Hizentra Prescribing Information
Package insert / product label
Generic name: human immunoglobulin g
Dosage form: subcutaneous infusion
Drug class: Immune globulins
J Code (medical billing code): J1555 (100 mg, injection)
Medically reviewed by Drugs.com. Last updated on May 4, 2023.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- References
- How Supplied/Storage and Handling
- Storage and Handling
- Patient Counseling Information
Highlights of Prescribing Information
HIZENTRA, Immune Globulin Subcutaneous (Human), 20% Liquid
Initial U.S. Approval: 2010
WARNING: THROMBOSIS
See full prescribing information for complete boxed warning.
- Thrombosis may occur with immune globulin products, including HIZENTRA. Risk factors may include: advanced age, prolonged immobilization, hypercoagulable conditions, history of venous or arterial thrombosis, use of estrogens, indwelling vascular catheters, hyperviscosity, and cardiovascular risk factors.
- For patients at risk of thrombosis, administer HIZENTRA at the minimum dose and infusion rate practicable. Ensure adequate hydration in patients before administration. Monitor for signs and symptoms of thrombosis and assess blood viscosity in patients at risk for hyperviscosity.
Recent Major Changes
| Dosage and Administration (2.3) | 04/2023 |
Indications and Usage for Hizentra
HIZENTRA is an Immune Globulin Subcutaneous (Human) (IGSC), 20% Liquid indicated for the treatment of:
Hizentra Dosage and Administration
For subcutaneous infusion only.
Dose (2.2)
PI
Before switching to HIZENTRA, obtain the patient's serum IgG trough level to guide subsequent dose adjustments.
- Weekly: Start HIZENTRA 1 week after last Immune Globulin Intravenous (Human) (IGIV) infusion.
| Initial weekly dose = | Previous IGIV dose (in grams) × 1.37 |
| No. of weeks between IGIV doses |
- Biweekly (every 2 weeks): Start HIZENTRA 1 or 2 weeks after the last IGIV infusion or 1 week after the last weekly IGSC infusion. Administer twice the calculated weekly dose.
- Frequent dosing (2 to 7 times per week): Start HIZENTRA 1 week after the last IGIV or IGSC infusion. Divide the calculated weekly dose by the desired number of times per week.
- Adjust the dose based on clinical response and serum IgG trough levels.
CIDP
- Initiate therapy with HIZENTRA 1 week after the last IGIV infusion.
- Recommended subcutaneous dose is 0.2 g/kg (1 mL/kg) body weight per week.
- -
- In the clinical study after transitioning from IGIV to HIZENTRA, a dose of 0.4 g/kg (2 mL/kg) body weight per week was also safe and effective to prevent CIDP relapse.
- If CIDP symptoms worsen, on 0.2 g/kg (1 mL/kg) body weight per week, consider increasing the HIZENTRA dose from 0.2 g/kg to 0.4 g/kg body weight per week.
- -
- If CIDP symptoms worsen on 0.4 g/kg body weight per week, consider re-initiating therapy with IGIV, while discontinuing HIZENTRA.
- Monitor patient's clinical response and adjust duration of therapy based on patient need.
Administration (2.3)
- PI: Administer at regular intervals from daily up to every 2 weeks.
- CIDP: Administer weekly.
- Infusion sites – Up to 8 infusion sites are allowed simultaneously, with at least 2 inches between sites.
Dosage Forms and Strengths
0.2 g per mL (20%) protein solution for subcutaneous infusion available in a single-dose prefilled syringe (5 mL, 10 mL, 20 mL, and 50 mL) or tamper-evident vial (5 mL, 10 mL, 20 mL and 50 mL). (3)
Contraindications
Warnings and Precautions
- IgA-deficient patients with anti-IgA antibodies are at greater risk of severe hypersensitivity and anaphylactic reactions. (5.1)
- Thrombosis may occur following treatment with immune globulin products, including HIZENTRA. (5.2)
- Aseptic meningitis syndrome has been reported with IGIV or IGSC, including HIZENTRA treatment. (5.3)
- Monitor renal function, including blood urea nitrogen, serum creatinine, and urine output in patients at risk of acute renal failure. (5.4)
- Monitor for clinical signs and symptoms of hemolysis. (5.5)
- Monitor for pulmonary adverse reactions (transfusion-related acute lung injury [TRALI]). (5.6)
- HIZENTRA is made from human blood and may contain infectious agents, e.g., viruses, the variant Creutzfeldt-Jakob disease (vCJD) agent and, theoretically, the Creutzfeldt-Jakob disease (CJD) agent. (5.7)
Adverse Reactions/Side Effects
The most common adverse reactions observed in ≥5% of study subjects were local infusion site reactions, headache, diarrhea, fatigue, back pain, nausea, pain in extremity, cough, upper respiratory tract infection, rash, pruritus, vomiting, abdominal pain (upper), migraine, arthralgia, pain, fall and nasopharyngitis. (6)
To report SUSPECTED ADVERSE REACTIONS, contact CSL Behring Pharmacovigilance at 1-866-915-6958 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 4/2023
Full Prescribing Information
WARNING: THROMBOSIS
- Thrombosis may occur with immune globulin products1-3, including HIZENTRA. Risk factors may include: advanced age, prolonged immobilization, hypercoagulable conditions, history of venous or arterial thrombosis, use of estrogens, indwelling central vascular catheters, hyperviscosity, and cardiovascular risk factors. Thrombosis may occur in the absence of known risk factors [see Warnings and Precautions (5.2), and Patient Counseling Information (17).
- For patients at risk of thrombosis, administer HIZENTRA at the minimum dose and infusion rate practicable. Ensure adequate hydration in patients before administration. Monitor for signs and symptoms of thrombosis and assess blood viscosity in patients at risk for hyperviscosity [see Warnings and Precautions (5.2)].
1. Indications and Usage for Hizentra
HIZENTRA is an Immune Globulin Subcutaneous (Human) (IGSC), 20% Liquid indicated for the treatment of the following conditions:
1.1 Primary Immunodeficiency (PI)
HIZENTRA is indicated as replacement therapy for primary humoral immunodeficiency (PI) in adults and pediatric patients 2 years of age and older. This includes, but is not limited to, the humoral immune defect in congenital agammaglobulinemia, common variable immunodeficiency, X-linked agammaglobulinemia, Wiskott-Aldrich syndrome, and severe combined immunodeficiencies.
1.2 Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
HIZENTRA is indicated for the treatment of adult patients with chronic inflammatory demyelinating polyneuropathy (CIDP) as maintenance therapy to prevent relapse of neuromuscular disability and impairment.
Limitations of Use:
HIZENTRA maintenance therapy in CIDP has been systematically studied for 6 months and for a further 12 months in a follow-up study. Maintenance therapy beyond these periods should be individualized based upon the patient's response and need for continued therapy [see Dosage and Administration (2)].
2. Hizentra Dosage and Administration
For subcutaneous infusion only.
2.1 Preparation and Handling
HIZENTRA is a clear and pale yellow to light brown solution. Do not use if the solution is cloudy or contains particulates.
- Prior to administration, visually inspect each prefilled syringe or vial of HIZENTRA for particulate matter or discoloration, whenever the solution and container permit.
- Do not freeze. Do not use any solution that has been frozen.
- Check the product expiration date on the prefilled syringe or vial label. Do not use beyond the expiration date.
- Do not mix HIZENTRA with other products.
- Do not shake the prefilled syringe or vial.
- Use aseptic technique when preparing and administering this product.
- Both the HIZENTRA prefilled syringe and vial are single-dose containers. Multiple HIZENTRA prefilled syringes or vials can be administered to achieve the prescribed dose. Discard all used administration supplies and any unused product immediately after each infusion in accordance with local requirements.
2.2 Dose
Primary Immunodeficiency (PI)
- HIZENTRA can be administered at regular intervals from daily up to every 2 weeks (biweekly).
- Individualize the dose based on the patient's clinical response to HIZENTRA therapy and serum immunoglobulin G (IgG) trough levels.
- Before receiving treatment with HIZENTRA:
- Ensure that patients have received Immune Globulin Intravenous (Human) (IGIV) treatment at regular intervals for at least 3 months.
- Obtain the patient's serum IgG trough level to guide subsequent dose adjustments (see below, under Dose Adjustment).
Dosage for patients switching to HIZENTRA from IGIV
- Establish the initial weekly dose of HIZENTRA by converting the monthly IGIV dose into a weekly equivalent and increasing it using the dose adjustment factor. The goal is to achieve a systemic serum IgG exposure (area under the concentration-time curve [AUC]) not inferior to that of the previous IGIV treatment.
- To calculate the initial weekly dose of HIZENTRA, divide the previous IGIV dose in grams by the number of weeks between doses during the patient's IGIV treatment (e.g., 3 or 4); then multiply this by the dose adjustment factor of 1.37 [see Clinical Pharmacology (12.3, Table 9)].
Initial HIZENTRA dose = Previous IGIV dose (in grams) × 1.37 Number of weeks between IGIV doses - To convert the HIZENTRA dose (in grams) to milliliters (mL), multiply the calculated dose (in grams) by 5.
- To calculate the initial weekly dose of HIZENTRA, divide the previous IGIV dose in grams by the number of weeks between doses during the patient's IGIV treatment (e.g., 3 or 4); then multiply this by the dose adjustment factor of 1.37 [see Clinical Pharmacology (12.3, Table 9)].
- Provided the total weekly dose is maintained, any dosing interval from daily up to biweekly can be used and will result in systemic serum IgG exposure that is comparable to the previous IGIV or weekly HIZENTRA treatment [see Clinical Pharmacology (12.3)].
- For biweekly dosing, multiply the calculated HIZENTRA weekly dose by 2.
- For frequent dosing (2 to 7 times per week), divide the calculated weekly dose by the desired number of times per week (e.g., for 3 times per week dosing, divide weekly dose by 3).
Dosage for patients switching to HIZENTRA from IGSC
- The previous weekly IGSC dose should be maintained.
- For biweekly dosing, multiply the previous weekly dose by 2.
- For frequent dosing (2 to 7 times per week), divide the previous weekly dose by the desired number of times per week (e.g., for 3 times per week dosing, divide weekly dose by 3).
Start HIZENTRA treatment
- For weekly or frequent dosing, start treatment with HIZENTRA 1 week after the patient's last IGIV infusion or IGSC infusion.
- For biweekly dosing, start treatment 1 or 2 weeks after the last IGIV infusion or 1 week after the last weekly IGSC infusion.
Dose Adjustment
The dose may need to be adjusted to achieve the desired clinical response and serum IgG trough level, irrespective of the frequency of administration.
To determine if a dose adjustment should be considered, measure the patient's serum IgG trough level 2 to 3 months after switching to HIZENTRA.
Weekly dosing: When switching from IGIV to weekly HIZENTRA dosing, the target serum IgG trough level is projected to be approximately 16% higher than the last trough level during prior IGIV therapy [see Clinical Pharmacology (12.3)].
Biweekly dosing: When switching from IGIV to biweekly HIZENTRA dosing, the target serum IgG trough level is projected to be approximately 10% higher than the last IGIV trough level. When switching from weekly to biweekly dosing, the target trough is projected to be approximately 5% lower than the last trough level on weekly therapy [see Clinical Pharmacology (12.3)].
Frequent dosing: When switching from weekly dosing to more frequent dosing, the target serum IgG trough level is projected to be approximately 3 to 4% higher than the last trough level on weekly therapy [see Clinical Pharmacology (12.3)].
To adjust the dose based on serum trough levels, calculate the difference (in mg/dL) between the patient's IgG trough level obtained 2 to 3 months following the switch from IGIV or the last IGSC dose adjustment and the target IgG trough level for weekly or biweekly dosing. Then find this difference in Table 1 (Column 1) and, based on the HIZENTRA dosing frequency (for weekly or biweekly) and the patient's body weight, locate the corresponding adjustment amount (in mL) by which to increase (or decrease) the dose. For frequent dosing, add the weekly increment from Table 1 to the weekly-equivalent dose and then divide by the number of days of dosing.
Use the patient's clinical response as the primary consideration in dose adjustment. Additional dosage increments may be indicated based on the patient's clinical response (infection frequency and severity).
| Difference From Target Serum IgG Trough Level (mg/dL) | Dosing Frequency | Weight Adjusted Dose Increment (mL)* | ||||
|---|---|---|---|---|---|---|
| Weight Group | ||||||
| >10 to ≤30 kg | >30 to ≤50 kg | >50 to ≤70 kg | >70 to ≤90 kg | >90 kg | ||
| n/a, not applicable. | ||||||
|
||||||
| 50 | Weekly‡ | n/a | 2.5 | 5 | 5 | 10 |
| Biweekly | 5 | 5 | 10 | 10 | 20 | |
| 100 | Weekly‡ | 2.5 | 5 | 10 | 10 | 15 |
| Biweekly | 5 | 10 | 20 | 20 | 30 | |
| 200 | Weekly‡ | 5 | 10 | 15 | 20 | 30 |
| Biweekly | 10 | 20 | 30 | 40 | 60 | |
For example, if a patient with a body weight of 70 kg has an actual IgG trough level of 900 mg/dL and the target trough level is 1000 mg/dL, this results in a difference of 100 mg/dL. Therefore, increase the weekly dose of HIZENTRA by 10 mL. For biweekly dosing, increase the biweekly dose by 20 mL. For 2 times per week dosing, increase the dose by 5 mL.
Monitor the patient's clinical response, and repeat the dose adjustment as needed.
Dosage requirements for patients switching to HIZENTRA from another IGSC product: If a patient on HIZENTRA does not maintain an adequate clinical response or a serum IgG trough level equivalent to that of the previous IGSC treatment, the physician may want to adjust the dose. For such patients, Table 1 also provides guidance for dose adjustment if their desired IGSC trough level is known.
Measles Exposure
Administer a minimum total weekly HIZENTRA dose of 0.2 g/kg body weight for 2 consecutive weeks if a patient is at risk of measles exposure (i.e., due to an outbreak in the U.S. or travel to endemic areas outside of the U.S.). For biweekly dosing, one infusion of a minimum at 400 mg/kg is recommended. If a patient has been exposed to measles, ensure this minimum dose is administered as soon as possible after exposure.
Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
- Initiate therapy with HIZENTRA 1 week after the last IGIV infusion.
- The recommended subcutaneous dose is 0.2 g/kg (1 mL/kg) body weight per week, administered in 1 or 2 sessions over 1 or 2 consecutive days.
- -
- In the clinical study after transitioning from IGIV to HIZENTRA treatment, a dose of 0.4 g/kg (2 mL/kg) body weight per week was also safe and effective in preventing CIDP relapse.
- If CIDP symptoms worsen on 0.2 g/kg (1 mL/kg) body weight per week, consider increasing the HIZENTRA dose from 0.2 g/kg (1 mL/kg) to 0.4 g/kg (2 mL/kg) body weight per week, administered in 2 sessions per week over 1 or 2 consecutive days.
- -
- If CIDP symptoms worsen on the 0.4 g/kg body weight per week dose, consider re-initiating therapy with an IGIV product approved for treatment of CIDP, while discontinuing HIZENTRA.
- Monitor the patient's clinical response and adjust the duration of therapy based on patient need.
2.3 Administration
HIZENTRA is for subcutaneous infusion only.
HIZENTRA is intended for subcutaneous administration using an infusion pump. Infuse HIZENTRA in the abdomen, thigh, upper arm, and/or lateral hip.
- Infusion sites – A HIZENTRA dose may be infused into multiple infusion sites. Use up to 8 infusion sites in parallel. More than one infusion device can be used simultaneously. Infusion sites should be at least 2 inches apart. Change the actual site of infusion with each administration.
- Volume (as tolerated) – For the first infusion of HIZENTRA, do not exceed a volume of 15 mL per infusion site in patients with PI or up to 20 mL per infusion site in patients with CIDP. For subsequent infusions, the volume may be increased to 25 mL per infusion site for patients with PI or to 50 mL per site for patients with CIDP.
- Rate (as tolerated) – For the first infusion of HIZENTRA, the recommended flow rate is up to 15 mL per hour per infusion site in patients with PI or up to 20 mL per hour per site in patients with CIDP. For subsequent infusions, the flow rate may be increased to 25 mL per hour per site in patients with PI or up to 50 mL per hour per site in patients with CIDP.
Follow the steps below and use aseptic technique to administer HIZENTRA, either as prefilled syringe(s) or vial(s).
- 1.
- Assemble supplies Gather the HIZENTRA prefilled syringe(s) or vial(s), all supplies, and infusion log book.
- 2.
- Clean surface Clean a table or other flat surface.
- 3.
-
Wash hands – Thoroughly wash and dry hands (Figure 1).

