Developmental Dysplasia of the Hip in Children
Medically reviewed by Drugs.com. Last updated on Apr 2, 2024.
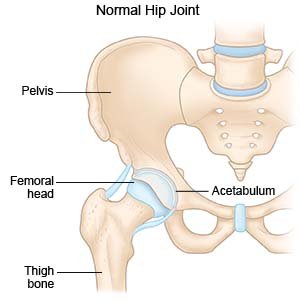
DDH is a condition that prevents parts of your child's hip joints from fitting together correctly.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- Your child feels lightheaded, short of breath, and has chest pain.
Seek care immediately if:
- Your child's splint or cast gets damaged or breaks.
- Your child's skin around his or her toes or hips is blue, cold, or numb.
Call your child's doctor if:
- Your child's pain is getting worse, even after he or she has taken pain medicine.
- Your child's skin is itchy, swollen, or has a rash.
- You have questions or concerns about your child's condition or care.
Medicines:
- Prescription pain medicine may be given. Ask your child's healthcare provider how to give this medicine safely.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Give your child's medicine as directed. Contact your child's healthcare provider if you think the medicine is not working as expected. Tell the provider if your child is allergic to any medicine. Keep a current list of the medicines, vitamins, and herbs your child takes. Include the amounts, and when, how, and why they are taken. Bring the list or the medicines in their containers to follow-up visits. Carry your child's medicine list with you in case of an emergency.
Prevent blood clots:
Your child may be at risk for blood clots if he or she has limited movement. Ask your child's healthcare provider if your child needs to elevate his or her legs above the level of his or her heart. Elevation will keep blood from staying in his or her legs and may prevent blood clots from forming. As pain decreases, your child may need to start moving or walking to improve blood circulation and bone healing.
Manage your child's DDH:
- Your child needs rest to heal. Quiet play will keep your child safely busy. Have your child read or draw quietly when he or she is awake. Follow instructions for how much rest your child should get while he or she heals.
- Talk to your child's healthcare provider about exercise and play for your child. Together you can plan the best exercise program for your child. It is best to start slowly and do more as he or she gets stronger. Exercise will help make his or her bones and muscles stronger.
- Use a car seat and safety vest in the car. These are made for children in spica casts and Pavlik harnesses. They should be used while your child is in a car. Ask where you can get a car seat or safety vest for your child.
- Ask your child's healthcare provider how to use a hip brace correctly. To keep your child from falling, remove loose carpeting from the floor. Have him or her use chairs with side arms and hard cushions to make it easier to get out of a chair. You may want to put a chair or a commode inside the shower.
- Take your child to physical and occupational therapy as directed. A physical therapist teaches your child exercises to help him or her improve movement and strength. An occupational therapist teaches your child skills to help with his or her daily activities.
Follow up with your child's doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Developmental Dysplasia of the Hip
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
