Mycobutin: Package Insert / Prescribing Info
Package insert / product label
Generic name: rifabutin
Dosage form: capsule
Drug class: Rifamycin derivatives
Medically reviewed by Drugs.com. Last updated on Jul 24, 2024.
On This Page
Mycobutin Description
MYCOBUTIN Capsules for oral administration contain 150 mg of the rifamycin antimycobacterial agent rifabutin, USP, per capsule, along with the inactive ingredients, microcrystalline cellulose, magnesium stearate, red iron oxide, silica gel, sodium lauryl sulfate, titanium dioxide, and edible white ink.
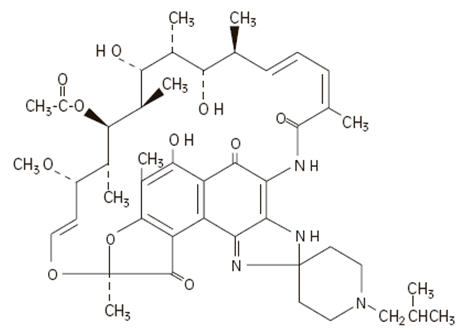
The chemical name for rifabutin is 1',4-didehydro-1-deoxy-1,4-dihydro-5'-(2-methylpropyl)-1-oxorifamycin XIV (Chemical Abstracts Service, 9th Collective Index) or (9S,12E,14S,15R, 16S,17R,18R,19R,20S,21S,22E, 24Z)-6,16,18,20-tetrahydroxy-1'-isobutyl-14-methoxy-7,9,15,17,19,21,25-heptamethyl-spiro [9,4-(epoxypentadeca[1,11,13]trienimino)-2H-furo[2',3':7,8]naphth[1,2-d] imidazole-2,4'-piperidine]-5,10,26-(3H,9H)-trione-16-acetate. Rifabutin has a molecular formula of C46H62N4O11, a molecular weight of 847.02 and the following structure:
Rifabutin is a red-violet powder soluble in chloroform and methanol, sparingly soluble in ethanol, and very slightly soluble in water (0.19 mg/mL). Its log P value (the base 10 logarithm of the partition coefficient between n-octanol and water) is 3.2 (n-octanol/water).
Mycobutin - Clinical Pharmacology
Pharmacokinetics
Absorption
Following a single oral dose of 300 mg to nine healthy adult volunteers, rifabutin was readily absorbed from the gastrointestinal tract with mean (±SD) peak plasma levels (Cmax) of 375 (±267) ng/mL (range: 141 to 1033 ng/mL) attained in 3.3 (±0.9) hours (Tmax range: 2 to 4 hours). Absolute bioavailability assessed in five HIV-positive patients, who received both oral and intravenous doses, averaged 20%. Total recovery of radioactivity in the urine indicates that at least 53% of the orally administered rifabutin dose is absorbed from the gastrointestinal tract. The bioavailability of rifabutin from the capsule dosage form, relative to an oral solution, was 85% in 12 healthy adult volunteers. High-fat meals slow the rate without influencing the extent of absorption from the capsule dosage form. Plasma concentrations post-Cmax declined in an apparent biphasic manner. Pharmacokinetic dose-proportionality was established over the 300 mg to 600 mg dose range in nine healthy adult volunteers (crossover design) and in 16 early symptomatic human immunodeficiency virus (HIV)-positive patients over a 300 mg to 900 mg dose range.
Distribution
Due to its high lipophilicity, rifabutin demonstrates a high propensity for distribution and intracellular tissue uptake. Following intravenous dosing, estimates of apparent steady-state distribution volume (9.3 ± 1.5 L/kg) in five HIV-positive patients exceeded total body water by approximately 15-fold. Substantially higher intracellular tissue levels than those seen in plasma have been observed in both rat and man. The lung-to-plasma concentration ratio, obtained at 12 hours, was approximately 6.5 in four surgical patients who received an oral dose. Mean rifabutin steady-state trough levels (Cp,minss; 24-hour post-dose) ranged from 50 to 65 ng/mL in HIV-positive patients and in healthy adult volunteers. About 85% of the drug is bound in a concentration-independent manner to plasma proteins over a concentration range of 0.05 to 1 µg/mL. Binding does not appear to be influenced by renal or hepatic dysfunction. Rifabutin was slowly eliminated from plasma in seven healthy adult volunteers, presumably because of distribution-limited elimination, with a mean terminal half-life of 45 (±17) hours (range: 16 to 69 hours). Although the systemic levels of rifabutin following multiple dosing decreased by 38%, its terminal half-life remained unchanged.
Metabolism
Of the five metabolites that have been identified, 25-O-desacetyl and 31-hydroxy are the most predominant, and show a plasma metabolite:parent area under the curve ratio of 0.10 and 0.07, respectively. The former has an activity equal to the parent drug and contributes up to 10% to the total antimicrobial activity.
