Patellofemoral Pain Syndrome
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is patellofemoral pain syndrome (PFPS)?
PFPS is pain in or around your patella (kneecap). PFPS is also called runner's knee or jumper's knee and is common in athletes. PFPS can develop when the patella rubs against the femur (thigh bone) as you move your knee. It may also happen when the patella moves out of place. PFPS may be caused by chondromalacia. This is a softening and breakdown of the cartilage under your kneecap. The kneecap is a natural shock absorber. Trauma, previous injury to your knee, excessive use, or activities such as running can cause your symptoms.
What increases my risk for PFPS?
- Increased activity, or overactivity
- A hip, knee, and ankle that are not lined up correctly
- Leg muscles that are not balanced or are weak
- Fallen or high arches
- Obesity
What are the signs and symptoms of PFPS?
- Popping or crackling sounds when you move your knee
- Pain when you go up or down the stairs, squat, run, or ride a bike
- Pain after you sit for a long time with your knees bent
- Swelling, stiffness, or weakness in your knee
How is PFPS diagnosed?
Your healthcare provider will examine your knee and ask about your symptoms. He or she may move your legs in different directions to check for pain, and to see how your kneecap moves. You may also need the following:
- An x-ray, CT, or MRI may show damage to your knee and the tissues that surround it. You may be given contrast liquid to help your knee show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- Arthroscopy may be used to look inside your knee. Healthcare providers use a scope (thin, bendable tube with a light and camera on the end) to examine your knee.
How can I manage my symptoms?
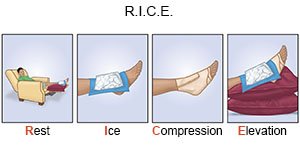 |
- Change your activity. You may need to rest your knee. You may need to change your exercise routine to low-impact activities.
- Apply ice on your knee for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it. Ice helps prevent tissue damage and decreases swelling and pain.
- Elevate your knee above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your leg on pillows or blankets to keep it elevated comfortably. Do not put a pillow directly under your knee.

- Support your knee by wrapping it with tape or an elastic bandage. You may need a brace for more support. This will help decrease swelling and keep your kneecap in the correct spot.
- Wear shoe inserts as directed. Orthotics or arch supports help keep your foot and ankle stable and in line to decrease stress on your knee.
- Go to physical therapy as directed. A physical therapist will teach you exercises to help improve movement and strength, and to decrease pain.
- Maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Ask him or her to help you create a weight loss plan if you are overweight. Weight loss can help decrease pressure on your knee.
How is PFPS treated?
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Surgery may be needed if other treatments do not work. During surgery, the back of your kneecap is smoothed. A ligament may also be cut to allow the knee to return to its normal position. Surgery may be done through small incisions as during arthroscopy, or you may need a larger incision. A cut in your shin bone may also be needed to help line up your kneecap correctly.
How can I prevent another episode?
- Wear the right shoes for your activities. Increase activity gradually.
- Warm up before you exercise. Stretch your leg muscles before and after activity.
When should I call my doctor?
- You have trouble walking.
- You have a fever.
- Your knee brace or sleeve is too tight.
- Your symptoms are not getting better, or they get worse.
- Your pain and swelling increase even after you take pain medicine.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
