Chemical Skin Burn
Medically reviewed by Drugs.com. Last updated on May 6, 2024.
Examples of chemicals that can burn skin are found in cleaning products, paint stripper, and pesticides. Chemicals may also be found in some workplaces, such as wet or dry cement or battery acid. Signs and symptoms may not develop for several days. A burn may be worse than it appears at first. It may also get worse over the first few days.
DISCHARGE INSTRUCTIONS:
Return to the emergency department if:
- Your burn has more redness, pain, or swelling.
- Your burn oozes yellow liquid that smells bad.
- Your burned skin starts to tighten and restrict your movement.
- Your burned skin changes color or a new wound develops.
Call your doctor or burn specialist if:
- You have a fever.
- You have less energy and feel ill.
- You have blisters that rupture.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Antibiotics help fight or prevent an infection caused by bacteria.
- Anti-itching medicine may help keep your burned skin from itching as it heals. It may be given as a pill or cream.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Early care of the burn area:
Your burn will be covered with a bandage to keep it moist and clean. The bandage absorbs fluid that drains from the wound and helps prevent infection. Change your bandage as often as directed, and if it becomes soaked with fluid from the wound. You may need to change the bandage 2 times each day to start, and then 1 time each week after that.
Later care of the burn area:
Do the following after healthy skin covers the burn area:
- Apply a moisturizer such as aloe vera cream to the burn area. This can help keep the skin moist and reduce itching. Loose, soft clothing can also help relieve itching.
- Do not expose your wound to direct sunlight. For at least 12 months, apply sunblock to your wound every time you go outside during the day. Use a sunblock with an SPF of 25 or higher.
- Follow instructions to help reduce scarring. Scars can limit your movement.
Prevent chemical skin burns:
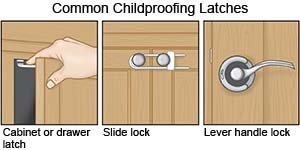
- Store cleaning products out of the reach of children. Read the safety information on the labels of household cleaning products before you use them. Use child safety locks to keep children out of storage areas.
- Wear safety equipment when you use chemicals. Examples include gloves, protective clothing, and goggles. Read all labels before you use any chemical. Make sure you know how to use the chemicals correctly. Follow all safety rules in your workplace.
Follow up with your doctor or burn specialist in 1 day, or as directed:
You may need regular follow-up visits until your burn heals. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