Excretion
A mass-balance study in three healthy adult volunteers with 14C-labeled rifabutin showed that 53% of the oral dose was excreted in the urine, primarily as metabolites. About 30% of the dose is excreted in the feces. Mean systemic clearance (CLs/F) in healthy adult volunteers following a single oral dose was 0.69 (±0.32) L/hr/kg (range: 0.46 to 1.34 L/hr/kg). Renal and biliary clearance of unchanged drug each contribute approximately 5% to CLs/F.
Pharmacokinetics in Special Populations
Geriatric
Compared to healthy volunteers, steady-state kinetics of MYCOBUTIN are more variable in elderly patients (>70 years).
Pediatric
The pharmacokinetics of MYCOBUTIN have not been studied in subjects under 18 years of age.
Renal Impairment
The disposition of rifabutin (300 mg) was studied in 18 patients with varying degrees of renal function. Area under plasma concentration time curve (AUC) increased by about 71% in patients with severe renal impairment (creatinine clearance below 30 mL/min) compared to patients with creatinine clearance (Crcl) between 61–74 mL/min. In patients with mild to moderate renal impairment (Crcl between 30–61 mL/min), the AUC increased by about 41%. In patients with severe renal impairment, carefully monitor for rifabutin associated adverse events. A reduction in the dosage of rifabutin is recommended for patients with Crcl <30 mL/min if toxicity is suspected (see DOSAGE AND ADMINISTRATION).
Hepatic Impairment
Mild hepatic impairment does not require a dose modification. The pharmacokinetics of rifabutin in patients with moderate and severe hepatic impairment is not known.
Malabsorption in HIV-Infected Patients
Alterations in gastric pH due to progressing HIV disease has been linked with malabsorption of some drugs used in HIV-positive patients (e.g., rifampin, isoniazid). Drug serum concentrations data from AIDS patients with varying disease severity (based on CD4+ counts) suggests that rifabutin absorption is not influenced by progressing HIV disease.
Drug-Drug Interactions
(see also PRECAUTIONS-Drug Interactions)
Multiple dosing of rifabutin has been associated with induction of hepatic metabolic enzymes of the CYP3A subfamily. Rifabutin's predominant metabolite (25-desacetyl rifabutin: LM565), may also contribute to this effect. Metabolic induction due to rifabutin is likely to produce a decrease in plasma concentrations of concomitantly administered drugs that are primarily metabolized by the CYP3A enzymes. Similarly concomitant medications that competitively inhibit the CYP3A activity may increase plasma concentrations of rifabutin.
Clinical Studies
Two randomized, double-blind clinical trials (Study 023 and Study 027) compared MYCOBUTIN (300 mg/day) to placebo in patients with CDC-defined AIDS and CD4 counts ≤200 cells/µL. These studies accrued patients from 2/90 through 2/92. Study 023 enrolled 590 patients, with a median CD4 cell count at study entry of 42 cells/µL (mean 61). Study 027 enrolled 556 patients with a median CD4 cell count at study entry of 40 cells/µL (mean 58).
Endpoints included the following:
- •
- MAC bacteremia, defined as at least one blood culture positive for Mycobacterium avium complex (MAC) bacteria.
- •
- Clinically significant disseminated MAC disease, defined as MAC bacteremia accompanied by signs or symptoms of serious MAC infection, including one or more of the following: fever, night sweats, rigors, weight loss, worsening anemia, and/or elevations in alkaline phosphatase.
- •
- Survival.
MAC Bacteremia
Participants who received MYCOBUTIN were one-third to one-half as likely to develop MAC bacteremia as were participants who received placebo. These results were statistically significant (Study 023: p<0.001; Study 027: p = 0.002).
In Study 023, the one-year cumulative incidence of MAC bacteremia, on an intent to treat basis, was 9% for patients randomized to MYCOBUTIN and 22% for patients randomized to placebo. In Study 027, these rates were 13% and 28% for patients receiving MYCOBUTIN and placebo, respectively.
Most cases of MAC bacteremia (approximately 90% in these studies) occurred among participants whose CD4 count at study entry was ≤100 cells/µL. The median and mean CD4 counts at onset of MAC bacteremia were 13 cells/µL and 24 cells/µL, respectively. These studies did not investigate the optimal time to begin MAC prophylaxis.
Clinically Significant Disseminated MAC Disease
In association with the decreased incidence of bacteremia, patients on MYCOBUTIN showed reductions in the signs and symptoms of disseminated MAC disease, including fever, night sweats, weight loss, fatigue, abdominal pain, anemia, and hepatic dysfunction.
Microbiology
Mechanism of Action
Rifabutin inhibits DNA-dependent RNA polymerase in susceptible strains of Escherichia coli and Bacillus subtilis but not in mammalian cells. In resistant strains of E. coli, rifabutin, like rifampin, did not inhibit this enzyme. It is not known whether rifabutin inhibits DNA-dependent RNA polymerase in Mycobacterium avium or in M. intracellulare which comprise M. avium complex (MAC).
Susceptibility Testing
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC.
In Vitro Studies
Rifabutin has demonstrated in vitro activity against M. avium complex (MAC) organisms isolated from both HIV-positive and HIV-negative people. While-gene probe techniques may be used to identify these two organisms, many reported studies did not distinguish between these two species. The vast majority of isolates from MAC-infected, HIV-positive people are M. avium, whereas in HIV-negative people, about 40% of the MAC isolates are M. intracellulare.
