Nutropin Prescribing Information
Package insert / product label
Generic name: somatropin [ rDNA-origin ]
Dosage form: for injection
Drug class: Growth hormones
Medically reviewed by Drugs.com. Last updated on Mar 25, 2024.
On This Page
Nutropin Description
Nutropin® [somatropin (rDNA origin) for injection] is a human growth hormone (hGH) produced by recombinant DNA technology. Nutropin has 191 amino acid residues and a molecular weight of 22,125 daltons. The amino acid sequence of the product is identical to that of pituitary‑derived human growth hormone. The protein is synthesized by a specific laboratory strain of E. coli as a precursor consisting of the rhGH molecule preceded by the secretion signal from an E. coli protein. This precursor is directed to the plasma membrane of the cell. The signal sequence is removed and the native protein is secreted into the periplasm so that the protein is folded appropriately as it is synthesized.
Nutropin is a highly purified preparation. Biological potency is determined using a cell proliferation bioassay.
Nutropin is a sterile, white, lyophilized powder intended for subcutaneous administration after reconstitution with Bacteriostatic Water for Injection, USP (benzyl alcohol preserved). The reconstituted product is nearly isotonic at a concentration of 5 mg/mL growth hormone (GH) and has a pH of approximately 7.4.
Each 5 mg Nutropin vial contains 5 mg (approximately 15 IU) somatropin, lyophilized with 45 mg mannitol, 1.7 mg sodium phosphates (0.4 mg sodium phosphate monobasic and 1.3 mg sodium phosphate dibasic), and 1.7 mg glycine.
Each 10 mg Nutropin vial contains 10 mg (approximately 30 IU) somatropin, lyophilized with 90 mg mannitol, 3.4 mg sodium phosphates (0.8 mg sodium phosphate monobasic and 2.6 mg sodium phosphate dibasic), and 3.4 mg glycine.
Bacteriostatic Water for Injection, USP is sterile water containing 0.9 percent benzyl alcohol per mL as an antimicrobial preservative packaged in a multidose vial. The diluent pH is 4.5–7.0.
Nutropin - Clinical Pharmacology
General
In vitro and in vivo preclinical and clinical testing have demonstrated that Nutropin is therapeutically equivalent to pituitary‑derived human GH (hGH). Pediatric patients who lack adequate endogenous GH secretion, patients with chronic renal insufficiency, and patients with Turner syndrome that were treated with Nutropin resulted in an increase in growth rate and an increase in insulin‑like growth factor‑I (IGF‑I) levels similar to that seen with pituitary‑derived hGH.
Actions that have been demonstrated for Nutropin, somatrem, and/or pituitary‑derived hGH include:
A. Tissue Growth
- 1)
- Skeletal Growth: GH stimulates skeletal growth in pediatric patients with growth failure due to a lack of adequate secretion of endogenous GH or secondary to chronic renal insufficiency and in patients with Turner syndrome. Skeletal growth is accomplished at the epiphyseal plates at the ends of a growing bone. Growth and metabolism of epiphyseal plate cells are directly stimulated by GH and one of its mediators, IGF‑I. Serum levels of IGF‑I are low in children and adolescents who are GH deficient, but increase during treatment with GH. In pediatric patients, new bone is formed at the epiphyses in response to GH and IGF‑I. This results in linear growth until these growth plates fuse at the end of puberty.
- 2)
- Cell Growth: Treatment with hGH results in an increase in both the number and the size of skeletal muscle cells.
- 3)
- Organ Growth: GH influences the size of internal organs, including kidneys, and increases red cell mass. Treatment of hypophysectomized or genetic dwarf rats with GH results in organ growth that is proportional to the overall body growth. In normal rats subjected to nephrectomy‑induced uremia, GH promoted skeletal and body growth.
B. Protein Metabolism
Linear growth is facilitated in part by GH‑stimulated protein synthesis. This is reflected by nitrogen retention as demonstrated by a decline in urinary nitrogen excretion and blood urea nitrogen during GH therapy.
C. Carbohydrate Metabolism
GH is a modulator of carbohydrate metabolism. For example, patients with inadequate secretion of GH sometimes experience fasting hypoglycemia that is improved by treatment with GH. GH therapy may decrease insulin sensitivity. Untreated patients with chronic renal insufficiency and Turner syndrome have an increased incidence of glucose intolerance. Administration of hGH to adults or children resulted in increases in serum fasting and postprandial insulin levels, more commonly in overweight or obese individuals. In addition, mean fasting and postprandial glucose and hemoglobin A1c levels remained in the normal range.
D. Lipid Metabolism
In GH‑deficient patients, administration of GH resulted in lipid mobilization, reduction in body fat stores, increased plasma fatty acids, and decreased plasma cholesterol levels.
E. Mineral Metabolism
The retention of total body potassium in response to GH administration apparently results from cellular growth. Serum levels of inorganic phosphorus may increase slightly in patients with inadequate secretion of endogenous GH, chronic renal insufficiency, or patients with Turner syndrome during GH therapy due to metabolic activity associated with bone growth as well as increased tubular reabsorption of phosphate by the kidney. Serum calcium is not significantly altered in these patients. Sodium retention also occurs. Adults with childhood‑onset GH deficiency show low bone mineral density (BMD). GH therapy results in increases in serum alkaline phosphatase. (See PRECAUTIONS: Laboratory Tests.)
Pharmacokinetics
Subcutaneous Absorption
The absolute bioavailability of recombinant human growth hormone (rhGH) after subcutaneous administration in healthy adult males has been determined to be 81±20%. The mean terminal t½ after subcutaneous administration is significantly longer than that seen after intravenous administration (2.1±0.43 hours vs. 19.5±3.1 minutes) indicating that the subcutaneous absorption of the compound is slow and rate‑limiting.
Distribution
Animal studies with rhGH showed that GH localizes to highly perfused organs, particularly the liver and kidney. The volume of distribution at steady state for rhGH in healthy adult males is about 50 mL/kg body weight, approximating the serum volume.
Metabolism
Both the liver and kidney have been shown to be important metabolizing organs for GH. Animal studies suggest that the kidney is the dominant organ of clearance. GH is filtered at the glomerulus and reabsorbed in the proximal tubules. It is then cleaved within renal cells into its constituent amino acids, which return to the systemic circulation.
Elimination
The mean terminal t½ after intravenous administration of rhGH in healthy adult males is estimated to be 19.5±3.1 minutes. Clearance of rhGH after intravenous administration in healthy adults and children is reported to be in the range of 116–174 mL/hr/kg.
Bioequivalence of Formulations
Nutropin has been determined to be bioequivalent to Nutropin AQ® [somatropin (rDNA origin) injection] based on the statistical evaluation of AUC and Cmax.
SPECIAL POPULATIONS
Pediatric
Available literature data suggest that rhGH clearances are similar in adults and children.
Gender
No data are available for exogenously administered rhGH. Available data for methionyl recombinant GH, pituitary‑derived GH, and endogenous GH suggest no consistent gender‑based differences in GH clearance.
