Traumatic Pneumothorax
Medically reviewed by Drugs.com. Last updated on May 6, 2024.
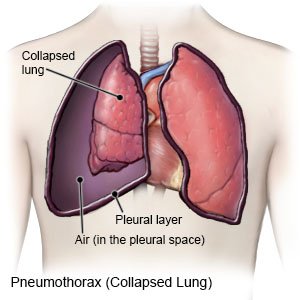
A traumatic pneumothorax is a collapsed lung. All or part of your lung may collapse. A traumatic pneumothorax is caused by an injury that tears your lung and allows air to enter the pleural space. The pleural space is the area between your lungs and your chest wall. The air trapped in your pleural space prevents your lung from filling, and it collapses. A pneumothorax can happen in one or both lungs.
 |
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
A pulse oximeter
is a device that measures the amount of oxygen in your blood. A cord with a clip or sticky strip is placed on your finger, ear, or toe. The other end of the cord is hooked to a machine.
A ventilator
is a machine that gives you oxygen and breathes for you when you cannot breathe well on your own. An endotracheal (ET) tube is put into your mouth or nose and attached to the ventilator. You may need a trach if an ET tube cannot be placed. A trach is a tube put through an incision and into your windpipe.
Medicines:
- Antibiotics help prevent or treat a bacterial infection.
- Pain medicine may be given if other pain medicines do not work. Do not wait until the pain is severe before you ask for more medicine.
- Sedatives help you stay calm and relaxed.
Tests:
- Blood tests may be used to measure the amount of oxygen and carbon dioxide. The results can tell healthcare providers how well your lungs are working.
- A heart monitor is used to record your heart's electrical activity.
- X-rays may be used to check the bones, lungs, and other tissues in your chest. The pictures may show broken ribs. X-rays may show the size of your pneumothorax and if you have fluid around your heart and lungs.
- CT scan or ultrasound pictures may be used to check for a pneumothorax that did not show up on a chest x-ray. You may be given contrast liquid to help your lungs show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
Treatment:
- Extra oxygen may be given if your oxygen level is too low. Oxygen may help the pneumothorax get better faster.
- Needle aspiration is used to pull the air out of your pleural space through a needle.
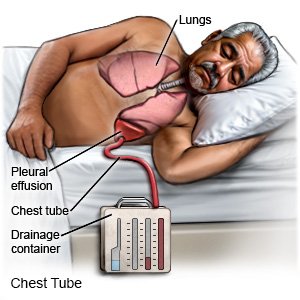
- A chest tube may be placed to remove air, blood, or fluid from around your collapsed lung. This allows your lung to fill with air when you breathe, and helps your heart beat normally. The chest tube is attached to a container to remove air and collect any blood or fluid.
- Pleurodesis is a procedure used to irritate the walls of your pleural space. This causes the walls to close so air can no longer be trapped.
- Surgery may be used to repair your lung.
RISKS:
- Air may continue to enter the pleural space and you may get a tension pneumothorax. With a tension pneumothorax, the injured lung and trapped air push against your uninjured lung. A tension pneumothorax can lead to low blood pressure, decreased oxygen in your blood, and heart problems.
- Without treatment, your lungs may completely collapse. Your heart could stop working. These risks can be life-threatening.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Traumatic Pneumothorax
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