Figure 1
- 4.
-
Check prefilled syringe(s) or vial(s):
-
If using prefilled syringes, carefully peel back the transparent covering from the tray and inspect the protective cap. Peel back the outer layer of the wrap-around label to allow for viewing of HIZENTRA through the fully transparent inner layer, but don't remove the label completely (Figure 2).

Figure 2
- If using vials, inspect the protective cap of the vials (Figure 3).
Figure 3
-
If using prefilled syringes, carefully peel back the transparent covering from the tray and inspect the protective cap. Peel back the outer layer of the wrap-around label to allow for viewing of HIZENTRA through the fully transparent inner layer, but don't remove the label completely (Figure 2).
Carefully inspect each prefilled syringe(s) or vial(s) of HIZENTRA. HIZENTRA is a clear and pale yellow to light brown solution. Do not use the prefilled syringe or vial if damaged, the liquid looks cloudy, contains particles, has changed color, the protective cap of the prefilled syringe or the vial is missing or defective, or the expiration date on the label has passed.
- 5.
-
Prepare HIZENTRA for infusion
If using HIZENTRA prefilled syringes, go to Step 5.1
If using HIZENTRA vials, go to Step 5.2 - 5.1
-
HIZENTRA prefilled syringe(s)
- The 5 mL, 10 mL, 20 mL, and 50 mL prefilled syringes are supplied and ready to use. The 5 mL and 10 mL prefilled syringes are fully assembled (Figure 4). For the 20 mL and 50 mL prefilled syringes, screw the plunger rod onto the prefilled syringe stopper prior to use (Figure 5).

Figure 4

Figure 5
- HIZENTRA prefilled syringes can be placed directly in the infusion pump if the prefilled syringe size matches the pump requirements. If the prefilled syringe can be placed directly in the infusion pump, then go to Step 6.
NOTE:
An additional adapter may be required for the HIZENTRA prefilled syringes to fit properly in the infusion pump. Check with the provider of your supplies for the appropriate adapter and installation instructions. - If the HIZENTRA prefilled syringe size does not match the infusion pump requirements, transfer the contents of the prefilled syringe to another syringe of a size specific for the infusion pump by following the directions below:
- Use a syringe-to-syringe transfer device (tip-to-tip connector) (Figure 6) to transfer the contents of the prefilled syringe to the empty syringe specific for the infusion pump.

Figure 6
- Remove the protective cap from the prefilled syringe. Attach the transfer device (tip-to-tip connector) by twisting it onto the prefilled syringe. Attach the empty syringe by screwing it onto the other side of the transfer device (Figure 7).

Figure 7
- Make sure you transfer the amount needed to achieve the prescribed dose.
- Measure dose from the top of the stopper
- Push the plunger of the prefilled syringe (e.g., using your fingers, thumb or the palm of your hand) to transfer HIZENTRA from the prefilled syringe to the empty syringe.
- Repeat this step if multiple prefilled syringes are necessary to achieve the prescribed dose. Remove the emptied prefilled syringe and attach another prefilled syringe to the transfer device (tip-to-tip connector).
- After the transfer is complete, remove the emptied prefilled syringe and the transfer device (tip-to-tip connector) by unscrewing them from the syringe specific for your pump. Connect the filled syringe to the infusion tubing.
- Use a syringe-to-syringe transfer device (tip-to-tip connector) (Figure 6) to transfer the contents of the prefilled syringe to the empty syringe specific for the infusion pump.
- The 5 mL, 10 mL, 20 mL, and 50 mL prefilled syringes are supplied and ready to use. The 5 mL and 10 mL prefilled syringes are fully assembled (Figure 4). For the 20 mL and 50 mL prefilled syringes, screw the plunger rod onto the prefilled syringe stopper prior to use (Figure 5).
Go to Step 6.
- 5.2
-
Transfer HIZENTRA from vial to syringe
- Take the protective cap off the vial (Figure 8).

Figure 8
- Clean the vial stopper with an alcohol wipe (Figure 9). Let the stopper dry.

Figure 9
- If using a transfer device, follow the instructions provided by the device manufacturer.
- If using a needle and a syringe to transfer HIZENTRA, follow the instructions below:
- Attach a sterile transfer needle to a sterile syringe (Figure 10).
Figure 10
- Pull out the plunger of the syringe to fill the syringe with air. Make sure that the amount of air is the same as the amount of HIZENTRA you will transfer from the vial.
- Put the HIZENTRA vial on a flat surface. Keeping the vial upright, insert the transfer needle into the center of the rubber stopper.
- Check that the tip of the needle is not in the liquid. Then, push the plunger of the syringe down. This will inject the air from the syringe into the airspace of the vial.
- Leaving the needle in the stopper, carefully turn the vial upside down (Figure 11).
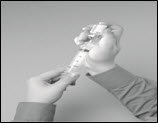
Figure 11
- Slowly pull back on the plunger of the syringe to fill the syringe with HIZENTRA.
- Take the filled syringe and needle out of the stopper.
- Take off the needle and throw it away in the sharps container.
- Attach a sterile transfer needle to a sterile syringe (Figure 10).
- Take the protective cap off the vial (Figure 8).
When using multiple vials to achieve the prescribed dose, repeat this step.
- 6.
-
Prepare infusion pump and tubing
- Prior to preparing the pump(s), make sure you have the prescribed dose in the syringe(s) and the infusion tubing is attached.
- Prepare the infusion pump following the manufacturer's instructions, including attaching any necessary adapters.
- Do not remove the needle caps until you are ready to infuse.
- Prime (fill) the infusion. To prime the tubing, connect the syringe filled with HIZENTRA to the infusion tubing and gently push on the syringe plunger (e.g., using your fingers or thumb or the palm of your hand) to fill the tubing with HIZENTRA (Figure 12).
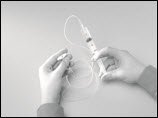
Figure 12
- Stop priming before HIZENTRA fluid reaches the capped needle.
- Insert the syringe filled with HIZENTRA into the infusion pump.
- Prime (fill) the infusion. To prime the tubing, connect the syringe filled with HIZENTRA to the infusion tubing and gently push on the syringe plunger (e.g., using your fingers or thumb or the palm of your hand) to fill the tubing with HIZENTRA (Figure 12).
- 7.
-
Prepare infusion site(s)
- Select an area on your abdomen, thigh, upper arm, or side of upper leg/hip for the infusion (Figure 13).The number and location of infusion sites depends on the volume of the total dose.

Figure 13
- Never infuse into areas where the skin is tender, bruised, red, or hard. Avoid infusing into scars or stretch marks.
- Infuse HIZENTRA into a maximum of 8 sites simultaneously; or up to 12 consecutively per infusion. Infusion sites should be at least 2 inches apart.
- Clean the skin at each infusion site with an antiseptic skin prep (Figure 14). Let the skin dry.
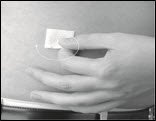
Figure 14
- Select an area on your abdomen, thigh, upper arm, or side of upper leg/hip for the infusion (Figure 13).The number and location of infusion sites depends on the volume of the total dose.
- 8.
-
Insert needle(s)
- Use just one needle per site. If injecting in more than one site, the following steps should be completed for each needle, one at a time:
- Remove the needle cap.
- Using 2 fingers, pinch together the skin around the infusion site. With a quick dart-like motion, insert the needle straight into the skin (Figure 15).
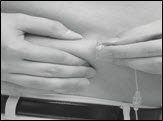
Figure 15
- Put sterile gauze and tape or a transparent dressing over the infusion site (Figure 16) to hold the needle in place.
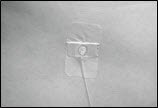
Figure 16
- 9.
-
Start infusion
- Follow the manufacturer's instructions to turn on the infusion pump and start the infusion (Figure 17).