Geriatrics
Limited published data suggest that the plasma clearance and average steady‑state plasma concentration of rhGH may not be different between young and elderly patients.
Race
Reported values for half‑lives for endogenous GH in normal adult black males are not different from observed values for normal adult white males. No data for other races are available.
Growth Hormone Deficiency (GHD)
Reported values for clearance of rhGH in adults and children with GHD range 138–245 mL/hr/kg and are similar to those observed in healthy adults and children. Mean terminal t½ values following intravenous and subcutaneous administration in adult and pediatric GHD patients are also similar to those observed in healthy adult males.
Renal Insufficiency
Children and adults with chronic renal failure (CRF) and end‑stage renal disease (ESRD) tend to have decreased clearance compared to normals. In a study with six pediatric patients 7 to 11 years of age, the clearance of Nutropin was reduced by 21.5% and 22.6% after the intravenous infusion and subcutaneous injection, respectively, of 0.05 mg/kg of Nutropin compared to normal healthy adults. Endogenous GH production may also increase in some individuals with ESRD. However, no rhGH accumulation has been reported in children with CRF or ESRD dosed with current regimens.
Turner Syndrome
No pharmacokinetic data are available for exogenously administered rhGH. However, reported half‑lives, absorption, and elimination rates for endogenous GH in this population are similar to the ranges observed for normal subjects and GHD populations.
Hepatic Insufficiency
A reduction in rhGH clearance has been noted in patients with severe liver dysfunction. The clinical significance of this decrease is unknown.
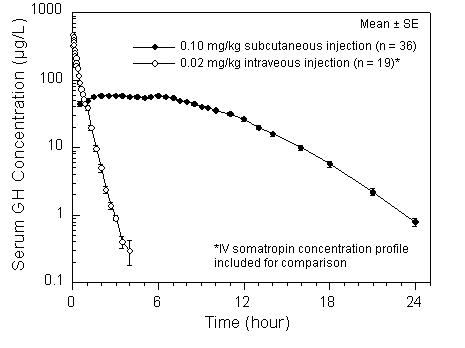
| Cmax (µg/L) | Tmax (hr) | t½ (hr) | AUC0-∞ (µg ∙ hr/L) | CL/Fsc (mL/[hr ∙ kg]) | |
|---|---|---|---|---|---|
| Abbreviations: | |||||
| Cmax=maximum concentration | |||||
| t½=half‑life | |||||
| AUC0-∞=area under the curve | |||||
| CL/Fsc=systemic clearance | |||||
| Fsc=subcutaneous bioavailability (not determined) | |||||
| CV%=coefficient of variation in %; SC=subcutaneous | |||||
| MEAN† | 67.2 | 6.2 | 2.1 | 643 | 158 |
| CV% | 29 | 37 | 20 | 12 | 12 |
Single Dose Mean Growth Hormone Concentrations in Healthy Adult Males
Clinical Studies
Growth Hormone Deficiency (GHD) in Pubertal Patients
One open‑label, multicenter, randomized clinical trial of two dosages of Nutropin was performed in pubertal patients with GHD. Ninety‑seven patients (mean age 13.9 years, 83 male, 14 female) currently being treated with approximately 0.3 mg/kg/wk of GH were randomized to 0.3 mg/kg/wk or 0.7 mg/kg/wk Nutropin doses. All patients were already in puberty (Tanner stage ≥2) and had bone ages ≤14 years in males or ≤12 years in females. Mean baseline height standard deviation (SD) score was –1.3.
The mean last measured height in all 97 patients after a mean duration of 2.7±1.2 years, by analysis of covariance (ANCOVA) adjusting for baseline height, is shown below.
| Last Measured Height* (cm) | Height Difference Between Groups (cm) | |||
|---|---|---|---|---|
| Age (yr) | 0.3 mg/kg/wk | 0.7 mg/kg/wk | ||
| Mean±SD (range) | Mean±SD | Mean±SD | Mean±SE | |
|
||||
| Male | 17.2±1.3 (13.6 to 19.4) | 170.9±7.9 (n=42) | 174.5±7.9 (n=41) | 3.6±1.7 |
| Female | 15.8±1.8 (11.9 to 19.3) | 154.7±6.3 (n=7) | 157.6±6.3 (n=7) | 2.9±3.4 |
The mean height SD score at last measured height (n=97) was –0.7±1.0 in the 0.3 mg/kg/wk group and –0.1± 1.2 in the 0.7 mg/kg/wk group. For patients completing 3.5 or more years (mean 4.1 years) of Nutropin treatment (15/49 patients in the 0.3 mg/kg/wk group and 16/48 patients in the 0.7 mg/kg/wk group), the mean last measured height was 166.1±8.0 cm in the 0.3 mg/kg/wk group and 171.8±7.1 cm in the 0.7 mg/kg/wk group, adjusting for baseline height and sex.
The mean change in bone age was approximately one year for each year in the study in both dose groups. Patients with baseline height SD scores above –1.0 were able to attain normal adult heights with the 0.3 mg/kg/wk dose of Nutropin (mean height SD score at near‑adult height=–0.1, n=15).
Thirty‑one patients had bone mineral density (BMD) determined by dual energy x‑ray absorptiometry (DEXA) scans at study conclusion. The two dose groups did not differ significantly in mean SD score for total body BMD (–0.9±1.9 in the 0.3 mg/kg/wk group vs. –0.8±1.2 in the 0.7 mg/kg/wk group, n=20) or lumbar spine BMD (–1.0±1.0 in the 0.3 mg/kg/wk group vs. –0.2±1.7 in the 0.7 mg/kg/wk group, n=21).
Over a mean duration of 2.7 years, patients in the 0.7 mg/kg/wk group were more likely to have IGF‑I values above the normal range than patients in the 0.3 mg/kg/wk group (27.7% vs. 9.0% of IGF‑I measurements for individual patients). The clinical significance of elevated IGF‑I values is unknown.
Effects of Nutropin on Growth Failure Due to Chronic Renal Insufficiency (CRI)
Two multicenter, randomized, controlled clinical trials were conducted to determine whether treatment with Nutropin prior to renal transplantation in patients with chronic renal insufficiency could improve their growth rates and height deficits. One study was a double‑blind, placebo‑controlled trial and the other was an open‑label, randomized trial. The dose of Nutropin in both controlled studies was 0.05 mg/kg/day (0.35 mg/kg/week) administered daily by subcutaneous injection. Combining the data from those patients completing two years in the two controlled studies results in 62 patients treated with Nutropin and 28 patients in the control groups (either placebo‑treated or untreated). The mean first year growth rate was 10.8 cm/yr for Nutropin‑treated patients, compared with a mean growth rate of 6.5 cm/yr for placebo/untreated controls (p<0.00005). The mean second year growth rate was 7.8 cm/yr for the Nutropin‑treated group, compared with 5.5 cm/yr for controls (p<0.00005). There was a significant increase in mean height standard deviation (SD) score in the Nutropin group (−2.9 at baseline to −1.5 at Month 24, n=62) but no significant change in the controls (−2.8 at baseline to −2.9 at Month 24, n=28). The mean third year growth rate of 7.6 cm/yr in the Nutropin‑treated patients (n=27) suggests that Nutropin stimulates growth beyond two years. However, there are no control data for the third year because control patients crossed over to Nutropin treatment after two years of participation. The gains in height were accompanied by appropriate advancement of skeletal age. These data demonstrate that Nutropin therapy improves growth rate and corrects the acquired height deficit associated with chronic renal insufficiency.
