Stillbirth
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is stillbirth?
A stillbirth is the loss of a baby after 20 weeks of pregnancy. Sometimes a stillbirth happens before labor begins. A stillbirth may also happen during labor and delivery.
What causes a stillbirth?
The cause of a stillbirth may not be known. The following are possible causes of a stillbirth:
- An infection such as cytomegalovirus, toxoplasmosis, or a sexually transmitted infection in the mother, baby, or placenta
- Complications during pregnancy, such as preeclampsia, preterm labor, or trauma
- Problems with the baby, such as a birth defect, fetal growth restriction, or a genetic condition
- Problems with the placenta, such as blood clots, swelling, or separation of the placenta from the wall of the uterus
- Problems with the umbilical cord, such as a knot that prevents oxygen and blood flow to the baby
- Problems during labor and delivery that prevent blood and oxygen from reaching the baby
What increases my risk for a stillbirth?
- Age 35 or older
- Use of drugs, alcohol, or cigarettes during pregnancy
- Black or African-American ancestry
- Overweight or obesity
- A past miscarriage or stillbirth
- Being pregnant with 2 or more babies
- Stressful life events such as the death of a loved one
- Fertility treatments to help you get pregnant
What are the signs and symptoms of stillbirth?
You may not have any signs or symptoms, or you may have any of the following:
- Decreased fetal movement
- Vaginal bleeding
- Abdominal cramping or contractions
- Abdominal or back pain
- No heartbeat in the baby
How is stillbirth diagnosed?
Your healthcare provider will ask about your medical history, past pregnancies, and your medicines. Tell your provider if you can feel your baby moving inside your uterus. Your provider will check if your baby has a heartbeat. You may need any of the following tests:
- External fetal heart monitoring is used to find and monitor your baby's heartbeat and the contractions of your uterus. A small monitor is placed on your abdomen. A belt will be put around your waist to hold the monitor in place.
- Ultrasound pictures may be used to check for your baby's heartbeat.
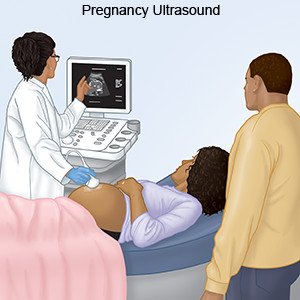
How will my baby be delivered?
Talk to your healthcare provider about the ways your baby can be delivered, such as the following:
- Natural labor may happen within 2 weeks of a stillbirth.
- Induction means your provider will give you medicine to make labor and delivery happen. Your labor may be induced if you do not go into natural labor within 2 weeks of a stillbirth.
- Dilation and evacuation is surgery to deliver your baby. Your provider will dilate (open) your cervix and deliver your baby through your vagina.
- A cesarean , or C-section, is surgery to deliver your baby. Your provider will make an incision in your lower abdomen. Your baby will be delivered through the incision.
What can I expect after delivery?
You will have a choice to see your baby after delivery. You and your loved ones will have time alone with your baby. You can hold and name your baby, take pictures, or have a religious ceremony. Ask your healthcare provider if you can have something to remember your baby. This can include a handprint, a footprint, or baby blanket.
What tests can be done after a stillbirth?
Tests can be done to help find the cause of a stillbirth. Information from these tests may also help you plan for a future pregnancy. You can choose to have you or your baby tested. Your healthcare provider may also examine the fetus, umbilical cord, and placenta for problems. Tests may include any of the following:
- A blood test may be used to check for infections.
- A tissue biopsy is a procedure to remove a small amount of tissue from your baby. The sample will be sent to the lab to be tested.
- Amniocentesis is used to take a sample of amniotic fluid to be tested for an infection or birth defect. The amniotic sac contains the fluid around your baby. A needle will be put through your skin and into your uterus. Amniotic fluid is pulled out through the needle. The sample will then be sent to the lab for tests.
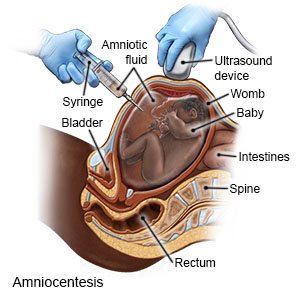
- An autopsy is a procedure used to examine your baby to look for problems with the brain, heart, or other organs.
How can I care for myself after a stillbirth?
- Rest as directed. You will need time to heal after a stillbirth. Ask when it is safe for you to drive, walk up stairs, lift heavy objects, and have sex. Ask when it is okay to exercise, and what types of exercise to do. Slowly start to do more each day. Return to your daily activities as directed.
- Care for your breasts. Your breasts prepare for lactation during pregnancy. Your breast milk will come in 3 to 4 days after delivery. Breast milk production will stop over time. Your breasts may start to swell and feel hard to the touch. Drops of milk may leak from your breasts. You may need medicines to reduce discomfort and pain, or stop milk production. Ask your provider how to care for your breasts.
- Use sanitary pads as needed. You may have light bleeding or spotting for 1 to 2 weeks.
- Eat healthy foods. Healthy foods will help maintain your energy levels while you recover. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish.

- Share your thoughts and feelings. Talk to someone you trust about your feelings. Allow yourself to cry when you need to.
- Practice mindfulness or relaxation techniques. Yoga, meditation, or deep breathing can help you relax and improve emotional health.
- Join a support group or seek counseling. The loss of a baby can be difficult for you and your partner. You and your loved ones need time to grieve. You may feel shock, anger, helpless, or lonely. You may be at an increased risk for postpartum depression. A support group or counselor can help you talk about the loss of your baby. Ask your healthcare provider for more information on support groups.
- Remember your baby. Create a memory box, plant a tree, or have a spiritual ceremony to help with your grief.
Where can I find support and more information?
- March of Dimes Birth Defects Foundation
1275 Mamaroneck Avenue
White Plains , NY 10605
Web Address: http://www.marchofdimes.com
- First Candle
1314 Bedford Avenue, Suite 210
Baltimore , MD 21208
Phone: 1- 800 - 221-7437
Web Address: http://www.firstcandle.org
When should I seek immediate care?
- You have heavy vaginal bleeding that fills 1 or more sanitary pads in 1 hour.
- You have severe abdominal pain even after you take pain medicine.
- You feel weak, dizzy, or faint.
- You have thoughts of harming yourself.
When should I call my obstetrician?
- You have a fever.
- You have nausea or are vomiting.
- You have foul-smelling fluid coming from your vagina.
- You or your partner feel depressed, hopeless, or cannot cope with what has happened.
- You have trouble sleeping or eating.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Stillbirth
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