Figure 17
- Follow the manufacturer's instructions to turn on the infusion pump and start the infusion (Figure 17).
- 10.
-
Complete infusion and record treatment (Figure 18)
- When all the HIZENTRA has been infused, turn off the infusion pump.
- Remove the needle(s) from the skin.
- Once you have removed the needle(s), remove the empty syringe from the infusion pump.
- Disconnect the infusion set from the empty syringe.
- Cover the infusion site(s) with a protective dressing.
- Peel-off the removable part of the label for each prefilled syringe or vial used Affix it to the patient's log book with the date and time of infusion, or scan the prefilled syringe or vial if recording the infusion electronically.

Figure 18
- 11.
-
Clean up
- If applicable, remove adapter from the infusion pump following the manufacturer's instructions.
- Throw away the empty HIZENTRA prefilled syringe(s) or vial(s), along with the used disposable supplies in the sharps container (Figure 19) in accordance with local requirements.
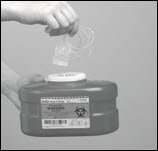
Figure 19
- Clean and store the infusion pump, following the manufacturer's instructions.
For self-administration, provide the patient with instructions and training for subcutaneous infusion in the home or other appropriate setting.
3. Dosage Forms and Strengths
HIZENTRA is a 0.2 g/mL (20%) protein solution for subcutaneous infusion available in a single-dose, prefilled syringe (5 mL, 10 mL, 20 mL, and 50 mL) or tamper-evident vial (5 mL, 10 mL, 20 mL and 50 mL).
4. Contraindications
HIZENTRA is contraindicated in patients with:
- History of anaphylactic or severe systemic reaction to human immune globulin or inactive ingredients of HIZENTRA, such as polysorbate 80.
- Hyperprolinemia Type I or II because it contains L-proline as a stabilizer [see Description (11)].
- IgA-deficiency with antibodies against IgA and a history of hypersensitivity [see Description (11)].
5. Warnings and Precautions
5.1 Hypersensitivity
Severe hypersensitivity reactions may occur to human immune globulin or components of HIZENTRA, such as polysorbate 80. If a hypersensitivity reaction occurs, discontinue the HIZENTRA infusion immediately and institute appropriate treatment.
Individuals with IgA deficiency can develop anti-IgA antibodies and anaphylactic reactions (including anaphylaxis and shock) after administration of blood components containing IgA. Patients with known antibodies to IgA may have a greater risk of developing potentially severe hypersensitivity and anaphylactic reactions with administration of HIZENTRA. HIZENTRA contains ≤50 mcg/mL IgA [see Description (11)].
5.2 Thrombosis
Thrombosis may occur following treatment with immune globulin products1-3, including HIZENTRA. Risk factors may include: advanced age, prolonged immobilization, hypercoagulable conditions, history of venous or arterial thrombosis, use of estrogens, indwelling central vascular catheters, hyperviscosity, and cardiovascular risk factors. Thrombosis may occur in the absence of known risk factors.
Consider baseline assessment of blood viscosity in patients at risk for hyperviscosity, including those with cryoglobulins, fasting chylomicronemia/markedly high triglycerides, or monoclonal gammopathies. For patients at risk of thrombosis, administer HIZENTRA at the minimum dose and infusion rate practicable. Ensure adequate hydration in patients before administration. Monitor for signs and symptoms of thrombosis and assess blood viscosity in patients at risk for hyperviscosity [see Boxed Warning, Dosage and Administration (2) and Patient Counseling Information (17)].
5.3 Aseptic Meningitis Syndrome (AMS)
AMS has been reported with use of IGIV4 or IGSC, including HIZENTRA. The syndrome usually begins within several hours to 2 days following immune globulin treatment. AMS is characterized by the following signs and symptoms: severe headache, nuchal rigidity, drowsiness, fever, photophobia, painful eye movements, nausea, and vomiting. Cerebrospinal fluid (CSF) studies frequently show pleocytosis up to several thousand cells per cubic millimeter, predominantly from the granulocytic series, and elevated protein levels up to several hundred mg/dL. AMS may occur more frequently in association with high doses (≥2 g/kg) and/or rapid infusion of immune globulin product.
Patients exhibiting such signs and symptoms should receive a thorough neurological examination, including CSF studies, to rule out other causes of meningitis. Discontinuation of immune globulin treatment has resulted in remission of AMS within several days without sequelae.
5.4 Renal Dysfunction/Failure
Acute renal dysfunction/failure, acute tubular necrosis, proximal tubular nephropathy, osmotic nephrosis and death may occur with use of human immune globulin products, especially those containing sucrose.5 HIZENTRA does not contain sucrose. Ensure that patients are not volume depleted before administering HIZENTRA.
For patients judged to be at risk for developing renal dysfunction, including patients with any degree of pre-existing renal insufficiency, diabetes mellitus, age greater than 65, volume depletion, sepsis, paraproteinemia, or patients receiving known nephrotoxic drugs, monitor renal function and consider lower, more frequent dosing [see Dosage and Administration (2)].
Periodic monitoring of renal function and urine output is particularly important in patients judged to have a potential increased risk of developing acute renal failure.6 Assess renal function, including measurement of blood urea nitrogen (BUN) and serum creatinine, before the initial infusion of HIZENTRA and at appropriate intervals thereafter. If renal function deteriorates, consider discontinuing HIZENTRA.
5.5 Hemolysis
HIZENTRA can contain blood group antibodies that may act as hemolysins and induce in vivo coating of red blood cells (RBCs) with immunoglobulin, causing a positive direct antiglobulin (Coombs') test result and hemolysis.7,9 Delayed hemolytic anemia can develop subsequent to immune globulin therapy due to enhanced RBC sequestration, and acute hemolysis, consistent with intravascular hemolysis, has been reported.10
Monitor recipients of HIZENTRA for clinical signs and symptoms of hemolysis. If signs and/or symptoms of hemolysis are present after HIZENTRA infusion, perform appropriate confirmatory laboratory testing.
5.6 Transfusion-Related Acute Lung Injury (TRALI)
Noncardiogenic pulmonary edema may occur in patients administered human immune globulin products.11 TRALI is characterized by severe respiratory distress, pulmonary edema, hypoxemia, normal left ventricular function, and fever. Typically, it occurs within 1 to 6 hours following transfusion. Patients with TRALI may be managed using oxygen therapy with adequate ventilatory support.
Monitor HIZENTRA recipients for pulmonary adverse reactions. If TRALI is suspected, perform appropriate tests for the presence of anti-neutrophil antibodies in both the product and patient's serum.
5.7 Transmissible Infectious Agents
Because HIZENTRA is made from human blood, it may carry a risk of transmitting infectious agents, e.g., viruses, the variant Creutzfeldt-Jakob disease (vCJD) agent and, theoretically, the Creutzfeldt-Jakob disease (CJD) agent. This also applies to unknown or emerging viruses and other pathogens. No cases of transmission of viral diseases or CJD have been associated with the use of HIZENTRA. All infections suspected by a physician possibly to have been transmitted by HIZENTRA should be reported to CSL Behring Pharmacovigilance at 1-866-915-6958.
6. Adverse Reactions/Side Effects
The most common adverse reactions (ARs) observed in ≥5% of study subjects receiving HIZENTRA were local reactions (e.g., swelling, redness, heat, pain, hematoma and itching at the infusion site), headache, diarrhea, fatigue, back pain, nausea, pain in extremity, cough, upper respiratory tract infection, rash, pruritus, vomiting, abdominal pain (upper), migraine, arthralgia, pain, fall and nasopharyngitis.
6.1 Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, AR rates observed in clinical studies of a product cannot be directly compared to rates in the clinical studies of another product and may not reflect the rates observed in clinical practice.
Treatment of Primary Immunodeficiency (PI)
PI U.S. Study
The safety of HIZENTRA was evaluated in a clinical study in the U.S. for 15 months (3-month wash-in/wash-out period followed by a 12-month efficacy period) in subjects with PI who had been treated previously with IGIV every 3 or 4 weeks. The safety analyses included 49 subjects in the intention-to-treat (ITT) population. The ITT population consisted of all subjects who received at least one dose of HIZENTRA [see Clinical Studies (14)].
Subjects were treated with HIZENTRA at weekly median doses ranging from 66 to 331 mg/kg body weight (mean: 181.4 mg/kg) during the wash-in/wash-out period and from 72 to 379 mg/kg (mean: 213.2 mg/kg) during the efficacy period. The 49 subjects received a total of 2264 weekly infusions of HIZENTRA.
Table 2 summarizes the most frequent adverse reactions (ARs) (experienced by at least 2 subjects) occurring during or within 72 hours after the end of an infusion. Local reactions were assessed by the investigators 15 to 45 minutes post-infusion and by the subjects 24 hours post-infusion. The investigators then evaluated the ARs arising from the subject assessments. Local reactions were the most frequent ARs observed, with infusion-site reactions (e.g., swelling, redness, heat, pain, and itching at the site of infusion) comprising 98% of local reactions.
| ARs* Occurring During or Within 72 Hours of Infusion | ||
|---|---|---|
| AR (≥2 Subjects) | Number (%) of Subjects (n=49) | Number (Rate†) of ARs (n=2264 Infusions) |
| Local reactions‡ | 49 (100) | 1322 (0.584) |
| Other ARs: | ||
| Headache | 12 (24.5) | 32 (0.014) |
| Diarrhea | 5 (10.2) | 6 (0.003) |
| Fatigue | 4 (8.2) | 4 (0.002) |
| Back pain | 4 (8.2) | 5 (0.002) |
| Nausea | 4 (8.2) | 4 (0.002) |
| Pain in extremity | 4 (8.2) | 6 (0.003) |
| Cough | 4 (8.2) | 4 (0.002) |
| Vomiting | 3 (6.1) | 3 (0.001) |
| Abdominal pain, upper | 3 (6.1) | 3 (0.001) |
| Migraine | 3 (6.1) | 4 (0.002) |
| Pain | 3 (6.1) | 4 (0.002) |
| Arthralgia | 2 (4.1) | 3 (0.001) |
| Contusion | 2 (4.1) | 3 (0.001) |
| Rash | 2 (4.1) | 3 (0.001) |
| Urticaria | 2 (4.1) | 2 (<0.001) |
The ratio of infusions with ARs, including local reactions, to all infusions was 1303 to 2264 (57.6%). Excluding local reactions, the corresponding ratio was 56 to 2264 (2.5%).
Table 3 summarizes infusion-site reactions based on investigator assessments 15 to 45 minutes after the end of the 683 infusions administered during regularly scheduled visits (every 4 weeks).
| Infusion-Site Reaction | Number† (Rate‡) of Reactions (n=683 Infusions§) |
|---|---|
|
|
| Edema/induration | 467 (0.68) |
| Erythema | 346 (0.51) |
| Local heat | 108 (0.16) |
| Local pain | 88 (0.13) |
| Itching | 64 (0.09) |
Most local reactions were either mild (does not interfere with routine activities [93.4%]) or moderate (interferes somewhat with routine activities and may have warranted intervention [6.3%]) in intensity.
No deaths or serious ARs occurred during the study. Two subjects withdrew from the study due to ARs. One subject experienced a severe infusion-site reaction one day after the third weekly infusion, and the other subject experienced moderate myositis.
PI European Study
In a clinical study conducted in Europe, the safety of HIZENTRA was evaluated for 10 months (3-month wash-in/wash-out period followed by a 7-month efficacy period) in 51 subjects with PI who had been treated previously with IGIV every 3 or 4 weeks or with IGSC weekly.
Subjects were treated with HIZENTRA at weekly median doses ranging from 59 to 267 mg/kg body weight (mean: 118.8 mg/kg) during the wash-in/wash-out period and from 59 to 243 mg/kg (mean: 120.1 mg/kg) during the efficacy period. The 51 subjects received a total of 1831 weekly infusions of HIZENTRA.
Table 4 summarizes the most frequent ARs (experienced by at least 2 subjects) occurring during or within 72 hours after the end of an infusion. Local reactions were assessed by the subjects between 24 and 72 hours post-infusion. The investigators then evaluated the ARs arising from the subject assessments.
| ARs* Occurring During or Within 72 Hours of Infusion | ||
|---|---|---|
| AR (≥2 Subjects) | Number (%) of Subjects (n=51) | Number (Rate†) of ARs (n=1831 Infusions) |
| Local reactions‡ | 24 (47.1) | 105 (0.057) |
| Other ARs: | ||
| Headache | 9 (17.6) | 20 (0.011) |
| Rash | 4 (7.8) | 4 (0.002) |
| Pruritus | 4 (7.8) | 13 (0.007) |
| Fatigue | 3 (5.9) | 5 (0.003) |
| Abdominal pain, upper | 2 (3.9) | 3 (0.002) |
| Arthralgia | 2 (3.9) | 2 (0.001) |
| Erythema | 2 (3.9) | 4 (0.002) |
| Abdominal discomfort | 2 (3.9) | 3 (0.002) |
| Back pain | 2 (3.9) | 2 (0.001) |
| Hematoma | 2 (3.9) | 3 (0.002) |
| Hypersensitivity | 2 (3.9) | 4 (0.002) |
The proportion of subjects reporting local reactions decreased over time from approximately 20% following the first infusion to <5% by the end of the study.
Three subjects withdrew from the study due to ARs of mild to moderate intensity. One subject experienced infusion-site pain and infusion-site pruritus; the second subject experienced infusion-site reaction, fatigue, and feeling cold; and the third subject experienced infusion-site reaction and hypersensitivity.
Biweekly (Every 2 Weeks) or Frequent (2 To 7 Times per Week) Dosing
No data regarding ARs are available for these alternative HIZENTRA dosing regimens because no clinical trials using these regimens were conducted.
Treatment of Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
PATH Study
The safety of 2 doses of HIZENTRA (0.2 g/kg body weight or 0.4 g/kg body weight) versus placebo was evaluated in the 24-week subcutaneous (SC) treatment period of the PATH (Polyneuropathy AND Treatment with Hizentra) study in subjects with CIDP who had been treated previously with IGIV [see Clinical Studies (14.2)]. The dose was administered once a week in 2 infusion sessions conducted on 1 or 2 consecutive day(s). The safety population included 172 subjects.
Table 5 summarizes the most frequent ARs that occurred in ≥5% of subjects treated with HIZENTRA and at a higher frequency than placebo. The overall AR rates were similar in the 0.2 g/kg body weight and 0.4 g/kg body weight HIZENTRA dose groups (50.9% and 46.6%, respectively) and higher than placebo (33.3%). The most frequent ARs were local infusion site reactions. Local reactions were more frequent among subjects who received the 0.4 g/kg body weight dose than among subjects who received the 0.2 g/kg body weight dose (29.3% and 19.3%, respectively). The exposure-adjusted rate of local reactions per subject remained greater in the 0.4 g/kg body weight dose group compared to the 0.2 g/kg body weight dose group after adjusting for the greater mean duration of exposure to HIZENTRA in the 0.4 g/kg body weight dose group (129 days) compared to that of the 0.2 g/kg body weight dose group (119 days). All local reactions were either mild (does not interfere with routine activities [94.5%]) or moderate (interferes somewhat with routine activities and may have warranted intervention [5.5%]) in intensity and the frequency tended to decrease over time. No subject withdrew because of local reaction.