Post-Transplant Growth
The North American Pediatric Renal Transplant Cooperative Study (NAPRTCS) has reported data for growth post‑transplant in children who did not receive GH prior to transplantation as well as children who did receive Nutropin during the clinical trials prior to transplantation. The average change in height SD score during the initial two years post transplant was 0.15 for the 2391 patients who did not receive GH pre-transplant and 0.28 for the 57 patients who did (J Pediatr. 2000;136:376-382). For patients who were followed for 5 years post-transplant, the corresponding changes in height SD score were also similar between groups.
Turner Syndrome
One long‑term, randomized, open‑label, multicenter, concurrently controlled study, two long‑term, open‑label, multicenter, historically controlled studies, and one long‑term, randomized, dose‑response study were conducted to evaluate the efficacy of GH for the treatment of girls with short stature due to Turner syndrome.
In the randomized study GDCT, comparing GH‑treated patients to a concurrent control group who received no GH, the GH‑treated patients who received a dose of 0.3 mg/kg/week given 6 times per week from a mean age of 11.7 years for a mean duration of 4.7 years attained a mean near final height of 146.0 cm (n=27) as compared to the control group who attained a near final height of 142.1 cm (n=19). By analysis of covariance, the effect of GH therapy was a mean height increase of 5.4 cm (p=0.001).
In two of the studies (85‑023 and 85‑044), the effect of long‑term GH treatment (0.375 mg/kg/week given either 3 times per week or daily) on adult height was determined by comparing adult heights in the treated patients with those of age‑matched historical controls with Turner syndrome who never received any growth‑promoting therapy. In Study 85‑023, estrogen treatment was delayed until patients were at least age 14. GH therapy resulted in a mean adult height gain of 7.4 cm (mean duration of GH therapy of 7.6 years) vs. matched historical controls by analysis of covariance.
In Study 85‑044, patients treated with early GH therapy were randomized to receive estrogen‑replacement therapy (conjugated estrogens, 0.3 mg escalating to 0.625 mg daily) at either age 12 or 15 years. Compared with matched historical controls, early GH therapy (mean duration of GH therapy 5.6 years) combined with estrogen replacement at age 12 years resulted in an adult height gain of 5.9 cm (n=26), whereas girls who initiated estrogen at age 15 years (mean duration of GH therapy 6.1 years) had a mean adult height gain of 8.3 cm (n=29). Patients who initiated GH therapy after age 11 (mean age 12.7 years; mean duration of GH therapy 3.8 years) had a mean adult height gain of 5.0 cm (n=51).
Thus, in both studies, 85‑023 and 85‑044, the greatest improvement in adult height was observed in patients who received early GH treatment and estrogen after age 14 years.
In a randomized, blinded, dose‑response study, GDCI, patients were treated from a mean age of 11.1 years for a mean duration of 5.3 years with a weekly dose of either 0.27 mg/kg or 0.36 mg/kg administered 3 or 6 times weekly. The mean near final height of patients receiving growth hormone was 148.7 cm (n=31). This represents a mean gain in adult height of approximately 5 cm compared with previous observations of untreated Turner syndrome girls.
In these studies, Turner syndrome patients (n=181) treated to final adult height achieved statistically significant average estimated adult height gains ranging from 5.0–8.3 cm.
Idiopathic Short Stature (ISS)
A long‑term, open‑label, multicenter study (86‑053) was conducted to examine the safety and efficacy of Nutropin in pediatric patients with idiopathic short stature, also called non‑GH deficient short stature. For the first year, 122 pre‑pubertal subjects over the age of 5 years with stimulated serum GH≥10 ng/mL were randomized into two treatment groups of approximately equal size; one group was treated with Nutropin 0.3 mg/kg weekly divided into three doses per week (TIW) and the other group served as untreated controls. For the second and subsequent years of the study, all subjects were re‑randomized to receive the same total weekly dose of Nutropin (0.3 mg/kg weekly) administered either daily or TIW. Treatment with Nutropin was continued until a subject’s bone age was >15.0 years (boys) or >14.0 years (girls) and the growth rate was <2 cm/yr, after which subjects were followed until adult height was achieved. The mean baseline values were: height SD score –2.8, IGF‑I SD score –0.9, age 9.4 years, bone age 7.8 years, growth rate 4.4 cm/yr, mid‑parental target height SD score –0.7, and Bayley‑Pinneau predicted adult height SD score –2.3. Nearly all subjects had predicted adult height that was less than mid‑parental target height.
During the one‑year controlled phase of the study, the mean height velocity increased by 0.5±1.8 cm (mean±SD) in the no‑treatment control group and by 3.1±1.7 cm in the Nutropin group (p<0.0001). For the same period of treatment the mean height SD score increased by 0.4±0.2 and remained unchanged (0.0±0.2) in the control group (p<0.001).
Of the 118 subjects who were treated with Nutropin in Study 86‑053, 83 (70%) reached near‑adult height (hereafter called adult height) after 2–10 years of Nutropin therapy. Their last measured height, including post‑treatment follow‑up, was obtained at a mean age of 18.3 years in males and 17.3 years in females. The mean duration of therapy was 6.2 and 5.5 years, respectively. Adult height was greater than pretreatment predicted adult height in 49 of 60 males (82%) and 19 of 23 females (83%). The mean difference between adult height and pretreatment predicted adult height was 5.2 cm (2.0 inches) in males and 6.0 cm (2.4 inches) in females (p<0.0001 for both). The table (below) summarizes the efficacy data.
| Characteristic | Males(n=60) | Females(n=23) | ||||
|---|---|---|---|---|---|---|
|
||||||
| Adult height (cm) | 166.3±5.8 | 153.1±4.8 | ||||
| Pretreatment predicted adult height (cm) | 161.1±5.5 | 147.1±5.1 | ||||
| Adult height minus pretreatment
predicted adult height (cm) | +5.2±5.0 * | +6.0±5.0 * | ||||
| Adult height SD score | –1.5±0.8 | –1.6±0.7 | ||||
| Pretreatment predicted adult height SD score | –2.2±0.8 | –2.5±0.8 | ||||
| Adult height minus pretreatment
predicted adult height SD score | +0.7±0.7 * | +0.9±0.8 * | ||||
Nutropin therapy resulted in an increase in mean IGF‑I SD score from –0.9±1.0 to –0.2±0.9 in Treatment Year 1. During continued treatment, mean IGF‑I levels remained close to the normal mean. IGF‑I SD scores above +2 occurred sporadically in 14 subjects.