Various in vitro methodologies employing broth or solid media, with and without polysorbate 80 (Tween 80), have been used to determine rifabutin MIC values for mycobacterial species. In general, MIC values determined in broth are several fold lower than that observed with methods employing solid media. Utilization of Tween 80 in these assays has been shown to further lower MIC values.
However, MIC values were substantially higher for egg-based compared to agar-based solid media.
Rifabutin activity against 211 MAC isolates from HIV-positive people was evaluated in vitro utilizing a radiometric broth and an agar dilution method. Results showed that 78% and 82% of these isolates had MIC99 values of ≤0.25 µg/mL and ≤1.0 µg/mL, respectively, when evaluated by these two methods. Rifabutin was also shown to be active against phagocytized, M. avium complex in a mouse macrophage cell culture model.
Rifabutin has in vitro activity against many strains of Mycobacterium tuberculosis. In one study, utilizing the radiometric broth method, each of 17 and 20 rifampin-naive clinical isolates tested from the United States and Taiwan, respectively, were shown to be susceptible to rifabutin concentrations of ≤0.125 µg/mL.
Cross-resistance between rifampin and rifabutin is commonly observed with M. tuberculosis and M. avium complex isolates. Isolates of M. tuberculosis resistant to rifampin are likely to be resistant to rifabutin. Rifampicin and rifabutin MIC99 values against 523 isolates of M. avium complex were determined utilizing the agar dilution method (Heifets, Leonid B. and Iseman, Michael D. Determination of in vitro susceptibility of Mycobacteria to Ansamycin. Am. Rev. Respir. Dis. 1985; 132(3):710–711).
| % of Strains Susceptible/Resistant to Different Concentrations of Rifabutin (μg/mL) | |||||
|---|---|---|---|---|---|
| Susceptibility to Rifampin
(µg/mL) | Number of Strains | Susceptible to 0.5 | Resistant to 0.5 only | Resistant to 1.0 | Resistant to 2.0 |
|
Susceptible to 1.0 |
30 |
100.0 |
0.0 |
0.0 |
0.0 |
|
Resistant to 1.0 only |
163 |
88.3 |
11.7 |
0.0 |
0.0 |
|
Resistant to 5.0 |
105 |
38.0 |
57.1 |
2.9 |
2.0 |
|
Resistant to 10.0 |
225 |
20.0 |
50.2 |
19.6 |
10.2 |
|
TOTAL |
523 |
49.5 |
36.7 |
9.0 |
4.8 |
Rifabutin in vitro MIC99 values of ≤0.5 µg/mL, determined by the agar dilution method, for M. kansasii, M. gordonae and M. marinum have been reported; however, the clinical significance of these results is unknown.
Indications and Usage for Mycobutin
MYCOBUTIN Capsules are indicated for the prevention of disseminated Mycobacterium avium complex (MAC) disease in patients with advanced HIV infection.
Contraindications
MYCOBUTIN Capsules are contraindicated in patients who have had clinically significant hypersensitivity to rifabutin or to any other rifamycins.
Warnings
Tuberculosis
MYCOBUTIN Capsules must not be administered for MAC prophylaxis to patients with active tuberculosis. Patients who develop complaints consistent with active tuberculosis while on prophylaxis with MYCOBUTIN should be evaluated immediately, so that those with active disease may be given an effective combination regimen of anti-tuberculosis medications. Administration of MYCOBUTIN as a single agent to patients with active tuberculosis is likely to lead to the development of tuberculosis that is resistant both to MYCOBUTIN and to rifampin.
There is no evidence that MYCOBUTIN is an effective prophylaxis against M. tuberculosis. Patients requiring prophylaxis against both M. tuberculosis and Mycobacterium avium complex may be given isoniazid and MYCOBUTIN concurrently.
Tuberculosis in HIV-positive patients is common and may present with atypical or extrapulmonary findings. Patients are likely to have a nonreactive purified protein derivative (PPD) despite active disease. In addition to chest X-ray and sputum culture, the following studies may be useful in the diagnosis of tuberculosis in the HIV-positive patient: blood culture, urine culture, or biopsy of a suspicious lymph node.
MAC Treatment with Clarithromycin
When MYCOBUTIN is used concomitantly with clarithromycin for MAC treatment, a decreased dose of MYCOBUTIN is recommended due to the increase in plasma concentrations of MYCOBUTIN (see PRECAUTIONS-Drug Interactions, Table 2).
Hypersensitivity and Related Reactions
Hypersensitivity reactions may occur in patients receiving rifamycins. Signs and symptoms of these reactions may include hypotension, urticaria, angioedema, acute bronchospasm, conjunctivitis, thrombocytopenia, neutropenia or flu-like syndrome (weakness, fatigue, muscle pain, nausea, vomiting, headache, fever, chills, aches, rash, itching, sweats, dizziness, shortness of breath, chest pain, cough, syncope, palpitations). There have been reports of anaphylaxis with the use of rifamycins.