One serious AR, allergic dermatitis was reported in the 0.2 g/kg body weight HIZENTRA group which started at SC Week 9 and lasted 15 days. One subject withdrew from the study due to a non-serious AR, fatigue.
| Placebo | 0.2 g/kg HIZENTRA | 0.4 g/kg HIZENTRA | ||||
|---|---|---|---|---|---|---|
| Number (%) of Subjects n=57 | Number of Events (Rate/Infusion) n=1514* | Number (%) of Subjects n=57 | Number of Events (Rate/Infusion) n=2007* | Number (%) of Subjects n=58 | Number of Events (Rate/Infusion) n=2218* |
|
| AR = adverse reaction; SC = subcutaneous. | ||||||
| Local Reactions† | 4 (7.0) | 7 (0.005) | 11 (19.3) | 54 (0.027) | 17 (29.3) | 49 (0.022) |
| Headache | 2 (3.5) | 2 (0.001) | 4 (7.0) | 5 (0.002) | 4 (6.9) | 4 (0.002) |
| Nasopharyngitis | 1 (1.8) | 1 (<0.001) | 4 (7.0) | 6 (0.003) | 2 (3.4) | 2 (<0.001) |
| Fatigue | 1 (1.8) | 1 (<0.001) | 5 (8.8) | 5 (0.002) | 0 | 0 |
| Upper respiratory tract infection | 2 (3.5) | 2 (0.001) | 3 (5.3) | 3 (0.001) | 2 (3.4) | 2 (<0.001) |
| Fall | 0 | 0 | 3 (5.3) | 8 (0.004) | 1 (1.7) | 1 (<0.001) |
| Back Pain | 1 (1.8) | 1 (<0.001) | 3 (5.3) | 4 (0.002) | 1 (1.7) | 1 (<0.001) |
| Arthralgia | 1 (1.8) | 1 (<0.001) | 3 (5.3) | 4 (0.002) | 1 (1.7) | 1 (<0.001) |
| Pain in Extremity | 0 | 0 | 1 (1.8) | 1 (<0.001) | 3 (5.2) | 3 (0.001) |
Hypertension was reported in 2 subjects (3.5%) in the 0.2 g/kg HIZENTRA group, 2 subjects (3.4%) in the 0.4 g/kg group, and zero subjects in the placebo group. Systemic adverse reactions in the 13-week IGIV Restabilization Period of the study for subjects also randomized and treated with HIZENTRA during the 24-week subcutaneous treatment period (N=115) occurred at a rate of 0.098 (956 infusions) relative to a rate of 0.027 (4225 infusions) during treatment with HIZENTRA in the IGSC period of the study. The systemic adverse reaction rate per infusion for HIZENTRA was 3.6-fold lower than the corresponding rate for IGIV.
The exposure-adjusted rate for systemic adverse reactions in the 13-week single-arm IGIV Restabilization Period of the study for subjects also randomized and treated with HIZENTRA during the 24-week subcutaneous treatment period (N=115) was 0.075 reactions per week, relative to an exposure-adjusted rate of 0.052 reactions per week during treatment with HIZENTRA in the IGSC period of the study. The exposure-adjusted systemic adverse reaction rate for HIZENTRA was 31% lower than the corresponding rate for IGIV. However, this difference should be interpreted with caution, because there was no parallel group of subjects receiving placebo during the period of IGIV treatment.
PATH Extension Study
The PATH Extension study was a multicenter, 48-week, open-label extension study that evaluated the long -term safety and efficacy of HIZENTRA 0.2 g/kg and 0.4 g/kg doses, per body weight, in the maintenance treatment of CIDP in subjects who either completed or were being successfully rescued from CIDP relapse with IGIV in the PATH study. A total of 82 subjects were enrolled. Of these, 66 (80.5%) subjects completed the study, and 16 (19.5%) subjects discontinued.
In the study, 30.1% of subjects in the HIZENTRA 0.2 g/kg group and 51.4% of subjects in the 0.4 g/kg group experienced adverse reactions. Similar to the PATH study, the most frequent ARs were local infusion site reactions, and local reactions were more frequent among subjects who received the 0.4 g/kg body weight dose than among subjects who received the 0.2 g/kg body weight dose (18.1% and 9.6%, respectively). Of all the local reactions, 1 subject had 3 severe reactions (interrupts routine activities or may require intensive therapeutic intervention [7.5%]) with the 0.4 g/kg dose; the rest were either mild (85.0%) or moderate (7.5%). Two subjects withdrew because of local reactions.
The total exposure was 25.1 subject years in the HIZENTRA 0.2 g/kg group and 38.7 subject years in the 0.4 g/kg group. The mean duration of exposure was 125.8 (range 1 to 330) days in the HIZENTRA 0.2 g/kg group and 196.1 (range 1 to 330) days in the 0.4 g/kg group.
6.2 Postmarketing Experience
Because postmarketing reporting of adverse reactions is voluntary and from a population of uncertain size, it is not always possible to reliably estimate the frequency of these reactions or establish a causal relationship to product exposure.
HIZENTRA
The following adverse reactions have been identified during postmarketing use of HIZENTRA. This list does not include reactions already reported in clinical studies with HIZENTRA [see Adverse Reactions (6.1)].
- Infusion reactions: Allergic-anaphylactic reactions such as swollen face or tongue and pharyngeal edema, pyrexia, chills, dizziness, hypertension/changes in blood pressure, malaise, tachycardia, flushing.
- Cardiovascular: Chest discomfort (including chest pain)
- Respiratory: Dyspnea
- Neurological: Tremor, burning sensation
- General disorders and administration site conditions: Infusion site ulcer, infusion site necrosis
Immune Globulin Products
The following adverse reactions have been reported during postmarketing use of immune globulin products:5
- Infusion reactions: Wheezing, rigors, myalgia
- Renal: Osmotic nephropathy
- Respiratory: Apnea, Acute Respiratory Distress Syndrome (ARDS), cyanosis, hypoxemia, pulmonary edema, bronchospasm
- Cardiovascular: Cardiac arrest, vascular collapse, hypotension
- Neurological: Coma, loss of consciousness, seizures, aseptic meningitis syndrome
- Integumentary: Stevens-Johnson syndrome, epidermolysis, erythema multiforme, dermatitis (e.g., bullous dermatitis)
- Hematologic: Pancytopenia, leukopenia, hemolysis, positive direct antiglobulin (Coombs') test
- Gastrointestinal: Hepatic dysfunction
To report SUSPECTED ADVERSE REACTIONS, contact CSL Behring Pharmacovigilance at 1-866-915-6958 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
7. Drug Interactions
7.1 Live Virus Vaccines
The passive transfer of antibodies with immunoglobulin administration may interfere with the response to live virus vaccines such as measles, mumps, rubella, and varicella [see Patient Counseling Information (17)].
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
No human data are available to indicate the presence or absence of drug-associated risk. Animal reproduction studies have not been conducted with HIZENTRA. It is not known whether HIZENTRA can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Immune globulins cross the placenta from maternal circulation increasingly after 30 weeks of gestation. HIZENTRA should be given to pregnant women only if clearly needed. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
8.2 Lactation
Risk Summary
No human data are available to indicate the presence or absence of drug-associated risk. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for HIZENTRA and any potential adverse effects on the breastfed infant from HIZENTRA or from the underlying maternal condition.
8.4 Pediatric Use
Treatment of Primary Immunodeficiency
Clinical Studies (Weekly Dosing)
The safety and effectiveness of weekly HIZENTRA have been established in the pediatric age groups 2 to 16. HIZENTRA was evaluated in 10 pediatric subjects with PI (3 children and 7 adolescents) in a study conducted in the U.S. [see Clinical Studies (14)] and in 23 pediatric subjects with PI (18 children and 5 adolescents) in Europe. There were no differences in the pharmacokinetics, safety and efficacy profiles as compared with adult subjects. No pediatric-specific dose requirements were necessary to achieve the desired serum IgG levels.
Pharmacokinetic Modeling and Simulation (Biweekly or more Frequent Dosing)
The biweekly (every 2 weeks) or more frequent dosing (2 to 7 times per week) regimens, developed from population PK-based modeling and simulation, included 57 pediatric subjects (32 from HIZENTRA clinical studies) [see Clinical Pharmacology (12.3)]. HIZENTRA dosing is adjusted to body weight. No pediatric-specific dose requirements are necessary for these regimens.
Safety and effectiveness of HIZENTRA in pediatric patients below the age of 2 have not been established.
8.5 Geriatric Use
Treatment of Primary Immunodeficiency
Of the 49 subjects evaluated in the U.S. clinical study of HIZENTRA, 6 subjects were 65 years of age or older. No overall differences in safety or efficacy were observed between these subjects and subjects 18 to 65 years of age. The clinical study of HIZENTRA in Europe did not include subjects over the age of 65.
Treatment of Chronic Inflammatory Demyelinating Polyneuropathy
Of the 172 subjects evaluated in the SC treatment period of a global study (HIZENTRA vs placebo), 50 subjects were >65 years of age (34 HIZENTRA and 16 placebo subjects). No overall differences in safety or efficacy were observed between these subjects and subjects 18 to 65 years of age.
11. Hizentra Description
HIZENTRA, Immune Globulin Subcutaneous (Human), 20% Liquid, is a ready-to-use, sterile 20% (0.2 g/mL) protein liquid preparation of polyvalent human immunoglobulin G (IgG) for subcutaneous administration. HIZENTRA is manufactured from large pools of human plasma by a combination of cold alcohol fractionation, octanoic acid fractionation, and anion exchange chromatography. The IgG proteins are not subjected to heating or to chemical or enzymatic modification. The Fc and Fab functions of the IgG molecule are retained. Fab functions tested include antigen binding capacities, and Fc functions tested include complement activation and Fc-receptor-mediated leukocyte activation (determined with complexed IgG). The IgG subclass distribution is similar to that of normal human plasma.
HIZENTRA has a purity of ≥98% IgG and a pH of 4.6 to 5.2. This product contains approximately 250 mmol/L (range: 210 to 290 mmol/L) L-proline (a nonessential amino acid) as a stabilizer, 8 to 30 mg/L polysorbate 80, and trace amounts of sodium. HIZENTRA contains ≤50 mcg/mL IgA, no carbohydrate stabilizers (e.g., sucrose, maltose) and no preservative.
Plasma units used in the manufacture of HIZENTRA are tested using FDA-licensed serological assays for hepatitis B surface antigen and antibodies to human immunodeficiency virus (HIV)-1/2 and hepatitis C virus (HCV) as well as FDA-licensed Nucleic Acid Testing (NAT) for HBV, HCV and HIV-1. All plasma units have been found to be nonreactive (negative) in these tests. In addition, the plasma has been tested for B19 virus (B19V) DNA by NAT. Only plasma that passes virus screening is used for production, and the limit for B19V in the fractionation pool is set not to exceed 104 IU of B19V DNA per mL.
The manufacturing process for HIZENTRA includes three steps to reduce the risk of virus transmission. Two of these are dedicated virus clearance steps: pH 4 incubation to inactivate enveloped viruses, and virus filtration to remove, by size exclusion, both enveloped and non-enveloped viruses as small as approximately 20 nanometers. In addition, a depth filtration step contributes to the virus reduction capacity.12
These steps have been independently validated in a series of in vitro experiments for their capacity to inactivate and/or remove both enveloped and non-enveloped viruses. Table 6 shows the virus clearance during the manufacturing process for HIZENTRA, expressed as the mean log10 reduction factor (LRF).
| HIV-1 | PRV | BVDV | WNV | EMCV | MVM | |
|---|---|---|---|---|---|---|
| HIV-1, human immunodeficiency virus type 1, a model for HIV-1 and HIV-2; PRV, pseudorabies virus, a nonspecific model for large enveloped DNA viruses (e.g., herpes virus); BVDV, bovine viral diarrhea virus, a model for hepatitis C virus; WNV, West Nile virus; EMCV, encephalomyocarditis virus, a model for hepatitis A virus; MVM, minute virus of mice, a model for a small highly resistant non-enveloped DNA virus (e.g., parvovirus); LRF, log10 reduction factor; nt, not tested; na, not applicable. | ||||||
|
||||||
| Virus Property | ||||||
| Genome | RNA | DNA | RNA | RNA | RNA | DNA |
| Envelope | Yes | Yes | Yes | Yes | No | No |
| Size (nm) | 80-100 | 120-200 | 50-70 | 50-70 | 25-30 | 18-24 |
| Manufacturing Step | Mean LRF | |||||
| pH 4 incubation | ≥5.6 | ≥6.1 | 4.6 | ≥7.8 | nt | nt |
| Depth filtration | ≥6.7 | ≥5.7 | 3.5±0.2 | 3.0±0.4 | 5.7±0.2 | 3.7±0.3 |
| Virus filtration | ≥4.7 | ≥5.8 | ≥4.6 | ≥6.8 | ≥6.3 | ≥6.5 |
| Overall Reduction (Log10 Units) | ≥17.0 | ≥17.6 | ≥12.7 | ≥17.6 | ≥12.0 | ≥10.2 |
12. Hizentra - Clinical Pharmacology
12.1 Mechanism of Action
HIZENTRA supplies a broad spectrum of opsonizing and neutralizing IgG antibodies against a wide variety of bacterial and viral agents. The mechanism of action has not been fully elucidated, but may include immunomodulatory effects.
12.3 Pharmacokinetics
Treatment of Primary Immunodeficiency
Clinical Studies
The pharmacokinetics (PK) of HIZENTRA was evaluated in a PK substudy of subjects (14 adults, 1 pediatric subject aged 6 to <12 years, and 3 adolescent subjects aged 12 to <16 years) with PI participating in the 15-month efficacy and safety study [see Clinical Studies (14)]. All PK subjects were treated previously with PRIVIGEN®, Immune Globulin Intravenous (Human), 10% Liquid and were switched to weekly subcutaneous treatment with HIZENTRA. After a 3-month wash-in/wash-out period, doses were adjusted individually with the goal of providing a systemic serum IgG exposure (area under the IgG serum concentration vs time curve; AUC) not inferior to that of the previous weekly-equivalent IGIV dose. Table 7 summarizes PK parameters for subjects in the substudy following treatment with HIZENTRA and IGIV.
| HIZENTRA | IGIV* (PRIVIGEN®) | |
|---|---|---|
| AUC, area under the curve; CL, clearance. | ||
| Number of subjects | 18 | 18 |
| Dose* (mg/kg) | ||
| Mean | 228 | 152 |
| Range | 141-381 | 86-254 |
| IgG peak levels (mg/dL) | ||
| Mean | 1616 | 2564 |
| Range | 1090-2825 | 2046-3456 |
| IgG trough levels (mg/dL) | ||
| Mean | 1448 | 1127 |
| Range | 952-2623 | 702-1810 |
| AUC† (day × mg/dL) | ||
| Mean | 10560 | 10320 |
| Range | 7210-18670 | 8051-15530 |
| CL‡ (mL/day/kg) | ||
| Mean | 2.2 | 1.3§ |
| Range | 1.2-3.7 | 0.9-2.1 |
For the 19 subjects completing the wash-in/wash-out period, the average dose adjustment for HIZENTRA was 153% (range: 126% to 187%) of the previous weekly-equivalent IGIV dose. After 12 weeks of treatment with HIZENTRA at this individually adjusted dose, the final steady-state AUC determinations were made in 18 of the 19 subjects. The geometric mean ratio of the steady-state AUCs, standardized to a weekly treatment period, for HIZENTRA vs IGIV treatment was 1.002 (range: 0.77 to 1.20) with a 90% confidence limit of 0.951 to 1.055 for the 18 subjects.