Adult Growth Hormone Deficiency (GHD)
Two multicenter, double‑blind, placebo‑controlled clinical trials were conducted using Nutropin [somatropin (rDNA origin) for injection] in GH‑deficient adults. One study was conducted in subjects with adult‑onset GHD, mean age 48.3 years, n=166, at doses of 0.0125 or 0.00625 mg/kg/day; doses of 0.025 mg/kg/day were not tolerated in these subjects. A second study was conducted in previously treated subjects with childhood‑onset GHD, mean age 23.8 years, n=64, at randomly assigned doses of 0.025 or 0.0125 mg/kg/day. The studies were designed to assess the effects of replacement therapy with GH on body composition.
Significant changes from baseline to Month 12 of treatment in body composition (i.e., total body % fat mass, trunk % fat mass, and total body % lean mass by DEXA scan) were seen in all Nutropin groups in both studies (p<0.0001 for change from baseline and vs. placebo), whereas no statistically significant changes were seen in either of the placebo groups. In the adult‑onset study, the Nutropin group improved mean total body fat from 35.0% to 31.5%, mean trunk fat from 33.9% to 29.5%, and mean lean body mass from 62.2% to 65.7%, whereas the placebo group had mean changes of 0.2% or less (p=not significant). Due to the possible effect of GH‑induced fluid retention on DEXA measurements of lean body mass, DEXA scans were repeated approximately 3 weeks after completion of therapy; mean % lean body mass in the Nutropin group was 65.0%, a change of 2.8% from baseline, compared with a change of 0.4% in the placebo group (p<0.0001 between groups).
In the childhood‑onset study, the high‑dose Nutropin group improved mean total body fat from 38.4% to 32.1%, mean trunk fat from 36.7% to 29.0%, and mean lean body mass from 59.1% to 65.5%; the low‑dose Nutropin group improved mean total body fat from 37.1% to 31.3%, mean trunk fat from 37.9% to 30.6%, and mean lean body mass from 60.0% to 66.0%; the placebo group had mean changes of 0.6% or less (p=not significant).
| M0431g | M0381g | ||||||
|---|---|---|---|---|---|---|---|
| Proportion | Placebo (n=62) | Nutropin (n=63) | Between-Groups t‑test p‑value | Placebo (n=13) | Nutropin 0.0125 mg/kg/day (n=15) | Nutropin 0.025 mg/kg/day (n=15) | Placebo vs. Pooled
Nutropin t‑test p‑value |
| Total body percent fat | |||||||
| Baseline | 36.8 | 35.0 | 0.38 | 35.0 | 37.1 | 38.4 | 0.45 |
| Month 12 | 36.8 | 31.5 | 35.2 | 31.3 | 32.1 | ||
| Baseline to Month 12 change | −0.1 | −3.6 | <0.0001 | + 0.2 | −5.8 | −6.3 | <0.0001 |
| Post-washout | 36.4 | 32.2 | N/A | N/A | N/A | ||
| Baseline to post-washout change | −0.4 | −2.8 | <0.0001 | N/A | N/A | N/A | |
| Trunk percent fat | |||||||
| Baseline | 35.3 | 33.9 | 0.50 | 32.5 | 37.9 | 36.7 | 0.23 |
| Month 12 | 35.4 | 29.5 | 33.1 | 30.6 | 29.0 | ||
| Baseline to Month 12 change | 0.0 | −4.3 | <0.0001 | + 0.6 | −7.3 | −7.6 | <0.0001 |
| Post-washout | 34.9 | 30.5 | N/A | N/A | N/A | ||
| Baseline to post-washout change | −0.3 | −3.4 | N/A | N/A | N/A | ||
| Total body percent lean | |||||||
| Baseline | 60.4 | 62.2 | 0.37 | 62.0 | 60.0 | 59.1 | 0.48 |
| Month 12 | 60.5 | 65.7 | 61.8 | 66.0 | 65.5 | ||
| Baseline to Month 12 change | + 0.2 | + 3.6 | <0.0001 | −0.2 | + 6.0 | + 6.4 | <0.0001 |
| Post-washout | 60.9 | 65.0 | N/A | N/A | N/A | ||
| Baseline to post-washout change | + 0.4 | + 2.8 | <0.0001 | N/A | N/A | N/A | |
In the adult‑onset study, significant decreases from baseline to Month 12 in LDL cholesterol and LDL:HDL ratio were seen in the Nutropin group compared to the placebo group, p<0.02; there were no statistically significant between‑group differences in change from baseline to Month 12 in total cholesterol, HDL cholesterol, or triglycerides. In the childhood‑onset study, significant decreases from baseline to Month 12 in total cholesterol, LDL cholesterol, and LDL:HDL ratio were seen in the high‑dose Nutropin group only, compared to the placebo group, p<0.05. There were no statistically significant between‑group differences in HDL cholesterol or triglycerides from baseline to Month 12.
In the childhood‑onset study, 55% of the patients had decreased spine bone mineral density (BMD) (z‑score <–1) at baseline. The administration of Nutropin (n=16) (0.025 mg/kg/day) for two years resulted in increased spine BMD from baseline when compared to placebo (n=13) (4.6% vs. 1.0%, respectively, p<0.03); a transient decrease in spine BMD was seen at six months in the Nutropin‑treated patients. Thirty‑five percent of subjects treated with this dose had supraphysiological levels of IGF‑I at some point during the study, which may carry unknown risks. No significant improvement in total body BMD was found when compared to placebo. A lower GH dose (0.0125 mg/kg/day) did not show significant increments in either of these bone parameters when compared to placebo. No statistically significant effects on BMD were seen in the adult‑onset study where patients received GH (0.0125 mg/kg/day) for one year.
Muscle strength, physical endurance, and quality of life measurements were not markedly abnormal at baseline, and no statistically significant effects of Nutropin therapy were observed in the two studies.
A subsequent 32‑week, multicenter, open‑label, controlled clinical trial (M2378g) was conducted using Nutropin AQ, Nutropin Depot, or no treatment in adults with both adult‑onset and childhood‑onset GHD. Subjects were randomized into the three groups to evaluate effects on body composition, including change in visceral adipose tissue (VAT) as determined by computed tomography (CT) scan.
For subjects evaluable for change in VAT in the Nutropin AQ (n=44) and untreated (n=19) groups, the mean age was 46.2 years and 78% had adult‑onset GHD. Subjects in the Nutropin AQ group were treated at doses up to 0.012 mg/kg per day in women (all of whom received estrogen replacement therapy) and men under age 35 years, and up to 0.006 mg/kg per day in men over age 35 years.
