Gallstones
Medically reviewed by Drugs.com. Last updated on Jul 10, 2023.
What are Gallstones?

Gallstones are hardened collections of bile and other compounds that often form inside the gallbladder. The gallbladder is a pouch that collects bile as that liquid flows from the liver to the intestine through the bile ducts. Bile is a fluid that is made, in part, to help with digestion. The salts in bile make it easier for you to digest fat. Bile also contains additional compounds such as cholesterol and bilirubin (created when old red blood cells are destroyed).
Gallstones form in the gallbladder when cholesterol or bilirubin particles begin to cluster together into a solid lump. The stone grows in size as the bile fluid washes over it, much like a pearl forms inside an oyster.
Most of the time, gallstones do not cause any symptoms or problems. Small gallstones can leave the gallbladder and its draining ducts, then pass out of the body through the intestines.
Gallstones can cause symptoms if they become caught in the narrow outlet of the gallbladder, or in the ducts that drain the gallbladder. After meals, especially meals high in fat, thin muscles in the wall of the gallbladder squeeze to help release bile into the intestines. If the gallbladder squeezes against a gallstone, or if a gallstone blocks the fluid from draining easily, it can be very painful.
More serious problems can develop if a gallstone gets into the drainage-duct system but does not make it all the way through to the intestines. In this case, the stone can cause a blockage with buildup of bile in the gallbladder or liver. If bacteria get into the blocked fluid, it can lead to a very serious infection called cholecystitis. If a gallstone lodges low down in the draining ducts, it can also block drainage of digestive enzymes from the pancreas. This can lead to inflammation of the pancreas (pancreatitis).
Gallstones are very common. They occur in 1 out of 5 women by age 60, and they are half as common in men. Gallstones occur more commonly in older people, in people who are overweight, and in people who lose weight suddenly. They also are more likely to occur in women who have been exposed to extra estrogen over their lifetime by having multiple pregnancies, by taking birth control pills, or by taking hormone replacement after menopause.
Symptoms
Eighty percent of people with gallstones do not have any symptoms and do not need treatment. When gallstones do cause symptoms, you might experience:
- abdominal pain, usually high in the abdomen and more often on the right side. The pain can radiate to the back. Pain from gallstones can be steady or come and go. It can last between 15 minutes and several hours each time it occurs.
- sensitivity to high-fat meals. Fats trigger the gallbladder to contract and can worsen your pain.
- belching, gas, nausea, or a general decrease in appetite.
Occasionally, gallstones cause more serious complications, including pancreatitis or infections in the gallbladder or bile ducts. If one of these problems occurs, you may experience fever, more severe abdominal pain, or jaundice (a yellow color of the skin or whites of the eyes).
Diagnosis
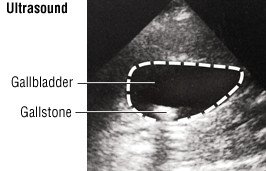
Most gallstones do not show up on regular x-rays, but they are seen easily with an ultrasound. Gallstones are very common, but don't cause symptoms in most people. If you have symptoms that aren't very typical for gallstones, even if you are found to have gallstones on an ultrasound or computed tomography (CT) scan, it may be difficult for your doctor to know if the stones are causing your symptoms.
|
|
If a stone is blocking drainage of bile, an ultrasound might show widened bile ducts. Your doctor may also order blood tests and an abdominal CT scan to evaluate injury to the liver and pancreas.
Expected duration
Smaller gallstones sometimes float out of the gallbladder on their own and are eliminated from the body in feces. Gallstone attacks also can calm down on their own if the bothersome stones shift position within the gallbladder. However, the majority of people whose gallstones cause symptoms will require surgery to cure the problem and will continue to have symptoms until the gallbladder is removed. Even when a gallstone attack subsides on its own, the symptoms will return within two years in about two of three untreated people.
Prevention
You are less likely to form gallstones if you avoid becoming overweight. If you are a dieter, try to avoid diets that cause you to lose weight very quickly, such as diets restricted to fewer than 500 calories daily.
Birth control pills and estrogen can increase the likelihood of gallstones. Consider avoiding these medications if you already have other risk factors for gallstones. Groups at higher than average risk of gallstones include Native Americans, Latinas, people with sickle cell anemia, and women who have had multiple pregnancies.
Treatment
Gallstones require treatment only if they are causing symptoms.
Nearly 90% of patients who want treatment for their gallstones undergo a type of surgery called laparoscopic cholecystectomy. In this procedure, a surgeon uses a small light and camera placed through a small incision into your abdomen. The camera, called a laparoscope, allows the surgeon to see what he or she is doing during the operation by watching a video screen.
Using small instruments that are placed through other small incisions, the surgeon is able to remove fluid and stones from the gallbladder to deflate it. The gallbladder then can be removed and pulled out through one of the same small holes. People recover very quickly from laparoscopic surgery because the surgical wounds are very small.
Some patients need to have their gallbladders removed through a larger incision in a type of surgery called open cholecystectomy. In this surgery, a larger diagonal incision is made above the gallbladder, and the surgeon removes the gallbladder using a direct view instead of a camera.
It is also important to know that in about 5% of cases, a surgeon may start a laparoscopic procedure, but choose to change to an open cholecystectomy for technical reasons.
For stones that are caught in the common bile duct, an additional treatment is usually required. Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure done by a gastroenterology specialist or surgeon to view the opening of the bile duct where it empties into the intestine.
For an ERCP, your doctor uses miniature instruments attached to a camera at the end of a flexible tube (an endoscope). The endoscope is inserted into the intestine through the mouth. During ERCP the gastroenterologist can widen the lower part of the duct so that the stones can pass out into the intestine on their own, and when possible tug out the stone.
For people who cannot tolerate surgery, an oral medication known as ursodeoxycholic acid (Actigall) may be used to help dissolve stones. This treatment usually requires at least six months before results are seen and is only effective in about half of patients. Once the medication is stopped, gallstones are likely to return.
Two other ways to break up gallstones are to use shockwaves (lithotripsy) or to dissolve the stones with solvents injected directly into the gallbladder with a needle. Surgery is strongly preferred over these other treatments because stones are likely to form again if the gallbladder is not removed.
When to call a professional
If you know that you have gallstones, contact your doctor if you develop
- an unexplained fever
- severe or persistent pain in the right side of the abdomen, mid-abdomen, or back
- persistent vomiting
- yellowing of your skin or eyes (jaundice).
Prognosis
Surgical treatment for gallstones is highly effective. In most patients, symptoms go away completely and stay away. The gallbladder is not a necessary organ, and most people do not notice any digestive changes after it is removed. In a few cases, abdominal pain or diarrhea may develop after the gallbladder is removed, and additional treatment or changes in the diet are needed.
Additional info
American College of Gastroenterology (ACG)
https://www.gi.org/
American Gastroenterological Association
https://www.gastro.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.