With HIZENTRA, peak serum levels are lower (1616 vs 2564 mg/dL) than those achieved with IGIV while trough levels are generally higher (1448 vs 1127 mg/dL). In contrast to IGIV administered every 3 to 4 weeks, weekly subcutaneous administration results in relatively stable steady-state serum IgG levels.13,14 After the subjects had reached steady-state with weekly administration of HIZENTRA, peak serum IgG levels were observed after a mean of 2.9 days (range: 0 to 7 days) in 18 subjects.
Table 8 summarizes PK parameters at steady state for pediatric subjects (age groups: 6 to <12 years and 12 to <16 years) and adult subjects (≥16 years) in the European HIZENTRA study following weekly treatment [see Clinical Studies (14.1)]. Pediatric PK parameters are similar to those of adult subjects; thus no pediatric specific dose requirements are needed for HIZENTRA dosing.
| Age Group | Age Group | Age Group | ||
|---|---|---|---|---|
| 6 to <12 years (n=9) | 12 to <16 years (n=3) | 16 to <65 years (n=11) | Total (n=23) |
|
| AUC0-7d, area under the curve for the 7-day dosing interval; CL, apparent clearance (CL/F) (F = bioavailability). | ||||
| Dose (mg/kg) | ||||
| Mean | 120 | 115 | 117 | 118 |
| Range | 71-170 | 72-150 | 87-156 | 71-170 |
| IgG trough levels (mg/dL) | ||||
| Mean | 731 | 764 | 754 | 746 |
| Range | 531-915 | 615-957 | 505-898 | 505-957 |
| AUC0-7d (day × mg/dL) | ||||
| Mean | 5230 | 5491 | 5452 | 5370 |
| Range | 3890-6950 | 4480-6750 | 3860-6810 | 3860-6950 |
| CL (mL/day/kg) | ||||
| Mean | 2.19 | 2.17 | 2.30 | 2.23 |
| Range | 1.57-3.05 | 1.38-3.34 | 1.82-3.01 | 1.38-3.34 |
Pharmacokinetic Modeling and Simulation
Biweekly (Every 2 Weeks) or more Frequent Dosing
Pharmacokinetic characterization of biweekly or more frequent dosing of HIZENTRA was undertaken using population PK-based modeling and simulation. Serum IgG concentration data consisted of 3837 samples from 151 unique pediatric and adult subjects with PI from four clinical studies of IGIV (PRIVIGEN®) and/or HIZENTRA. Of the 151 subjects, 94 were adult subjects (63 from HIZENTRA clinical studies) and 57 were pediatric subjects (32 from HIZENTRA clinical studies). Compared with weekly administration, PK modeling and simulation predicted that administration of HIZENTRA on a biweekly basis at double the weekly dose results in comparable IgG exposure [equivalent AUCs, with a slightly higher IgG peak (Cmax) and slightly lower trough (Cmin)]. In addition, PK modeling and simulation predicted that for the same total weekly dose, HIZENTRA infusions given 2, 3, 5, or 7 times per week (frequent dosing) produce IgG exposures comparable to weekly dosing [equivalent AUCs, with a slightly lower IgG peak (Cmax) and slightly higher trough (Cmin)]. Frequent dosing reduces the peak-to-trough variation in HIZENTRA serum levels, thus resulting in more sustained IgG exposures. See Table 9 (columns for AUC, Cmax and Cmin).
Dose Adjustment Factor
Using data from four clinical studies, results of model-based simulations demonstrated that weekly or biweekly HIZENTRA dosing regimens with an IGIV:IGSC dose adjustment factor of 1:1.37 adequately maintain median AUC0-28days and Cmin ratios at ≥90% of values observed with 4-weekly IGIV dosing. See Table 9 (top two rows).
Prediction of Trough Levels Following Regimen Changes
PK modeling and simulation also predicted changes in trough levels after switching from (a) monthly IGIV to weekly or biweekly HIZENTRA dosing, (b) weekly to biweekly HIZENTRA dosing, or (c) weekly to more frequent dosing. Table 9 (last column) shows the predicted changes in steady-state IgG trough levels after switching between the various dosing regimens.
| IgG Dosing Regimen Switch | AUC | Cmax | Cmin | Predicted Change in Trough† | |
|---|---|---|---|---|---|
| From: | To: | ||||
| AUC, area under the curve, calculated as AUC0-28days for the IGIV to HIZENTRA switches, AUC0-14days for the weekly to biweekly HIZENTRA switch, and AUC0-7days for weekly to more frequent HIZENTRA switches; Cmax, maximum IgG concentration; Cmin, minimum IgG concentration during a 28-day period (for the IGIV to HIZENTRA switches), a 14-day period (for the weekly to biweekly HIZENTRA switch), or a 7-day period (for the weekly to more frequent HIZENTRA switches). | |||||
|
|||||
| IGIV | Weekly HIZENTRA‡ | 0.97 (0.90, 1.04) | 0.68 (0.60, 0.76) | 1.16 (1.07, 1.26) | 16% increase |
| IGIV | Biweekly HIZENTRA§ | 0.97 (0.91, 1.04) | 0.71 (0.63, 0.78) | 1.10 (1.02, 1.18) | 10% increase |
| Weekly HIZENTRA | Biweekly HIZENTRA§ | 1.00 (0.98, 1.03) | 1.06 (1.02, 1.09) | 0.95 (0.92, 0.98) | 5% decrease |
| Weekly HIZENTRA | 2 times per week HIZENTRA | 1.01 (0.98, 1.03) | 0.99 (0.96, 1.02) | 1.03 (1.00, 1.06) | 3% increase |
| Weekly HIZENTRA | 3 times per week HIZENTRA | 1.01 (0.98, 1.03) | 0.99 (0.96, 1.02) | 1.04 (1.01, 1.07) | 4% increase |
| Weekly HIZENTRA | 5 times per week HIZENTRA (daily for 5 days) | 1.01 (0.98, 1.03) | 0.99 (0.97, 1.01) | 1.04 (1.01, 1.06) | 4% increase |
| Weekly HIZENTRA | Daily HIZENTRA (7 times per week) | 1.00 (0.98, 1.03) | 0.98 (0.95, 1.01) | 1.04 (1.02, 1.08) | 4% increase |
PI Pediatric Pharmacokinetics
PK-based modeling and simulation results indicate that, similar to observations from the clinical study with weekly HIZENTRA dosing (Table 8), body weight-adjusted biweekly dosing accounted for age-related (>3 years) differences in clearance of HIZENTRA, thereby maintaining systemic IgG exposure (AUC values) in the therapeutic range.
Treatment of Chronic Inflammatory Demyelinating Polyneuropathy
PATH Study
In the PATH study, subjects (n=172) achieved sustained trough levels over a period of 24 weeks when receiving weekly doses of 0.2 g/kg body weight and 0.4 g/kg body weight, respectively. The mean (SD) IgG trough concentration after 24 weeks of HIZENTRA treatment in the 0.2 g/kg body weight group was 15.3 (2.57) g/L and in the 0.4 g/kg body weight group was 20.8 (3.23) g/L.
PATH Extension Study
A total of 82 subjects were enrolled in the PATH Extension study. The mean serum IgG concentration remained stable at approximately 20 g/L until Week 33, after this period it decreased to 17.1 g/L. The Week 33 decrease in IgG level matched the level in subjects being down titrated from 0.4 g/kg to 0.2 g/kg at Week 25. The mean IgG level decreased by 19% from enrollment into the extension study for subjects who remained stable after down-titrating to 0.2 g/kg versus the 0.4 g/kg dosing. The mean IgG level decreased by 27% from enrollment into the extension study for subjects who relapsed after down-titrating to 0.2 g/kg versus 0.4 g/kg dosing. The mean (SD) IgG level increased to 20.2 (3.59) g/L at the end of the study for subjects who relapsed on 0.2 g/kg and up-titrated to 0.4 g/kg dosing.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
No animal studies were conducted to evaluate the carcinogenic or mutagenic effects of HIZENTRA or its effects on fertility.
13.2 Animal Toxicology and/or Pharmacology
Long- and short-term memory loss was seen in juvenile rats in a study modeling hyperprolinemia. In this study, rats received daily subcutaneous injections with L-proline from day 6 to day 28 of life.15 The daily amounts of L-proline used in this study were more than 60 times higher than the L-proline dose that would result from the administration of 400 mg/kg body weight of HIZENTRA once weekly. In unpublished studies using the same animal model (i.e., rats) dosed with the same amount of L-proline with a dosing interval relevant to IGSC treatment (i.e., on 5 consecutive days on days 9 to 13, or once weekly on days 9, 16, and 23), no effects on learning and memory were observed. The clinical relevance of these studies is not known.
14. Clinical Studies
14.1 Primary Immunodeficiency (PI)
U.S. Study
A prospective, open-label, multicenter, single-arm, clinical study conducted in the U.S. evaluated the efficacy, tolerability, and safety of HIZENTRA in 49 adult and pediatric subjects with PI. Subjects previously receiving monthly treatment with IGIV were switched to weekly subcutaneous administration of HIZENTRA for 15 months. Following a 3-month wash-in/wash-out period, subjects received a dose adjustment to achieve an equivalent AUC to their previous IGIV dose [see Clinical Pharmacology (12.3)] and continued treatment for a 12-month efficacy period. The efficacy analyses included 38 subjects in the modified intention-to-treat (MITT) population. The MITT population consisted of subjects who completed the wash-in/wash-out period and received at least one infusion of HIZENTRA during the efficacy period.
Although 5% of the administered doses could not be verified, the weekly median doses of HIZENTRA ranged from 72 to 379 mg/kg body weight during the efficacy period. The mean dose was 213.2 mg/kg, which was 149% of the previous IGIV dose.
In the study, the number of infusion sites per infusion ranged from 1 to 12. In 73% of infusions, the number of infusion sites was 4 or fewer. Up to 4 simultaneous infusion sites were permitted using 2 pumps; however, more than 4 sites could be used consecutively during one infusion. The infusion flow rate did not exceed 50 mL per hour for all infusion sites combined. During the efficacy period, the median duration of a weekly infusion ranged from 1.6 to 2.0 hours.
The study evaluated the annual rate of serious bacterial infections (SBIs), defined as bacterial pneumonia, bacteremia/septicemia, osteomyelitis/septic arthritis, bacterial meningitis, and visceral abscess. The study also evaluated the annual rate of any infections, the use of antibiotics for infection (prophylaxis or treatment), the days out of work/school/kindergarten/day care or unable to perform normal activities due to infections, hospitalizations due to infections, and serum IgG trough levels.
Table 10 summarizes the efficacy results for subjects in the efficacy period (MITT population) of the study. No subjects experienced an SBI in this study.
| Number of subjects (efficacy period) | 38 |
| Total number of subject days | 12,697 |
| Infections | |
| Annual rate of SBIs* | 0 SBIs per subject year† |
| Annual rate of any infections | 2.76 infections/subject year‡ |
| Antibiotic use for infection (prophylaxis or treatment) | |
| Number of subjects (%) | 27 (71.1) |
| Annual rate | 48.5 days/subject year |
| Total number of subject days | 12,605 |
| Days out of work/school/kindergarten/day care or unable to perform normal activities due to infections | |
| Number of days (%) | 71 (0.56) |
| Annual rate | 2.06 days/subject year |
| Hospitalizations due to infections | |
| Number of days (%) | 7 (0.06)§ |
| Annual rate | 0.2 days/subject year |
The mean IgG trough levels increased by 24.2%, from 1009 mg/dL prior to the study to 1253 mg/dL during the efficacy period.
European Study
In a prospective, open-label, multicenter, single-arm, clinical study conducted in Europe, 51 adult and pediatric subjects with PI switched from monthly IGIV (31 subjects) or weekly IGSC (20 subjects) to weekly treatment with HIZENTRA. For the 46 subjects in the efficacy analysis, the weekly mean dose in the efficacy period was 120.1 mg/kg (range 59 to 243 mg/kg), which was 104% of the previous weekly equivalent IGIV or weekly IGSC dose.
None of the subjects had an SBI during the efficacy period, resulting in an annualized rate of 0 (upper one-sided 99% confidence limit of 0.192) SBIs per subject. The annualized rate of any infections was 5.18 infections per subject for the efficacy period.
14.2 Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)
PATH Study
A multicenter, double-blind, randomized, placebo-controlled, parallel-group phase 3 study evaluated the efficacy, safety, and tolerability of 2 different weekly doses of HIZENTRA (0.4 g/kg body weight and 0.2 g/kg body weight) versus placebo in 172 adult subjects with CIDP and previously treated with IGIV (PATH study). The mean treatment duration was 129 days in the 0.4 g/kg HIZENTRA group and 118.9 days in the 0.2 g/kg HIZENTRA group (treatment duration up to 166 and 167 days in each group, respectively). Subjects generally used 4 infusion sites in parallel (maximum: 8 sites in parallel). Subjects infused an average of 20 mL per infusion site (maximum: 50 mL/site) with an infusion rate of 20 mL/h (maximum: 50 mL/h) and volumes up to 140 mL per infusion session. The infusion time was approximately 1 hour.
The main endpoint was the percentage of subjects who had a CIDP relapse or were withdrawn for any other reason during the SC Treatment Period. CIDP relapse was defined as a ≥1 point increase in adjusted Inflammatory Neuropathy Cause and Treatment [INCAT] score compared with baseline. Both HIZENTRA doses demonstrated superiority over placebo for the main endpoint (32.8% for 0.4 g/kg HIZENTRA and 38.6% for 0.2 g/kg HIZENTRA compared with 63.2% for placebo, p<0.001 or p=0.007, respectively), with no statistically significant difference between the doses. When only considering relapse, the CIDP relapse rates were 19.0% for 0.4 g/kg HIZENTRA and 33.3% for 0.2 g/kg HIZENTRA compared with 56.1% for placebo (p<0.001 or p=0.012, respectively), with no statistically significant difference between the doses. Eighty one percent (81%) and 67% of HIZENTRA-treated subjects remained relapse-free (0.4 g/kg body weight and 0.2 g/kg body weight, respectively); 44% of placebo subjects remained relapse-free for up to 24 weeks.
A Kaplan-Meier Plot of time to CIDP relapse or withdrawal for any other reason is shown in Figure 1.
Figure 1. Kaplan-Meier Plot Time to CIDP Relapse or Withdrawal for Any Other Reason
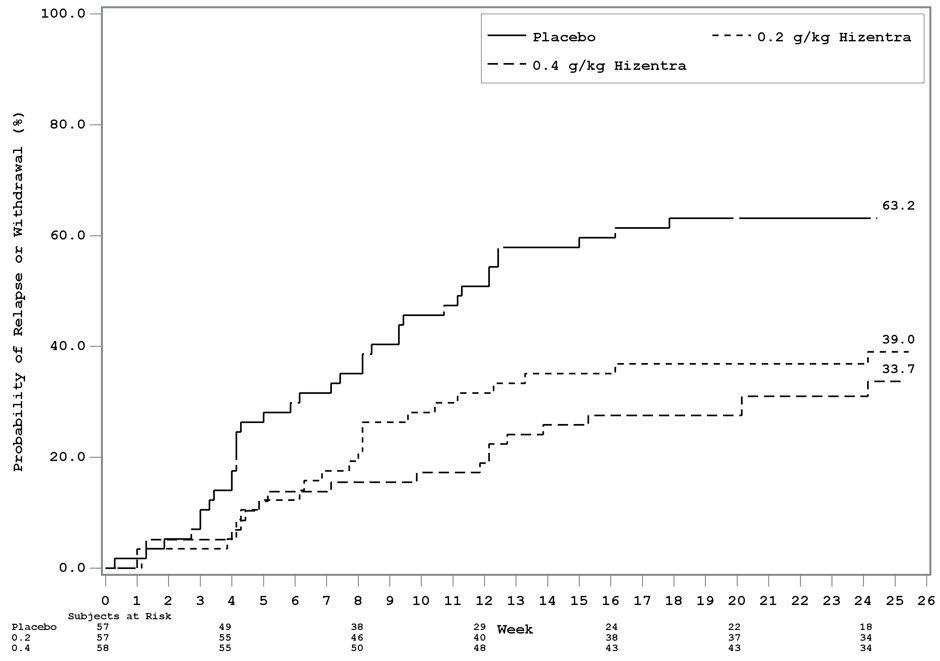
Subjects in both HIZENTRA dose groups remained relatively stable while subjects in the placebo group deteriorated in mean INCAT score, mean grip strength, mean Medical Research Council sum score, and mean Rasch-built Overall Disability Scale (R-ODS) centile score.
PATH Extension Study
The PATH Extension study was a multicenter, 48-week, open-label extension study that evaluated the long-term safety and efficacy of HIZENTRA 0.2 g/kg and 0.4 g/kg doses in the maintenance treatment of CIDP in subjects who either completed or were being successfully rescued from CIDP relapse with IGIV treatment in the PATH study.
A total of 82 subjects were enrolled. In the study, subjects who started on a HIZENTRA 0.2 g/kg dose were up-titrated to 0.4 g/kg dose if they relapsed. In the case of no relapse, subjects remained at a dose of 0.2 g/kg. Subjects who started on a HIZENTRA 0.4 g/kg dose were down-titrated to 0.2 g/kg dose after 24 weeks of treatment and subjects who relapsed on a HIZENTRA 0.2 g/kg dose were up-titrated to a 0.4 g/kg dose. Due to the study design, the same subject could have received both doses during the study; 72 subjects received doses of 0.4 g/kg, and 73 subjects received doses of 0.2 g/kg during the efficacy evaluation period.
