Epididymitis and orchitis
Medically reviewed by Drugs.com. Last updated on Jul 17, 2023.
What is Epididymitis and orchitis?

Epididymitis is an inflammation of the epididymis. The epididymis is the coiled tube at the back of the testicle. In most cases, an infection causes this inflammation.
Orchitis is an infection of the testicle. It is much less common than epididymitis. Orchitis usually spreads to the testicle through the bloodstream. Viruses commonly cause the infection.
Epididymo-orchitis is an inflammation of both the epididymis and the testicle.
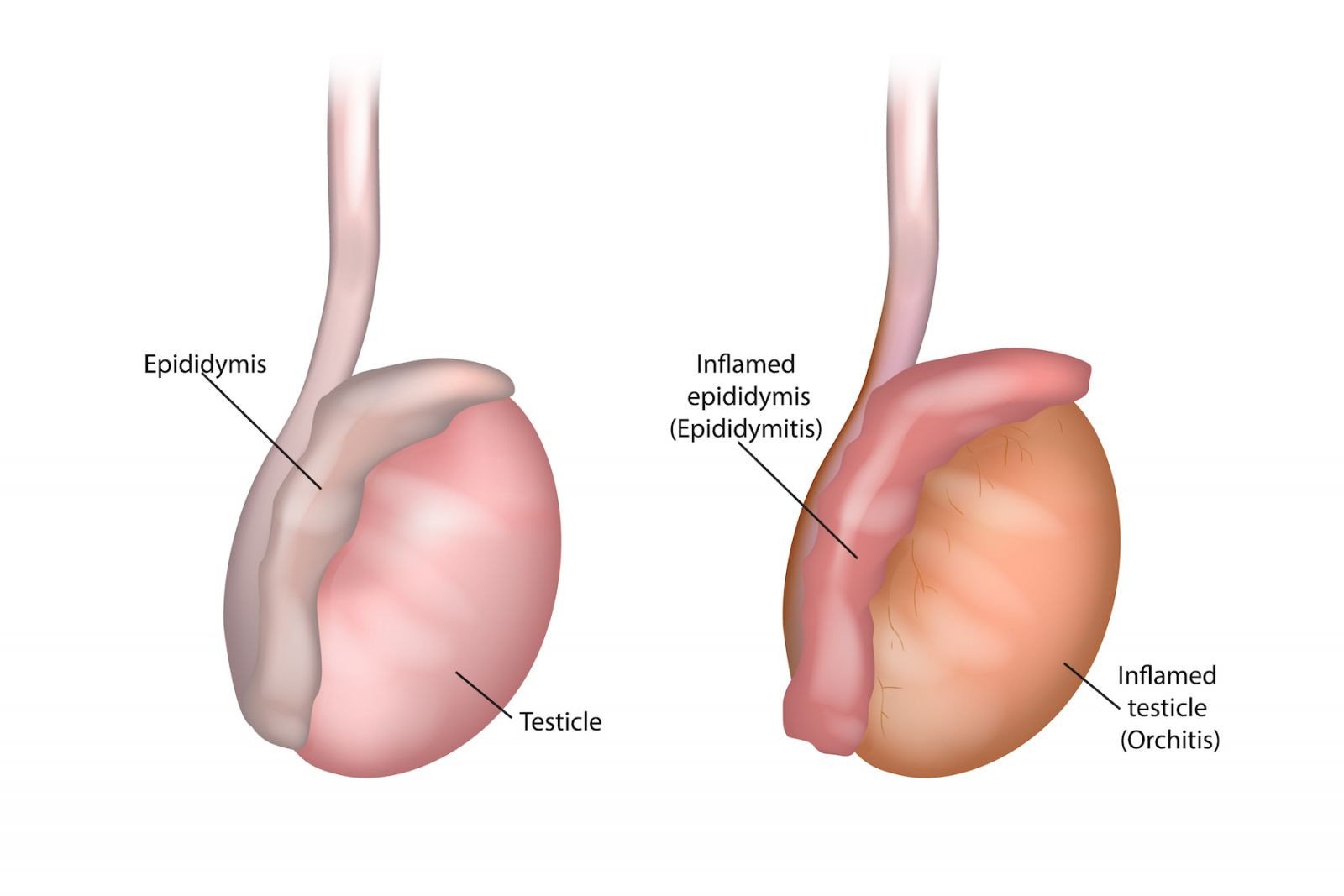
Infections that cause epididymitis usually are related to age, medical history and sexual activity.
Before puberty. Intestinal bacteria, such as E. coli, most often cause epididymitis. The bacteria travel from the bladder or some other site in the urinary tract.
In many cases, a birth-related abnormality affects the urinary tract's structure or function. These abnormalities increase the boy's risk of urinary tract infections (UTIs). The UTIs may eventually spread to the epididymis.
For example, a boy may be born with a structural abnormality of the tube that carries urine through the penis.
In sexually active men. The most common cause of epididymitis is a sexually transmitted disease (STD). The STD is usually chlamydia, gonorrhea or both.
The initial site of infection is the urethra. This is the tube-like passageway that carries urine and semen out of the penis. Eventually, bacteria spread backward through the reproductive tract to attack the epididymis.