Monitor patients receiving MYCOBUTIN therapy for signs and/or symptoms of hypersensitivity reactions. If these symptoms occur, administer supportive measures and discontinue MYCOBUTIN.
Uveitis
Due to the possible occurrence of uveitis, patients should also be carefully monitored when MYCOBUTIN is given in combination with clarithromycin (or other macrolides) and/or fluconazole and related compounds (see PRECAUTIONS-Drug Interactions, Table 2). If uveitis is suspected, the patient should be referred to an ophthalmologist and, if considered necessary, treatment with MYCOBUTIN should be suspended (see also ADVERSE REACTIONS).
Clostridioides difficile Associated Diarrhea
Clostridioides difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including MYCOBUTIN (rifabutin) Capsules, USP, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibacterial use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibacterial use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibacterial treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
Severe Cutaneous Adverse Reactions
There have been reports of severe cutaneous adverse reactions (SCAR), such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalized exanthematous pustulosis (AGEP) associated with MYCOBUTIN (see ADVERSE REACTIONS).
If patients develop a skin rash they should be monitored closely, and MYCOBUTIN discontinued if lesions progress. Specifically, for DRESS, a multi-system potential life-threatening SCAR, time to onset of the first symptoms may be prolonged. DRESS is a clinical diagnosis, and its clinical presentation remains the basis for decision making. An early withdrawal of MYCOBUTIN is essential because of the syndrome's mortality and visceral involvement (e.g., liver, bone marrow or kidney).
Antiretroviral Drug Interactions
Protease inhibitors act as substrates or inhibitors of CYP3A4 mediated metabolism. Therefore, due to significant drug-drug interactions between protease inhibitors and rifabutin, their concomitant use should be based on the overall assessment of the patient and a patient-specific drug profile. The concomitant use of protease inhibitors may require at least a 50% reduction in rifabutin dose, and depending on the protease inhibitor, an adjustment of the antiretroviral drug dose. Increased monitoring for adverse events is recommended when using these drug combinations (see PRECAUTIONS-Drug Interactions).
MYCOBUTIN is a CYP3A inducer. Co-administration with antiretroviral drugs metabolized by CYP3A, including but not limited to products containing bictegravir, rilpivirine, or doravirine may decrease plasma concentrations of those antiretroviral drugs, which may lead to loss of virologic response and possible development of resistance. Therefore, co-administration with antiretroviral drugs metabolized by CYP3A is not recommended or there may be a need to increase the dose of antiretroviral drugs (see PRECAUTIONS-Drug Interactions).
For further recommendations, please refer to the most recent prescribing information of the antiretrovirals or contact the specific manufacturer.
Precautions
General
Because treatment with MYCOBUTIN Capsules may be associated with neutropenia, and more rarely thrombocytopenia, physicians should consider obtaining hematologic studies periodically in patients receiving prophylaxis with MYCOBUTIN.
Information for Patients
Patients should be advised of the signs and symptoms of both MAC and tuberculosis, and should be instructed to consult their physicians if they develop new complaints consistent with either of these diseases. In addition, since MYCOBUTIN may rarely be associated with myositis and uveitis, patients should be advised to notify their physicians if they develop signs or symptoms suggesting either of these disorders.
Urine, feces, saliva, sputum, perspiration, tears, and skin may be colored brown-orange with rifabutin and some of its metabolites. Soft contact lenses may be permanently stained. Patients to be treated with MYCOBUTIN should be made aware of these possibilities.
Diarrhea is a common problem caused by antibacterials which usually ends when the antibacterial is discontinued. Sometimes, after starting treatment with antibacterials, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibacterial. If this occurs, patients should contact their physician as soon as possible.
Drug Interactions
Effect of Rifabutin on the Pharmacokinetics of Other Drugs
Rifabutin induces CYP3A enzymes and therefore may reduce the plasma concentrations of drugs metabolized by those enzymes. This effect may reduce the efficacy of standard doses of such drugs, which include itraconazole, clarithromycin, and saquinavir.
Effect of Other Drugs on Rifabutin Pharmacokinetics
Some drugs that inhibit CYP3A may significantly increase the plasma concentration of rifabutin. Therefore, carefully monitor for rifabutin associated adverse events in those patients also receiving CYP3A inhibitors, which include fluconazole and clarithromycin. In some cases, the dosage of MYCOBUTIN may need to be reduced when it is coadministered with CYP3A inhibitors.