Subjects who completed the PATH study without relapse on a 0.4 g/kg dose and initially received this dose in the PATH extension study, had a relapse rate of 5.6% (1/18 subjects). Subjects who completed the PATH study without relapse on a 0.2 g/kg dose and initially received this dose in the extension study had a relapse rate of 50% (3/6 subjects).
For all subjects who received 0.4 g/kg in the PATH Extension study, 9.7% (7/72 subjects) had a relapse. For all subjects who received 0.2 g/kg in the PATH extension study, 47.9% (35/73 subjects) had a relapse.
After down-titrating from HIZENTRA 0.4 g/kg to 0.2 g/kg, 50% (26/52) of subjects relapsed, of whom 92% (24/26) recovered after returning to HIZENTRA 0.4 g/kg. A total of 35 subjects relapsed on HIZENTRA 0.2 g/kg dose, of which 89% (31/35) subjects recovered after returning to 0.4 g/kg dose.
Both the PATH and PATH Extension studies demonstrated that HIZENTRA 0.2 g/kg or 0.4 g/kg dose was effective in preventing CIDP relapse when administered weekly with the HIZENTRA 0.4 g/kg dose more likely to prevent relapse.
15. References
- Dalakas MC. High-dose intravenous immunoglobulin and serum viscosity: risk of precipitating thromboembolic events. Neurology 1994;44:223-226.
- Woodruff RK, Grigg AP, Firkin FC, Smith IL. Fatal thrombotic events during treatment of autoimmune thrombocytopenia with intravenous immunoglobulin in elderly patients. Lancet 1986;2:217-218.
- Wolberg AS, Kon RH, Monroe DM, Hoffman M. Coagulation factor XI is a contaminant in intravenous immunoglobulin preparations. Am J Hematol 2000;65:30-34.
- Gabor EP, Meningitis and skin reaction after intravenous immune globulin therapy. Ann Intern Med 1997:127:1130.
- Pierce LR, Jain N. Risks associated with the use of intravenous immunoglobulin. Trans Med Rev 2003;17:241-251.
- Cayco AV, Perazella MA, Hayslett JP. Renal insufficiency after intravenous immune globulin therapy: a report of two cases and an analysis of the literature. J Am Soc Nephrol 1997;8:1788-1793.
- Copelan EA, Strohm PL, Kennedy MS, Tutschka PJ. Hemolysis following intravenous immune globulin therapy. Transfusion 1986;26:410-412.
- Thomas MJ, Misbah SA, Chapel HM, Jones M, Elrington G, Newsom-Davis J. Hemolysis after high-dose intravenous Ig. Blood 1993;15:3789.
- Wilson JR, Bhoopalam N, Fisher M. Hemolytic anemia associated with intravenous immunoglobulin. Muscle Nerve 1997;20:1142-1145.
- Kessary-Shoham H, Levy Y, Shoenfeld Y, Lorber M, Gershon H. In vivo administration of intravenous immunoglobulin (IVIg) can lead to enhanced erythrocyte sequestration. J Autoimmun 1999;13:129-135.
- Rizk A, Gorson KC, Kenney L, Weinstein R. Transfusion-related acute lung injury after the infusion of IVIG. Transfusion 2001;41:264-268.
- Stucki M, Boschetti N, Schäfer W, et al. Investigations of prion and virus safety of a new liquid IVIG product. Biologicals 2008;36:239-247.
- Smith GN, Griffiths B, Mollison D, Mollison PL. Uptake of IgG after intramuscular and subcutaneous injection. Lancet 1972;1:1208-1212.
- Waniewski I, Gardulf A, Hammarström L. Bioavailability of γ-globulin after subcutaneous infusions in patients with common variable immunodeficiency. J Clin Immunol 1994;14:90-97.
- Bavaresco CS, Streck EL, Netto CA, et al. Chronic hyperprolinemia provokes a memory deficit in the Morris Water Maze Task. Metabolic Brain Disease 2005;20:73-80.
16. How is Hizentra supplied
HIZENTRA is supplied in a prefilled syringe or a tamper-evident vial containing 0.2 grams of protein per mL of preservative-free liquid. The HIZENTRA packaging components are not made with natural rubber latex.
Each product presentation includes a package insert and the following components:
Table 11: How Supplied
Prefilled Syringes:
| Presentation | Carton NDC Number | Components |
|---|---|---|
| 5 mL | 44206-456-21 | Prefilled syringe containing 1 gram of protein (NDC 44206-456-94) |
| 10 mL | 44206-457-22 | Prefilled syringe containing 2 grams of protein (NDC 44206-457-95) |
| 20 mL | 44206-458-24 | Prefilled syringe containing 4 grams of protein (NDC 44206-458-96) with plunger rod. |
| 50 mL | 44206-455-25 | Prefilled syringe containing 10 grams of protein (NDC 44206-455-97) with plunger rod. |
Vials:
| Presentation | Carton NDC Number | Components |
|---|---|---|
| 5 mL | 44206-451-01 | Vial containing 1 gram of protein (NDC 44206-451-90) |
| 10 mL | 44206-452-02 | Vial containing 2 grams of protein (NDC 44206-452-91) |
| 20 mL | 44206-454-04 | Vial containing 4 grams of protein (NDC 44206-454-92) |
| 50 mL | 44206-455-10 | Vial containing 10 grams of protein (NDC 44206-455-93) |
Storage and Handling
- Store the HIZENTRA prefilled syringe or vial in its original carton to protect it from light.
- Each prefilled syringe or vial label contains a peel-off strip with the prefilled syringe or vial size and product lot number for use in recording doses in a patient treatment record.
- When stored at room temperature (up to 25°C [77°F]), HIZENTRA is stable for up to 30 months, as indicated by the expiration date printed on the outer carton of the prefilled syringe or vial label.
- Do not shake the HIZENTRA prefilled syringe or vial.
- Do not freeze. Do not use product that has been frozen.
- Discard any unused product and all used disposable supplies after each infusion.
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Information for Patients and Instructions for Use).
Inform patients to immediately report the following signs and symptoms to their healthcare provider:
- Hypersensitivity reactions to HIZENTRA (including hives, generalized urticaria, tightness of the chest, wheezing, hypotension, and anaphylaxis) [see Warnings and Precautions (5.1)].
- Pain and/or swelling of an arm or leg with warmth over the affected area, discoloration of an arm or leg, unexplained shortness of breath, chest pain or discomfort that worsens on deep breathing, unexplained rapid pulse, or numbness or weakness on one side of the body [see Warnings and Precautions (5.2)].
- Severe headache, neck stiffness, drowsiness, fever, sensitivity to light, painful eye movements, nausea, and vomiting [see Warnings and Precautions (5.3)].
- Decreased urine output, sudden weight gain, fluid retention/edema, and/or shortness of breath [see Warnings and Precautions (5.4)].
- Fatigue, increased heart rate, yellowing of the skin or eyes, and dark-colored urine [see Warnings and Precautions (5.5)].
- Severe breathing problems, lightheadedness, drops in blood pressure, and fever [see Warnings and Precautions (5.6)].
Inform patients that because HIZENTRA is made from human blood, it may carry a risk of transmitting infectious agents, e.g., viruses, the variant Creutzfeldt-Jakob disease (vCJD) agent and, theoretically, the Creutzfeldt-Jakob disease (CJD) agent [see Warnings and Precautions (5.7) and Description (11)].
Inform patients that HIZENTRA may interfere with the response to live virus vaccines (e.g., measles, mumps, rubella, and varicella) and to notify their immunizing physician of recent therapy with HIZENTRA [see Drug Interactions (7)].
Home Treatment with Subcutaneous Administration
- If self-administration is deemed to be appropriate, ensure that the patient receives clear instructions and training on subcutaneous administration in the home or other appropriate setting and has demonstrated the ability to independently administer subcutaneous infusions.
- Ensure the patient understands the importance of adhering to their prescribed administration schedule to maintain appropriate steady IgG levels.
- Instruct patients to scan the prefilled syringe or vial if recording the infusion electronically and keep a diary/log book that includes information about each infusion such as, the time, date, dose, lot number(s) and any reactions.
- Inform the patient that mild to moderate local infusion-site reactions (e.g., swelling and redness) are a common side effect of subcutaneous therapy, but to contact their healthcare professional if a local reaction increases in severity or persists for more than a few days.
- Inform patients of the importance of having an infusion needle long enough to reach the subcutaneous tissue and of changing the actual site of infusion with each infusion. Explain that HIZENTRA is for subcutaneous infusion only.
- Inform patients to consider adjusting the infusion-site location, volume per site, and rate of infusion based on how infusions are tolerated.
- Inform patient to interrupt or terminate the HIZENTRA infusion if a hypersensitivity reaction occurs.
- Inform PI patients that they should be tested regularly to make sure they have the correct levels of HIZENTRA (IgG) in their blood. These tests may result in adjustments to the HIZENTRA dose.
Information for Patients
HIZENTRA®
(hi-ZEN-tra)
Immune Globulin Subcutaneous (Human), 20% Liquid
Information for Patients
This patient package insert summarizes important information about HIZENTRA. Please read it carefully before using this medicine. This information does not take the place of talking with your healthcare professional, and it does not include all of the important information about HIZENTRA. If you have any questions after reading this, ask your healthcare professional.
What is the most important information I should know about HIZENTRA?
HIZENTRA is supposed to be infused under your skin only. DO NOT inject HIZENTRA into a blood vessel (vein or artery).
What is HIZENTRA?
HIZENTRA is a prescription medicine used to treat primary immune deficiency (PI) and chronic inflammatory demyelinating polyneuropathy (CIDP). HIZENTRA is made from human blood. HIZENTRA contains antibodies called immunoglobulin G (IgG). People with PI get a lot of infections, and IgG fights germs (bacteria and viruses). People with CIDP have a form of autoimmune disease where it is believed the body's defenses attack the nerves and cause muscle weakness and numbness mainly in the legs and arms. IgG is believed to help protect the nerve from being attacked.
Who should NOT take HIZENTRA?
Do not take HIZENTRA if you have too much proline in your blood (called "hyperprolinemia") or if you have had reactions to polysorbate 80.
Tell your doctor if you have had a serious reaction to other immune globulin medicines or if you have been told that you also have a deficiency of the immunoglobulin called IgA.
Tell your doctor if you have a history of heart or blood vessel disease or blood clots, have thick blood, or have been immobile for some time. These things may increase your risk of having a blood clot after using HIZENTRA. Also tell your doctor what drugs you are using, as some drugs, such as those that contain the hormone estrogen (for example, birth control pills), may increase your risk of developing a blood clot.
How should I take HIZENTRA?
You will take HIZENTRA through an infusion, only under your skin. You will place up to 8 needles into different areas of your body each time you use HIZENTRA. The needles are attached to a pump with an infusion tube. For PI, you can have infusions as often as every day up to every two (2) weeks. For CIDP, infusions are given once weekly (in 1 or 2 sessions conducted on 1 day or 2 consecutive days). For weekly infusions, it can take about 1 to 2 hours to complete an infusion; however, this time may be shorter or longer depending on the dose and frequency your doctor has prescribed for you.
Instructions for using HIZENTRA are at the end of this patient package insert (see "How do I use HIZENTRA?"). Do not use HIZENTRA by yourself until you have been taught how by your doctor or healthcare professional.
What should I avoid while taking HIZENTRA?
Vaccines may not work well for you while you are taking HIZENTRA. Tell your doctor or healthcare professional that you are taking HIZENTRA before you get a vaccine.
Tell your doctor or healthcare professional if you are pregnant or plan to become pregnant, or if you are nursing.
What are possible side effects of HIZENTRA?
The most common side effects with HIZENTRA are:
- Redness, swelling, itching, and/or bruising at the infusion site
- Headache/migraine
- Nausea and/or vomiting
- Pain (including pain in the chest, back, joints, arms, legs)
- Fatigue
- Diarrhea
- Stomach ache/bloating
- Cough, cold or flu symptoms
- Rash (including hives)
- Itching
- Fever and/or chills
- Shortness of breath
- Dizziness
- Fall
- Runny or stuffy nose
Tell your doctor right away or go to the emergency room if you have hives, trouble breathing, wheezing, dizziness, or fainting. These could be signs of a bad allergic reaction.
Tell your doctor right away if you have any of the following symptoms. They could be signs of a serious problem.
- Reduced urination, sudden weight gain, or swelling in your legs. These could be signs of a kidney problem.
- Pain and/or swelling of an arm or leg with warmth over the affected area, discoloration of an arm or leg, unexplained shortness of breath, chest pain or discomfort that worsens on deep breathing, unexplained rapid pulse, or numbness or weakness on one side of the body. These could be signs of a blood clot.
- Bad headache with nausea, vomiting, stiff neck, fever, and sensitivity to light. These could be signs of a brain swelling called meningitis.
- Brown or red urine, fast heart rate, yellow skin or eyes. These could be signs of a blood problem.
- Chest pains or trouble breathing.
- Fever over 100ºF. This could be a sign of an infection.
Tell your doctor about any side effects that concern you. You can ask your doctor to give you more information that is available to healthcare professionals.
Infuse HIZENTRA only after you have been trained by your doctor or healthcare professional. Below are step-by-step instructions to help you remember how to use HIZENTRA. Ask your doctor or healthcare professional about any instructions you do not understand.
INSTRUCTIONS FOR USE
HIZENTRA® (hi-ZEN-tra)
(Immune Globulin Subcutaneous (Human), 20% Liquid)
for subcutaneous use only
HIZENTRA is provided in a carton containing:
- Single-dose prefilled syringes (5 mL, 10 mL, 20 mL, and 50 mL) or
- Single-dose vials (5 mL, 10 mL, 20 mL, and 50 mL).
Store HIZENTRA in its original carton at room temperature until ready to use. Do not use the prefilled syringe or vial if the packaging is damaged.
Step 1: Assemble supplies
Gather the HIZENTRA prefilled syringe(s) or vial(s), all supplies, and infusion log book:
- Infusion administration tubing
- Subcutaneous needle or catheter sets
- Syringes
- Transfer device or needle(s)
- Syringe-to-syringe transfer device (tip-to-tip connector)
- Gauze and tape, or transparent dressing
- Infusion pump and any adapters (if required)
- Sharps container
- Alcohol wipes
- Antiseptic skin preps
Step 2: Clean surface
Clean a table or other flat surface.
Step 3: Wash hands
Thoroughly wash and dry your hands (Figure 1).

