Tetralogy of Fallot in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
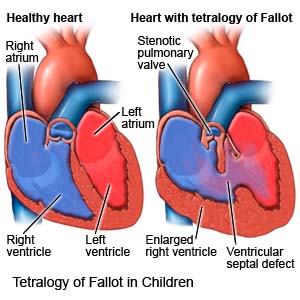
Tetralogy of Fallot (TOF) is a heart condition your child was born with. TOF causes the following 4 heart structure defects that lead to a weak heart and decreased blood flow:- A narrowed blood vessel that connects the heart to the lungs
- A hole in the wall that separates the heart
- Aorta (major artery) growth from both sides of the heart instead of from one side as normal
- Blood flow that backs up and causes the right side of the heart to enlarge and thicken
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- Your child has sudden trouble breathing.
- Your child has a seizure.
Seek care immediately if:
- Your child faints.
- Your child's lips or fingernails are blue or white.
Call your child's doctor or cardiologist if:
- Your child has a fever.
- Your child's signs and symptoms get worse.
- Your child is unusually fussy or irritable.
- Your child has weakness.
- You have questions or concerns about your child's condition or care.
Medicines:
- Medicines help your child's heart beat strongly and regularly, or help get rid of extra fluid.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Give your child's medicine as directed. Contact your child's healthcare provider if you think the medicine is not working as expected. Tell the provider if your child is allergic to any medicine. Keep a current list of the medicines, vitamins, and herbs your child takes. Include the amounts, and when, how, and why they are taken. Bring the list or the medicines in their containers to follow-up visits. Carry your child's medicine list with you in case of an emergency.
Care for your child:
- Place your child on his or her side and pull his or her knees up to his or her chest if he or she turns blue. This will help increase blood flow to his or her lungs.
- Keep your child's gums and teeth clean and healthy. Brush your child's gums or teeth regularly. Ask if your child needs antibiotics when he or she gets his or her teeth cleaned.
- Do not smoke around your child. If you smoke, it is never too late to quit. Smoke can harm your child's heart and lungs and make it hard for him or her to breathe. Ask for information if you need help quitting.
- Have your child vaccinated to help protect him or her against infections caused by viruses or bacteria. Ask for more information about vaccinations for your child.
Follow up with your child's doctor or cardiologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Tetralogy of Fallot
- Atorvastatin (Lipitor): Top 12 Drug Facts You Need to Know
- Do blood pressure drugs interact with alcohol?
- Side Effects of Weight Loss Drugs
Treatment options
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