Table 2 summarizes the results and magnitude of the pertinent drug interactions assessed with rifabutin. The clinical relevance of these interactions and subsequent dose modifications should be judged in light of the population studied, severity of the disease, patient's drug profile, and the likely impact on the risk/benefit ratio.
| Coadministered drug | Dosing regimen of coadministered drug | Dosing regimen of rifabutin | Study population (n) | Effect on rifabutin | Effect on coadministered drug | Recommendation |
|---|---|---|---|---|---|---|
| ↑ indicates increase; ↓ indicates decrease; ↔ indicates no significant change ND - No Data AUC - Area under the Concentration vs. Time Curve; Cmax - Maximum serum concentration; Cmin – Minimum serum concentration |
||||||
|
||||||
|
ANTIRETROVIRALS |
||||||
|
Amprenavir |
1200 mg twice a day for 10 days |
300 mg once a day for 10 days |
Healthy male subjects (6) |
↑ AUC by 193%, |
↔ |
Reduce rifabutin dose by at least 50%. Monitor closely for adverse reactions. |
|
Bictegravir |
75 mg once a day |
300 mg once a day (fasted) |
Healthy subjects |
ND |
↓ AUC 38% |
Co-administration of rifabutin with Biktarvy (bictegravir/emtricitabine/tenofovir alafenamide) is not recommended due to an expected decrease in tenofovir alafenamide in addition to the reported reduction in bictegravir. Refer to Biktarvy prescribing information for additional information |
|
Delavirdine |
400 mg three times a day |
300 mg once a day |
HIV-infected patients (7) |
↑ AUC by 230%, |
↓ AUC by 80%, |
CONTRAINDICATED |
|
Didanosine |
167 or 250 mg twice a day for 12 days |
300 or 600 mg once a day for 12 days |
HIV-infected patients (11) |
↔ |
↔ | |
|
Doravirine |
100 mg single dose |
300 mg once a day for 16 days |
Healthy subjects (12) |
ND |
↓ 50% in AUC, |
If concomitant use is necessary, increase the doravirine dosage as instructed in doravirine-containing product prescribing information. |
|
Fosamprenavir/ ritonavir |
700 mg twice a day plus ritonavir 100 mg twice a day for 2 weeks |
150 mg every other day for 2 weeks |
Healthy subjects (15) |
↔ AUC*
|
↑ AUC by 35%†, |
Reduce rifabutin dose by at least 75% (to a maximum 150 mg every other day or three times per week) when given with fosamprenavir/ritonavir combination. |
|
Indinavir |
800 mg three times a day for 10 days |
300 mg once a day for 10 days |
Healthy subjects (10) |
↑ AUC by 173%, |
↓ AUC by 34%, |
Reduce rifabutin dose by 50%, and increase indinavir dose from 800 mg to 1000 mg three times a day. |
|
Lopinavir/ ritonavir |
400/100 mg twice a day for 20 days |
150 mg once a day for 10 days |
Healthy subjects (14) |
↑ AUC by 203% ‡
|
↔ |
Reduce rifabutin dose by at least 75% (to a maximum 150 mg every other day or three times per week) when given with lopinavir/ritonavir combination. Monitor closely for adverse reactions. Reduce rifabutin dosage further, as needed. |
|
Saquinavir/ ritonavir |
1000/100 mg twice a day for 14 or 22 days |
150 mg every 3 days for 21–22 days |
Healthy subjects |
↑ AUC by 53% §
|
↓ AUC by 13%, |
Reduce rifabutin dose by at least 75% (to a maximum 150 mg every other day or three times per week) when given with saquinavir/ritonavir combination. Monitor closely for adverse reactions. |
|
Rilpivirine |
25 mg once a day |
300 mg once a day |
Healthy subjects (18) |
ND |
↓ AUC by 42% |
Co-administration of rifabutin with Odefsey (rilpivirine/tenofovir alafenamide/emtricitabine) is not recommended, due to an expected decrease in tenofovir alafenamide in addition to the reported reduction in rilpivirine. Refer to Odefsey prescribing information for additional information. |
|
Ritonavir |
500 mg twice a day for 10 days |
150 mg once a day for 16 days |
Healthy subjects (5) |
↑ AUC by 300%, |
ND |
Reduce rifabutin dose by at least 75% (to a maximum 150 mg every other day or three times per week) when given with lopinavir/ritonavir combination. Monitor closely for adverse reactions. |
|
Tipranavir/ ritonavir |
500/200 twice a day for 15 doses |
150 mg single dose |
Healthy subjects (20) |
↑ AUC by 190%, |
↔ |
Reduce rifabutin dose by at least 75% (to a maximum 150 mg every other day or three times per week) when given with tipranavir/ritonavir combination. Monitor closely for adverse reactions. Reduce rifabutin dosage further, as needed. |
|
Nelfinavir |
1250 mg twice a day for 7–8 days |
150 mg once a day for 8 days |
HIV-infected patients (11) |
↑ AUC by 83%, ¶
|
↔ |
Reduce rifabutin dose by 50% (to 150 mg once a day) and increase the nelfinavir dose to 1250 mg twice a day. |
|
Zidovudine |
100 or 200 mg every four hours |
300 or 450 mg once a day |
HIV-infected patients (16) |
↔ |
↓ AUC by 32%, |
Because zidovudine levels remained within the therapeutic range during co-administration of rifabutin, dosage adjustments are not necessary. |