Figure 1
Step 4: Check prefilled syringe(s) or vial(s)
-
If using prefilled syringes, carefully peel back the transparent covering from the tray and inspect the protective cap. Peel back the outer layer of the wrap-around label to allow for viewing of HIZENTRA through the fully transparent inner layer, but don't remove the label completely (Figure 2).

Figure 2
-
If using vials, inspect the protective cap of the vials (Figure 3).
Figure 3
Carefully inspect each prefilled syringe(s) or vial(s) of HIZENTRA. HIZENTRA is a clear and pale yellow to light brown solution. Do not use the prefilled syringe or vial if:
|
Step 5: Prepare HIZENTRA for infusion
- If using HIZENTRA prefilled syringes, go to Step 5.1
- If using HIZENTRA vials, go to Step 5.2
Step 5.1: HIZENTRA prefilled syringe(s)
- The 5 mL, 10 mL, 20 mL, and 50 mL prefilled syringes are supplied and ready to use. The 5 mL and 10 mL prefilled syringes are fully assembled (Figure 4). For the 20 mL and 50 mL prefilled syringes, screw the plunger rod onto the prefilled syringe stopper prior to use Figure 5).
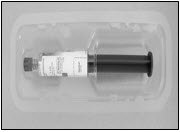
Figure 4

Figure 5
- HIZENTRA prefilled syringes can be placed directly in the infusion pump if the prefilled syringe size matches the pump requirements. If the prefilled syringe can be placed directly in the infusion pump, then go to Step 6.
NOTE:
An additional adapter may be required for the HIZENTRA prefilled syringes to fit properly in the infusion pump. Check with the provider of your supplies for the appropriate adapter and installation instructions.
- If the HIZENTRA prefilled syringe size does not match the infusion pump requirements, transfer the contents of the prefilled syringe to another syringe of a size specific for the infusion pump by following the directions below:
- Use a syringe-to-syringe transfer device (tip-to-tip connector) (Figure 6) to transfer the contents of the prefilled syringe to the empty syringe specific for the infusion pump.

