Tularemia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is tularemia?
Tularemia is an illness caused by the bacteria Francisella tularensis. It is also called deer-fly fever or rabbit fever. The bacteria that cause tularemia are often found in animals, such as rodents, birds, reptiles, and fish. The bacteria can survive for weeks at low temperatures in water, moist soil, hay, and straw.
How is tularemia spread?
Tularemia is not spread from person to person. You may become infected through any of the following:
- Direct contact by touching the skin, tissues, or fluids of an infected animal. You may also get the disease from any tools that come into contact with an infected animal.
- Food and water that has come into contact with the bacteria. Infected animals can spread the bacteria to water through their urine.
- Breathing in infected dust or spray. This may happen when you mow, harvest, or sweep areas where infected animals have lived or died. You may also breathe in the bacteria if you work with it, such as in a lab.
- Insect bites from ticks, flies, or mosquitoes that have bitten an infected animal. When the insect bites you, the bacteria may be passed to you.
What are the signs and symptoms of tularemia?
Any of the following may begin 1 to 21 days after infection, usually in 3 to 5 days:
- Fever and chills
- Eye redness and pain, swelling of your eyelids, or watery eyes
- Headache and body aches
- Loss of appetite and weight loss
- Shortness of breath, a cough, sore throat, or chest discomfort
- Skin sores
- Vomiting and diarrhea
How is tularemia diagnosed and treated?
Your healthcare provider will examine you and ask about your symptoms. Tell your provider if you recently handled a dead animal or were bitten by an insect. Antibiotics will be used to treat the infection if tests confirm tularemia:
- Blood tests are done to check for the bacteria that causes tularemia.
- A chest x-ray is done to look for a lung infection, such as pneumonia.
- Cultures may be done to check for the bacteria that cause tularemia. A sample of your urine, skin, wound, or mucus may be taken and sent for tests.
How can I prevent tularemia?
- Cook meat thoroughly before you eat it. This is especially important when you eat meat from hunting.
- Get vaccinated if you are at high risk for tularemia. This includes people who hunt or work around the bacteria.
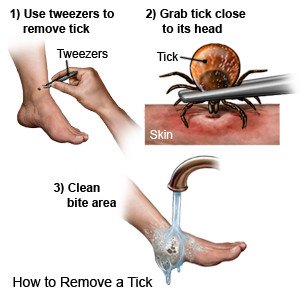
- Remove ticks immediately. Use an insect repellant to prevent insect bites.
- Wash all items that come into contact with a sick or dead animal. Wash your hands as soon as possible. Use soap and water. Wash the front and back of your hands, and in between your fingers. Wash for at least 20 seconds. Rinse with warm, running water for several seconds. Then dry your hands with a clean towel or paper towel. Carefully clean tools that have been used on an infected animal. Use bleach or alcohol to kill the bacteria and prevent them from spreading.

- Wear protective clothing when you contact animals. Examples include gloves, long sleeves, and pants. Protective clothing will also help prevent insect bites. A mask may help prevent exposure when you work outside.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your local emergency number (911 in the US) or have someone call if:
- You have fainted.
- You have sudden chest pain.
- You have sudden trouble breathing.
When should I seek immediate care?
- You have a severe headache and neck pain.
- You feel weak and confused.
- Your symptoms do not improve even after you take antibiotics.
When should I call my doctor?
- You have a fever with or without chills.
- You have a new rash.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Tularemia
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
