Leg Fracture in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
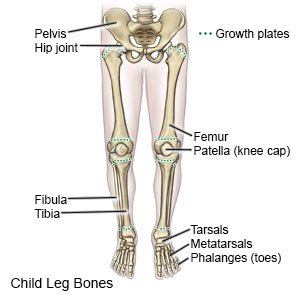
A leg fracture is a break in a bone in your child's leg.
 |
DISCHARGE INSTRUCTIONS:
Return to the emergency department if:
- Your child has increased pain in his or her leg that does not go away, even after he or she takes medicine.
- Your child's cast gets wet or damaged.
- Your child's leg or toes are numb.
- Your child's skin or toenails become swollen, cold, white, or blue.
Call your child's doctor or bone specialist if:
- Your child has a fever.
- Your child's cast or brace is too tight.
- You notice new blood stains or a bad smell coming from under the cast.
- Your child has new or worsening trouble moving his or her leg.
- You have questions or concerns about your child's condition or care.
Medicines:
Your child may need any of the following:
- Prescription pain medicine may be given. Ask your child's healthcare provider how to give this medicine safely. Some prescription pain medicines contain acetaminophen. Do not give your child other medicines that contain acetaminophen without talking to a healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your child's healthcare provider how to prevent or treat constipation.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If your child takes blood thinner medicine, always ask if NSAIDs are safe for him or her. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to give your child and how often to give it. Follow directions. Read the labels of all other medicines your child uses to see if they also contain acetaminophen, or ask your child's doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Give your child's medicine as directed. Contact your child's healthcare provider if you think the medicine is not working as expected. Tell the provider if your child is allergic to any medicine. Keep a current list of the medicines, vitamins, and herbs your child takes. Include the amounts, and when, how, and why they are taken. Bring the list or the medicines in their containers to follow-up visits. Carry your child's medicine list with you in case of an emergency.
Care for your child at home:
- Have your child rest as much as possible and get plenty of sleep.
- Apply ice on your child's leg for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it. Ice helps prevent tissue damage and decreases swelling and pain.
- Elevate your child's leg above the level of his or her heart as often as possible. This will help decrease swelling and pain. Prop your child's leg on pillows or blankets to keep it elevated comfortably.

- Have your child use crutches as directed. Crutches will help your child keep some weight off the leg while it heals.
- Take your child to physical therapy as directed. A physical therapist teaches your child exercises to help improve movement and strength, and to decrease pain.
Cast or brace care:
- Your child may take a bath as directed. Do not let your child's cast or brace get wet. Before he or she bathes, cover the cast or brace with a plastic trash bag. Tape the bag to your child's skin above the cast to seal out water. Have your child keep his or her leg out of the water in case the bag breaks. If a plaster cast gets wet and soft, call your child's healthcare provider.
- Check the skin around the cast or brace every day. You may put lotion on any red or sore areas.
- If your child has a hip spica cast, you will be taught to help him or her use the bathroom and take a bath. You will learn how to clean the cast and keep it dry. You will also learn how to move and dress your child.
- Do not let your child push down or lean on the cast or brace.
- Do not let your child put a sharp or pointed object inside the cast to scratch an itch.
Physical therapy:
Your child may need physical therapy. A physical therapist will help him or her with exercises to make his or her bones and muscles stronger.
Follow up with your child's doctor or bone specialist as directed:
Your child may need to return to have his or her cast removed. He or she may also need an x-ray to check how well the bone has healed. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Leg Fracture
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