The mean absolute change in VAT from baseline to Week 32 was –10.7 cm2 in the Nutropin AQ group and +8.4 cm2 in the untreated group (p=0.013 between groups). There was a 6.7% VAT loss in the Nutropin AQ group (mean percent change from baseline to Week 32) compared with a 7.5% increase in the untreated group (p=0.012 between groups). The effect of reducing VAT in adult GHD patients with Nutropin AQ on long‑term cardiovascular morbidity and mortality has not been determined.
| Nutropin AQ (n = 44) | Untreated (n = 19) | Treatment Difference (adjusted mean) | p-value | |
|---|---|---|---|---|
|
||||
| Baseline VAT (cm2)(mean) | 126.2 | 123.3 | ||
| Change in VAT (cm2)(adjusted mean) | -10.7 | +8.4 | -19.1 | 0.013* |
| Percent change in VAT (adjusted mean) | -6.7 | +7.5 | -14.2 | 0.012* |
Indications and Usage for Nutropin
Pediatric Patients
Nutropin® [somatropin (rDNA origin) for injection] is indicated for the long‑term treatment of growth failure due to a lack of adequate endogenous GH secretion.
Nutropin® [somatropin (rDNA origin) for injection] is also indicated for the treatment of growth failure associated with chronic renal insufficiency up to the time of renal transplantation. Nutropin therapy should be used in conjunction with optimal management of chronic renal insufficiency.
Nutropin® [somatropin (rDNA origin) for injection] is also indicated for the long‑term treatment of short stature associated with Turner syndrome.
Nutropin® [somatropin (rDNA origin) for injection] is also indicated for the long‑term treatment of idiopathic short stature, also called non‑growth hormone‑deficient short stature, defined by height SDS ≤–2.25, and associated with growth rates unlikely to permit attainment of adult height in the normal range, in pediatric patients whose epiphyses are not closed and for whom diagnostic evaluation excludes other causes associated with short stature that should be observed or treated by other means.
Adult Patients
Nutropin® [somatropin (rDNA origin) for injection] is indicated for the replacement of endogenous growth hormone in adults with growth hormone deficiency who meet either of the following two criteria:
Adult Onset: Patients who have adult growth hormone deficiency either alone or associated with multiple hormone deficiencies (hypopituitarism) as a result of pituitary disease, hypothalamic disease, surgery, radiation therapy, or trauma; or
Childhood Onset: Patients who were growth hormone deficient during childhood as a result of congenital, genetic, acquired, or idiopathic causes.
In general, confirmation of the diagnosis of adult growth hormone deficiency in both groups usually requires an appropriate growth hormone stimulation test. However, confirmatory growth hormone stimulation testing may not be required in patients with congenital/genetic growth hormone deficiency or multiple pituitary hormone deficiencies due to organic disease.
Contraindications
Somatropin should not be used for growth promotion in pediatric patients with closed epiphyses.
Somatropin is contraindicated in patients with active proliferative or severe non-proliferative diabetic retinopathy.
In general, somatropin is contraindicated in the presence of active malignancy. Any pre‑existing malignancy should be inactive and its treatment complete prior to instituting therapy with somatropin. Somatropin should be discontinued if there is evidence of recurrent activity. Since growth hormone deficiency may be an early sign of the presence of a pituitary tumor (or, rarely, other brain tumors), the presence of such tumors should be ruled out prior to initiation of treatment. Somatropin should not be used in patients with any evidence of progression or recurrence of an underlying intracranial tumor.
Somatropin should not be used to treat patients with acute critical illness due to complications following open heart surgery, abdominal surgery or multiple accidental trauma, or those with acute respiratory failure. Two placebo‑controlled clinical trials in non‑growth hormone‑deficient adult patients (n=522) with these conditions in intensive care units revealed a significant increase in mortality (41.9% vs. 19.3%) among somatropin‑treated patients (doses 5.3–8 mg/day) compared to those receiving placebo (see WARNINGS).
Somatropin is contraindicated in patients with Prader‑Willi syndrome who are severely obese or have severe respiratory impairment (see WARNINGS). Unless patients with Prader‑Willi syndrome also have a diagnosis of growth hormone deficiency, Nutropin is not indicated for the long‑term treatment of pediatric patients who have growth failure due to genetically confirmed Prader‑Willi syndrome.
Nutropin, when reconstituted with Bacteriostatic Water for Injection, USP (benzyl alcohol preserved), should not be used in patients with a known sensitivity to benzyl alcohol. For use in newborns see WARNINGS.
Warnings
See CONTRAINDICATIONS for information on increased mortality in patients with acute critical illness due to complications following open heart surgery, abdominal surgery or multiple accidental trauma, or those with acute respiratory failure. The safety of continuing somatropin treatment in patients receiving replacement doses for approved indications who concurrently develop these illnesses has not been established. Therefore, the potential benefit of treatment continuation with somatropin in patients having acute critical illnesses should be weighed against the potential risk.
There have been reports of fatalities after initiating therapy with somatropin in pediatric patients with Prader‑Willi syndrome who had one or more of the following risk factors: severe obesity, history of upper airway obstruction or sleep apnea, or unidentified respiratory infection. Male patients with one or more of these factors may be at greater risk than females. Patients with Prader‑Willi syndrome should be evaluated for signs of upper airway obstruction and sleep apnea before initiation of treatment with somatropin. If, during treatment with somatropin, patients show signs of upper airway obstruction (including onset of or increased snoring) and/or new onset sleep apnea, treatment should be interrupted. All patients with Prader‑Willi syndrome treated with somatropin should also have effective weight control and be monitored for signs of respiratory infection, which should be diagnosed as early as possible and treated aggressively (see CONTRAINDICATIONS). Unless patients with Prader‑Willi syndrome also have a diagnosis of growth hormone deficiency, Nutropin is not indicated for the long‑term treatment of pediatric patients who have growth failure due to genetically confirmed Prader‑Willi syndrome.
Benzyl alcohol as a preservative in Bacteriostatic Water for Injection, USP, has been associated with toxicity in newborns. When administering Nutropin to newborns, reconstitute with Sterile Water for Injection, USP. USE ONLY ONE DOSE PER NUTROPIN VIAL AND DISCARD THE UNUSED PORTION.
Precautions
General
Nutropin should be prescribed by physicians experienced in the diagnosis and management of patients with GH deficiency, idiopathic short stature, Turner syndrome, or chronic renal insufficiency. No studies have been completed evaluating Nutropin therapy in patients who have received renal transplants. Currently, treatment of patients with functioning renal allografts is not indicated.
Treatment with somatropin may decrease insulin sensitivity, particularly at higher doses in susceptible patients. As a result, previously undiagnosed impaired glucose tolerance and overt diabetes mellitus may be unmasked during somatropin treatment. Therefore, glucose levels should be monitored periodically in all patients treated with somatropin, especially in those with risk factors for diabetes mellitus, such as obesity (including obese patients with Prader-Willi syndrome), Turner syndrome, or a family history of diabetes mellitus. Patients with preexisting type 1 or type 2 diabetes mellitus or impaired glucose tolerance should be monitored closely during somatropin therapy. The doses of antihyperglycemic drugs (i.e., insulin or oral agents) may require adjustment when somatropin therapy is instituted in these patients.
