Second-Degree Burn
Medically reviewed by Drugs.com. Last updated on Jun 2, 2025.
What is a second-degree burn?
A second-degree burn is also called a partial-thickness burn. A second-degree burn occurs when the first layer and some of the second layer of skin are burned. A superficial second-degree burn usually heals within 2 to 3 weeks with some scarring. A deep second-degree burn can take longer to heal. A second-degree burn can also get worse after a few days and become a third-degree burn.
What causes a second-degree burn?
Direct exposure to heat or flame is the most common cause of second-degree burn. This includes contact with hot objects or flames such as an iron, a skillet, tar, cigarettes, or fireworks. The following may also cause a second-degree burn:
- Harsh chemicals, such as cleaning products, car battery acid, gasoline, or cement
- Damaged electrical cords or electrical outlets
- Hot water or steam
- Exposure to harmful rays from the sun or from tanning beds
What are the signs and symptoms of a second-degree burn?
- A superficial second-degree burn includes the first layer and some of the second layer. The deeper layers, sweat glands, and oil glands are not damaged. The skin is red, moist, very painful to the touch, and has blisters. Areas of redness turn white when pressure is applied. The area returns to red quickly when the pressure is removed.
- A deep second-degree burn includes damage in the middle layer, and in the sweat glands and oil glands. The skin is mixed red or waxy white, and wet or moist. Some areas of redness may turn white when pressure is applied. The area may return to red slowly or not all when the pressure is removed.
How is a second-degree burn diagnosed?
Your healthcare provider will ask how you were burned. Tell him or her about your symptoms. He or she will examine your burn and determine how severe it is. Laser scanners may be used to check the blood flow in your skin.
How is a second-degree burn treated?
- Medicines may be used to decrease pain, prevent infection, or help your burn heal. They may be given as a pill or as an ointment applied to your skin.
- Surgery may remove damaged tissue, replace or cover lost skin, or relieve pressure and improve blood flow. Surgery can help prevent infection, decrease inflammation, and improve healing. Surgery can also improve the appearance of your skin and reduce scarring.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How do I care for the burn?
- Wash your hands with soap and water. Dry your hands with a clean towel or paper towel.

- Remove old bandages. You may need to soak the bandage in water before you remove it so it will not stick to your wound.
- Gently clean the burned area daily with mild soap and water. Pat the area dry. Look for any swelling or redness around the burn. Do not break closed blisters. You may cause a skin infection.
- Apply cream or ointment to the burn with a cotton swab. Place a nonstick bandage over your burn.
- Wrap a layer of gauze around the bandage to hold it in place. The wrap should be snug but not tight. It is too tight if you feel tingling or lose feeling in that area.
- Apply gentle pressure for a few minutes if bleeding occurs.
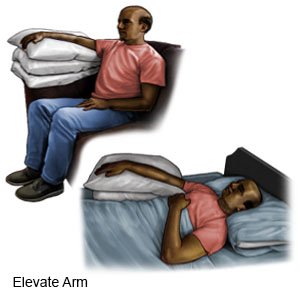
- Elevate your burned arm or leg above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your burned arm or leg on pillows or blankets to keep it elevated comfortably.
What can I do to care for myself?
- Drink liquids as directed. You may need to drink extra liquid to help prevent dehydration. Ask how much liquid to drink each day and which liquids are best for you.
- Go to physical therapy, if directed. Your muscles and joints may not work well after a second-degree burn. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain.
Why may I need physical therapy?
Your muscles and joints may not work well after a second-degree burn. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain.
How can I prevent second-degree burns?
- Do not leave cups, mugs, or bowls containing hot liquids at the edge of a table. Keep pot handles turned away from the stove front.
- Do not leave a lit cigarette. Make sure it is no longer lit. Then dispose of it safely.
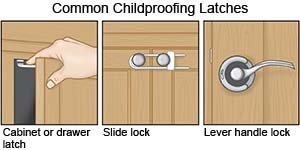
- Store dangerous items out of the reach of children. Store cigarette lighters, matches, and chemicals where children cannot reach them. Use child safety latches on the door of the safe storage area.
- Keep your water heater setting to low or medium (90°F to 120°F, or 32°C to 48°C).
- Wear sunscreen that has a sun protectant factor (SPF) of 15 or higher. The sunscreen should also have ultraviolet A (UVA) and ultraviolet B (UVB) protection. Follow the directions on the label when you use sunscreen. Put on more sunscreen if you are in the sun for more than an hour. Reapply sunscreen often if you go swimming or are sweating.
Related medications
Xylocaine Jelly
Xylocaine Jelly is used for anal itching, anesthesia, burns, external, gastrointestinal surgery ...
Mounjaro
Mounjaro is used for type 2 diabetes to help lower blood sugar levels. Mounjaro has also been shown ...
Bactine
Bactine is used for burns, external, local anesthesia, pain, pruritus, sunburn
AneCream
AneCream is used for anal itching, burns, external, hemorrhoids, local anesthesia, pain, pruritus ...
Xylocaine Topical
Xylocaine Topical is used for anal itching, anesthesia, burns, external, hemorrhoids, local ...
CidalEaze
CidalEaze is used for anal itching, anesthesia, burns, external, hemorrhoids, local anesthesia ...
Eha Lotion
Eha Lotion is used for anesthesia, burns, external, hemorrhoids, local anesthesia, pain, pruritus ...
DermacinRx Lido V Pak
DermacinRx Lido V Pak is used for anesthesia, burns, external, gastrointestinal tract examination ...
When should I seek immediate care?
- You have a fast heartbeat or breathing.
- You are not urinating.
When should I call my doctor?
- You have a fever.
- You have increased redness, numbness, or swelling in the burn area.
- Your wound or bandage is leaking pus and has a bad smell.
- Your pain does not get better, or gets worse, even after you take pain medicine.
- You have a dry mouth or eyes.
- You are overly thirsty or tired.
- You have dark yellow urine or urinate less than usual.
- You have a headache or feel dizzy.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Second-Degree Burn
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
