Foot Care for People with Diabetes
Medically reviewed by Drugs.com. Last updated on Sep 1, 2024.
What do I need to know about foot care?
Long-term high blood sugar levels can damage the blood vessels and nerves in your legs and feet. This damage makes it hard to feel pressure, pain, temperature, and touch. You may not be able to feel a cut or sore, or shoes that are too tight. Foot care is needed to prevent serious problems, such as an infection or amputation. Diabetes may cause your toes to become crooked or curved under. These changes may affect the way you walk and can lead to increased pressure on your foot. The pressure can decrease blood flow to your feet. Lack of blood flow increases your risk for a foot ulcer.
How do I care for my feet?
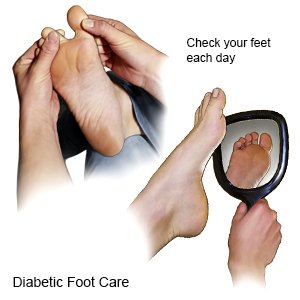
- Check your feet each day. Look at your whole foot, including the bottom, and between and under your toes. Check for wounds, corns, and calluses. Use a mirror to see the bottom of your feet. The skin on your feet may be shiny, tight, or darker than normal. Your feet may also be cold and pale. Feel your feet by running your hands along the tops, bottoms, sides, and between your toes. Redness, swelling, and warmth are signs of blood flow problems that can lead to a foot ulcer. Do not try to remove corns or calluses yourself. Do not ignore small problems, such as dry skin or small wounds. These can become life-threatening over time without proper care.
- Wash your feet each day with soap and warm water. Do not use hot water, because this can injure your foot. Dry your feet gently with a towel after you wash them. Dry between and under your toes.
- Apply lotion or a moisturizer on your dry feet. Ask your care team provider what lotions are best to use. Do not put lotion or moisturizer between your toes. Moisture between your toes could lead to skin breakdown.
- Cut your toenails correctly. File or cut your toenails straight across. Use a soft brush to clean around your toenails. If your toenails are very thick, you may need to have a care team provider or specialist cut them.
- Protect your feet. Do not walk barefoot or wear your shoes without socks. Check your shoes for rocks or other objects that can hurt your feet. Wear cotton socks to help keep your feet dry. Wear socks without toe seams, or wear them with the seams inside out. Change your socks each day. Do not wear socks that are dirty or damp.
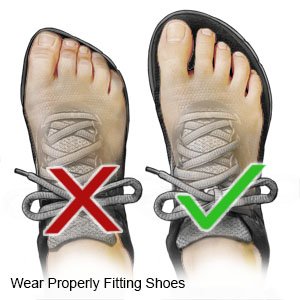
- Wear shoes that fit well. Wear shoes that do not rub against any area of your feet. Your shoes should be ½ to ¾ inch (1 to 2 centimeters) longer than your feet. Your shoes should also have extra space around the widest part of your feet. Walking or athletic shoes with laces or straps that adjust are best. Ask your care team provider for help to choose shoes that fit you best. Ask your provider if you need to wear an insert, orthotic, or bandage on your feet.
- Go to your follow-up visits. Your care team provider will do a foot exam at least 1 time each year. You may need a foot exam more often if you have nerve damage, foot deformities, or ulcers. Your provider will check for nerve damage and how well you can feel your feet. Your provider will check your shoes to see if they fit well.
- Do not smoke. Smoking can damage your blood vessels and put you at increased risk for foot ulcers. Ask your care team provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your care team provider before you use these products.
When should I call my care team provider?
- Your feet become numb, weak, or hard to move.
- You have pus draining from a sore on your foot.
- You have a wound on your foot that gets bigger, deeper, or does not heal.
- You see blisters, cuts, scratches, calluses, or sores on your foot.
- You have a fever, and your feet become red, warm, and swollen.
- Your toenails become thick, curled, or yellow.
- You find it hard to check your feet because your vision is poor.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
