How to Prevent Pressure Injuries
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a pressure injury?
A pressure injury is an injury to the skin or tissue over a bony area. A pressure injury is also called a pressure sore, bedsore, wound, or decubitus ulcer. Pressure injuries can form over any area but are most common on the back, buttocks, hips, and heels.
What causes pressure injuries?
- Continuous pressure builds when you sit or lie on a bony area for too long. Pressure slows or stops the blood from flowing to the skin. This may hurt the skin and cause tissue damage. Pressure can start to cause damage to your skin and tissue about 2 hours after staying in the same position.
- Shearing or friction happens when delicate skin is dragged across a surface, such as sheets. This may cause your skin to tear or a blister to form. Sliding up or down in bed or moving from the bed to a chair may tear your skin. Muscle spasms may cause your arms or legs to jerk and rub the sheets, causing tears in your skin.
What increases my risk for a pressure injury?
- Long periods of time without moving
- Short periods of increased pressure, such as sitting in a wheelchair
- Not being able to control your urine or bowel movements
- Dehydration or poor nutrition
- Numbness
- Poor blood flow to your limbs
- Age over 65 years
- Previous pressure injury
What can I do to help prevent a pressure injury?
 |
- Check your skin several times each day. Check for red skin, or other color changes, over bony areas. Use a mirror if you have trouble seeing certain areas, or ask another person to look.
- Change wet bedding and clothes right away. The wet material may rub against your skin and cause damage.
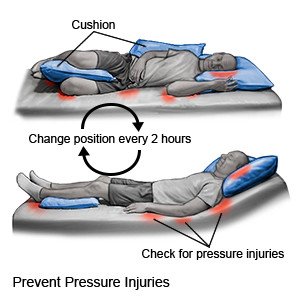
- Change your position often. Change your position every 2 hours if you are in a bed all day. Change your position every hour if you are in a wheelchair all day. Set an alarm to help remind you when it is time to turn. Keep a written turning schedule to help you remember to turn. If you are helping a person move in bed, lift him. Do not slide him. Keep the head of the bed as low as possible. This may help prevent damage to the skin from sliding down in bed.
- Protect the skin over bony areas. Use pillows or foam wedges to keep bony areas from touching, and to relieve pressure. For example, put a pillow or foam wedge between your knees to keep them from pressing on one another. Place a pillow or foam wedge under you to keep your hip raised when you lie on your side. Do not rest directly on your hipbone. Put a foam pad or pillow under your legs from calf to ankle when you lie on your back. The pad or pillow should raise your heels so that they are not touching the bed.
- Use medical equipment and pads. A draw sheet or large pad under you may help others move you up in bed. An overhead trapeze can help you change positions in bed. Mattresses and overlays made to provide more cushioning may help decrease the risk of pressure injuries. Examples include a foam mattress pad and air or water mattresses. Ask about equipment that may be right for you and how you use it.
- Keep your skin clean, dry, and moisturized. Use mild soap and warm water to clean your skin. Do not rub or scrub when you wash. Do not use products that contain alcohol, because they can dry out your skin. Gently pat your skin dry. Do not rub your skin with a towel. Apply lotion or a moisturizer on your skin often.
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, and fish. Foods that are high in protein may help your pressure injury heal. This includes lean meats, beans, milk, yogurt, and cheese. Nutrition shakes may also give you extra calories and protein if you have trouble eating or are underweight.

When should I contact my healthcare provider?
- You have a fever.
- You see red or purple skin over a bony area.
- You see a blister or open sore over a bony area.
- Your skin feels warm, spongy, or tight.
- You have new pain, or pain that is getting worse.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