In subjects treated in a long‑term study of Nutropin for idiopathic short stature, mean fasting and postprandial insulin levels increased, while mean fasting and postprandial glucose levels remained unchanged. Mean hemoglobin A1c levels rose slightly from baseline as expected during adolescence; sporadic values outside normal limits occurred transiently.
Nutropin therapy in adults with GH deficiency of adult onset was associated with an increase of median fasting insulin level in the Nutropin 0.0125 mg/kg/day group from 9.0 µU/mL at baseline to 13.0 µU/mL at Month 12 with a return to the baseline median level after a 3‑week post‑washout period of GH therapy. In the placebo group there was no change from 8.0 µU/mL at baseline to Month 12, and after the post‑washout period the median level was 9.0 µU/mL. The between‑treatment groups difference on change from baseline to Month 12 in median fasting insulin level was significant, p<0.0001. In childhood‑onset subjects, there was an increase of median fasting insulin level in the Nutropin 0.025 mg/kg/day group from 11.0 µU/mL at baseline to 20.0 µU/mL at Month 12, in the Nutropin 0.0125 mg/kg/day group from 8.5 µU/mL to 11.0 µU/mL, and in the placebo group from 7.0 µU/mL to 8.0 µU/mL. The between‑treatment groups differences for these changes were significant, p=0.0007.
In subjects with adult-onset GH deficiency , there were no between-treatment group differences on changes from baseline to Month 12 in mean HbA1c level, p = 0.08. In childhood-onset GH deficiency, the mean HbA1c level increased in the Nutropin 0.025 mg/kg/day group from 5.2% at baseline to 5.5% at Month 12, and did not change in the Nutropin 0.0125 mg/kg/day group from 5.1% at baseline or in the placebo group from 5.3% at baseline. The between-treatment group differences were significant, p = 0.009.
Patients with preexisting tumors or growth hormone deficiency secondary to an intracranial lesion should be examined routinely for progression or recurrence of the underlying disease process. In pediatric patients, clinical literature has revealed no relationship between somatropin replacement therapy and central nervous system (CNS) tumor recurrence or new extracranial tumors. However, in childhood cancer survivors, an increased risk of a second neoplasm has been reported in patients treated with somatropin after their first neoplasm. Intracranial tumors, in particular meningiomas, in patients treated with radiation to the head for their first neoplasm, were the most common of these second neoplasms. In adults, it is unknown whether there is any relationship between somatropin replacement therapy and CNS tumor recurrence.
Intracranial hypertension (IH) with papilledema, visual changes, headache, nausea, and/or vomiting has been reported in a small number of patients treated with somatropin products. Symptoms usually occurred within the first eight (8) weeks after the initiation of somatropin therapy. In all reported cases, IH-associated signs and symptoms rapidly resolved after cessation of therapy or a reduction of the somatropin dose. Funduscopic examination should be performed routinely before initiating treatment with somatropin to exclude preexisting papilledema, and periodically during the course of somatropin therapy. If papilledema is observed by funduscopy during somatropin treatment, treatment should be stopped. If somatropin-induced IH is diagnosed, treatment with somatropin can be restarted at a lower dose after IH-associated signs and symptoms have resolved. Patients with Turner syndrome, CRI, and Prader-Willi syndrome may be at increased risk for the development of IH.
In patients with hypopituitarism (multiple hormone deficiencies), standard hormonal replacement therapy should be monitored closely when somatropin therapy is administered.
Undiagnosed/untreated hypothyroidism may prevent an optimal response to somatropin, in particular, the growth response in children. Patients with Turner syndrome have an inherently increased risk of developing autoimmune thyroid disease and primary hypothyroidism. In patients with growth hormone deficiency, central (secondary) hypothyroidism may first become evident or worsen during somatropin treatment. Therefore, patients treated with somatropin should have periodic thyroid function tests and thyroid hormone replacement therapy should be initiated or appropriately adjusted when indicated.
Patients should be monitored carefully for any malignant transformation of skin lesions.
When somatropin is administered subcutaneously at the same site over a long period of time, tissue atrophy may result. This can be avoided by rotating the injection site.
As with any protein, local or systemic allergic reactions may occur. Parents/Patients should be informed that such reactions are possible and that prompt medical attention should be sought if allergic reactions occur.
Pediatric Patients
(see PRECAUTIONS, General)
Slipped capital femoral epiphysis may occur more frequently in patients with endocrine disorders (including GH deficiency and Turner syndrome) or in patients undergoing rapid growth. Any pediatric patient with the onset of a limp or complaints of hip or knee pain during somatropin therapy should be carefully evaluated.
Children with growth failure secondary to CRI should be examined periodically for evidence of progression of renal osteodystrophy. Slipped capital femoral epiphysis or avascular necrosis of the femoral head may be seen in children with advanced renal osteodystrophy, and it is uncertain whether these problems are affected by somatropin therapy. X-rays of the hip should be obtained prior to initiating somatropin therapy in CRI patients. Physicians and parents should be alert to the development of a limp or complaints of hip or knee pain in CRI patients treated with Nutropin.
Progression of scoliosis can occur in patients who experience rapid growth. Because somatropin increases growth rate, patients with a history of scoliosis who are treated with somatropin should be monitored for progression of scoliosis. However, somatropin has not been shown to increase the occurrence of scoliosis. Skeletal abnormalities including scoliosis are commonly seen in untreated Turner syndrome patients. Scoliosis is also commonly seen in untreated patients with Prader-Willi syndrome. Physicians should be alert to these abnormalities, which may manifest during somatropin therapy.
Patients with Turner syndrome should be evaluated carefully for otitis media and other ear disorders since these patients have an increased risk of ear and hearing disorders. In a randomized, controlled trial, there was a statistically significant increase, as compared to untreated controls, in otitis media (43% vs. 26%) and ear disorders (18% vs. 5%) in patients receiving somatropin. In addition, patients with Turner syndrome should be monitored closely for cardiovascular disorders (e.g., stroke, aortic aneurysm/dissection, hypertension) as these patients are also at risk for these conditions.
Adult Patients
(see PRECAUTIONS, General)
Patients with epiphyseal closure who were treated with somatropin replacement therapy in childhood should be reevaluated according to the criteria in INDICATIONS AND USAGE before continuation of somatropin therapy at the reduced dose level recommended for GH deficient adults. Fluid retention during somatropin replacement therapy in adults may occur. Clinical manifestations of fluid retention are usually transient and dose dependent (see ADVERSE REACTIONS).
Experience with prolonged somatropin treatment in adults is limited.
Information for Patients
Patients being treated with Nutropin (and/or their parents) should be informed about the potential benefits and risks associated with Nutropin treatment, including a review of the contents of the Patient Information Insert. This information is intended to better educate patients (and caregivers); it is not a disclosure of all possible adverse or intended effects.