Figure 6
- Remove the protective cap from the prefilled syringe. Attach the transfer device (tip-to-tip connector) by twisting it onto the prefilled syringe. Attach the empty syringe by screwing it onto the other side of the transfer device (Figure 7).
- Use a syringe-to-syringe transfer device (tip-to-tip connector) (Figure 6) to transfer the contents of the prefilled syringe to the empty syringe specific for the infusion pump.

Figure 7
|
Go to Step 6.
Step 5.2: Transfer HIZENTRA from vial to syringe
- Take the protective cap off the vial (Figure 8).

Figure 8
- Clean the vial stopper with an alcohol wipe (Figure 9). Let the stopper dry.

Figure 9
- Attach a needle or transfer device to a syringe tip, using aseptic technique.
- If using a transfer device, follow the instructions provided by the device manufacturer.
- If using a needle and a syringe to transfer HIZENTRA, follow the instructions below:
- Attach a sterile transfer needle to a sterile syringe (Figure 10).
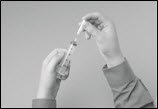
Figure 10
- Pull out the plunger of the syringe to fill the syringe with air. Make sure the amount of air is the same as the amount of HIZENTRA you will transfer from the vial.
- Put the HIZENTRA vial on a flat surface. Keeping the vial upright, insert the transfer needle into the center of the rubber stopper.
- Check that the tip of the needle is not in the liquid. Push the plunger of the syringe down. This will inject the air from the syringe into the airspace of the vial.
- Leaving the needle in the stopper, carefully turn the vial upside down (Figure 11).
Figure 11
- Slowly pull back on the plunger of the syringe to fill the syringe with HIZENTRA.
- Take the filled syringe and needle out of the stopper. Take off the needle and throw it away in the sharps container.
- Attach a sterile transfer needle to a sterile syringe (Figure 10).
When using multiple vials to achieve the prescribed dose, repeat this step.
Step 6: Prepare infusion pump and tubing
- Prior to preparing the pump(s), make sure you have the prescribed dose in the syringe(s) and the infusion tubing is attached.
- Prepare the infusion pump (following the manufacturer's instructions), including attaching any necessary adapters.
- Do not remove the needle caps until you are ready to infuse.
- Prime (fill) the infusion tubing. To prime the tubing, connect the syringe filled with HIZENTRA to the infusion tubing and gently push on the syringe plunger (e.g., using your fingers, thumb or the palm of your hand) to fill the tubing with HIZENTRA (Figure 12).
- Stop priming before HIZENTRA fluid reaches the capped needle.
- Insert the syringe filled with HIZENTRA into the infusion pump
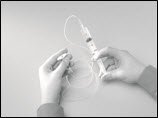
Figure 12
Step 7: Prepare infusion site(s)
- Select an area on your abdomen, thigh, upper arm, or side of upper leg/hip for the infusion (Figure 13).
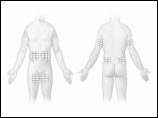
Figure 13
- Use a different site with every HIZENTRA infusion. New sites should be at least 1 inch from a previous infusion site.
- Never infuse into areas where the skin is tender, bruised, red, or hard. Avoid infusing into scars or stretch marks.
- You can use up to 8 infusion sites at the same time. If you are using more than one infusion site, at the same time, be sure the infusion sites are at least 2 inches apart. More than one infusion device can be used simultaneously.
- Clean the skin at each infusion site with an antiseptic skin prep (Figure 14). Let the skin dry.
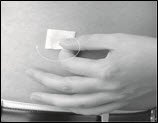
Figure 14
Step 8: Insert needle(s)
- Use one needle per site. If injecting in more than one site, the following steps should be completed for each needle, one at a time.
- Remove the needle cap.
- Using two fingers, pinch together the skin around the infusion site. With a quick dart-like motion, insert the needle straight into the skin (Figure 15).
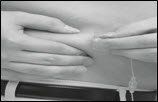
Figure 15
- Put sterile gauze and tape or a transparent dressing over the infusion site (Figure 16). This will keep the needle from coming out.
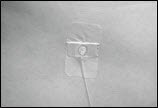
Figure 16
Step 9: Start infusion
- Follow the manufacturer's instructions to turn on the infusion pump and start the infusion (Figure 17).

Figure 17
Step 10: Complete infusion and record treatment (Figure 18)
- When all the HIZENTRA has been infused turn off the infusion pump (if used).
- Remove the needle(s) from the skin.
- Once you have removed the needle(s), remove the empty syringe from the infusion pump. Disconnect the infusion set from the empty syringe.
- Cover the infusion site with a protective dressing.
- Peel off the removable part of the label for each prefilled syringe or vial. Put this label in your log book with the date and time of the infusion and include the exact amount of HIZENTRA that you infused. Scan the prefilled syringe or vial if recording the infusion electronically.

Figure 18
Step 11: Clean up
- If applicable, remove adapter from the infusion pump following the manufacturer's instructions.
- Throw away the empty HIZENTRA prefilled syringe(s) or vial(s), along with the used disposable supplies, in the sharps container (Figure 19) in accordance with local requirements.
Figure 19
- Clean and store the infusion pump, following the manufacturer's instructions.
Be sure to tell your doctor about any problems you have doing your infusions. Your doctor may ask to see your treatment diary or log book, so be sure to take it with you each time you visit the doctor's office.
Call your doctor for medical advice about side effects. You can also report side effects to FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Manufactured by:
CSL Behring AG
Bern, Switzerland
U.S. License No. 1766
Distributed by:
CSL Behring LLC
Kankakee, IL 60901 USA
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Revised: 04/2023
PRINCIPAL DISPLAY PANEL - 5 mL Vial Carton
NDC 44206-451-01
1 g
5 mL
Immune Globulin
Subcutaneous (Human),
20% Liquid
Hizentra®
Single-dose vial
For Subcutaneous Administration
Only
Rx only
CSL Behring
PRINCIPAL DISPLAY PANEL - 10 mL Vial Carton
NDC 44206-452-02
2 g
10 mL
Immune Globulin
Subcutaneous (Human),
20% Liquid
Hizentra®
Single-dose vial
For Subcutaneous Administration
Only
Rx only
CSL Behring
PRINCIPAL DISPLAY PANEL - 20 mL Vial Carton
NDC 44206-454-04
4 g
20 mL
Immune Globulin
Subcutaneous (Human),
20% Liquid
Hizentra®
Single-dose vial
For Subcutaneous Administration
Only
Rx only
CSL Behring
PRINCIPAL DISPLAY PANEL - 50 mL Vial Carton
NDC 44206-455-10
10 g
50 mL
Immune Globulin
Subcutaneous (Human),
20% Liquid
Hizentra®
Single-dose vial
For Subcutaneous Administration
Only
Rx only
CSL Behring
PRINCIPAL DISPLAY PANEL - 5 mL Syringe Carton
NDC 44206-456-21
1 g
5 mL
Immune Globulin Subcutaneous (Human), 20% Liquid
Hizentra®
Single-dose prefilled syringe
For Subcutaneous Administration Only
Rx only
CSL Behring
PRINCIPAL DISPLAY PANEL - 10 mL Syringe Carton
NDC 44206-457-22
2 g
10 mL
Immune Globulin Subcutaneous (Human), 20% Liquid
Hizentra®
Single-dose prefilled syringe
For Subcutaneous Administration Only
Rx only
CSL Behring

| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| HIZENTRA
human immunoglobulin g liquid |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - CSL Behring AG (481152762) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| CSL Behring AG | 481152762 | MANUFACTURE | |
More about Hizentra (immune globulin subcutaneous)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Reviews (26)
- Latest FDA alerts (1)
- Side effects
- Dosage information
- During pregnancy
- FDA approval history
- Drug class: immune globulins
- En español