Laser Assisted Uvulopalatoplasty
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
WHAT YOU NEED TO KNOW:
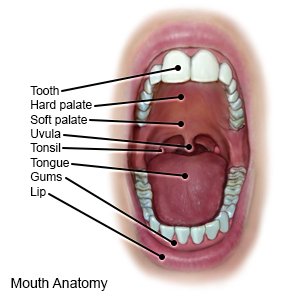
Laser assisted uvulopalatoplasty (LAUP) is a procedure to remove part or all of your uvula. The uvula is the small piece of flesh that hangs at the back of your throat. LAUP may help you breathe easier, decrease snoring, and improve your sleep.
 |
HOW TO PREPARE:
The week before your procedure:
- Arrange to have someone drive you home the procedure.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine before the procedure, and when to stop. He or she will tell you which medicines to take or not take on the day of the procedure.
- Tell your surgeon about all your allergies. Include medicines, antibiotics, and anesthesia.
- You may need blood or urine tests before your procedure. You may also need x-rays, an EKG, or a pharyngoscopy. Talk to your healthcare provider about these or other tests you may need. Write down the date, time, and location for each test.
The night before your procedure:
You may be told not to eat or drink anything after midnight.
The day of your procedure:
- Take only the medicines your surgeon told you to take.
- Healthcare providers may insert an intravenous tube (IV) into your vein. A vein in the arm is usually chosen. You may be given liquids or medicine through the IV.
- An anesthesiologist will talk to you before your surgery. You may need medicine to keep you asleep or numb an area of your body during surgery. Tell healthcare providers if you or anyone in your family has had a problem with anesthesia in the past.
- You or a close family member will be asked to sign a legal document called a consent form. It gives healthcare providers permission to do the procedure or surgery. It also explains the problems that may happen, and your choices. Make sure all your questions are answered before you sign this form.
WHAT WILL HAPPEN:
What will happen:
Anesthesia medicine will be sprayed in the back of your mouth and throat. After a few minutes, anesthesia medicine will also be injected in the back of your mouth. This will keep your mouth and throat numb during the procedure. Medical tools will be used to hold your mouth open during the procedure. Your surgeon will use a laser to cut away part or all of your uvula.
After your procedure:
You will be taken to a room to recover. You will be monitored closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You will then be able to go home.
CONTACT YOUR HEALTHCARE PROVIDER IF:
- You have a fever.
- You get a cold or the flu.
- You have questions or concerns about your procedure.
Risks
You may bleed more than expected or get an infection. The sound of your voice may change. You may lose your sense of taste temporarily. The laser may scar the inside of your throat. Your snoring or sleep apnea may not go away or may get worse.
Related medications
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Laser Assisted Uvulopalatoplasty
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