Patients and caregivers who will administer Nutropin should receive appropriate training and instruction on the proper use of Nutropin from the physician or other suitably qualified health care professional. A puncture-resistant container for the disposal of used syringes and needles should be strongly recommended. Patients and/or parents should be thoroughly instructed in the importance of proper disposal, and cautioned against any reuse of needles and syringes. This information is intended to aid in the safe and effective administration of the medication (see Patient Information Insert).
See WARNINGS for use of Bacteriostatic Water for Injection, USP, (benzyl alcohol preserved), in newborns.
Laboratory Tests
Serum levels of inorganic phosphorus, alkaline phosphatase, and parathyroid hormone (PTH) may increase during somatropin therapy.
Drug Interactions
Somatropin inhibits 11β‑hydroxysteroid dehydrogenase type 1 (11βHSD‑1) in adipose/hepatic tissue and may significantly impact the metabolism of cortisol and cortisone. As a consequence, in patients treated with somatropin, previously undiagnosed central (secondary) hypoadrenalism may be unmasked requiring glucocorticoid replacement therapy. In addition, patients treated with glucocorticoid replacement therapy for previously diagnosed hypoadrenalism may require an increase in their maintenance or stress doses; this may be especially true for patients treated with cortisone acetate and prednisone since conversion of these drugs to their biologically active metabolites is dependent on the activity of the 11βHSD‑1 enzyme.
Excessive glucocorticoid therapy may attenuate the growth-promoting effects of somatropin in children. Therefore, glucocorticoid replacement therapy should be carefully adjusted in children with concomitant GH and glucocorticoid deficiency to avoid both hypoadrenalism and an inhibitory effect on growth.
The use of Nutropin in patients with CRI requiring glucocorticoid therapy has not been evaluated. Concomitant glucocorticoid therapy may inhibit the growth promoting effect of Nutropin. Therefore, if glucocorticoid replacement is required for CRI, the glucocorticoid dose should be carefully adjusted to avoid an inhibitory effect on growth.
There was no evidence in the controlled studies of Nutropin’s interaction with drugs commonly used in chronic renal insufficiency patients. Limited published data indicate that somatropin treatment increases cytochrome P450 (CP450) mediated antipyrine clearance in man. These data suggest that somatropin administration may alter the clearance of compounds known to be metabolized by CP450 liver enzymes (e.g., corticosteroids, sex steroids, anticonvulsants, cyclosporin). Careful monitoring is advisable when somatropin is administered in combination with other drugs known to be metabolized by CP450 liver enzymes. However, formal drug interaction studies have not been conducted.
In adult women on oral estrogen replacement, a larger dose of somatropin may be required to achieve the defined treatment goal (see DOSAGE AND ADMINISTRATION).
In patients with diabetes mellitus requiring drug therapy, the dose of insulin and/or oral agent may require adjustment when somatropin therapy is initiated (see PRECAUTIONS, General).
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity, mutagenicity, and reproduction studies have not been conducted with Nutropin.
Pregnancy
Pregnancy (Category C). Animal reproduction studies have not been conducted with Nutropin. It is also not known whether Nutropin can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Nutropin should be given to a pregnant woman only if clearly needed.
Nursing Mothers
It is not known whether Nutropin is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when Nutropin is administered to a nursing mother.
Geriatric Usage
Clinical studies of Nutropin did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Elderly patients may be more sensitive to the action of somatropin, and therefore may be more prone to develop adverse reactions. A lower starting dose and smaller dose increments should be considered for older patients (see DOSING AND ADMINISTRATION).
Adverse Reactions/Side Effects
As with all protein pharmaceuticals, a small percentage of patients may develop antibodies to the protein. GH antibody binding capacities below 2 mg/L have not been associated with growth attenuation. In some cases when binding capacity exceeds 2 mg/L, growth attenuation has been observed. In clinical studies of pediatric patients that were treated with Nutropin for the first time, 0/107 growth hormone–deficient (GHD) patients, 0/125 CRI patients, 0/112 Turner syndrome, and 0/117 ISS patients screened for antibody production developed antibodies with binding capacities ≥ 2 mg/L at six months.
Additional short‑term immunologic and renal function studies were carried out in a group of patients with CRI after approximately one year of treatment to detect other potential adverse effects of antibodies to GH. Testing included measurements of C1q, C3, C4, rheumatoid factor, creatinine, creatinine clearance, and BUN. No adverse effects of GH antibodies were noted.
In addition to an evaluation of compliance with the prescribed treatment program and thyroid status, testing for antibodies to GH should be carried out in any patient who fails to respond to therapy.
In a post‑marketing surveillance study, the National Cooperative Growth Study, the pattern of adverse events in over 8000 patients with idiopathic short stature was consistent with the known safety profile of GH, and no new safety signals attributable to GH were identified. The frequency of protocol‑defined targeted adverse events is described in the table, below.
| Reported Events | NCGS (N=8018) |
|||
|---|---|---|---|---|
| AVN=avascular necrosis; SCFE=slipped capital femoral epiphysis. | ||||
| Data obtained with several rhGH products (Nutropin, Nutropin AQ, Nutropin Depot and Protropin). | ||||
| Any adverse event | ||||
| Overall | 103 (1.3%) | |||
| Targeted adverse event | ||||
| Overall | 103 (1.3%) | |||
| Injection-site reaction | 28 (0.3%) | |||
| New onset or progression of scoliosis | 16 (0.2%) | |||
| Gynecomastia | 12 (0.1%) | |||
| Any new onset or recurring tumor (benign) | 12 (0.1%) | |||
| Arthralgia or arthritis | 10 (0.1%) | |||
| Diabetes mellitus | 5 (0.1%) | |||
| Edema | 5 (0.1%) | |||
| Cancer, neoplasm (new onset or recurrence) | 4(0.0%) | |||
| Fracture | 4(0.0%) | |||
| Intracranial hypertension | 4(0.0%) | |||
| Abnormal bone or other growth | 3(0.0%) | |||
| Central nervous system tumor | 2(0.0%) | |||
| New or recurrent SCFE or AVN | 2(0.0%) | |||
| Carpal tunnel syndrome | 1(0.0%) | |||
In studies in patients treated with Nutropin, injection site pain was reported infrequently.
Leukemia has been reported in a small number of GHD patients treated with GH. It is uncertain whether this increased risk is related to the pathology of GH deficiency itself, GH therapy, or other associated treatments such as radiation therapy for intracranial tumors. On the basis of current evidence, experts cannot conclude that GH therapy is responsible for these occurrences. The risk to GHD, CRI, or Turner syndrome patients, if any, remains to be established.
Other adverse drug reactions that have been reported in GH‑treated patients include the following:
- 1)
- Metabolic: mild, transient peripheral edema. In GHD adults, edema or peripheral edema was reported in 41% of GH‑treated patients and 25% of placebo‑treated patients;
- 2)
- Musculoskeletal: arthralgias; carpal tunnel syndrome. In GHD adults, arthralgias and other joint disorders were reported in 27% of GH‑treated patients and 15% of placebo‑treated patients;
- 3)
- Skin: rare increased growth of pre‑existing nevi; patients should be monitored for malignant transformation; and
- 4)
- Endocrine: gynecomastia. Rare pancreatitis.