|
ANTIFUNGALS |
||||||
|
Fluconazole |
200 mg once a day for 2 weeks |
300 mg once a day for 2 weeks |
HIV-infected patients (12) |
↑ AUC by 82%, |
↔ |
Monitor for rifabutin associated adverse events. Reduce rifabutin dose or suspend MYCOBUTIN use if toxicity is suspected. |
|
Posaconazole |
200 mg once a day for 10 days |
300 mg once a day for 17 days |
Healthy subjects (8) |
↑ AUC by 72%, |
↓ AUC by 49%, |
If co-administration of these two drugs cannot be avoided, patients should be monitored for adverse events associated with rifabutin administration, and lack of posaconazole efficacy. |
|
Itraconazole |
200 mg once a day |
300 mg once a day |
HIV-Infected patients (6) |
↑# |
↓ AUC by 70%, |
If co-administration of these two drugs cannot be avoided, patients should be monitored for adverse events associated with rifabutin administration, and lack of itraconazole efficacy. In a separate study, one case of uveitis was associated with increased serum rifabutin levels following co-administration of rifabutin (300 mg once a day) with itraconazole (600–900 mg once a day). |
|
Voriconazole |
400 mg twice a day for 7 days (maintenance dose) |
300 mg once a day for 7 days |
Healthy male subjects (12) |
↑ AUC by 331%, |
↑ AUC by ~100%, |
CONTRAINDICATED |
|
ANTI-PCP (Pneumocystis carinii pneumonia) |
||||||
|
Dapsone |
50 mg once a day |
300 mg once a day |
HIV-infected patients (16) |
ND |
↓ AUC by 27 –40% | |
|
Sulfamethoxazole- Trimethoprim |
800/160 mg |
300 mg once a day |
HIV-infected patients (12) |
↔ |
↓ AUC by 15–20% | |
|
ANTI-MAC (Mycobacterium avium intracellulare complex) |
||||||
|
Azithromycin |
500 mg once a day for 1 day, then 250 mg once a day for 9 days |
300 mg once a day |
Healthy subjects (6) |
↔ |
↔ | |
|
Clarithromycin |
500 mg twice a day |
300 mg once a day |
HIV-infected patients (12) |
↑ AUC by 75% |
↓ AUC by 50% |
Monitor for rifabutin associated adverse events. Reduce dose or suspend use of MYCOBUTIN if toxicity is suspected. Alternative treatment for clarithromycin should be considered when treating patients receiving rifabutin |
|
ANTI-TB (Tuberculosis) |
||||||
|
Ethambutol |
1200 mg |
300 mg once a day for 7 days |
Healthy subjects (10) |
ND |
↔ | |
|
Isoniazid |
300 mg |
300 mg once a day for 7 days |
Healthy subjects (6) |
ND |
↔ | |
|
OTHER |
||||||
|
Methadone |
20 – 100 mg once a day |
300 mg once a day for 13 days |
HIV-infected patients (24) |
ND |
↔ | |
|
Ethinylestradiol (EE)/Norethindrone (NE) |
35 mg EE / 1 mg NE for 21 days |
300 mg once a day for 10 days |
Healthy female subjects (22) |
ND |
EE: ↓ AUC by |
Patients should be advised to use additional or alternative methods of contraception. |
|
Theophylline |
5 mg/kg |
300 mg for 14 days |
Healthy subjects (11) |
ND |
↔ | |
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies were conducted with rifabutin in mice and in rats. Rifabutin was not carcinogenic in mice at doses up to 180 mg/kg/day, or approximately 36 times the recommended human daily dose. Rifabutin was not carcinogenic in the rat at doses up to 60 mg/kg/day, about 12 times the recommended human dose.
Rifabutin was not mutagenic in the bacterial mutation assay (Ames Test) using both rifabutin-susceptible and resistant strains. Rifabutin was not mutagenic in Schizosaccharomyces pombe P1 and was not genotoxic in V-79 Chinese hamster cells, human lymphocytes in vitro, or mouse bone marrow cells in vivo.
Fertility was impaired in male rats given 160 mg/kg (32 times the recommended human daily dose).
Pregnancy
Rifabutin should be used in pregnant women only if the potential benefit justifies the potential risk to the fetus. There are no adequate and well-controlled studies in pregnant or breastfeeding women.
Reproduction studies have been carried out in rats and rabbits given rifabutin using dose levels up to 200 mg/kg (about 6 to 13 times the recommended human daily dose based on body surface area comparisons). No teratogenicity was observed in either species. In rats, given 200 mg/kg/day, (about 6 times the recommended human daily dose based on body surface area comparisons), there was a decrease in fetal viability. In rats, at 40 mg/kg/day (approximately equivalent to the recommended human daily dose based on body surface area comparisons), rifabutin caused an increase in fetal skeletal variants. In rabbits, at 80 mg/kg/day (about 5 times the recommended human daily dose based on body surface area comparisons), rifabutin caused maternotoxicity and increase in fetal skeletal anomalies. Because animal reproduction studies are not always predictive of human response, rifabutin should be used in pregnant women only if the potential benefit justifies the potential risk to the fetus.
