Obesity in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is obesity?
Obesity means your child's body mass index (BMI) is at or above the 95th percentile. BMI is your child's weight divided by height. The percentile compares your child's BMI with the BMIs of children his or her age.
What are the risks of obesity?
- Low self-esteem, being bullied, depression, or eating disorders
- Diabetes
- Heart disease, high blood pressure, and high cholesterol
- Asthma and sleep apnea (episodes in which your child stops breathing at night)
- Arthritis, knee, and hip pain
- Gallbladder and liver disease
- Abnormal monthly periods and other hormone problems
- A higher risk for obesity as an adult
How is obesity treated?
The goal of treatment is to decrease your child's BMI and decrease the risk for health problems. Your child's healthcare provider may suggest that the current weight is maintained. As your child grows in height, the BMI will decrease. Even a small decrease in BMI can reduce the risk for many health problems. Your child's provider will work with you and your child to set goals.
- Meet with other healthcare providers to help you and your child start to make lifestyle changes. Your child may have counseling from providers such as a dietitian, physical therapist, and psychologist. Your child may meet with providers, or you may meet as a family. Family meetings may help everyone in the family understand how to support your child. Counseling may help your child change his or her nutrition or activity habits.
- Lifestyle changes include making healthy food choices and getting regular physical activity.
- Other treatments may be suggested by your child's provider if your child is older and has medical problems caused by obesity. These treatments are used in addition to lifestyle changes to treat severe obesity. Medicine may be given to decrease the amount of fat your child's body absorbs from food.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What eating changes can our family make?
 |
- Stick to a schedule of 3 meals a day and 1 or 2 healthy snacks. Meals and snacks should be 2 to 4 hours apart. Only offer water between meals.
- Eat dinner together as a family as often as possible. Ask your child to help you prepare meals. Limit fast food and restaurant meals because they are often high in calories.

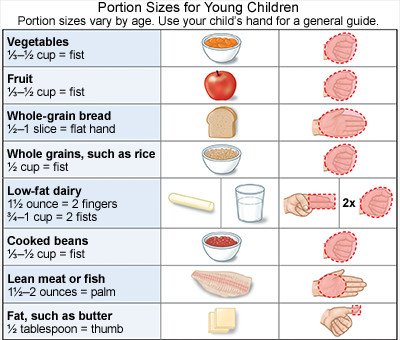
- Decrease portion sizes. Use small plates, no larger than 9 inches in diameter. Fill your child's plate half full of fruits and vegetables. Do not put serving dishes on the table. Do not make your child finish everything on the plate.
- Limit soda, sports drinks, and fruit juice. These sugary beverages are high in calories. Offer your child water as the main beverage.
- Pack healthy lunches. An example is a turkey sandwich on whole-wheat bread with an apple, baby carrots, and low-fat milk.
Related medications
What activity changes can our family make?
- Encourage your child to be active for 60 minutes most days of the week. Find sports or activities that are fun for your child, such as cycling, swimming, or running. Be active with your child. Go for a walk, go bowling, or play at a park.
- Limit your child's screen time. Screen time is the amount of television, computer, smart phone, and video game time your child has each day. It is important to limit screen time. This helps your child get enough sleep, physical activity, and social interaction each day. Your child's pediatrician can help you create a screen time plan. The daily limit is usually 1 hour for children 2 to 5 years. The daily limit is usually 2 hours for children 6 years or older. You can also set limits on the kinds of devices your child can use, and where he or she can use them. Keep the plan where your child and anyone who takes care of him or her can see it. Create a plan for each child in your family. You can also go to https://www.healthychildren.org/English/media/Pages/default.aspx#planview for more help creating a plan.
- Help your child have a regular sleep schedule. Make sure your child gets at least 8 hours of sleep each night. Sleep schedules that are not consistent can affect your child's weight.
What are other things I can do to help my child?
- Help your child set small, realistic goals. Do not talk about diets or weight. Focus instead on helping your child create his or her own goals. An example of a small goal is to have a vegetable with every meal.
- Teach your child how to make healthy choices. This includes when your child is at school or away from home. Teach your child to use nutrition information on food labels to make healthy choices. Ask your child to help you make healthy choices while grocery shopping. Shop for healthy snacks, such as fruit, yogurt, nuts, and low-fat cheese. Praise your child for healthy choices.
- Practice healthy habits with your child. Teach by example to motivate your child. Remove unhealthy foods and replace them with healthy options for the whole family. Help your child learn not to use food as a way to manage stress. Encourage your child to start a hobby or to use relaxation methods such as breathing or stretching exercises.
- Do not use food to reward or punish your child. Reward your child with fun activities or social events with friends.
When should I seek immediate care?
- Your child has a severe headache or vision problems.
- Your child has trouble breathing during physical activity.
When should I call my child's doctor?
- Your child has lost interest in social activities, does not want to go to school, or seems depressed.
- Your child has signs of diabetes, such as being very hungry, very thirsty, and urinating often.
- Your child has signs of gallbladder or liver disease, such as pain in the upper abdomen.
- Your child has hip or knee pain and discomfort while walking.
- Your child has signs of sleep apnea, such as daytime sleepiness, snoring, or bed wetting.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Obesity
- Can You Mix Weight Loss Drugs and Alcohol?
- FDA-Approved Weight Loss Drugs: Can They Help You?
- Side Effects of Weight Loss Drugs
- Top 10 Diabetes Treatments You May Have Missed
- Weight Loss Drugs & Injections: What Are Your Options?
- Which Drugs Cause Weight Gain?
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