This condition may appear several months after the sexual encounter that caused the STD. In some cases, the man first has symptoms of an infected urethra. In other cases, symptoms of epididymitis are the first and only signs of an STD.
Among men who have anal intercourse, epididymitis can be caused by intestinal bacteria from the anus. These bacteria enter the urethra through the penis. They then travel backward through the reproductive tract.
In adults with a high-risk medical history. Some men have a history of UTIs or prostate infections. For them, epididymitis usually is caused by intestinal bacteria that have spread from the infected site.
After surgery, testing or catheterization. Epididymitis may develop after surgery or a diagnostic test that involves the bladder or urethra. Or it may occur after a catheter has been inserted to collect urine.
In these cases, the infection usually is caused by intestinal bacteria. These bacteria enter the urethra or bladder, either during the procedure or through the catheter.
Other forms (all age groups). Rarely, epididymitis can occur when a systemic (whole body) infection spreads through the bloodstream and moves to the epididymis.
Noninfectious epididymitis. A noninfectious form of this condition can occur. Often the exact cause remains unknown. It sometimes develops in men who take amiodarone (Cordarone, Pacerone). This is a heart medication that seems to build up in the epididymis.
Some cases have been blamed on intense exercise, especially heavy lifting. The strain of heavy lifting may force urine from the bladder into the epididymis. There, it can cause a form of chemical irritation that triggers epididymitis.
Many cases of this condition can be treated at home. But some are so severe that hospitalization is necessary.
Symptoms
Symptoms of epididymitis and orchitis can include:
- pain, swelling and tenderness in your scrotum. Only one side of the scrotum is affected.
- pain that at first is most intense at the back of one testicle. Within a few hours the pain spreads to
- the entire testicle
- the overlying scrotum
- in some cases, the groin
- inability to walk without limping because of pain
- redness and heat in the painful area
- burning when you urinate
- an accumulation of watery fluid in the scrotum
- fever, chills and a burning sensation during urination
- a clear, white or yellow abnormal discharge from the tip of your penis.
Diagnosis
You will describe your symptoms. Your doctor will ask questions about your medical history, surgical history and sexual activity. He or she then will examine you, including your genital area.
You may need one or more of the following tests:
- Urinalysis. A chemical analysis of urine.
- Urine cultures. These determine whether bacteria are present in the urine, indicating a possible UTI.
- Laboratory tests. Of fluid taken from inside the urethra or of discharge from the penis.
- Blood tests. To check for signs of infection, including STDs.
Symptoms may be so severe that the doctor must test to see if you have testicular torsion. This is a sudden, painful twisting of the testicle that cuts off the testicle's blood supply.
You may need an ultrasound if there is a concern for testicular torsion. This is a painless test that uses sound waves. In this case, it measures blood flow in the testicles.
Radionuclide scanning is another test you may need. In this test, a small amount of a radioactive isotope is injected into your blood. If the isotope collects near the testicle, it may indicate testicular torsion.
Expected duration
In most cases of mild bacterial epididymitis, pain decreases within one to three days after you start taking antibiotics. However, swelling in the scrotum and testicle may last for several weeks.
Prevention
You can reduce your risk of developing epididymitis caused by STDs. Practice safe sex. Have sex with only one, uninfected partner. Use latex or polyurethane condoms during every sexual activity. This includes oral and anal sex.
Treatment
Antibiotics are used to treat epididymitis caused by:
- STDs. A variety of antibiotics work against chlamydia and gonorrhea. These infections are the most common causes of epididymitis related to STDs. To prevent the spread of these diseases, all your sex partners should receive antibiotics as well.
- Intestinal bacteria. A variety of antibiotics work against this type of infection.
A young boy with epididymitis probably will be referred to a urologist. This doctor specializes in illnesses of the urinary tract and male reproductive organs. The urologist will check for urinary tract problems.
For both epididymitis and orchitis, the following measures can help relieve the discomfort and may lead to quicker recovery:
- Rest in bed for a day or two.
- Elevate your scrotum with a towel.
- Apply cold packs to the painful area.
- Drink plenty of fluids, especially water.
- Take a nonsteroidal anti-inflammatory drug (NSAID) to relieve pain and inflammation. Ibuprofen (Advil, Motrin) and naproxen (Aleve, Naprosyn) are NSAIDs.
People with severe pain in the scrotum may need a prescription pain medication.
When to call a professional
A doctor must evaluate severe pain in the scrotum or testicles. This can be a symptom of testicular torsion, as well as epididymitis.
Call your doctor immediately if you develop pain, tenderness or swelling in your scrotum. Call especially if these symptoms develop rapidly over a few hours.
Also, contact your doctor if you notice an abnormal discharge from your penis or burning when you urinate.
Prognosis
With treatment, most cases of mild epididymitis and orchitis can be cured. There is usually no long-term effect on fertility, especially when only one side of the scrotum is involved.
Additional info
National Institute of Diabetes & Digestive & Kidney Disorders
https://www.niddk.nih.gov/
American Urological Association
https://www.urologyhealth.org/
Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