Nursing Mothers
It is not known whether rifabutin is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants, a decision should be made whether to discontinue nursing or discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness of rifabutin for prophylaxis of MAC in children have not been established. Limited safety data are available from treatment use in 22 HIV-positive children with MAC who received MYCOBUTIN in combination with at least two other antimycobacterials for periods from 1 to 183 weeks. Mean doses (mg/kg) for these children were: 18.5 (range 15.0 to 25.0) for infants 1 year of age, 8.6 (range 4.4 to 18.8) for children 2 to 10 years of age, and 4.0 (range 2.8 to 5.4) for adolescents 14 to 16 years of age. There is no evidence that doses greater than 5 mg/kg daily are useful. Adverse experiences were similar to those observed in the adult population, and included leukopenia, neutropenia, and rash. In addition, corneal deposits have been observed in some patients during routine ophthalmologic surveillance of HIV-positive pediatric patients receiving MYCOBUTIN as part of a multiple-drug regimen for MAC prophylaxis. These are tiny, almost transparent, asymptomatic peripheral and central corneal deposits which do not impair vision. Doses of MYCOBUTIN may be administered mixed with foods such as applesauce.
Geriatric Use
Clinical studies of MYCOBUTIN did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy (see CLINICAL PHARMACOLOGY).
Adverse Reactions/Side Effects
Adverse Reactions from Clinical Trials
MYCOBUTIN Capsules were generally well tolerated in the controlled clinical trials. Discontinuation of therapy due to an adverse event was required in 16% of patients receiving MYCOBUTIN, compared to 8% of patients receiving placebo in these trials. Primary reasons for discontinuation of MYCOBUTIN were rash (4% of treated patients), gastrointestinal intolerance (3%), and neutropenia (2%).
The following table enumerates adverse experiences that occurred at a frequency of 1% or greater, among the patients treated with MYCOBUTIN in studies 023 and 027.
| Adverse event | MYCOBUTIN
(n = 566) % | Placebo
(n = 580) % |
|---|---|---|
|
Body as a whole | ||
|
Abdominal pain |
4 |
3 |
|
Asthenia |
1 |
1 |
|
Chest pain |
1 |
1 |
|
Fever |
2 |
1 |
|
Headache |
3 |
5 |
|
Pain |
1 |
2 |
|
Blood and lymphatic system | ||
|
Leucopenia |
10 |
7 |
|
Anemia |
1 |
2 |
|
Digestive System | ||
|
Anorexia |
2 |
2 |
|
Diarrhea |
3 |
3 |
|
Dyspepsia |
3 |
1 |
|
Eructation |
3 |
1 |
|
Flatulence |
2 |
1 |
|
Nausea |
6 |
5 |
|
Nausea and vomiting |
3 |
2 |
|
Vomiting |
1 |
1 |
|
Musculoskeletal system | ||
|
Myalgia |
2 |
1 |
|
Nervous system | ||
|
Insomnia |
1 |
1 |
|
Skin and appendages | ||
|
Rash |
11 |
8 |
|
Special senses | ||
|
Taste perversion |
3 |
1 |
|
Urogenital system | ||
|
Discolored urine |
30 |
6 |
CLINICAL ADVERSE EVENTS REPORTED IN <1% OF PATIENTS WHO RECEIVED MYCOBUTIN
Considering data from the 023 and 027 pivotal trials, and from other clinical studies, MYCOBUTIN appears to be a likely cause of the following adverse events which occurred in less than 1% of treated patients: flu-like syndrome, hepatitis, hemolysis, arthralgia, myositis, chest pressure or pain with dyspnea, skin discoloration, thrombocytopenia, pancytopenia and jaundice.
The following adverse events have occurred in more than one patient receiving MYCOBUTIN, but an etiologic role has not been established: seizure, paresthesia, aphasia, confusion, and non-specific T wave changes on electrocardiogram.
When MYCOBUTIN was administered at doses from 1050 mg/day to 2400 mg/day, generalized arthralgia and uveitis were reported. These adverse experiences abated when MYCOBUTIN was discontinued.
Mild to severe, reversible uveitis has been reported less frequently when MYCOBUTIN is used at 300 mg as monotherapy in MAC prophylaxis versus MYCOBUTIN in combination with clarithromycin for MAC treatment (see also WARNINGS).
Uveitis has been infrequently reported when MYCOBUTIN is used at 300 mg/day as monotherapy in MAC prophylaxis of HIV-infected persons, even with the concomitant use of fluconazole and/or macrolide antibacterials. However, if higher doses of MYCOBUTIN are administered in combination with these agents, the incidence of uveitis is higher.
Patients who developed uveitis had mild to severe symptoms that resolved after treatment with corticosteroids and/or mydriatic eye drops; in some severe cases, however, resolution of symptoms occurred after several weeks.
When uveitis occurs, temporary discontinuance of MYCOBUTIN and ophthalmologic evaluation are recommended. In most mild cases, MYCOBUTIN may be restarted; however, if signs or symptoms recur, use of MYCOBUTIN should be discontinued (Morbidity and Mortality Weekly Report, September 9, 1994).