Overdosage
Acute overdosage could lead to hyperglycemia. Long‑term overdosage could result in signs and symptoms of gigantism and/or acromegaly consistent with the known effects of excess GH. (See recommended and maximal dosage instructions given below.)
Nutropin Dosage and Administration
The Nutropin® [somatropin (rDNA origin) for injection] dosage and administration schedule should be individualized for each patient. Response to growth hormone therapy in pediatric patients tends to decrease with time. However, in pediatric patients failure to increase growth rate, particularly during the first year of therapy, suggests the need for close assessment of compliance and evaluation of other causes of growth failure, such as hypothyroidism, under‑nutrition, and advanced bone age.
Dosage
Pediatric Growth Hormone Deficiency (GHD)
A weekly dosage of up to 0.3 mg/kg of body weight divided into daily subcutaneous injection is recommended. In pubertal patients, a weekly dosage of up to 0.7 mg/kg divided daily may be used.
Adult Growth Hormone Deficiency (GHD)
Based on the weight-based dosing utilized in the original pivotal studies described herein, the recommended dosage at the start of therapy is not more than 0.006 mg/kg given as a daily subcutaneous injection. The dose may be increased according to individual patient requirements to a maximum of 0.025 mg/kg daily in patients under 35 years old and to a maximum of 0.0125 mg/kg daily in patients over 35 years old. Clinical response, side effects, and determination of age- and gender-adjusted serum IGF-I levels may be used as guidance in dose titration.
Alternatively, taking into account more recent literature, a starting dose of approximately 0.2 mg/day (range, 0.15‑0.30 mg/day) may be used without consideration of body weight. This dose can be increased gradually every 1-2 months by increments of approximately 0.1-0.2 mg/day, according to individual patient requirements based on the clinical response and serum IGF-I concentrations. During therapy, the dose should be decreased if required by the occurrence of adverse events and/or serum IGF-I levels above the age- and gender-specific normal range. Maintenance dosages vary considerably from person to person.
A lower starting dose and smaller dose increments should be considered for older patients, who are more prone to the adverse effects of somatropin than younger individuals. In addition, obese individuals are more likely to manifest adverse effects when treated with a weight-based regimen. In order to reach the defined treatment goal, estrogen-replete women may need higher doses than men. Oral estrogen administration may increase the dose requirements in women.
Chronic Renal Insufficiency (CRI)
A weekly dosage of up to 0.35 mg/kg of body weight divided into daily subcutaneous injection is recommended.
Nutropin therapy may be continued up to the time of renal transplantation.
In order to optimize therapy for patients who require dialysis, the following guidelines for injection schedule are recommended:
- Hemodialysis patients should receive their injection at night just prior to going to sleep or at least 3–4 hours after their hemodialysis to prevent hematoma formation due to the heparin.
- Chronic Cycling Peritoneal Dialysis (CCPD) patients should receive their injection in the morning after they have completed dialysis.
- Chronic Ambulatory Peritoneal Dialysis (CAPD) patients should receive their injection in the evening at the time of the overnight exchange.
Administration
After the dose has been determined, reconstitute as follows: each 5 mg vial should be reconstituted with 1–5 mL of Bacteriostatic Water for Injection, USP (benzyl alcohol preserved); or each 10 mg vial should be reconstituted with 1–10 mL of Bacteriostatic Water for Injection, USP (benzyl alcohol preserved), only. For use in newborns, see WARNINGS. The pH of Nutropin after reconstitution with Bacteriostatic Water for Injection, USP (benzyl alcohol preserved), is approximately 7.4.
To prepare the Nutropin solution, inject the Bacteriostatic Water for Injection, USP (benzyl alcohol preserved) into the Nutropin vial, aiming the stream of liquid against the glass wall. Then swirl the product vial with a GENTLE rotary motion until the contents are completely dissolved. DO NOT SHAKE . Because Nutropin is a protein, shaking can result in a cloudy solution. The Nutropin solution should be clear immediately after reconstitution. Occasionally, after refrigeration, you may notice that small colorless particles of protein are present in the Nutropin solution. This is not unusual for solutions containing proteins. If the solution is cloudy immediately after reconstitution or refrigeration, the contents MUST NOT be injected.
Before needle insertion, wipe the septum of both the Nutropin and diluent vials with rubbing alcohol or an antiseptic solution to prevent contamination of the contents by microorganisms that may be introduced by repeated needle insertions. It is recommended that Nutropin be administered using sterile, disposable syringes and needles. The syringes should be of small enough volume that the prescribed dose can be drawn from the vial with reasonable accuracy.
STABILITY AND STORAGE
Before Reconstitution—Nutropin and Bacteriostatic Water for Injection, USP (benzyl alcohol preserved), must be stored at 2–8°C/36–46°F (under refrigeration). Avoid freezing the vials of Nutropin and Bacteriostatic Water for Injection, USP (benzyl alcohol preserved). Expiration dates are stated on the labels.
After Reconstitution—Vial contents are stable for 14 days when reconstituted with Bacteriostatic Water for Injection, USP (benzyl alcohol preserved), and stored at 2–8°C/36–46°F (under refrigeration). Avoid freezing the reconstituted vial of Nutropin and the Bacteriostatic Water for Injection, USP (benzyl alcohol preserved).
How is Nutropin supplied
Nutropin® [somatropin (rDNA origin) for injection] is supplied as 5 mg (approximately 15 IU) or 10 mg (approximately 30 IU) of lyophilized, sterile somatropin per vial.
Each 5 mg carton contains one vial of Nutropin® [somatropin (rDNA origin) for injection] (5 mg per vial) and one 10 mL multiple dose vial of Bacteriostatic Water for Injection, USP (benzyl alcohol preserved). NDC 50242‑072‑03.
Each 10 mg carton contains one vial of Nutropin® [somatropin (rDNA origin) for injection] (10 mg per vial) and one 10 mL multiple dose vial of Bacteriostatic Water for Injection, USP (benzyl alcohol preserved). NDC 50242‑018‑21.
|
Nutropin®
Bacteriostatic Water for Injection, USP |
7123911 |
Representative sample of labeling (see the HOW SUPPLIED section for complete listing):
| NUTROPIN
somatropin kit |
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
| NUTROPIN
somatropin kit |
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
|
|||||||||||||||
| Labeler - Genentech, Inc. (080129000) |
| Registrant - Genentech, Inc. (080129000) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Genentech, Inc. (SSF) | 080129000 | API MANUFACTURE, MANUFACTURE, ANALYSIS | |
More about Nutropin (somatropin)
- Check interactions
- Compare alternatives
- Reviews (4)
- Side effects
- Dosage information
- During pregnancy
- Drug class: growth hormones
- Breastfeeding
Patient resources
Professional resources
Other brands
Genotropin, Omnitrope, Norditropin, Humatrope, ... +3 more


