your symptoms do not get better.
- SARAFEM may be taken with or without food.
- If you take too much SARAFEM, call your healthcare provider or go to the nearest hospital emergency room right away.
What should I avoid while taking SARAFEM?
SARAFEM can cause sleepiness or may affect your ability to make decisions, think clearly, or react quickly. You should not drive, operate heavy machinery, or do other dangerous activities until you know how SARAFEM affects you. Do not drink alcohol while using SARAFEM.
What are the possible side effects of SARAFEM?
SARAFEM may cause serious side effects, including:
- See “What is the most important information I should know about SARAFEM?”
-
Problems with blood sugar control. Women who have diabetes and take SARAFEM may have problems with low blood sugar while taking SARAFEM. High blood sugar can happen when SARAFEM is stopped. Your healthcare provider may need to change the dose of your diabetes medicines when you start or stop taking SARAFEM.
- Feeling anxious or trouble sleeping
The most common side effects of SARAFEM include:
- headache
- weakness (asthenia)
- pain
- accidental injury
- infection
- flu symptoms
- nausea
- diarrhea
- trouble sleeping (insomnia)
- dizziness
- feeling anxious or nervous
- thinking differently
- sexual problems
- runny or stuffy nose (rhinitis)
- sore throat (pharyngitis)
Tell your healthcare provider if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of SARAFEM. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store SARAFEM?
- Store SARAFEM at room temperature between 68° F and 77° F (20° C to 25° C).
Keep SARAFEM and all medicines out of the reach of children.
General information about SARAFEM
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use SARAFEM for a condition for which it was not prescribed. Do not give SARAFEM to other people, even if they have the same condition. It may harm them.
This Medication Guide summarizes the most important information about SARAFEM. If you would like more information, talk with your healthcare provider. You may ask your healthcare provider or pharmacist for information about SARAFEM that is written for healthcare professionals.
For more information about SARAFEM call 1-800-678-1605.
What are the ingredients in SARAFEM?
Active ingredient: fluoxetine hydrochloride
Inactive ingredients: microcrystalline cellulose, croscarmellose sodium, colloidal silicon dioxide, magnesium stearate, FD&C Yellow No. 6 aluminum lake (10 mg and 20 mg tablets) and D&C Yellow No. 10 aluminum lake (10 mg and 20 mg tablets)
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Distributed by:
Allergan USA, Inc.
Irvine, CA 92612
Sarafem® is a registered trademark of Allergan Pharmaceuticals International Limited
© 2016 Allergan. All rights reserved.
01/2017
| SARAFEM
fluoxetine hydrochloride tablet |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| SARAFEM
fluoxetine hydrochloride tablet |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| SARAFEM
fluoxetine hydrochloride tablet |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Allergan, Inc. (144796497) |
Frequently asked questions
- SSRIs vs SNRIs - What's the difference between them?
- Is Prozac (fluoxetine) safe for dogs?
- Prozac vs Zoloft - What are the Differences & Similarities?
- What are some common side effects of antidepressants?
- Taking fluoxetine, what can I use for a bad cough from cold or strep throat?
More about fluoxetine
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (2,203)
- Drug images
- Side effects
- Dosage information
- Patient tips
- During pregnancy
- Support group
- Drug class: selective serotonin reuptake inhibitors
- Breastfeeding
Patient resources
Professional resources
- FLUoxetine monograph
- Fluoxetine (FDA)
- Fluoxetine Capsules (FDA)
- Fluoxetine Delayed Release Capsules (FDA)
- Fluoxetine Solution (FDA)
Other brands
Prozac, Sarafem, Prozac Weekly