Corneal deposits have been reported during routine ophthalmologic surveillance of some HIV-positive pediatric patients receiving MYCOBUTIN as part of a multiple drug regimen for MAC prophylaxis. The deposits are tiny, almost transparent, asymptomatic peripheral and central corneal deposits, and do not impair vision.
The following table enumerates the changes in laboratory values that were considered as laboratory abnormalities in Studies 023 and 027.
| Laboratory abnormalities | MYCOBUTIN
(n = 566) % | PLACEBO
(n = 580) % |
|---|---|---|
| Includes grades 3 or 4 toxicities as specified: | ||
|
Chemistry | ||
|
Increased alkaline phosphatase * |
<1 |
3 |
|
Increased SGOT † |
7 |
12 |
|
Increased SGPT † |
9 |
11 |
|
Hematology | ||
|
Anemia ‡ |
6 |
7 |
|
Eosinophilia |
1 |
1 |
|
Leukopenia § |
17 |
16 |
|
Neutropenia ¶ |
25 |
20 |
|
Thrombocytopenia # |
5 |
4 |
The incidence of neutropenia in patients treated with MYCOBUTIN was significantly greater than in patients treated with placebo (p = 0.03). Although thrombocytopenia was not significantly more common among patients treated with MYCOBUTIN in these trials, MYCOBUTIN has been clearly linked to thrombocytopenia in rare cases. One patient in Study 023 developed thrombotic thrombocytopenic purpura, which was attributed to MYCOBUTIN.
Adverse Reactions from Post-Marketing Experience
Adverse reactions identified through post-marketing surveillance by system organ class (SOC) are listed below:
Blood and lymphatic system disorders: White blood cell disorders (including agranulocytosis, lymphopenia, granulocytopenia, neutropenia, white blood cell count decreased, neutrophil count decreased), platelet count decreased.
Immune system disorders: Hypersensitivity, bronchospasm, rash, and eosinophilia.
Gastrointestinal disorders: Clostridioides difficile colitis/Clostridioides difficile associated diarrhea.
Pyrexia, rash and other hypersensitivity reactions such as eosinophilia and bronchospasm might occur, as has been seen with other antibacterials.
A limited occurrence of skin discoloration has been reported.
ANIMAL TOXICOLOGY
Liver abnormalities (increased bilirubin and liver weight) occurred in mice, rats and monkeys at doses (respectively) 0.5, 1, and 3 times the recommended human daily dose based on body surface area comparisons. Testicular atrophy occurred in baboons at doses 2 times the recommended human dose based on body surface area comparisons, and in rats at doses 6 times the recommended human daily dose based on body surface area comparisons.
Overdosage
No information is available on accidental overdosage in humans.
Treatment
While there is no experience in the treatment of overdose with MYCOBUTIN Capsules, clinical experience with rifamycins suggests that gastric lavage to evacuate gastric contents (within a few hours of overdose), followed by instillation of an activated charcoal slurry into the stomach, may help absorb any remaining drug from the gastrointestinal tract.
Rifabutin is 85% protein bound and distributed extensively into tissues (Vss:8 to 9 L/kg). It is not primarily excreted via the urinary route (less than 10% as unchanged drug); therefore, neither hemodialysis nor forced diuresis is expected to enhance the systemic elimination of unchanged rifabutin from the body in a patient with an overdose of MYCOBUTIN.
Mycobutin Dosage and Administration
It is recommended that MYCOBUTIN Capsules be administered at a dose of 300 mg once daily. For those patients with propensity to nausea, vomiting, or other gastrointestinal upset, administration of MYCOBUTIN at doses of 150 mg twice daily taken with food may be useful.
For patients with severe renal impairment (creatinine clearance less than 30 mL/min), consider reducing the dose of MYCOBUTIN by 50%, if toxicity is suspected. No dosage adjustment is required for patients with mild to moderate renal impairment. Reduction of the dose of MYCOBUTIN may also be needed for patients receiving concomitant treatment with certain other drugs (see PRECAUTIONS-Drug Interactions).
Mild hepatic impairment does not require a dose modification. The pharmacokinetics of rifabutin in patients with moderate and severe hepatic impairment is not known.
How is Mycobutin supplied
MYCOBUTIN (rifabutin) Capsules, USP are supplied as hard gelatin capsules having an opaque red-brown cap and body, imprinted with MYCOBUTIN/PHARMACIA & UPJOHN in white ink, each containing 150 mg of rifabutin, USP.
MYCOBUTIN is available as follows:
NDC 0013-5301-17 Bottles of 100 capsules
| MYCOBUTIN
rifabutin capsule |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Labeler - Pfizer Laboratories Div Pfizer Inc (134489525) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Pfizer Italia S.r.l. | 458521908 | ANALYSIS(0013-5301) , MANUFACTURE(0013-5301) , PACK(0013-5301) , LABEL(0013-5301) | |
More about Mycobutin (rifabutin)
- Check interactions
- Compare alternatives
- Pricing & coupons
- Drug images
- Side effects
- Dosage information
- During pregnancy
- Generic availability
- Drug class: rifamycin derivatives
- Breastfeeding
- En español